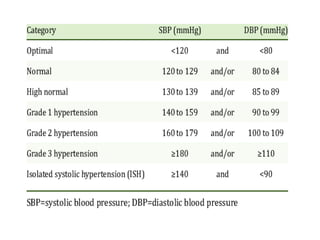
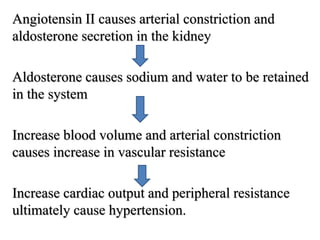
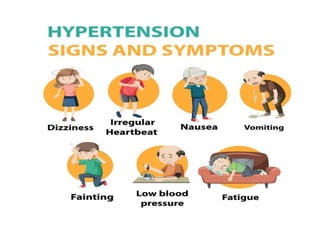
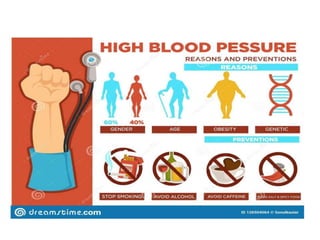
The document discusses the history, diagnosis, and management of hypertension. It notes that Stephen Hales first measured blood pressure in 1733. An estimated 1.28 billion people worldwide have hypertension, with two-thirds living in low- and middle-income countries. Risk factors include age, family history, obesity, physical inactivity, excessive alcohol consumption, and certain medical conditions. Treatment involves lifestyle modifications like diet, exercise and weight loss, as well as medications like diuretics, ACE inhibitors, calcium channel blockers, and beta blockers. Nursing care focuses on assessing symptoms, educating patients, monitoring blood pressure, and supporting lifestyle changes and medication adherence.