Cushing Syndrome and Pheochromocytoma: Signs, Symptoms, and Treatment
- 2. CUSHING SYNDROME • It is characterized by excess cortisol secretion resulting from too much ACTH by pituitary. • More in women of 20- 40 yrs
- 3. Cushing’s disease Cushing’s syndrome Hypersecretion of ACTH. (disease) Hypersecretion of ACTH by the anterior pituitary-causes increased release of both cortisol and androgenic hormones Hypersecretion of Cortisol. (syndrome) … too much cortisol secreted by the adrenal cortex organ itself
- 4. Causes Prolonged use of corticosteroid medicines Excess production of corticosteroid by adrenal cortex.- in adrenal tumor Pituitary tumor- excess ACTH Ectopic production of ACTH by malignancies.- CUSHING DISEASES.
- 5. Cushing’s- clinical manifestations serum glucose levels increased ….(gluconeogenesis) eventually the islet cells of the pancreas cannot produce enough insulin and DM results. Loss of protein stores occurs, muscle wasting Humoral immunity is reduced, decreasing the threshold to infection. Skin tissues lose collagen, and become very thin: tearing and bruising easily.
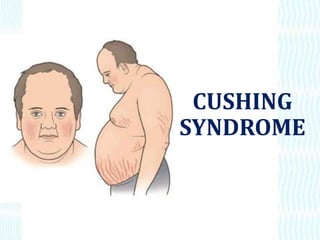
- 6. • Wt. gain • Thin arm and legs . • Moon face –deposit of adipose tissue at these sites. • Kyphosis- backpain, compression fracture of vertebra • Visual disturbance
- 8. Excess body and facial hair growth in women (from excess androgen secretion) Mood swings and psychosis may occur as the effect of excess cortisol on cognitive function. Truncal obesity: results from the mobilization of fat in the lower parts of the body, to the trunk causing the abdomen to become protuberant as the extremities become thin and wasted.
- 9. Purple striae: appear on the abdomen as a result of the stretching of the abdominal skin. They’re purple due to the collagen deficit in the tissues. Round facial features: fat accumulation around the neck and cervical area is termed the buffalo hump.
- 11. DIAGNOSIS A 24 hrs urine test – for Unbound cortisol Dexamethazone test Dexamethasone (1 mg) is administered orally at 11 pm, and a plasma cortisol level is obtained at 8 the next morning. Suppression of cortisol to less than 5 mg/dL indicates that the hypothalamic-pituitary-adrenal axis is functioning properly.
- 12. Management Radiation of the pituitary gland also has been successful, although it may take several months for control of symptoms. Adrenalectomy is the treatment of choice in patients with primary adrenal hypertrophy. K supplement
- 13. Adrenal enzyme inhibitors (eg, metyrapone, aminoglutethimide, mitotane, ketoconazole) may be used to reduce hyperadrenalism. • if the syndrome is caused by ectopic ACTH secretion by a tumor • Surgical removal of pituitary gland . • If due to steroid therapy – taper the dosage
- 14. Nursing Diagnoses • Risk for Infection R/T impaired immune response and tissue repair • Risk of Altered Health Maintenance R/T insufficient knowledge of disease process • Disturbed body image related to altered physical appearance, impaired sexual functioning, and decreased activity level • Risk for Fluid and Electrolyte imbalance
- 15. • DECREASING RISK FOR INJURY • Establishing a protective environment will help to prevent falls, fractures, and other injuries to bones and soft tissues. • DECREASING RISK FOR INFECTION • The nurse frequently assesses the patient for subtle signs of infection because the anti-inflammatory effects of corticosteroids may mask the common signs of inflammation and infection. Therefore, insulin therapy and medication to treat peptic ulcer may be initiated if needed.
- 16. • ENCORAGE REST AND ACTIVITY • the nurse should encourage moderate activity to prevent complications • of immobility and promote increased self-esteem
- 17. • PROMOTING SKIN INTEGRITY • The nurse frequently assesses the skin and bony prominences and encourages and assists the patient to change positions frequently to prevent skin breakdown.
- 18. • IMPROVE BODY IMAGE • Weight gain and edema may be modified by a low-carbohydrate, low-sodium diet, and a high- protein intake may reduce some of the other bothersome symptoms.
- 19. PHEOCHROMACYTOMA
- 20. PHEOCHROMACYTOMA • Pheochromacytoma is a catecholamine secreting tumor of the cromaffin cells of the sympathetic nervous system it is usually found in the adrenal medulla. • Peak at 40 – 50 yrs
- 22. • Pathophysiology • The tumor secrete epinephrine and nor epinephrine in excess amount – leads to life threatening arrhythmia and hypertension. • Increased gluconeogenesis. • Relaxes the bowel.
- 23. Signs and symptoms • Triad of symptoms are • Headache • Diaphoresis • Palpitation • Hypertesion causes face flushing. • Tremor • Anxiety • Wt. loss • Constipation – by catecholamines
- 25. Diagnostic tests • Adrenal biopsy • Catecholamines blood test • Glucose test • Scintiscan- biochemically confirmed cases with MRI doesnot show growth. • MRI of abdomen- to detect adrenal massess
- 26. • Urine catecholamines • Test for metanephrine – metabolite formed frombreakdown of catecholamines.
- 27. Management • Treatment involves removing the tumor with surgery. • It is important to stabilize blood pressure and pulse with medication before surgery.
- 28. • Phenoxybenzamine (Dibenzyline), a long-acting alpha-blocker, may be used when the blood pressure is stable to prepare the patient for surgery. • Beta-adrenergic blocking agents, such as propranolol (Inderal), may be used in patients with cardiac dysrhythmias
- 29. • The definitive treatment is adrenalectomy. Bilateral. • adrenalectomy may be necessary if tumors are present in both glands . • IV administration of corticosteroid .
- 30. Nursing management • The nurse instructs the patient about their purpose, the medication schedule, and the risks of skipping doses or stopping their administration abruptly. • Monitor for hypertensive crisis. • IV lines .
- 31. • Blood specimen – cannula inserted 30 min before sample collection. – stress causes release of catecholamines.
- 32. THANK YOU
