Ocular Chemical Burns Treatment Evidence
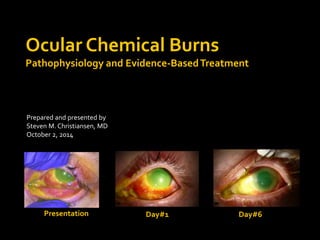
- 1. Ocular Chemical Burns Pathophysiology and Evidence-Based Treatment Prepared and presented by Steven M. Christiansen, MD October 2, 2014 Presentation Day#1 Day#6
- 2. Objectives Understand pathophysiology and classification of chemical burns Understand treatment of chemical burns ▪ Morgan Lens ▪ Medical Treatment ▪ ProKera Ring ▪ Amniotic membrane transplantation ▪ Limbal stem cell transplantation ▪ Tenonplasty ▪ Possible future treatments
- 3. Alkali Incidence greater than 2x that of acid burns 76% male, 24% female 90% accidental, 10% chemical assault ▪ Industrial, agricultural, and household accidents Most common causes: ammonia (NH3), lye (NaOH), potassium hydroxide (KOH), magnesium hydroxide [MG(OH)2], lime [Ca(OH)2] lye (NaOH) ammonia (NH3) magnesium hydroxide [MG(OH)2] lime [Ca(OH)2]
- 4. 30 year-old male transferred from OSH with 3-day history of chemical burn “Picked up bottle of drain cleaner and didn’t realize lid was off.” Pain began 30 minutes later; OTC irrigating kit and OTC triple antibiotic ointment at night 3 days later family urged to seek medical care ED at OSH irrigated with saline; pH reportedly neutral at transfer
- 5. Note the chemosis, 3+ injection, diffuse corneal edema and haze, significant epithelial defect, layering hypopyon, nasal limbal whitening, medial canthus whitening with possible necrosis, and loss of iris details
- 7. Four successive pH tests yielded a pH of approximately 8 Control testing of pH paper using sterile water with known pH of 5.5
- 8. During Morgan's third Vietnam War tour as a volunteer physician, he concluded that many serious eye problems developed in individuals because fairly simple infections had not been treated adequately and that a means for delivering constant irrigation or medication could decrease such infections. In February 1969, in Vinh Long, Morgan molded a simple device for cleaning the eye. Morgan was familiar with contact lenses (wearing them himself and often prescribing them to his patients), and his first Morgan Lens was larger than a modern contact lens, resembling the early contact lenses of the 1940s. His invention is known today as the Morgan Lens, and is used in many Emergency Departments to provide constant ocular irrigation following chemical injuries. http://www.youtube.com/watch?v=zmXqunkuVR4
- 10. Severity of ocular injury is related to surface area and degree of penetration (alkali>acids) The hydroxide ion saponifies fatty acid components of cell membranes, resulting in cell disruption and death, while the cation is responsible for penetration of the specific alkali
- 11. Hydration of the glycosaminoglycans within the corneal stroma results in loss of clarity Above is a slit lamp photo of the patient prior to fluorescein staining. Note the significant haze and loss of clarity
- 12. Hydration of collagen fibrils results in thickening and shortening causing distortion of the trabecular meshwork Release of prostaglandins are responsible for the elevation in IOP often seen immediately following alkali injuries
- 13. Damage to the ciliary body epithelium results in decreased secretion of ascorbate and a reduction in anterior chamber concentration Ascorbate is required by corneal keratocytes to synthesize collagen and repair stroma In a 1980 article published in Ophthalmology, authors found that severe ocular alkali burns in rabbits results in a decrease in aqueous humor ascorbate levels to 1/3 normal levels and that this deficiency can be reversed by immediate treatment with parenteral or topical ascorbate. Avoiding ascorbate deficiency decreases corneal ulceration by providing sufficient ascorbic acid to fibroblasts for collagen synthesis
