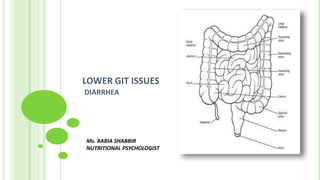
DIARRHEA
- 1. LOWER GIT ISSUES DIARRHEA Ms. RABIA SHABBIR NUTRITIONAL PSYCHOLOGIST
- 2. Introduction Pathophysiology Prevention Treatment Nutritional Assessment Medical Nutrition Therapy 2
- 3. Diarrhea is defined as an increase in frequency of bowel movements and/or an increase in water content of stools that affects either the consistency or the volume of fecal output. Other definitions describe abnormality in stool production as >200 g/day for adults and >20 g/kg for children Passage of 3 or more loose or liquid stools/day (WHO) 3
- 4. CONTD… Acute diarrhea is short-term (less than two weeks), whereas diarrhea lasting longer than four weeks is considered chronic. Diarrhea presents as a change from the normal bowel function. This is generally a watery stool that is increased in frequency. foul-smelling, frothy stools are associated with steatorrhea. 4
- 5. PATHOPHYSIOLOGY Diarrhea maybe related to any of the following conditions: Fungal infections Bacterial infections Viral agents Toxins Medications Excessive consumption of OCD’s Excessive sugar consumption Allergic reactions Inflammatory bowel diseases (Ulcerative collitis & Crohn’s disease) Inflammatory bowel syndrome (IBS) Short bowel syndrome (SBS) 5
- 6. Celiac disease Lactose intolerance Vitamin B12 malabsorption Heavy metal poisoning Gastric resection Endocrine & metabolic syndromes Antibiotics 6
- 8. 1. EXUDATIVE DIARRHEA Always associated with mucosal damage Damaged mucosa causes outpouring of mucus, blood, plasma proteins, electrolytes and water in gut Causes blood and pus in stools sometimes It is commonly associated with E.coli infections and IBDs 8
- 9. 2. OSMOTIC DIARRHEA It occurs when osmotically active solutes are present in intestinal tract Excessive sugar consumption is an example Usually relieved by fasting Lactose intolerance, fructose intolerance, dumping syndrome are classical examples of conditions associated with osmotic diarrhea 9
- 10. 3. SECRETORY DIARRHEA Active secretion of water and electrolytes by intestinal epithelium It can be because of bacterial or viral infections, toxins, increased intestinal hormonal secretions It also occurs due to inhibition of absorption Little or no structural damage to GIT 10
- 11. 4. MALABSORPTIVE DIARRHEA When some disease impairs digestion or absorption of nutrients Fats start appearing in stools “STEATORRHEA” Not enough health absorptive area or inadequate production or interrupted flow of bile and pancreatic enzymes 11
- 12. 5. MEDICATION INDUCED DIARRHEA Hospitalized and long term care patients ROLE OF ANTIBIOTICS Trillions of bacteria are present in gut These are responsible for fermenting the sloughed intestinal cells and undigested food materials into short chain FAs and gases Broad term use of antibiotics causes a decrease in gut bacterial count 12
- 13. Treatment of the underlying disorder is the most important component of therapy. If the diarrhea is infectious in nature, antibiotics will be the first line of treatment. Restoring normal fluid, electrolyte, and acid-base balance is crucial. Intravenous therapy or the use of rehydration solutions. 13
- 14. • Improving access to clean water and safe sanitation • Promoting hygiene education • Exclusive breast-feeding • Improving weaning practices • Immunizing all children, especially against measles • Using latrines • Keeping food and water clean • Washing hands with soap (the baby’s as well) before touching food • Sanitary disposal of stools 14
- 15. When completing the nutrition assessment for a patient with diarrhea, it is especially important to review the following types of assessment data: ◦ Fluid and beverage intake ◦ Energy and mineral intake ◦ Medication and herbal supplement use ◦ Weight change ◦ Biochemical data (reflective of hydration status-mineral content, urine output and color) ◦ Nutrition-focused physical findings (especially those related to the digestive system and skin) ◦ Past surgical history 15
