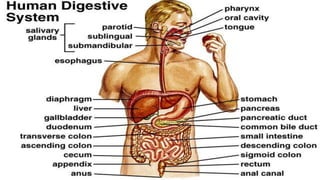
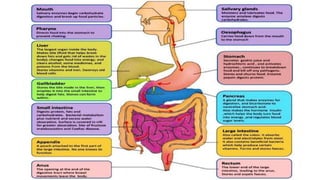
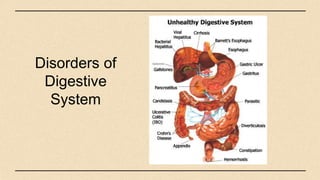
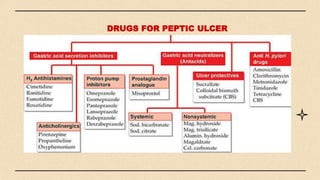
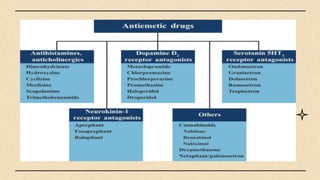
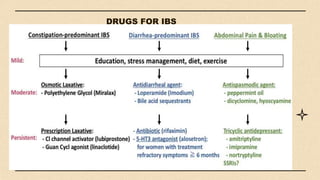
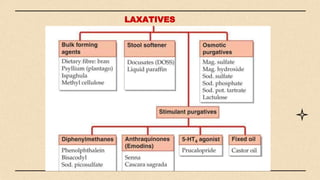
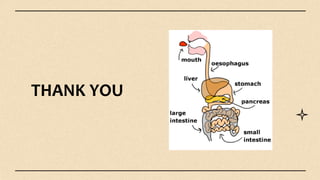
The digestive system consists of organs involved in food breakdown, regulated by specialties like gastroenterology and proctology. Major components include accessory organs and the gastrointestinal tract, with vital processes such as digestion, absorption, and elimination. Common disorders range from peritonitis to conditions like gastroesophageal reflux disease and peptic ulcers, each with distinct symptoms and treatments.