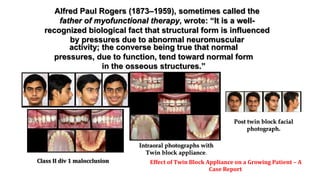
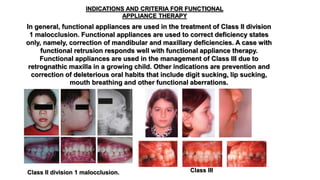
Functional appliances alter muscle function to induce orthopedic and orthodontic changes. They work by applying forces to move teeth and bone or by eliminating abnormal muscle forces. Common mechanisms include differential tooth eruption, tipping movements, and intrusion. The effects on dentition include correcting overjet through retroclination of upper incisors and proclination of lower incisors, as well as uprighting canines and premolars during eruption. Functional appliances aim to change either bone structure through growth modification or dental alignment through neuromuscular adaptation.