Prostate diseases
- 1. Presentor: Dr. Ameer Hamza Email. ameerhamza5382@gmail.com
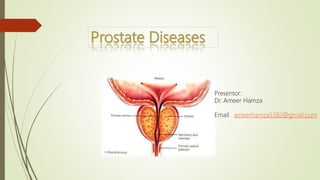
- 2. Anatomy The prostate is a walnut-sized gland located between the bladder and the penis. The prostate is just in front of the rectum. The urethra runs through the center of the prostate, from the bladder to the penis, letting urine flow out of the body. The prostate secretes fluid that nourishes and protects sperm. During ejaculation, the prostate squeezes this fluid into the urethra, and it’s expelled with sperm as semen
- 3. Lateral View
- 4. Zones The prostate gland is divided into : Peripheral zone. Central zone. Transition zone
- 5. Normal Physiology: Glandular cells Smooth muscle cells Stromal cells The prostate gland also contains an enzyme5 alpha-reductase type-2 that converts testosterone to Dihydrotestosterone (morepotent)
- 6. Conditions: Enlarged prostate i.e. Benign prostatic hyperplasia Prostate cancer Prostatitis
- 7. Benign Prostate Hyperplasia: Benign prostatic hyperplasia (BPH) is the enlargement of the gland . As the prostate starts to enlarge it exerts pressure on the walls of the urethra.
- 8. Symptoms Difficult for you to start urination • Weaken the flow of urine • Strain to pass urine • Frequently need to urinate • Wake up frequently during the night to urinate • Sudden urge to urinate • Blood in the urine (haematuria)
- 10. Cont.… Symptoms related to urine voiding from then bladder are the following: Reduction in urine flow and force. Intermittent micturition. Leak of urine drops after the end of micturition Feeling of incomplete bladder voiding. Urine retention. Dribbling
- 11. Etiology The exact etiology of BPH is still poorly Understood. In BPH there is decrease in testosterone level with advancing age but estrogen level does not decrease equally. Inc in estrogen level causes hypertrophy of prostate. DIHYDROTESTOSTRONE is main mediator of BPH.
- 12. Diagnosis: history Physical examination : • digital rectum test • palpate PR Urinalysis Uroflowmetry Cystoscopy Ultrasound prostate Specific Antigen (PSA) Test
- 13. Management • Eggs • Milk • Soya • Fish • Cheese • Chicken
- 14. BPH symptoms score: How often have you had a sensation of not emptying your bladder completely after you finished urinating? How often have you had to urinate again less than two hours after you finished urinating? How often have you stopped and started again several times when you urinated? How often have you found it difficult to urinate? How often have you had a weak urinary stream? How often had you had to push or strain to begin urination? How many times did you most typically get up to urinate from the time you went to bed at night until the time you got up in the morning?
- 15. Differential Diagnosis: Prostatitis Bladder obstruction Bladder cancer Neurogenic bladder DRE Elevated PSA Prostatic biopsy Other markers as serum acid phosphatase & serum alkaline phosphatase Plain X-ray spine for metastasis Isotopic bone scan CT scan Cystoscopy
- 16. Treatment Watching waiting Home plan Medications : surgery Radical surgery. Radiotherapy: External or brachytherapy Hormonal therapy: in advanced cases Depends on androgen ablation by: • Bilateral orchiectomy • Oral estrogen • Antiandrogens
- 17. Surgical treatment: • Indications: 1. Recurrent attacks of acute retention 2. Hematuria 3. Recurrent urinary tract infection 4. Bladder stone or diverticula 5. Renal insufficiency
- 18. Prostate Cancer:
- 19. Prostate Cancer: the prostate cancer starts in the gland cells - this is called adenocarcinoma. prostate cancer starts with tiny alterations in the shape and size of the prostate gland cells. Prostatic intraepithelial neoplasia (PIN). Prostatic intraepithelial neoplasia means "dysplastic changes involving glands and ducts of the prostate that may be a precursor of adenocarcinoma.
