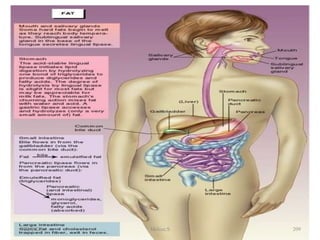
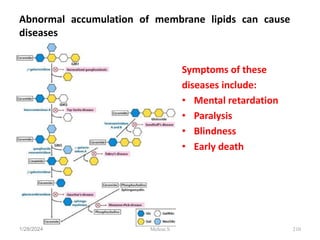
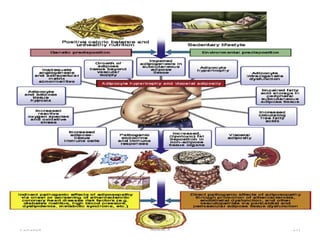
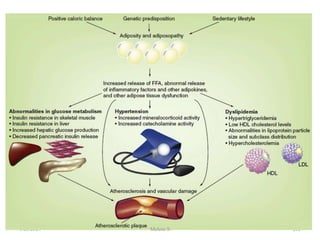
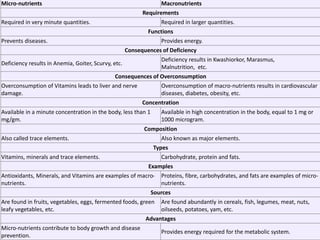
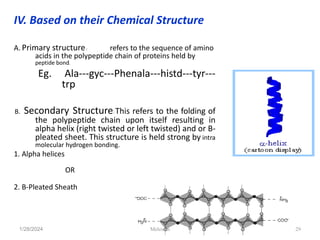
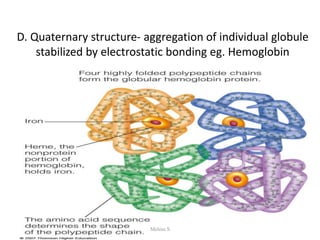
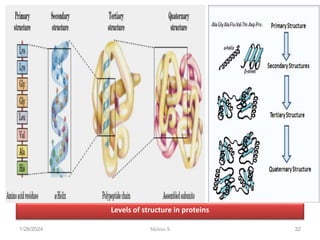
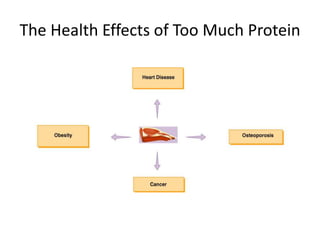
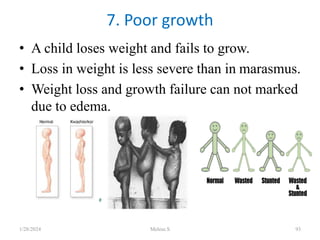
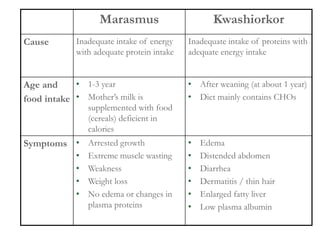
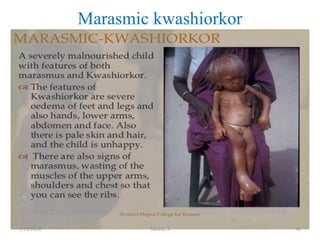
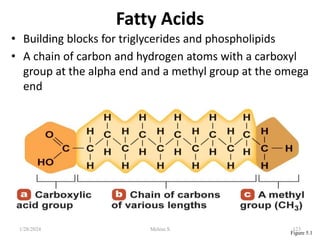
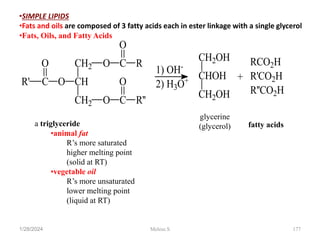
This document discusses proteins and lipids as macronutrients. It describes the functions and importance of proteins, including their roles in building tissues, making enzymes and hormones, and providing energy. It defines essential and non-essential amino acids and discusses protein deficiency diseases. The document also discusses different types of proteins like whey, casein and soy proteins. It describes the roles and health benefits of whey protein, as well as diseases associated with deficiencies in essential fatty acids and cholesterol abnormalities.



















































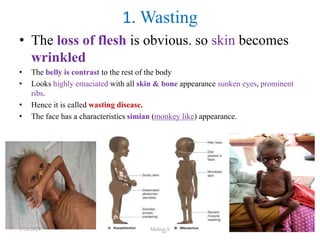

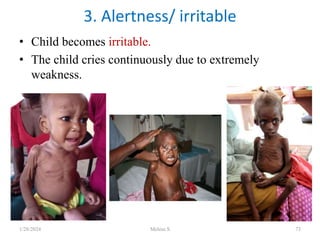


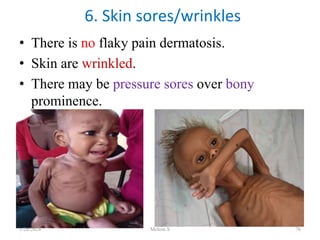
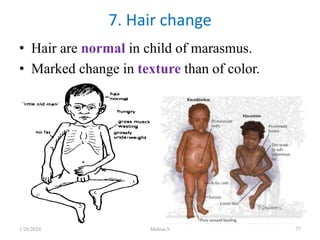















































































![HDL
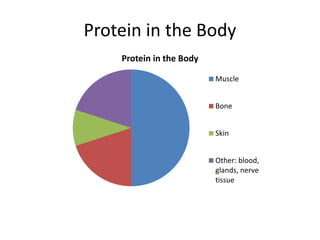
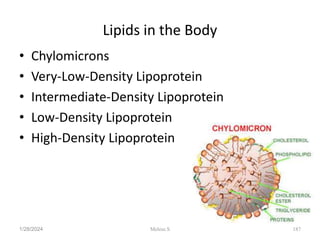
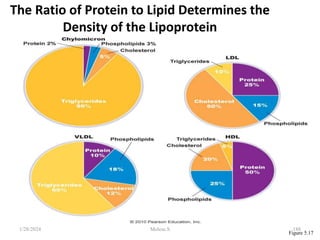
• HDL is a fraction of plasma lipoproteins
• It is composed of 50% protein, 25% phospholipid, 20%
cholesterol, and 5% triglycerides
• Evidence suggests that high-density lipoprotein (HDL)
cholesterol is cardioprotective.
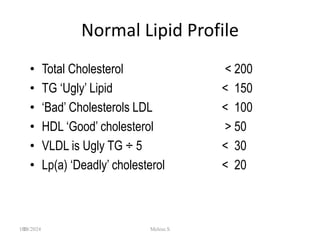
• LDL-chol = [Total chol] - [HDL-chol] - ([TG]/2.2) where
all concentrations are given in mmol/L
• (note that if calculated using all concentrations in
mg/dL then the equation is [LDL-chol] = [Total chol] -
[HDL-chol] - ([TG]/5))
1/28/2024 195
Melese.S](https://image.slidesharecdn.com/protienlecturelipids2024-240128112805-897653ba/85/protien-lecture-lipids-2024-pptx-195-320.jpg)