6.viral hepatitis
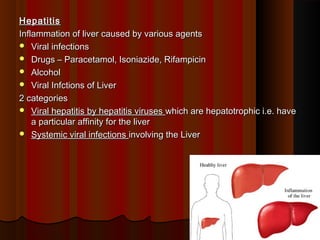
- 1. HepatitisHepatitis Inflammation of liver caused by various agentsInflammation of liver caused by various agents Viral infectionsViral infections Drugs – Paracetamol, Isoniazide, RifampicinDrugs – Paracetamol, Isoniazide, Rifampicin AlcoholAlcohol Viral Infctions of LiverViral Infctions of Liver 2 categories2 categories Viral hepatitis by hepatitis virusesViral hepatitis by hepatitis viruses which are hepatotrophic i.e. havewhich are hepatotrophic i.e. have a particular affinity for the livera particular affinity for the liver Systemic viral infectionsSystemic viral infections involving the Liverinvolving the Liver 11
- 2. Viral HepatitisViral Hepatitis Infection of liver almost always by one or other of the hepatitis virusInfection of liver almost always by one or other of the hepatitis virus The hepatotropic viruses includeThe hepatotropic viruses include - Hepatitis A (HAV),- Hepatitis A (HAV), - Hepatitis B (HBV),- Hepatitis B (HBV), - Hepatitis C (HCV),- Hepatitis C (HCV), - Hepatitis D (HDV), and- Hepatitis D (HDV), and - Hepatitis E (HEV).- Hepatitis E (HEV). Non hepatotropic virusesNon hepatotropic viruses - Epstein-Barr virus,- Epstein-Barr virus, - Cytomegalovirus,- Cytomegalovirus, - Herpes virus,- Herpes virus, - Measles,- Measles, - Rubella, and others.- Rubella, and others. 22
- 3. DefinitionsDefinitions Acute viral hepatitisAcute viral hepatitis is defined by the sudden onset of significant aminotransferaseis defined by the sudden onset of significant aminotransferase elevation as a consequence of diffuse necroinflammatory liverelevation as a consequence of diffuse necroinflammatory liver injury.injury. Symptoms may be variable.Symptoms may be variable. This condition may resolve or progress to fulminant failure orThis condition may resolve or progress to fulminant failure or chronic hepatitis.chronic hepatitis. Chronic viral hepatitisChronic viral hepatitis is defined as the presence of persistent (at least 6 months)is defined as the presence of persistent (at least 6 months) necroinflammatory injury that can lead to cirrhosis.necroinflammatory injury that can lead to cirrhosis. (Symptomatic, biochemical, serological & histological evidence of(Symptomatic, biochemical, serological & histological evidence of continuing or relapsing hepatic disease for more than 6 months)continuing or relapsing hepatic disease for more than 6 months) 33
- 4. 44
- 5. Hepatits A VirusHepatits A Virus HAV is the most common cause of viral hepatitis worldwide.HAV is the most common cause of viral hepatitis worldwide. Mode of TransmissionMode of Transmission HAV infection is usually transmitted via the fecal-oral route.HAV infection is usually transmitted via the fecal-oral route. Fecal shedding continues for 3 weeks before & 1 week after the onsetFecal shedding continues for 3 weeks before & 1 week after the onset of jaundiceof jaundice The period of greatest infectivity is 2 weeks before the onset ofThe period of greatest infectivity is 2 weeks before the onset of clinical illnessclinical illness 55
- 6. Clinical FeaturesClinical Features HAV can be silent (subclinical), especially in children and youngHAV can be silent (subclinical), especially in children and young adults. Symptoms vary from mild illness to fulminant hepatic failureadults. Symptoms vary from mild illness to fulminant hepatic failure (FHF). Malaise, fatigue, pruritus, headache, abdominal pain,(FHF). Malaise, fatigue, pruritus, headache, abdominal pain, myalgias, arthralgias, nausea, vomiting, anorexia, and fever aremyalgias, arthralgias, nausea, vomiting, anorexia, and fever are common but nonspecific symptoms.common but nonspecific symptoms. Physical examination may reveal jaundice, hepatomegaly, and inPhysical examination may reveal jaundice, hepatomegaly, and in rare cases lymphadenopathy, splenomegaly, or a vascular rash.rare cases lymphadenopathy, splenomegaly, or a vascular rash. 66
