BioPoly - ISAKOS Cartilage Symposium - Shanghai June 2017
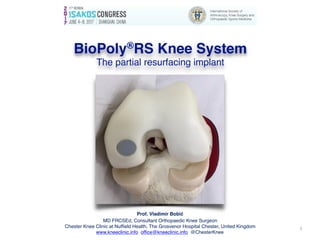
- 1. Prof. Vladimir Bobić MD FRCSEd, Consultant Orthopaedic Knee Surgeon Chester Knee Clinic at Nuffield Health, The Grosvenor Hospital Chester, United Kingdom www.kneeclinic.info office@kneeclinic.info @ChesterKnee BioPoly®RS Knee System The partial resurfacing implant 1
- 2. Relevant Disclosures 1: Royalties received from Schwartz Biomedical 3b: Paid Consultant for intellectual property (implant and instrument design), Schwartz Biomedical 2
- 3. Mr Mike McNicholas BSc, MD, FRCSEd(Tr&Orth), FFSEM RSCI Consultant, University Hospital Aintree, Liverpool Hon Prof, Directorate of Sport, University of Salford Hon Senior Lecturer, Department of Musculoskeletal Biology, University of Liverpool BioPoly® RS Knee System The partial resurfacing implant Cardiff, 3rd February 2017 3 @BioKneeSociety
- 4. Articular Cartilage Repair: Surgical Options ACI/MACI BioPoly: Filling the Void? OATSMicrofracture Allografts UKR & TKR 4
- 5. BioPoly Femoral Resurfacing Implant Articular Component: Patented Combination UHMWPE + HA 5
- 6. Poly vs BioPoly Wetability Hydrophilic 6
- 7. Self-lubricating material for better wear 7
- 8. • BioPoly® Material – “Microcomposite” (UHMWPE and Hyaluronic Acid) – Hydrophilic (water attracting) polymer • Hyaluronic Acid within BioPoly® – Attracts synovial fluid for lubrication – Allows for articulation with cartilage • No damage to opposing cartilage surfaces • No damage to implant surface • Resurfacing Applications BioPoly® Technology Overview Hyaluronic Acid 8
- 9. Material properties 9 Material Density Modulus Poisson’s ratio Hyperelastic Trabecular bone 1.8 g/cc1 1.15 GPa 0.22 NA Cartilage 1 g/cc 10 MPa 0.495 (incompressible) Neo Hooke C10 = 1.672 MPa, D1 = 0.0 Titanium 4.5 g/cc3 103 GPa 0.343 NA Co-Cr 8.41 g/cc3 233 GPa 0.3 NA UHMWPE (unhydrated) 0.945 g/cc4 830 MPa 0.464 NA 1 http://silver.neep.wisc.edu/~lakes/BoneTrab.html 2 van Rietbergen B, Majumdar S, Pistoia W, et al. Assessment of cancellous bone mechanical properties from micro-FE models based on micro-CT, pQCT and MR images. Technol Health Care. 1998;6:413–420. 3 http://www.fwmetals.com/titanium-wire-alloys.php 4 http://www.goodfellow.com/E/Polyethylene-UHMW.html
- 10. FEA Comparison of Partial Resurfacing Femoral Implants: BioPoly RS and a metallic implant • Contact biomechanics between femoral condyle focal defect implant and the opposing tibial articulating surface. • Resulting biomechanical interface: Reduced contact stresses and strains 10
- 11. Results: Compressive Strains 11 Metallic Implant Compressive Log strains at the tibial surface below implant apex Peak -0.3 BioPoly Compressive Log Strains at the tibial surface below implant apex Peak -0.100 Additional load sharing zones
- 13. BioPoly - Deformed shape at 1000N (note larger area of tibial cartilage engaged in load sharing) 13
- 14. Results in lower opposing cartilage contact pressure (2.5x body weight load) BioPoly Tibial Cartilage Contact Pressure Peak = 3.46 MPa Active Contact Zone Loaded Area ~ 471 mm2 Metal Implant Tibial Cartilage Contact Pressure Peak = 7.24 MPa Active Contact Zone Loaded Area ~ 314 mm2 14
- 15. ®Confidential BioPoly RS Knee and Patella System • CE Marked • Suitable for cartilage defects in the distal femur and patella up to 3.1 cm2 • Femoral Condyle and Trochlear Facet Implants – Ti64 grit blasted stems. Press fit or cemented • Patella implants – All BioPoly construction for cementation • Simple surgical instrument set and technique • Existing reimbursement codes Femoral Condyles and Trochlear Facets Patella 15mm 20mm 15x24mm 15mm/0 15mm/1 20mm/0 20mm/1 15
- 16. BioPoly RS Knee Surgical Technique 16
- 17. 17 The Race-track BioPoly RS Knee Surgical Technique
- 20. 20 BioPoly RS Knee Surgical Technique
- 21. 21 BioPoly RS Knee Surgical Technique
- 22. 22 BioPoly RS Knee Surgical Technique
- 23. 23 BioPoly RS Knee Surgical Technique
- 24. 24 BioPoly RS Knee Surgical Technique
- 25. 25 BioPoly RS Knee Surgical Technique
- 26. 26 BioPoly RS Knee Surgical Technique
- 27. 27 BioPoly RS Knee Surgical Technique
- 28. 28 BioPoly RS Knee Surgical Technique
