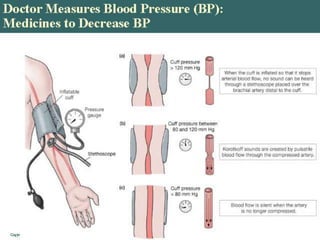
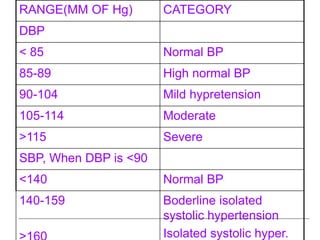
Hypertension, or high blood pressure, is defined as a systolic pressure above 140 mm Hg or a diastolic pressure above 90 mm Hg. It is a major public health problem affecting over 60 million Americans. Risk factors include family history, age, gender, ethnicity, stress, obesity, high sodium diet, and low calcium intake. Uncontrolled hypertension can lead to stroke, heart attack, and other cardiovascular diseases. Treatment involves lifestyle modifications and medication to prevent complications from this chronic condition.













































![Drugs
Diuretics:-
Thiazide and Related to sulfonamides
[Chlorothiazide, Methyclothiazide, Metolazone]
Action [Promote renal excretion of sodium,
water, and potassium. }](https://image.slidesharecdn.com/hypertensionfinal-200426030613/85/Hypertension-52-320.jpg)
![Drugs
Loop Diuretics [frusemide (Laxis), Bumetadine
(bumex)]
Action [Comparable to thiazides, Act on loop of,
Henle to minimize sodium and water
reabsorption]
Potassium-Sparing Diuretics [ (Aldactone),
Triamterene (Dyrenium)]
Action [Block action of aldosterone in distal
loop, promoting excretion of sodium and water
and retention of potassium. ]](https://image.slidesharecdn.com/hypertensionfinal-200426030613/85/Hypertension-53-320.jpg)










