- 14. Stem cells in the limbus divide to produce a daughter stem cell and a transient amplifying cell. These transient amplifying cells migrate within the cornea to lie in basal layer of corneal epithelium. Further cellular divisions of transient amplifying cells produce postmitotic cells, which lie in the suprabasal layers. Progressive differentiation of postmitotic cells produce terminally differentiated cells, which lie in the superficial corneal epithelial layers. These terminally differentiated cells are non-keratinized, stratified squamous corneal epithelial cells. These cells are continually sloughed away from the corneal surface and replaced by maturing, underlying cell layers. http://www.eophtha.com/eophtha/Anatomy/anatomyofcornea4.html
- 15. Limbal and Conjunctival stem cells resurface chemically injured corneal epithelium Conjunctival stem cells (as opposed to limbal stem cells) never fully transdifferentiate to corneal epithelium and may be associated with: ▪ Delayed reepithelialization, superficial and deep stromal vascularization, persistence of goblet cells, and poor epithelium-basement membrane adhesion Limbal stem cells recreate corneal surface (ideal) while conjunctival stem cells repair the epithelial defect (good) but leave vascularization and fibrosis (less than ideal, causing poor vision following reepithelialization
- 16. Keratocytes responsible for maintenance and regeneration Keratocytes may break down collagen via collagenase or synthesize collagen ▪ Matrix metalloproteinases active during remodeling ▪ Excessive degradation via MMP-1 and MMP-8 may lead to sterile corneal ulceration ▪ Goal = shift balance toward synthesizing, not degrading collagen
- 17. Within 12-24 hours, PMNs and mononuclear cells accumulate, leading to degranulation and release of MMP-8, also known as type 1 collagenase Debridement of necrotic conjunctiva eliminates a source for continuous leukocyte infiltration
- 18. Grade 1 Little or no loss of limbal stem cells* or limbal ischemia Grade 2 Subtotal loss of limbal stem cells and ischemia< ½ limbus Grade 3 Total loss of limbal stem cells, preservation of proximal conjunctival epithelium, and ischemia <1/2 limbus Grade 4 Total loss of limbal stem cells, loss of proximal conjunctival epithelium, with damage to entire anterior segment *Extent of limbal stem cell loss can be estimated only after weeks of observation (unless stem cell stains readily available)
- 19. Acute (0-7 days) Monitor IOP, inflammation, reepithelialization Little to no collagenolytic activity during this phase Early Repair (7-21 days) Grade I, II reepithelialization continues slowly Grade III, IV no reepithelialization due to loss of limbal stem cells Second wave of inflammatory cell infiltration with progressive inflammation as long as epi defect persists Late Repair (day 21 to several months later) By day 21, inflammation, collagen synthesis, and collagenase activity at highest levels Grade I - complete reepithelialization Grade II - with sectoral epi defect due to sectoral loss of limbal stem cells; conjunctiva may epithelialize; fibrovascular pannus Grade III - conjunctival epithelialization with fibrovascular pannus resulting in tectonically stable but scarred and vascularize cornea Grade IV – conjunctival epithelialization; ischemic necrosis, may develop cicatricial entropion, symblepharon
- 20. Topical Corticosteroids Q1-Q2H Medroxyprogesterone Q2H Sodium ascorbate 10% Q2H Sodium citrate 10% Q2H Tetracycline 1% ointment QID Cycloplegia as needed IOP control as needed Systemic Doxycycline 100 mg BID Sodium ascorbate 2 grams QID The Wagoner Chemical Injury Protocol as explained in the Iowa Ophthalmology Residency On-Call Survival Guide *Not included in most recently updated protocol
- 21. Topical Corticosteroids Q1-Q2H ▪ Decrease inflammation Medroxyprogesterone This study, published in IOVS in 1977 described a substantial reduction in perforation and deep ulceration of the alkali-burned rabbit cornea by topical or parenteral medroxyprogesterone. However, medroxyprogesterone has also been shown to suppress corneal neovascularization and minimally suppress stromal wound repair. Some authors recommend substituting corticosteroids for medroxyprogesterone after 10-14 days to minimize interruption of stromal repair.