- 7. Diagnosis – Serum markers for HAVDiagnosis – Serum markers for HAV The diagnosis of acute HAV is made by the detection ofThe diagnosis of acute HAV is made by the detection of IgMIgM anti-anti- HAV antibody. (appears at onset of symptoms)HAV antibody. (appears at onset of symptoms) The recovery phase and immunity phase are characterized byThe recovery phase and immunity phase are characterized by IgGIgG anti-HAV antibody.anti-HAV antibody. 77
- 8. Clinical CourseClinical Course It is a benign self limited diseaseIt is a benign self limited disease Almost all cases of acute HAV hepatitis will resolve in 4-6 weeks.Almost all cases of acute HAV hepatitis will resolve in 4-6 weeks. Acute liver failure is relatively rare, but risk increases with age: 0.1%Acute liver failure is relatively rare, but risk increases with age: 0.1% in patients younger than 15 years old to >1% in patients older thanin patients younger than 15 years old to >1% in patients older than 40 years old.40 years old. HAV does not induce chronic hepatitis or cirrhosis.HAV does not induce chronic hepatitis or cirrhosis. 88
- 9. TreatmentTreatment No specific treatment is available.No specific treatment is available. Supportive treatment is recommended.Supportive treatment is recommended. Liver transplantation may be an option for FHF.Liver transplantation may be an option for FHF. 99
- 10. Hepatitis B VirusHepatitis B Virus HBV causes 60%-80% of hepatocellular carcinoma worldwide.HBV causes 60%-80% of hepatocellular carcinoma worldwide. Mode of TransmissionMode of Transmission • Parenteral routes (e.g., needlestick injury, injection drug use, andParenteral routes (e.g., needlestick injury, injection drug use, and transfusion)transfusion) • Sexual contactSexual contact • Vertical or perinatal transmission (from mother to infant)Vertical or perinatal transmission (from mother to infant) 1010
- 11. Clinical FeaturesClinical Features Acute hepatitis BAcute hepatitis B Can be silent (subclinical), especially in children and young adults.Can be silent (subclinical), especially in children and young adults. Symptoms vary from mild illness to FHF. Malaise, fatigue, pruritus,Symptoms vary from mild illness to FHF. Malaise, fatigue, pruritus, headache, abdominal pain, myalgias, arthralgias, nausea, vomiting,headache, abdominal pain, myalgias, arthralgias, nausea, vomiting, anorexia, and fever are common but nonspecific symptoms.anorexia, and fever are common but nonspecific symptoms. Chronic hepatitis BChronic hepatitis B Runs an indolent course, sometimes for decades. Fatigue is aRuns an indolent course, sometimes for decades. Fatigue is a common symptom. The disease may only become clinicallycommon symptom. The disease may only become clinically apparent late in the natural course, when symptoms typically seenapparent late in the natural course, when symptoms typically seen in end-stage liver disease (ESLD) appear.in end-stage liver disease (ESLD) appear. Extrahepatic manifestations include polyarteritis nodosa,Extrahepatic manifestations include polyarteritis nodosa, glomerulonephritis, cryoglobulinemia, serum sickness like illness,glomerulonephritis, cryoglobulinemia, serum sickness like illness, papular acrodermatitis (predominantly in children), and aplasticpapular acrodermatitis (predominantly in children), and aplastic anemia.anemia. 1111
- 12. HBVHBV - Serum markers of HBV are:- Serum markers of HBV are: AntigensAntigens HBsAg - Done routinely. It appears before the onset of symptoms &HBsAg - Done routinely. It appears before the onset of symptoms & peaks during overt diseasepeaks during overt disease in 3 – 6 months it is usually undetectablein 3 – 6 months it is usually undetectable HBcAg is not found in serumHBcAg is not found in serum HBeAg appears shortly after HBsAg in the serumHBeAg appears shortly after HBsAg in the serum Rises early & declines rapidlyRises early & declines rapidly Its persistence is indicative of Chronic liver diseaseIts persistence is indicative of Chronic liver disease 1212
