A 45-year-old male presented with fever, abdominal pain, and jaundice. Examination found tender hepatomegaly. Tests found elevated inflammatory markers and mildly abnormal liver enzymes. Imaging showed a large abscess in the right lobe of the liver. Needle aspiration yielded anchovy paste-like pus. Given the patient's history, physical exam findings, and imaging results, he was diagnosed with amoebic liver abscess. He was treated medically and surgically with drainage but later developed complications of sepsis and a right pleural effusion, which also resolved with treatment. Amoebic liver abscess most commonly presents as this case outlines.























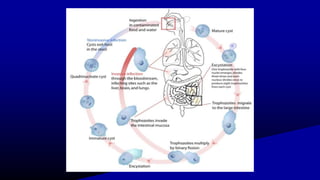
![AMEBIC LIVER ABSCESS
• Amebic liver abscess is the most common extraintestinal
manifestation of amebiasis caused by protozoa Entamoeba
histolytica.
• Is 7 to 10 times more common among adult men.
• seen in the fourth and fifth decades of life .
Risk factor includes
• Immigrants from endemic areas(India, Africa, Mexico, and parts of
Central and South America)
• Homeless person and those living in shelter homes
• People living in crowded places and poor hygiene
• Immunocompromised persons (eg, human immunodeficiency virus [HIV]
infection, malnutrition with hypoalbuminemia, chronic infections, post
traumatic splenectomy, steroid use)](https://image.slidesharecdn.com/finalcpcamoebicliverabscess-230716050103-9bd09642/85/Final-CPC-Amoebic-Liver-Abscess-pptx-25-320.jpg)