- 22. Topical and Systemic Sodium ascorbate is involved in collagen synthesis Treating with sodium ascorbate minimizes deficiency and enables corneal repair
- 23. Topical Sodium citrate ▪ Calcium required for chemotaxis, phagocytosis, and enzymatic release from PMNs ▪ Citrate chelates calcium This 1984 study published in Experimental Eye Research found that topical sodium citrate inhibited PMN infiltration and corneal ulceration
- 24. Systemic Doxycycline ▪ Tetracyclines ▪ restrict gene expression of neutrophil collagenase ▪ suppress 1-antitrypsin degradation ▪ scavenge reactive oxygen species This study, published in 2000 reported that tetracyclines inhibit matrix metalloproteinases by mechanisms independent of their antimicrobial properties, primarily through restriction of the gene expression of neutrophil collagenase and epithelial gelatinase, suppression of 1-antitrypsin degradation, and scavenging of reactive oxygen species.
- 25. Topical Corticosteroids Q1-Q2H Medroxyprogesterone Q2H Sodium ascorbate 10% Q2H Sodium citrate 10% Q2H Tetracycline 1% ointment QID Cycloplegia as needed IOP control as needed Systemic Doxycycline 100 mg BID Sodium ascorbate 2 grams QID *Not included in most recently updated protocol
- 26. Note the increased injection throughout the conjunctiva, as well as the ischemic limbal whitening. In the bottom left photo, note the partial reepithelialization from about 10 to 4 o’clock, suggestive of persistent limbal stem cells in this area
- 28. Amniotic membrane Thin, semitransparent innermost layer of fetal membrane; avascular stroma, basement membrane, and epithelium Requires at least partial limbal stem-cell function Reepithelialization facilitated by providing a basement membrane to which epithelium may adhere and promoting proliferation of limbal stem cells and transient amplifying cells via growth factors within transplanted membrane Orientation dictates area of epithelialization If basement membrane oriented towards eye, acts as an ‘onlay’ patch graft, promoting epithelialization beneath membrane If basement membrane oriented away from eye, acts as an ‘inlay’ graft, with amniotic membrane functioning as new basement membrane, promoting epithelialization above the graft Can also create amniotic membrane sandwich with basement membranes oriented towards each other to promote reepithelialization between the two basement membranes Successful reepithelialization reported in grade II and III injuries; disappointing results in grade IV injuries
- 29. Amniotic membrane transplantation can be performed using a ProKera Ring, which is essentially amniotic membrane within a ring-shaped material that can then be placed over the cornea much like a scleral contact lens. If a larger surface area needs to be covered, many surgeons prefer free amniotic membrane transplantation, which must be performed in the OR. This often takes place following use of a ProKera Ring.
- 30. Note the complete ischemia from 6:30 to 11:00, caruncle and nasal conjunctival necrosis, and scleral melting nasally. Also note the persistent but healing corneal epithelial defect.
- 31. Tenonplasty Use healthy, vascularized tissue to reduce necrosis, promote reepithelialization Debride devitalized conjunctiva, advance Tenon’s capsule to limbus
- 32. Limbal stem cell transplantation Only method of reestablishing phenotypically correct corneal epithelial surface in grade III or IV injuries to avoid fibrovascular pannus (III) or sterile corneal ulceration (IV) https://www.youtube.com/watch?v=3v1FGY2yhQY
- 33. Boston Keratoprosthesis A good option for patients who have failed prior medical and surgical therapy Wynn Institute for Vision Research at the University of Iowa Hoping to develop a method for harvesting residual stem cells from patients with bilateral eye injuries with loss of stem cells, culturing the enriched populations and implanting the stem cells back to the same patient at a later date, which would prove a great benefit over the current treatment which involves use of cadaver stem cells which often end up rejecting despite aggressive immunosuppression.