- 16. 16
- 17. Current practice recognizes the importance of stimulating the gastrointestinal tract by feeding the patient. This speeds recovery of damaged cells. In addition, clear liquids are typically high in simple carbohydrates, which increase osmolality of the gastrointestinal tract must be avoided. This actually can make diarrhea worse. Oral rehydration solutions are designed to both restore fluid and electrolyte balance and enhance absorption in the intestinal tract. 17
- 18. Nutrition therapy to decrease motility should focus on avoiding high- sugar beverages and foods high in simple carbohydrates (lactose, sucrose or fructose); sugar alcohols (sorbitol, xylitol, mannitol); caffeine; and alcoholic beverages. Gas-producing foods should be avoided. Adding sources of soluble fiber and resistant starch has been the most typical route to thicken the consistency of the stool. 18
- 19. If the infant has begun solid foods, use of strained bananas, apple sauce, and rice cereal are the best initial food choices. BRAT (bananas, rice, applesauce, and toast [bran]) eating pattern has been used to guide the initial food choices for acute diarrhea, but it does not provide a sufficient variety of nutrients for long periods of use. 19
- 20. ANOTHER STEP IN TREATING DIARRHEA IS THE USE OF PROBIOTICS AND PREBIOTICS. PROBIOTICS FOODS: ◦ Live culture yogurt Prebiotics foods: Any form of carbohydrates (preferably banana) 20
- 21. ORS: COMPOSITION Glucose 20 g/100ml Sodium 90mEQ/L Potassium 20mEQ/L Chloride 80mEQ/L Bicarbonate 30mEQ/L Osmolatrity 330mOsm/L 21
- 22. Medical Nutrition Therapyfor Diarrhea FoodGroup RecommendedFoods FoodsNot Recommended Milk andMilk Products • Buttermilk • Evaporated, skim,andlow-fat milk • Yogurtwith live activecultures • Cheese • Sherbet • Wholemilk •Half-and-half • Cream •Regular(whole milk) ice cream • Yogurtwith berries, dried fruit, ornuts Meat andOtherProtein Foods •Tender,well-cookedmeat, poultry, fish,eggs,or foodsmadewithout addedfat •Friedmeat,poultry, or fish • Sausage • Hot dogs • Fattymeats • Nuts • Chunkynut butters Grains • White flour • Bread,bagels,rolls,crackers,and pastamadefrom white or refinedflour •Coldor hot cerealsmadefrom white or refined flour •Whole-wheat or whole-grainbreads, rolls,crackers,or pasta • Brownor wild rice •Barley,oats,and other wholegrains •Cerealsmadefrom whole grainor bran • Breadsor cerealsmade with seedsor nuts • Popcorn 22
- 23. Medical Nutrition Therapyfor Diarrhea FoodGroup RecommendedFoods FoodsNot Recommended Vegetables •Most well-cookedvegetables without seedsor skins • Potatoeswithout skin • Lettuce • Strainedvegetable juice •Rawvegetables (exceptfor lettuce) • Friedvegetables • Beets • Broccoli • Brusselssprouts • Cabbage • Cauliflower • Turnipgreens • Corn • Potatoskins Fruits • Fruit juicewithout pulp,except prunejuice • Ripebananas • Melons •Allraw fruits exceptbananaand melons •Driedfruits, includingprunes andraisins • Fruit juicewithpulp • Anyfruits sweetened withsorbitol • Prune juice 23
- 24. Medical Nutrition Therapyfor Diarrhea FoodGroup Recommended Foods FoodsNot Recommended Beverages • Decaffeinated coffee • Caffeine-free teas •Softdrinkswithout caffeine • Rehydration beverages •Beverages containing caffeine, includingregular coffee, regular tea, colas,and energydrinks •Avoidbeverages sweetenedwith sorbitol • Alcoholicbeverages Fats •Limitfats to lessthan 8 teaspoonsper day Other foodsto avoid •Sugaralcoholssuchasxylitol and sorbitol;honey 24
- 25. NUTRITION THERAPY AND PATHOPHYSIOLOGY Marcia Nelms Katheryn Sucher 25