Fractures and Dislocations. Of joints pptx
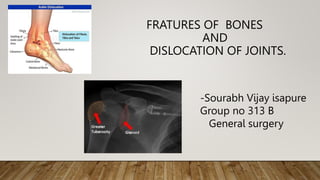
- 1. FRATURES OF BONES AND DISLOCATION OF JOINTS. -Sourabh Vijay isapure Group no 313 B General surgery
- 2. FRACTURES • Fracture is a break or interruption in the continuity of a bone ,which is caused by mechanical exposure (trauma) or pathology (trauma)
- 3. CLASSIFICATION OF FRATURES. (BASED ON ORIGIN) 1. Congenital (intrauterine) 2. Acquired. • Congenital: Fratures mostly multiple,due to change in fetal bones or maternal abdominal trauma during pregnancy.. • Acquired: :Further they are subdividedinto traumatic and pathological ones..obstetric fracture occur during delivery
- 4. BASED ON ORGAN OR TISSUE DAMAGE 1. Complicated 2. Non-complicated • Complicated (open): fratures are those with local damage to the skin a subcutaneous fat ,which allow microorganisms to enter the wound and cause inflammation. • Fracture their also damage to major vessels,neural trunk,(eg:lung , pelvic organ,brain and spinal cord) • closed fracture lack skin defect
- 5. FRACTURE BASED ON LOCATION (FRACTURE LINE.) • Diaphyseal: fracture happens near the centre of thigh bone. • Epiphyseal: fracture that affects the growing part of child’s bone. • Metaphyseal: fracture that occurs in the metaphysis,near wider part of bone near the growth plate.
- 6. FRACTURE BASED ON LONGITUDINAL AXIS OF BONE • Transverse: In this fracture ,fracture line is perpendicular to the long axis of bone.such fracture is caused by tapping or bending force. • Oblique fracture: In this fracture ,fracture line is oblique.such fracture is caused by bending force which ,additional has component along the long axis of bone. • Spiral fracture:In this fracture ,fracture line runs spirally in more than one plain. Such fracture is caused by primarily twisting force.
- 7. FRACTURE ON THE BASIS OF COMPLEXITY OF TREATMENT: 1. Simple fracture:A fracture in two pieces , usually easy to treat is called simple fracture. Eg :transverse fracture of humerus. 2. complex fracture:A fracture in multiple pieces, usually difficult to treat. Is called complex fracture eg :communited frature of tibia.
- 8. FRACTURE BASED ON ETIOLOGY: 1. Traumatic fracture: Fracture sustained due to trauma is called a traumatic fracture. Normal bone can withstand considerable force ,and breaks only when subjected yo excessive force. Most fractures seen in day –to –day practice fall into the category eg :fractures caused by a fall,road traffic accident ,fight etc.
- 9. 2.PATHOLOGICAL FRACTURE • A fracture through a bone which has been made weak by some underlying diseses is called a pathological fracture.eg a fracture through a bone weakened by metastasis.
- 10. 3.STRESS FRACTURE • This is special type of fracture sustained due to chronic repetitive injury(stress) causing a break in bony trabeculae. • They often present as only pain and may not be visible on x –rays.
- 11. FRACTURE ON THE BASIS WITH EXTERNAL ENVIRONMENT . • 1.Closed fracture: A fracture not communicating with the external environment, ie,the overlying skin and other soft tissues are intact ,is called a closed fracture • 2.open fracture: A fracture with break in the overlying skin and soft tissue,leading to the fracture communicating with the external environment, is called open fracture. • A fracture may be open from within or outside so called internally orexternally open fracture
- 12. SIGNS OF FRACTURES: • Probable signs of fractures are as follows:pain and tenderness,swelling,deformity and dysfunction. • Pain is an indispensable symptom localised,as a rule ,at the fracture site; it progresses on an attempt to move the limb.Firm but careful palpation with one finger away from the expected fracturesite helps find out tenderness.Tenderness localised at one site is an important sign. • Swelling may be due to bleeding ,haematoma,blood or lymphy circulatory defect.
- 13. • Deformation of the limb is elucidated on examination and depends on the angular displacements of the bone fragments.The limb can either be distorted or shortened. The distal end of the limb can be turned to either side(rotational displacement). • Pathological movements are a reliable sign of a fracture. They must be assessed very carefully and gently so as not to cause further damage to the adjacent tissues and organs by the bond fragment.
- 14. INSPECTION OF FRATURES: • Measurements and palpation of the limb help determine the location or displacement of the bone fragments. • The rotation of the distal end of a limb without a change in it’s length is indicative of a rotational displacement of fragments. • Lengthening or shortening of limb may be found in displacement along it’s length. • Change in the axis of the limb, i.e an angular twist at the fracture site at an angle is indicative of an axial (angular)displacement and finally an increase in the lamb’s size the limb suggests a transverse displacement. • The exact type of the fracture and location of bone fragments of afracture are established with xray pictures that are taken jn two views.
- 15. CONSERVATIVE TREATMENT OF FRACTURES. • Conservative methods are commonly used to treat fracture. • In both Conservative and surgical treatment of fractures the three main principles have to be followed. 1. Reposition of bone fragments; 2. Immobilisation of repositioned bone fragments: 3. Use of agents and physical methods that promote formation of new bone callus and bone consolidation.
- 16. The successful repositioning of bone fragments is achieved with adequate analgesia,which removes the reflective muscle contraction. Anaesthesia in fracture cases is achieved by injecting solutions of novocain,idocaine, or trimecain into the haematoma at the fracture site.
