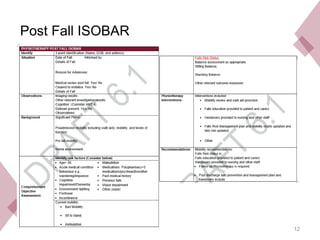
The document provides a summary of the updated 2023 Western Australian Multidisciplinary Post Fall Management Guidelines for physiotherapists. It outlines the physiotherapist's role in assessing, intervening, documenting, and discharging patients following a fall. Key responsibilities include reviewing patients within 2 days of a fall, assessing mobility and fall risks, providing interventions, documenting findings and recommendations, and identifying post-discharge needs. The guidelines aim to standardize best practice post-fall physiotherapy across Western Australian healthcare settings.