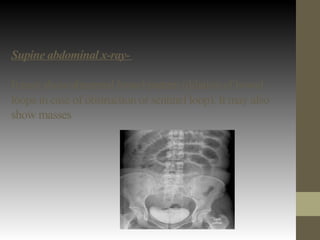
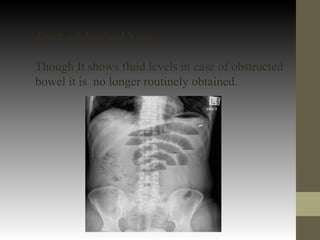
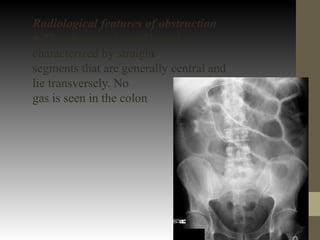
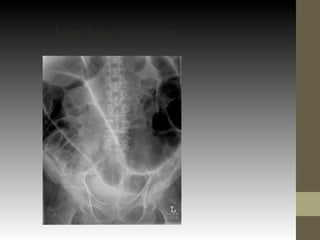
This document provides guidance on the emergency management of intestinal obstruction. It outlines the initial steps of airway, breathing and circulation management. It describes signs of airway obstruction and interventions like endotracheal intubation. It emphasizes fluid resuscitation to treat dehydration from vomiting and recommends nasogastric decompression. The document also differentiates between simple and strangulated obstructions and indications for emergency surgery, like perforation or irreducible hernia.