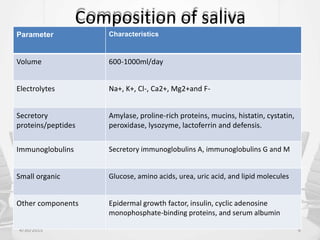
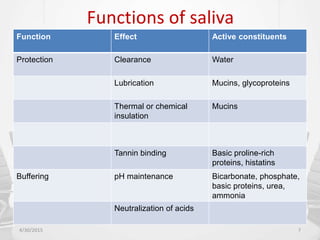
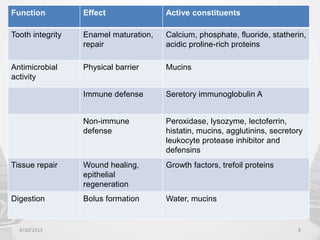
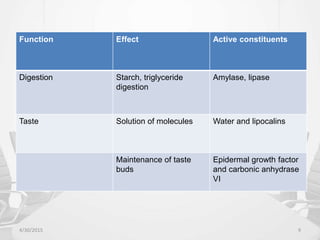
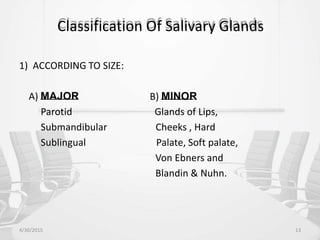
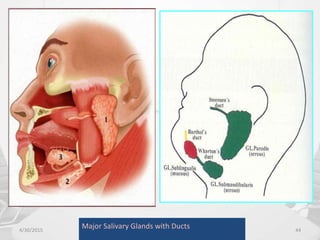
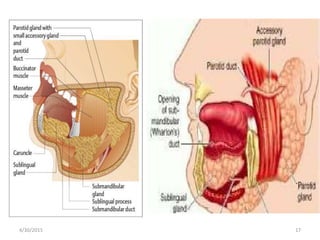
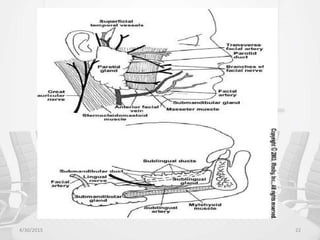
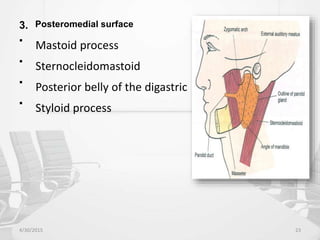
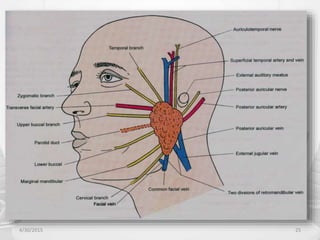
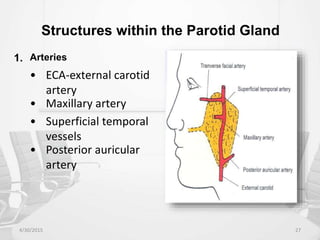
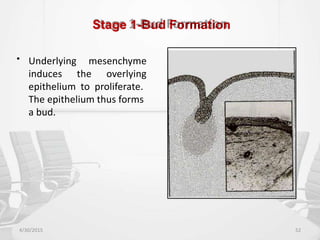
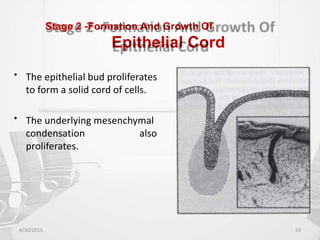
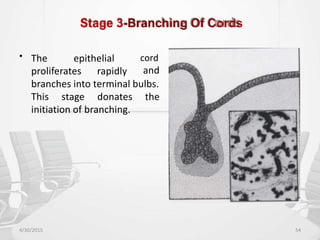
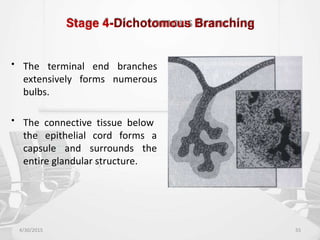
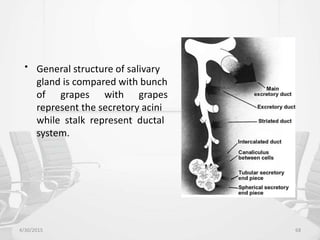
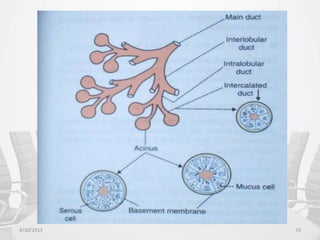
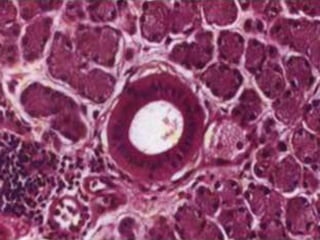
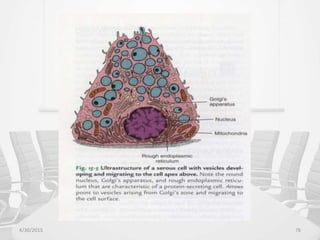
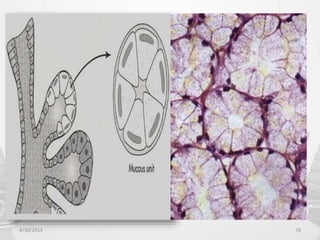
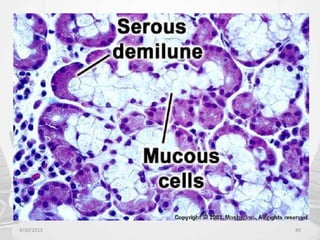
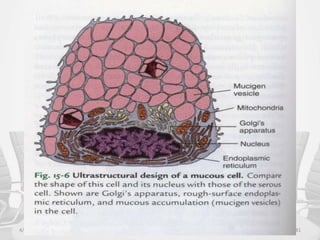
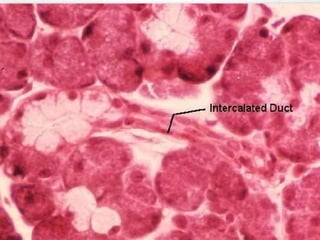
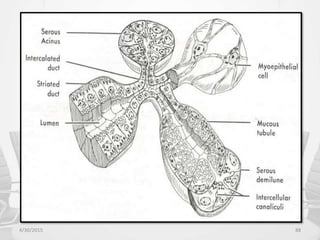
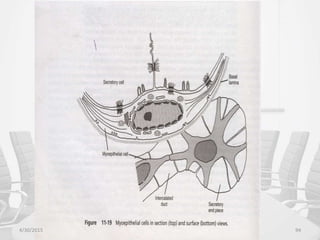
This document provides information about saliva and the salivary glands. It discusses the composition and functions of saliva, and the anatomy and histology of the major and minor salivary glands. The major salivary glands are the parotid, submandibular, and sublingual glands. They are located outside the oral cavity and secrete through duct systems. Numerous minor salivary glands are located within the oral cavity and secrete directly through short ducts. Development of the salivary glands occurs through stages including bud formation, cord formation, branching, and canalization.