- 13. AntibodiesAntibodies Anti -HBsAnti -HBs (IgG)(IgG) appears after the disappearance of HBsAg (3-6appears after the disappearance of HBsAg (3-6 months) and after vaccination. Persists for many years or perhapsmonths) and after vaccination. Persists for many years or perhaps permanently. Anti-HBs implies either a previous infectionpermanently. Anti-HBs implies either a previous infection Anti - HBcAgAnti - HBcAg (IgM anti-HBc) - appears early and rapidly reaches(IgM anti-HBc) - appears early and rapidly reaches a high titre which then subsides gradually. Anti-HBc is initially of IgMa high titre which then subsides gradually. Anti-HBc is initially of IgM type with IgG appearing later.type with IgG appearing later. Suggests an acute & continuing viral replicationSuggests an acute & continuing viral replication Anti-HBeAnti-HBe usually indicates low-level replication and a lower degreeusually indicates low-level replication and a lower degree of infectivity.of infectivity. 1313
- 14. 1414
- 15. 1515
- 16. 1616
- 17. Clinical CourseClinical Course • Incubation period after HBV infection ranges from 30-160 days.Incubation period after HBV infection ranges from 30-160 days. • Depending on the age of the person at infection, people may haveDepending on the age of the person at infection, people may have spontaneous resolution or progression to chronicity.spontaneous resolution or progression to chronicity. – Children younger than 5 years old: 90% will develop chronicChildren younger than 5 years old: 90% will develop chronic HBV infection.HBV infection. – Adults: 5% - 10% will develop chronic HBV.Adults: 5% - 10% will develop chronic HBV. • Chronic hepatitis BChronic hepatitis B – Spontaneous clearance of HBsAg occurs in 1% of patientsSpontaneous clearance of HBsAg occurs in 1% of patients annually.annually. – Thirty percent progress to cirrhosis.Thirty percent progress to cirrhosis. – Five to ten percent progress to HCC with or without precedingFive to ten percent progress to HCC with or without preceding cirrhosis. The risk of HCC is dependant on the degree of viralcirrhosis. The risk of HCC is dependant on the degree of viral replication.replication. 1717
- 18. Hepatitis C VirusHepatitis C Virus Modes of TransmissionModes of Transmission Parenterally (e.g., transfusion, injection drug use,Parenterally (e.g., transfusion, injection drug use, needlestick injury)needlestick injury) Sexually and from mother to offspring, although at aSexually and from mother to offspring, although at a much lower frequency than HBVmuch lower frequency than HBV 1818
- 19. Clinical FeaturesClinical Features Acute hepatitisAcute hepatitis Can be silent (subclinical), especially in children and young adults.Can be silent (subclinical), especially in children and young adults. Symptoms vary from mild illness to FHF. Malaise, fatigue, pruritus,Symptoms vary from mild illness to FHF. Malaise, fatigue, pruritus, headache, abdominal pain, myalgias, arthralgias, nausea, vomiting,headache, abdominal pain, myalgias, arthralgias, nausea, vomiting, anorexia, and fever are common but nonspecific symptoms.anorexia, and fever are common but nonspecific symptoms. Chronic hepatitisChronic hepatitis Runs an indolent course, sometimes for decades. Fatigue is aRuns an indolent course, sometimes for decades. Fatigue is a common symptom. The disease may only become clinicallycommon symptom. The disease may only become clinically apparent late in the natural course, when symptoms typically seenapparent late in the natural course, when symptoms typically seen in ESLD appear.in ESLD appear. Extrahepatic manifestations include mixed cryoglobulinemia (10%-Extrahepatic manifestations include mixed cryoglobulinemia (10%- 25% of patients with HCV), glomerulonephritis, porphyria cutanea25% of patients with HCV), glomerulonephritis, porphyria cutanea tarda, cutaneous necrotizing vasculitis, lichen planus, lymphoma,tarda, cutaneous necrotizing vasculitis, lichen planus, lymphoma, and other autoimmune disorders.and other autoimmune disorders. 1919
