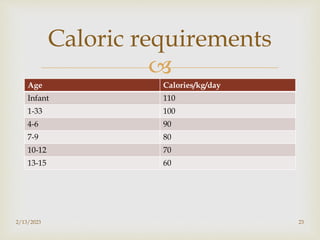
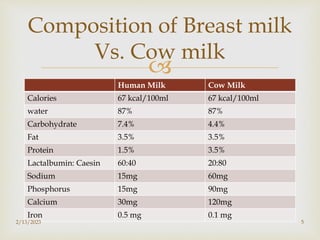
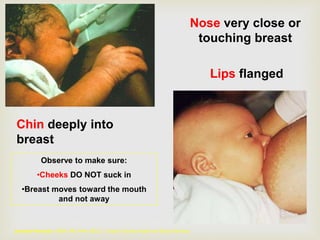
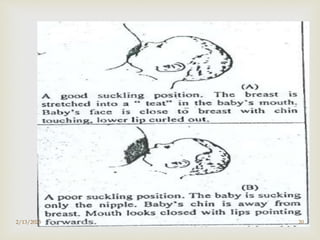
The document discusses breastfeeding and complementary feeding recommendations for infants and children. It provides guidelines on exclusive breastfeeding for the first 6 months, continued breastfeeding with solid foods introduced between 6-24 months, and assessing adequate breastfeeding. The document also outlines potential feeding problems in the first year like underfeeding, overfeeding, and colic, and recommends introducing cereals, fruits and vegetables between 6-8 months as complementary foods.