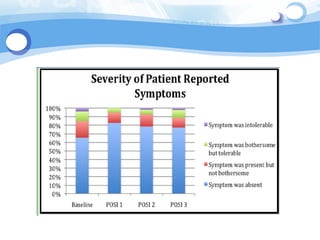
The document discusses an open-source electronic health record (EHR) system called Oscar and describes its architecture and features. It provides examples of how Oscar has been used in radiotherapy settings and primary care clinics. The document also discusses a personal health record (PHR) module called MyOSCAR that is integrated with Oscar. MyOSCAR allows patients to access and share their health records. Two pilot studies are summarized that examine the use of MyOSCAR for blood pressure management and collecting drug safety data from patients. The studies found high completion rates of tasks in MyOSCAR and positive feedback from patients wishing to continue using the application.























![Study Design & Methodology
Design Pilot randomized controlled trial; wait list control
group
Survey: QUAL and QUAN data
Study Length 3 months
Recruitment site McMaster Primary Health Centre
Inclusion criteria Between 40 to 79 years of age
Diagnosis of hypertension
Elevated office BP reading in past 12 months (SBP
≥140 mmHg [or ≥130 mmHg if diagnosed with
diabetes])
Regular access to email / internet
Exclusion criteria Patients with MyOSCAR account](https://image.slidesharecdn.com/definitvaehr-130308090429-phpapp02/85/Definitva-ehr-25-320.jpg)