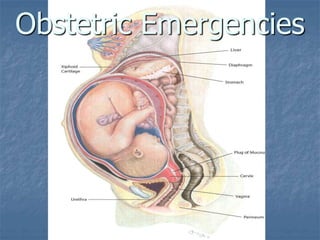
OB emergencies.ppt
- 2. Obstetric Emergencies: We will cover... Normal Pregnancy Common medical and surgical complications of pregnancy
- 3. Normal pregnancy All females of childbearing age are presumed to be pregnant until proven otherwise. All pregnancy tests detect B-HCG which is produced at the time of implantation (8-9 days post conception) B-HCG should double every day for the first weeks, peak at week 8 and remain elevated up to 60 days post-partum
- 4. False Negatives Too early in pregnancy Dilute/old urine Ectopic Incomplete Ab. False Positives Urine: hematuria/proteinuria Serum: T.O.A. Thyrotoxicosis Molar pregnancy Drugs (MJ, ASA, Phenothiazines, anticonvulsants, antidepressants, methadone
- 5. Some Important Physiological Changes in Pregnancy Cardiac: increased heart rate, decreased blood pressure. CO increases Respiratory: rate increases, TV increases, FRV decreases, pCO2 decreases Heme: Volume increases, HCT drops, WBC increases
- 6. Drugs in Pregnancy: A, B, C, D, X Considered Safe in pregnancy: PCN Cephalosporins Azithro/Erythromycin Acetaminophen Narcotics Heparin Asthma Drugs Reglan (Metoclopramide) Immunizations derived from killed viruses (tetanus, diptheria, Hep. B, Rabies)
- 7. Radiation in Pregnancy <5-10 rads = no significant risk of birth defects Beams aimed 10cm away from fetus pose no additional risk Initial trauma X-rays each deliver <1 rad One never withholds necessary radiography. Use MRI or U/S if available.
- 9. Normal, non-pregnant uterus on T/V U/S
- 10. The “Double-Ring” Sign or “Double Decidual” Sign of normal early pregnancy
- 11. Normal Pregnancy T/V Ultrasound Showing Gestational and Yolk Sac. No fetus is seen. 5w 2d
- 12. 6w 1d T/V U/S showing yolk sac
- 13. Normal T/V U/S with embryo at 10w 3d
- 14. Complications of Pregnancy – Vaginal Bleeding 1st Trimester Causes: 1. Ectopic 2. Abortion 3. Molar Pregnancy 4. Non-pregnancy Related a. Infectious b. Trauma c. Neoplasm
- 15. The work-up is the same! Pelvic Exam Beta HCG Transvaginal ultrasound Rh CBC, CMP PT/PTT/INR UA
- 17. Ectopic Pregnancy – A surgical emergency of pregnancy The leading cause of first trimester maternal death Usually 5-8 weeks after LMP High Risk: History of ectopic, tubal surgery or sterilization procedure, Known tubal scarring or pathology, Diethylstilbestrol exposure, IUD.
- 18. Signs/Symptoms Symptoms (in decreasing order of frequency): Abdominal pain, amenorrhea, vaginal bleeding (50-80%), dizziness, pregnancy symptoms, urge to defecate, passing tissue Signs: Adnexal tenderness, abdominal tenderness, adnexal mass, enlarged uterus, orthostatic changes, fever
- 19. Testing Beta > 6000 mIU/ml + empty uterus on transabdominal ultrasound OR Beta > 1200 mIU/ml + empty uterus on transvaginal ultrasound = Ectopic Pregnancy = Laparoscopy
- 20. Beta <6000 + empty uterus on transabdominal ultrasound OR Beta < 1200 + empty uterus on transvaginal ultrasound = serial outpatient beta measurements to ensure normal rise. This only applies to stable patients and should be done in consult with ob/gyn
- 21. A heterotopic pregnancy (to compare normal vs. abnormal)
- 23. 2nd Trimester Causes are abortion and non-pregnancy causes. Work-up is the same Management of threatened AB is the same If complete, may be D&C candidate If other types of AB, patient may undergo oxytocin induced labor as inpatient.