- 20. DiagnosisDiagnosis • Antibodies against HCV (anti-HCV) may be undetectable for the firstAntibodies against HCV (anti-HCV) may be undetectable for the first 8 weeks after infection.8 weeks after infection. • HCV RNA can be detected serum 1-3 weeks.HCV RNA can be detected serum 1-3 weeks. • Positive tests are usually diagnostic in patients with elevated liverPositive tests are usually diagnostic in patients with elevated liver enzymes and with risk factors for the infection.enzymes and with risk factors for the infection. • The antibody does not confer immunity.The antibody does not confer immunity. • It determines the presence of actual virus and ongoing infection.It determines the presence of actual virus and ongoing infection. 2020
- 21. 2121
- 22. 2222
- 23. Clinical CourseClinical Course The incubation period is 15-150 days.The incubation period is 15-150 days. Acute hepatitis is frequently clinically silent.Acute hepatitis is frequently clinically silent. Fifteen percent of people infected with HCV will have spontaneousFifteen percent of people infected with HCV will have spontaneous resolution.resolution. Chronic HCV will occur in 85% of infected people.Chronic HCV will occur in 85% of infected people. Progression to cirrhosis is slow (two to three decades) and is seenProgression to cirrhosis is slow (two to three decades) and is seen in a quarter of patients with chronic HCV.in a quarter of patients with chronic HCV. HCC develops in approximately 1%-2% of patients per year, andHCC develops in approximately 1%-2% of patients per year, and rarely occurs in the absence of cirrhosis.rarely occurs in the absence of cirrhosis. 2323
- 24. Hepatitis D VirusHepatitis D Virus HDV is a small RNA virus with an envelope consisting of HBsAg.HDV is a small RNA virus with an envelope consisting of HBsAg. High-risk groups are similar to HBVHigh-risk groups are similar to HBV HDV infection clinically presents as aHDV infection clinically presents as a Coinfection (acute hepatitis B and D),Coinfection (acute hepatitis B and D), as a superinfection (chronic hepatitis B with acute hepatitis D),as a superinfection (chronic hepatitis B with acute hepatitis D), or as a latent infection (e.g., in the liver transplant setting).or as a latent infection (e.g., in the liver transplant setting). 2424
- 25. DiagnosisDiagnosis Is made by finding HDV RNA or HDV antigen in serum or liver andIs made by finding HDV RNA or HDV antigen in serum or liver and by detecting antibody to the HDV antigen.by detecting antibody to the HDV antigen. 2525
- 26. Clinical courseClinical course In patients with co infection, the course is transient and self-limited.In patients with co infection, the course is transient and self-limited. The rate of progression to chronicity is similar to the one reportedThe rate of progression to chronicity is similar to the one reported for acute HBV.for acute HBV. In superinfection, the HBV carriers may present with a severe acuteIn superinfection, the HBV carriers may present with a severe acute hepatitis exacerbation with frequent progression to chronic HDVhepatitis exacerbation with frequent progression to chronic HDV infection.infection. INF-1 is the treatment of choice for chronic hepatitis D.INF-1 is the treatment of choice for chronic hepatitis D. HBV vaccine can prevent HDV infection too.HBV vaccine can prevent HDV infection too. 2626
- 27. Hepatitis E VirusHepatitis E Virus TransmissionTransmission Closely resembles that of HAV (i.e., fecal-oral route).Closely resembles that of HAV (i.e., fecal-oral route). 2727
- 28. Clinical courseClinical course Acute hepatitis E is clinically indistinguishable from other acute viralAcute hepatitis E is clinically indistinguishable from other acute viral hepatitis.hepatitis. HEV infection is associated with a high fatality rate in pregnantHEV infection is associated with a high fatality rate in pregnant women in the second and third trimesters.women in the second and third trimesters. There is no chronic infection associated with HEV.There is no chronic infection associated with HEV. Treatment is supportive.Treatment is supportive. There is not pre- or postexposure prophylaxis.There is not pre- or postexposure prophylaxis. 2828