- 17. Repositioning of displaced bone splinters involves their accurate resetting of bone fragments along the fracture line to provide for further consolidation. The outcome of treatment will be restoration of limb function,which mainly depends on the accuracy of repositioning.
- 18. IMMOBILISATION WITH PLASTER OF PARIS (POP) • In the Conservative treatment of fractures,the pop is widely used; it is the best material for external fixation of fracture fragments and limb immobilisation. • The pop is widely used both as a separate method of treating fractures and also to provide additional immobilisation on metal osteosynthesis and to prolong immobilisation following the removal of traction • The Pop (Calcium sulphate) consists of tiny powder ,which on mixing with water forms Porridge like mass that hardens within several minutes.
- 19. WHEN APPLYING THE POP ,SPECIFIC REGULATIONS ARE TO BE FOLLOWED • The limb must be placed in a functional position. • Bone fragments must be repositioned properly, the limb which being held firm during application of pop until it hardens; • The pop bandage must be applied to cover the two neighbouring jionts; • Finger or toe tips must be left uncovered. • Cotton wools pads (non-hygroscopic type ,which is more elastic and does not get soaked with sweat)must be placed under bone projection; • Pop must be well moulded and put evenly but it should not compress any underlying part of body. • After application a pop bandage must be marked:the date of fracture ,the date of application and supposed date of its removal are noted down on the popbandage
- 21. METHODS OF CONSTANT TRACTION:- • This method ensures both reposition and maintenance of the repositioned fragments. • It’s variants are skin and skeletal traction • Traction has to be done with the limb in median physiologic position ,I.e there should be equilibrium between antagonist muscles. • Resetting has to be done along the axis of Central bone fragments. • The weight for traction has yo be added gradually, which provides a painless traction on the muscles and reposition of fragments • It is necessary to establish a ciuntertraction,which is achieved for eg raising the foot end of bed treating lower limb fractures.
- 22. SKELETAL TRACTION • To perform skeletal traction following set of sterile instruments is required: • Kirschner’s wires or extension wires for skeletal traction , a special hand or electric drill for passing of wire • Wires are passed in operating theatre. • After anasthetising fracture site the patient limb is placed on a therapeutic Bohler’s splint. • Operative field is cleansed according to the generally accepted principle and site locally anaesthetised:skin is infiltrated with 0.5 % novocain first at the entry site and later at the site of exist
- 23. OPEN REPOSITION OF FRACTURES. • There are absolute and relative indication for surgical treatment of fractures. 1. The absolute indications are as follows: • Open fractures • Bone fragments damaging vital organs • Interpolation of soft tissue • Pseudoarthrosis 1. The relative indications : • Failure to reset bone fragments • Delayed bone consolidation • Transverse fracturevof long bone roads • Imperfectly United fracture with moderate organ dysfunction. 1.
- 24. DISLOCATIONS • Dislocation is a complete displacement of the joint ends of b relation to each other. • Partial dislocation may also occur. • Shoulder dislocation is one of the common types (50-60% of dislocation)
- 25. CLASSIFICATION OF DISLOCATIONS: • Dislocation are divided into congenital and acquired. • Acquired on other hand is subdivided into traumatic and pathologic. • Complicated and non complicated • Open and closed. • Habitual (repeated dislocations in one particular jiont )are also identifies.
- 26. MANAGEMENT OF DISLOCATION: • Patients usually complains of severe pain in the affected jionts and are unable to make any active or passive movements as an attempt cause extreme pain . • On inspection: deformation at the jiont region and atypical active movement is impossible, there is shortening of limb and limb axis • On palpation, there is tenderness at the joint ,occasionally joint end can even be palpation in abnormal position only. • X –ray is used confirm . • the diagnosis of dislocation and helps to determine exact position of joint surfaces
- 27. TREATMENT OF DISLOCATION • Treatment of a dislocation or subluxation depends upon it’s type, • Acute traumatic dislocation :In acute traumatic dislocation ,an urgent reduction of dislocation is of paramount importance • Often, it is possible to do so by Conservative methods ,although sometimes operative reduction may be required. • THE TREATMENT OF TRAUMATIC DISLOCATIONS INVOLVES 3 STAGES. • 1 Reduction • 2. immobilisation of the limb. • 3.Restoration of function.
- 28. DISLOCATION OF ELBOW JOINTS: • A characteristics sign is the projection of the olecranon (posterior dislocation).or the block of the humerus (anterior dislocation).To reduce a posterior dislocation the assistart pulls on the forearm flexed at right angles. In anterior dislocation, a big towel is applied and pulled along the axis of the humerus ,trying to pull th olecranon over the humeral block .A click sound indicates a successful reduction
- 29. HIP DISLOCATION: Hip dislocation : This is characterised by the general clinical symptoms of joint dislocation with the typical positioning of the limb. Reduction is achieved by using the Kocher’s method under general anaesthesia. The doctor holds the shin flexed in the knee joint at right angles, and strongly pulls the thigh upwards rotating it laterally at the same time
- 30. Dislocation of the shin : is accompanied by dam- age to the ligaments of the joint and characterised by a typical positioning of the shin. Reduction of this type of dislocation is done under general ana- esthesia by pulling on the limb along its length. Af- ter reduction, the POP bandage is applied to cover the limb from the ankle to the mid-third ofthe thigh. If it is not possible to reduce this type of dislocation in such a way, it means there is interposition of soft tissues or bone fragments in the joint, which is an indication for emergency surgery, i.e. open reduc- tion of the dislocation.
- 31. tibia