- 34. Presentation Day#1 Day#6 Thank you
- 35. References 1. Wagoner MD. Chemical injuries of the eye: current concepts in pathophysiology and therapy. Surv Ophthalmol. 1997 Jan-Feb;41(4):275-313. Review. PubMed PMID: 9104767. 2. The Morgan Lens for Eye Irrigation. YouTube. http://www.youtube.com/watch?v=zmXqunkuVR4. Accessed 10/6/14 3. Pfister RR, Paterson CA. Ascorbic acid in the treatment of alkali burns of the eye. Ophthalmology. 1980 Oct;87(10):1050-7. PubMed PMID: 7243199. 4. Newsome NA, Gross J. Prevention by medroxyprogesterone of perforation in the alkali-burned rabbit cornea: inhibition of collagenolytic activity. Invest Ophthalmol Vis Sci. 1977 Jan;16(1):21-31. PubMed PMID: 188776. 5. Paterson CA, Williams RN, Parker AV. Characteristics of polymorphonuclear leukocyte infiltration into the alkali burned eye and the influence of sodium citrate. Exp Eye Res. 1984 Dec;39(6):701-8. PubMed PMID: 6097468. 6. Ralph RA. Tetracyclines and the treatment of corneal stromal ulceration: a review. Cornea. 2000 May;19(3):274-7. Review. PubMed PMID: 10832682. 7. Clare G, Suleman H, Bunce C, Dua H. Amniotic membrane transplantation for acute ocular burns. Cochrane Database Syst Rev. 2012 Sep 12;9:CD009379. doi: 10.1002/14651858.CD009379.pub2. Review. PubMed PMID: 22972141. 8. The Wagoner Chemical Injury Protocol. Principles and Practice of Ophthalmology, 3rd Edition. Volume 1, Chapter 56, page 761. 9. Tenonplasty for Scleral Ischemia. YouTube. https://www.youtube.com/watch?v=3v1FGY2yhQY. Accessed 10/6/14.
Editor's Notes
- The hydroxide ion saponifies fatty acid components of cell membranes, resulting in cell disruption and death, while the cation is responsible for penetration of the specific alkali
- Hydration of the glycosaminoglycans within the corneal stroma results in loss of clarity
- Hydration of collagen fibrils results in thickening and shortening, which distorts the trabecular meshwork. Release of prostaglandins are responsible for the elevation in IOP often seen immediately following alkali injuries
- 1980 journal of Ophthalmology, authors found that severe ocular alkali burns in rabbits results in a decrease in aqueous humor ascorbate levels to 1/3 normal levels and that this deficiency can be reversed by immediate treatment with parenteral or topical ascorbate. Avoiding ascorbate deficiency decreases corneal ulceration by providing sufficient ascorbic acid to fibroblasts for collagen synthesis
- Stem cells in the limbus divide to produce a daughter stem cell and a transient amplifying cell. These transient amplifying cells migrate within the cornea to lie in basal layer of corneal epithelium. Further cellular divisions of transient amplifying cells produce postmitotic cells, which lie in the suprabasal layers. Progressive differentiation of postmitotic cells produce terminally differentiated cells, which lie in the superficial corneal epithelial layers. These terminally differentiated cells are non-keratinized, stratified squamous corneal epithelial cells. These cells are continually sloughed away from the corneal surface and replaced by maturing, underlying cell layers.
- Extent of epithelial and conjunctival surface involvement Depth of penetration based on corneal clarity, intraocular inflammation, IOP
- https://www.youtube.com/watch?v=3v1FGY2yhQY
- https://www.youtube.com/watch?v=3v1FGY2yhQY
- Of interest, we are hoping in the WIVR to develop a method for harvesting small residual stem cell populations in eyes with bilateral injury, culturing them in the lab, and then returning the culture-enriched populations back to the same patient at a later date, rather than relying on cadaver stem cells which ultimately end up rejecting despite aggressive systemic immunosuppression.
- 121 5/10
- 121 5/10