- 24. 3rd Trimester (>28 weeks) Placental Abruption Placenta separates from uterine wall Painful dark or clotted blood Risks: HTN, smoking, ETOH, cocaine, multiparity, previous abruption, trauma, mom > 40 Management: U/S, Ob consult, cardiac/fetal monitoring, IV, pre-op labs, delivery if possible Placenta Previa Placenta implants too low Painless bright red bleeding Risks: prior C-section, grand multiparity, previous previa, multiple gestations, multiple induced abortions, mom >40. Management: U/S, Ob consult, pre-op labs, avoid pelvic exam, c-section
- 25. 3rd Trimester Bleeding cont’d Uterine Rupture: Can be seen in scarred and unscarred uteri. (uteruses? uterata?)
- 28. Complications of Pregnancy: Trauma Key Concept: Although you have two patients, maternal circulation is to be maintained at the expense of the fetus. Without mom, the baby will surely die. Mom should be kept in left lateral decubitus This is where knowing the physiologic changes of pregnancy becomes extremely important ! Mom can lose up to 35% of her blood volume before showing any signs of shock!
- 29. Management Over 20 weeks: Goes to Ob for 4 hours of cardiotocographic monitoring All women with abdominal trauma get Rhogam (fetomaternal hemorrhage present in 30% of these patients) Kleihauer-Betke test: Used in women >12w to determine and quantify the amount of fetomaternal hemorrhage that occurred
- 30. Perimortem C-Section Fetus greater than 28weeks, maternal death less than 15 minutes = perimortem c-section
- 31. Complications of Pregnancy: Hypertension Can be chronic (meaning it began prior to conception or began during gestation and persists >6 weeks post-partum) or gestational. We care about this because HTN in pregnancy is associated with pre- eclampsia, abruption, prematurity, IUGR and stillbirth
- 32. Pre-eclampsia: To be considered in those >20wks with HTN Mild SBP > 140 (or +20 from baseline. Or DBP >90 (or +10 from baseline) Proteinuria .3g/24h +/- Edema No Oliguria No Associated symptoms Normal labs No IUGR Severe BP>160/90 Proteinuria >5g/24h Edema Present Oliguric Associated symptoms (H/A, visual symptoms, abdominal pain, pulm. edema Associated labs (dec. plts, inc. LFT, inc. bili, inc. creatinine, increased uric acid) IUGR present HELLP syndrome = very severe. Above +RUQ pain, n/v
- 33. Management Isolated HTN requires a 24h urine and close Ob f/u With other findings, admit, 24h urine, bed rest and HTN management in consult with ob/gyn. Hydralazine common though diazoxide, labetalol, nifedipine and nitroprusside also used +/- Mag to prevent seizures
- 34. Complications of Pregnancy: Eclampsia Preeclampsia +seizures or coma May occur without proteinuria, may occur up to 10 days postpartum ICH is the major cause of maternal death Warning signs = H/A, visual changes, hyperreflexia, Abd. pain Tx = Delivery. Magnesium, Phenytoin or Diazepam, Hydralazine or Labetalol
- 35. Complications of Pregnancy: UTI/Pyelo Pregnant women more prone to UTI secondary to physiologic changes of pregnancy Treat both symptomatic and asymptomatic bacturia (untreated = up to 40% risk of progression to pyelo) Culture urine, give 7 day course We admit pregnant women with pyelonephritis because of its increased risk of of progressing to preterm labor or septic shock.
- 36. Complications of Pregnancy: Appendicitis Appendicitis is the most frequent surgical emergency of pregnancy Incidence is the same as non-pregnant population but the complications are more frequent secondary to delayed diagnosis Again, the physiologic changes of pregnancy complicate the clinical picture (leukocytosis, displaced appendix) Picture mimics pyelo. When patients don’t improve with IV abx, the diagnosis is reconsidered. Laparotomy is the preferred diagnostic procedure. Ultrasound can used
- 38. References 1. Preparing for the Written Board Exam in Emergency Medicine. 5th ed. Vol 1. Rivers, Carol. pp 550-574 2. learnobultrasound.com/3trimesterbleed.htm 3. www.smbs.buffalo.edu/emed/emed/ultrasound.html 4. Harwood &Nuss’ Clinical Practice of Emergency Medicine 4th ed. Wolfson, Alan B Lippincott, Williams and Wilkins, Philadelphia, 2005. pp.496-497 5. home.flash.net/~drrad/tf/122396.htm 6. www.pwc-sii.com/Research/death/ribs.htm 7. www.jaapa.com/.../article/130146/ 8. www.advancedfertility.com/ultraso1.htm 9. Ma, John O. Emergency Ultrasound via access emergency medicine at http://0- www.accessem.com.innopac.lsuhsc.edu/content.aspx?aID=100900