- 29. Pathogenesis of Infective HepatitisPathogenesis of Infective Hepatitis Direct cytopathic effectDirect cytopathic effect Induction of immune responses against viral antigen that damageInduction of immune responses against viral antigen that damage virally infected hepatocytes.virally infected hepatocytes. Alteration of liver cell antigens and the initiation of an auto immuneAlteration of liver cell antigens and the initiation of an auto immune reaction.reaction. 2929
- 30. Acute Viral Hepatitis - MorphologyAcute Viral Hepatitis - Morphology Early stageEarly stage 3030
- 31. Later Stage & Healing stageLater Stage & Healing stage 3131
- 32. 3232
- 33. MacroscopicallyMacroscopically Liver is slightly enlargedLiver is slightly enlarged More or less green depending on the phase of acute disease &More or less green depending on the phase of acute disease & degree of jaundicedegree of jaundice 3333
- 34. Acute Viral Hepatitis - MicroscopicallyAcute Viral Hepatitis - Microscopically Necrosis is random isolated hepatocytes or even in an entire lobuleNecrosis is random isolated hepatocytes or even in an entire lobule Isolated necrotic hepatocytes appear as eosinophilic rounded upIsolated necrotic hepatocytes appear as eosinophilic rounded up cells (councilman bodies), lymphocytes, macrophages.cells (councilman bodies), lymphocytes, macrophages. Balloning degeneration may be seenBalloning degeneration may be seen Reactive changes in Kuffer’s cells show hyperplasia & InflammatoryReactive changes in Kuffer’s cells show hyperplasia & Inflammatory infiltrate to portal tractinfiltrate to portal tract Evidence of hepatocytes regeration during recovery phaseEvidence of hepatocytes regeration during recovery phase 3434
- 35. Chronic Viral Hepatitis /Chronic hepatitisChronic Viral Hepatitis /Chronic hepatitis Classification – according to extent of inflammationClassification – according to extent of inflammation Chronic persistent hepatitis – confined to portal tractChronic persistent hepatitis – confined to portal tract Chronic active hepatitis – spills into the parenchyma & surroundsChronic active hepatitis – spills into the parenchyma & surrounds regions of necrotic Hepatocytesregions of necrotic Hepatocytes Chronic lobular hepatitis – persistent inflammation is confined to theChronic lobular hepatitis – persistent inflammation is confined to the lobulelobule 3535
- 36. Chronic persistent hepatitisChronic persistent hepatitis Benign self limited relapsing remitting condition occurs as a sequelBenign self limited relapsing remitting condition occurs as a sequel to acute hepatitis (HBV or HBC rarely combined HBV & HDV)to acute hepatitis (HBV or HBC rarely combined HBV & HDV) It is not associated with progressive liver damageIt is not associated with progressive liver damage MorphologyMorphology MacroscopicMacroscopic The liver architecture is normalThe liver architecture is normal MicroscopicMicroscopic Chronic inflammatory infiltrate is limited to the portal tract & does notChronic inflammatory infiltrate is limited to the portal tract & does not spill out into the hepatic parenchymaspill out into the hepatic parenchyma 3636
- 37. Chronic active hepatitis (CAH)Chronic active hepatitis (CAH) Chronic active hepatitis may be defined as chronic necrotizing &Chronic active hepatitis may be defined as chronic necrotizing & fibrosing heptic disease of varied aetiologyfibrosing heptic disease of varied aetiology Seen inSeen in -- HBV, HCV & combined HBD & HDV , Chronic alcoholismHBV, HCV & combined HBD & HDV , Chronic alcoholism 3737
- 38. MorphologyMorphology Liver architecture is lostLiver architecture is lost MicroscopicMicroscopic An exuberrent portal infiltrate that spills out of portal tractAn exuberrent portal infiltrate that spills out of portal tract Piece meal necrosis / interface hepatitisPiece meal necrosis / interface hepatitis Bridging necrosisBridging necrosis Progressive fibrosis extending from portal tract into hepaticProgressive fibrosis extending from portal tract into hepatic parenchyma leading to cirrhosis in many casesparenchyma leading to cirrhosis in many cases 3838