- 29. 29 BioPoly RS Knee Surgical Technique
- 30. 30 BioPoly RS Knee Surgical Technique
- 31. 31 BioPoly RS Knee Surgical Technique
- 33. 33
- 36. Cemented all BioPoly Implant 36
- 37. Current BioPoly® RS Partial Resurfacing 3 Families of Products BioPoly® RS KNEE CE Marked BioPoly® RS PATELLA CE Marked BioPoly® RS SHOULDER CE Marked Patella Humeral head Distal Femur 37 + BioPoly® RS Femoral Trochlea and Talar Dome in the pipeline
- 38. BioPoly ® RS Partial Resurfacing Knee Implantations 5 yrs 600+ cases 38
- 39. BioPoly® RS Partial Resurfacing Knee System Typical Resurfacing Patient ▪ 21+ year old active adult ▪ Knee pain ▪ Too young for TKR ▪ Often failed Debridement, Microfracture, OATS or ACI ▪ Patients wanting to regain active lifestyle ▪ Focal defects ▪ Femoral condyles 39
- 40. Preoperative knee imaging + MRI and Arthroscopy for lesional characteristics 40
- 41. Indications : Lesion Characteristics • Medial or Lateral femoral condyle, NOT tibial condyles • Focal 2cm 2 or (2.4 x 1.5) cm 2 ≤3.1cm 2 (Entire lesion visualized in static knee through static arthroscope) • ICRS grade 2, 3, or 4 • Contained ICRS 0/1 • Depth from articular surface < 4mm • Good subchondral bone (MRI) X41
- 42. Contradictions Lesion characteristics: • Uncontained • Very large • >1 implant required • Kissing lesion 42
- 43. Contradictions Other joint pathology • Malalignment • Laxity • Major meniscal deficiency • Subchondral sclerosis • Advanced degenerative changes 43
- 44. Registry Study: Preliminary Report 44
- 45. Study Investigators and Collaborators: Prof Vladimir Bobic - Chester Knee Clinic, Chester, UK Prof Mike McNicholas – Aintree, Liverpool, UK Mr Dinesh Nathwani - Imperial College, London, UK Prof Alister Hart - RNOH Stanmore, London, UK Mr Jonathan Miles - RNOH Stanmore, London, UK Matt Hill - Schwartz Biomedical, USA Herb Schwartz - Schwartz Biomedical, USA 45
- 46. Registry Study Design • Study Type: Post-market registry • 35 patients & 4 UK Centres • Control: Historical microfracture outcomes • Outcome measures: KOOS, VAS, Tegner, SF-36 46 Major Inclusion and Exclusion Criteria Inclusion Criteria Exclusion Criteria • Age 21 years and older • Body Mass Index (BMI) ≥ 30 • Symptomatic lesions classified as ICRS grade 2, 3, or 4 • Generalized degenerative or autoimmune arthritis • Lesion size ≤ 3.1cm2 circumscribed by normal or nearly normal (ICRS grade 0 or 1) cartilage with an overall depth ≤ 4mm from the articulating surface • Uncorrected chronic malalignment of the knee* • Uncorrected ligamentous instability* • Uncorrected mechanically symptomatic meniscal tear or total meniscectomy* • Sufficient subchondral bone quality to support implant • Kissing lesion on tibia • More than one implant required to accommodate lesion • Use with opposing articulating tibial components *Can be corrected during surgery
- 47. 47
- 48. Registry Study Results • Interim results after 2 years indicate: – Significant improvement in all clinical outcomes – One revision (2.9%) due to subchondral bone disorder – No differences between younger and older patients • Mean Defect size = 2.7cm2 • Over half of patient population (54.3%) failed previous cartilage repair procedures 48
- 49. Rotation of BioPoly Implant 49
- 50. Failed BioPoly Implant • Why? No structural or technical problems identified. No infection. Patient selection? Surgical technique? • Very difficult to remove! Revised successfully with deep subchondral drilling + ChondroTissue patch. • Possible reasons: inadequate osseous support (previous microfractures + failed MACI = failure of implant to bone integration) 50
- 51. Patient Adverse Events • 1 Wound infection reported after 1/12 – Resolved quickly with medication • 1 Patient began experiencing pain at 3/12 – Arthroscopy revealed implant intact, and loose cartilage body as source of pain – Removal of loose cartilage body resolved 2symptoms 51
- 52. Registry Study Results • BioPoly compared to historical microfracture outcomes – BioPoly patients on average 7 – 9 years older • Significantly superior KOOS QoL and Sport after 2 years 52
- 54. 54
- 55. OrthoBiologics vs Metal and Plastic Hmmm ... not really. Not so soon, but will happen ... 55
