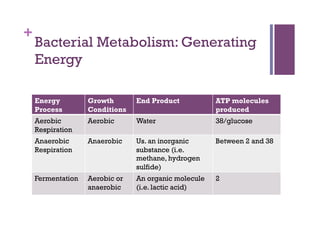
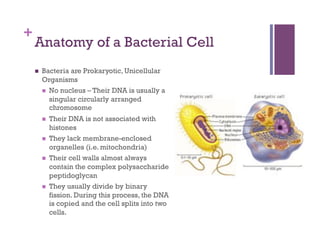
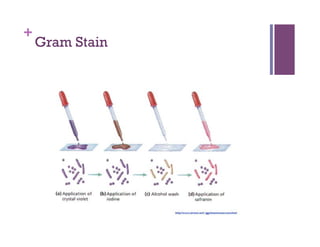
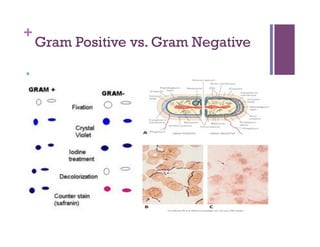
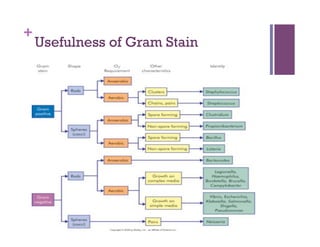
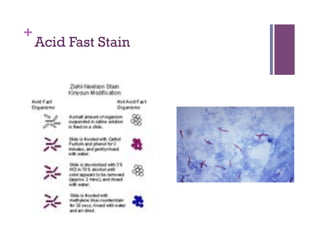
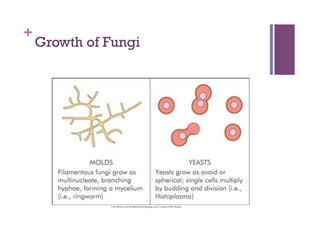
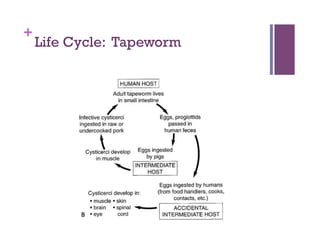
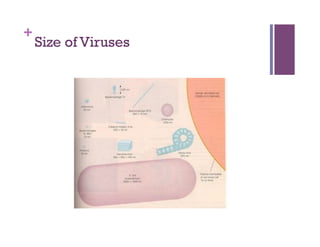
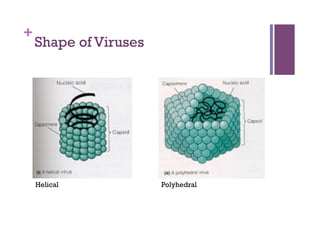
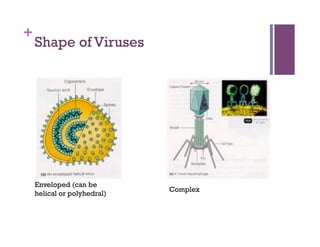
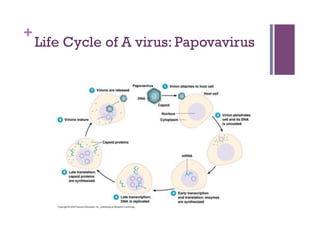
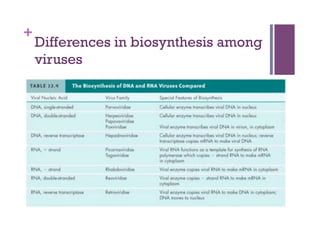
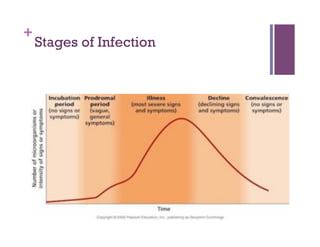
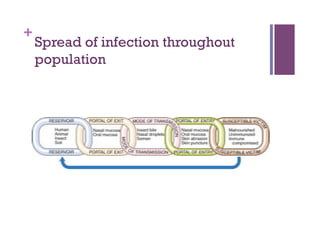
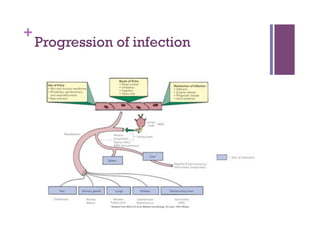
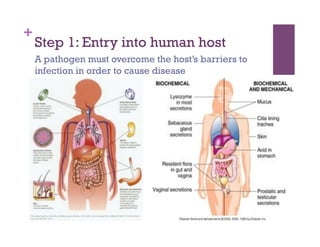
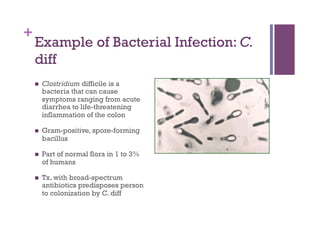
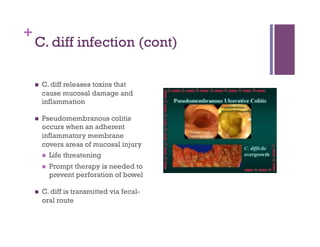
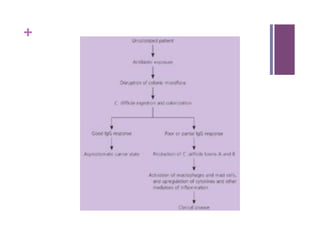
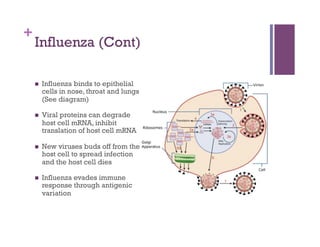
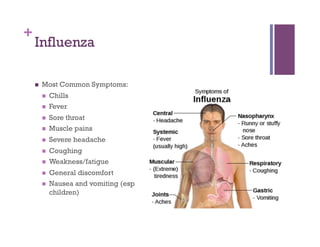
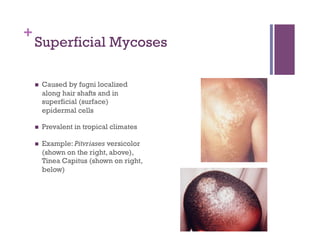
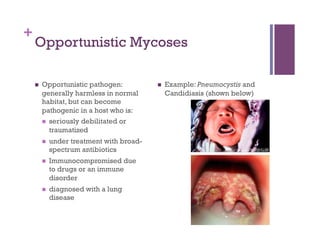
The document discusses microbiology concepts including bacteria, fungi, helminths, and viruses. It covers their basic structures and characteristics, how they cause disease, and modes of transmission. Key objectives are to describe how microbes penetrate host defenses, cause illness, and are diagnosed and treated. The document provides overviews of microbial cell structures, staining techniques to identify microbes, and the differences between bacteria, fungi, parasites, and viruses. It also outlines the basic stages of infection and methods of disease transmission between individuals and populations.