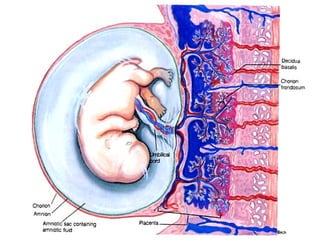
Placental Function: Transfer of Nutrients and Waste Between Mother and Fetus
- 2. PLACENTAL FUNCTION Transfer of nutrients and waste products bn the mother & fetus. RESPIRATORY EXCRETORY NUTRITIVE Produces or metabolizes the hormones & enzymes necessary to maintain the pregnancy.
- 4. Transfer function Transport is facilitated by the close approximation of maternal and fetal vascular systems within the placenta. It is important to recognize that there normally is no mixing of fetal and maternal blood within the placenta.
- 5. Respiratory function—Intake of o2 & output of co2 takes place by simple diffusion.o2 supply to fetus rate of 5ml/kg/min & this achieved with cord flow of 165-330ml/min. Excretory function—waste products urea, uric acid,creatinine are excreted to maternal blood by simple diffusion.
- 7. NUTRITIVE FUNCTION Glucose is the major energy substrate provided to the placenta and fetus. It is transported across the placenta by facilitated diffusion via hexose transporters Although the fetus receives large amounts of intact glucose, a large amount is oxidized within the placenta to lactate, which is used for fetal energy production.
- 8. Amino acid concentrations in fetal blood are higher than in maternal blood. Amino acids are therefore transported to the fetus by active transport . LIPIDS—TG`s & FA directly transported from mother to fetus in early pregnancy but synthesised in fetus later in pregnancy. Thus,fetal fat has got dual origin.
- 9. Water & electrolytes—Na,K+,Cl- by simple diffusion.Ca,Ph,iron by active transport. BARRIER FUNCTION:-Protective barrier to the fetus against noxious agents circulating in maternal blood. (High MW >500daltons.
- 10. IMMUNOLOGICAL FUNCTION Fetus & placenta contain paternally determined antigens,foreign to the mother . Inspite of this ,no evidence of graft rejection. Probably: 1. Fibrinoid & sialomucin coating of trophoblast may suppress the troblastic antigen. 2. Placental hormones ,steriods,HCG have got weak immunosuppressive effect,may be responsible for producing sialomucin.
- 11. 3.Nitabuch`s layer which intervenes bn decidua basalis &cytotrophoblast probably inactivates the antigenic property of tissue. 4.There is little HLA & blood group antigens on trophoblast surface.so antigenic stimulus is poor. 5. Production of block antibodies by mother ,protects fetus from rejection.
- 12. ENDOCRINE—hormones secreted internally. HORMONE--Any organic chemical that is secreted by a gland into the circulatory system and is transported to some target organ. The target may be either peripheral tissue (such as muscle or other gland) or brain.
- 13. Fetal, placental & maternal compartments form an integrated hormonal unit The feto-placental-maternal (FPM) unit creates the Endocrine Environment that maintains and drives the processes of pregnancy and pre-natal development.
- 14. PLACENTAL HORMONES Human Chorionic Gonadotropin (hCG Human Chorionic Somammotropin (hCS) or Placental Lactogen(hPL) OTHER HORMONES Chorionic Adrenocorticotropin Chorionic thyrotropin Relaxin PTH-rP hGH-V Estrogen (E) Progesterone (P) HYPOTHALAMIC-LIKE RELEASING HORMONES GnRH CRH cTRH GH-RH PLACENTAL PEPTIDE HORMONES Neuropeptide-Y Inhibin & Activin ANP
- 15. To understand the FPM one should know:1. The major hormones involved: hCGn Progesterone Estrogen Human Chorionic Somatomammotropin (hCS) (placental lactogen) 2. How the FPM compartments work together to produce the steroid hormones 3. The transfer of hormones between the FPM compartments.
- 17. Human Chorionic Gonadotropin (hCG) PREGNANCY HORMONE--- glycoprotein Half life –24hrsof hCG Levels peak at 60-70 days then remain at a low plateau for the rest of pregnancy. Placental GnRH have control of hCG. FUNCTIONS: 1. RESCUE &MAINTENANCE of function of corpus luteum.
- 18. Prevents degeneration of corpus luteum Stimulates corpus luteum to secrete E + P which, in turn, stimulate continual growth of endometrium. 2.hCG stimulates leydig cells of male fetus to produce testosterone in conjunction with fetal pituitary gonadotrophins.Thus indirectly involed in development of external genitalia. 3. Suppresses maternal immune function & reduces possibility of fetus immunorejection
- 19. Human Chorionic Somammotropin (hCS) or Placental Lactogen Structure similar to growth hormone Produced by the placenta Levels throughout pregnancy Large amounts in maternal blood but DO NOT reach the fetus
- 20. Human Chorionic Somammotropin (hCS) or Placental Lactogen Biological effects are reverse of those of insulin: utilization of lipids; make glucose more readily available to fetus, and for milk production. hCS levels proportionate to placental size hCS levels placental insuffiency
- 21. Estrogen (E) FORMS-estriol,estradiol &estrone . Estriol most important . Levels increase throughout pregnancy 90% produced by placenta. (syncytiotrophoblast) Placental production is transferred to both maternal and fetal compartments
- 23. Two of the principle effects of placental estrogens are: Stimulate growth of the myometrium and antagonize the myometrial-suppressing activity of progesterone. In many species, the high levels of estrogen in late gestation induces myometrial oxytocin receptors, thereby preparing the uterus for parturition. Stimulate mammary gland development. Estrogens are one in a battery of hormones necessary for both ductal and alveolar growth in the mammary gland.
- 24. Progesterone (P) Levels increase throughout pregnancy 80-90% is produced by placenta and secreted to both fetus and mother
- 25. Progestins, including progesterone, have two major roles during pregnancy: Support of the endometrium to provide an environment conducive to fetal survival. If the endometrium is deprived of progestins, the pregnancy will inevitably be terminated. Suppression of contractility in uterine smooth muscle, which, if unchecked, would clearly be a disaster. This is often called the "progesterone block" on the myometrium. Toward the end of gestation, this myometrial- quieting effect is antagonized by rising levels of estrogens, thereby facilitating parturition.
- 26. Progesterone and other progestins also potently inhibit secretion of the pituitary gonadotropins luteinizing hormone and follicle stimulating hormone. This effect almost always prevents ovulation from occuring during pregnancy
- 29. Adrenal Gland Development Adrenal Cortex Vital to organism survival Begins to develop at 4th week of embryonic life Functional around 10th to 12th week of embryonic life Enzymes necessary for biosynthesis of adrenocortical hormones do not develop simultaneously hCG may have a role in stimulating Adrenocortical development Adrenal Medulla Originates from nervous system Ganglia of Autonomic Nervous System
- 30. Fetal Adrenal Cortex Function Adrenal Cortex Zona Glomerulosa Has enzymes to convert Pregnenalone to: Progesterone Deoxycorticosterone Corticosterone Aldosterone Zona Fasciculata Converts Pregnenalone and Progesterone to 17OH-Pre and 17OH-Pro 17OH-Pro is converted to cortisol (major glucocorticoid) Zona Reticularis Converts 17OH-Pre into DHEA and Androstenedione (androgens)
Editor's Notes
- FETAL ADRENAL GLAND