- 20. Cont… Most prostate cancers are slow growing; however, there are cases of aggressive prostate cancers If the tumor is within the gland, the cancer is said to be localized and curable If the cancer escapes the gland it is considered incurable Early detection before the cancer escapes the gland becomes very important
- 21. Etiology: Age Genetics Faulty BRCA2 gene linked to aggressive. Diet Medication Obesity STDs Agent orange Enzyme PRSS3 linked to aggressive
- 22. Stages: Stage I Stage II Stage III Stage IV
- 23. Symptoms: During the early stages: The patient urinates more often The patient gets up at night more often to urinate He may find it hard to start urinating He may find it hard to keep urinating once he has started There may be blood in the urine Urination might be painful Ejaculation may be painful (less common) Achieving or maintaining an erection may be difficult (less common)
- 24. Symptoms of advanced cancer: Bone pain, often in the spine (vertebrae), pelvis, or ribs The proximal part of the femur can be painful Leg weakness (if cancer has spread to the spine and compressed the spinal cord) Urinary incontinence (if cancer has spread to the spine and compressed the spinal cord) Fecal incontinence (if cancer has spread to the spine and compressed the spinal cord)
- 25. Complications: Metastasis Incontinence Erectile dysfunction Metabolic factors
- 26. Diagnosis: PSA test blood test Prostate biopsy Trans rectal ultrasound Bone scan CT MRI ProstaScint scan
- 27. Medications: Medication Watchful waiting Prostatectomy Radiation placed inside your body (brachytherapy) Radiation that comes from outside of your body (external beam radiation) Hormonotherapy Chemotherapy Freezing prostate tissue Heating prostate tissue using Ultrasound cryotherapy
- 28. Cont… First line of defense against bothersome urinary symptoms Two major types: α blockers - relax the smooth muscle of prostate and provide a larger urethral opening (Hytrin,Doxaben,Harnalidge) 5 α reductase inhibitor – Shrink the prostate gland (Proscar,Avodart)
- 29. Medication Benefits Convenient No loss of work time Minimal risk Disadvantages Drug Interactions Must be taken every day Manages the problem instead of fixing it
- 30. Medication Possible side effects of medication • Impotence • Dizziness • Headaches • Fatigue • Loss of sexual drive
- 31. Prostatitis: Prostatitis is inflammation caused by an infection of the prostate. Treated with antibiotics
- 32. Etiology A bacterial infection is only sometimes responsible. • In many cases of chronic (long-term) prostatitis, doctors can't find any infection in the prostate gland, In these cases, the cause is poorly understood. • Chronic prostatitis is thought to be caused by a number of suggested factors, including partial blockage of the flow of urine and underlying problems with the immune system, pelvic floor or nervous system.
- 33. Symptoms: Pain in the pelvis, genitals, lower back and buttocks • Pain when urinating • Frequent need to urinate • Difficulty urinating, such as problems starting or 'stopstart‘ urination • Pain when ejaculating, which may contribute to erectile dysfunction • Discomfort in the perineal area (the area between the scrotum and the anus)
- 34. Diagnosis: Acute Prostatitis • Rectal examination. Chronic Prostatitis • Blood tests. • Ultrasound scan or ct scan • Cytoscope
- 35. Treatment: Acute Prostatitis • Antibiotic tablets • Paracetamol and/or ibuprofen • Codeine Chronic Prostatitis • Antibiotics • Alpha blockers
- 36. Etiology Age • Ethnic group • Family history • Obesity • Exercise • Diet
- 37. Symptoms Urinate more frequently, often during the night • Needing to rush to the toilet • Difficulty in starting to urinate • Straining long time while urinating • Feeling that your bladder has not emptied fully
- 38. Diagnosis Ask for a urine sample to check for infection • Take a blood sample to test your level of prostate-specific antigen (PSA) • Examine your prostate (digital rectal examination) • Gleason score • Biopsy