ERCP.pptx
•Download as PPTX, PDF•
0 likes•424 views
ERCP Indications and complications
Report
Share
Report
Share
Recommended
More Related Content
What's hot
What's hot (20)
LAP RIGHT HEMICOLECTOMY-STEP BY STEP Operative Surgery.pptx

LAP RIGHT HEMICOLECTOMY-STEP BY STEP Operative Surgery.pptx
Preoperative Evaluation For Living Donor Liver Transplantation

Preoperative Evaluation For Living Donor Liver Transplantation
Similar to ERCP.pptx
Similar to ERCP.pptx (20)
Perioperative care of patients with kidney diseases prof (1). ahmed rabee

Perioperative care of patients with kidney diseases prof (1). ahmed rabee
Perioperative evaluation and management of surgical

Perioperative evaluation and management of surgical
PERIOPERATIVE MANAGEMENT OF THE PATIENTS WITH LIVER DISEASE.pptx

PERIOPERATIVE MANAGEMENT OF THE PATIENTS WITH LIVER DISEASE.pptx
InTech-Critical_care_issues_after_major_hepatic_surgery

InTech-Critical_care_issues_after_major_hepatic_surgery
Acs0533 The Surgical Management Of Ulcerative Colitis 2004

Acs0533 The Surgical Management Of Ulcerative Colitis 2004
More from Dr.Amjed Alnatsheh
More from Dr.Amjed Alnatsheh (17)
Treatment of CAP in adults who require hospitalization.pptx

Treatment of CAP in adults who require hospitalization.pptx
Treatment of CAP in adults who require hospitalization.pptx

Treatment of CAP in adults who require hospitalization.pptx
Recently uploaded
Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent High Profile Call Girl 24×7
Booking Contact Details
WhatsApp Chat: +91-9930245274
Mumbai Escort Service includes providing maximum physical satisfaction to their clients as well as engaging conversation that keeps your time enjoyable and entertaining. Plus they look fabulously elegant; making an impressionable.
Independent Escorts Mumbai understands the value of confidentiality and discretion - they will go the extra mile to meet your needs. Simply contact them via text messaging or through their online profiles; they'd be more than delighted to accommodate any request or arrange a romantic date or fun-filled night together.
We provide -
Flexibility
Choices and options
Lists of many beauty fantasies
Turn your dream into reality
Perfect companionship
Cheap and convenient
In-call and Out-call services
And many more.
29-04-24 (Smt)Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...

Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...Call Girls in Nagpur High Profile
Recently uploaded (20)
Call Girls Aurangabad Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Aurangabad Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Tirupati Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Tirupati Just Call 8250077686 Top Class Call Girl Service Available
(Low Rate RASHMI ) Rate Of Call Girls Jaipur ❣ 8445551418 ❣ Elite Models & Ce...

(Low Rate RASHMI ) Rate Of Call Girls Jaipur ❣ 8445551418 ❣ Elite Models & Ce...
Premium Call Girls Cottonpet Whatsapp 7001035870 Independent Escort Service

Premium Call Girls Cottonpet Whatsapp 7001035870 Independent Escort Service
Call Girls Cuttack Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Cuttack Just Call 9907093804 Top Class Call Girl Service Available
Call Girls Agra Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Agra Just Call 8250077686 Top Class Call Girl Service Available
Premium Call Girls In Jaipur {8445551418} ❤️VVIP SEEMA Call Girl in Jaipur Ra...

Premium Call Girls In Jaipur {8445551418} ❤️VVIP SEEMA Call Girl in Jaipur Ra...
Best Rate (Hyderabad) Call Girls Jahanuma ⟟ 8250192130 ⟟ High Class Call Girl...

Best Rate (Hyderabad) Call Girls Jahanuma ⟟ 8250192130 ⟟ High Class Call Girl...
Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...

Book Paid Powai Call Girls Mumbai 𖠋 9930245274 𖠋Low Budget Full Independent H...
Call Girls Ludhiana Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Ludhiana Just Call 9907093804 Top Class Call Girl Service Available
Call Girls Nagpur Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Nagpur Just Call 9907093804 Top Class Call Girl Service Available
Call Girls Faridabad Just Call 9907093804 Top Class Call Girl Service Available

Call Girls Faridabad Just Call 9907093804 Top Class Call Girl Service Available
VIP Hyderabad Call Girls Bahadurpally 7877925207 ₹5000 To 25K With AC Room 💚😋

VIP Hyderabad Call Girls Bahadurpally 7877925207 ₹5000 To 25K With AC Room 💚😋
Premium Bangalore Call Girls Jigani Dail 6378878445 Escort Service For Hot Ma...

Premium Bangalore Call Girls Jigani Dail 6378878445 Escort Service For Hot Ma...
Call Girls Siliguri Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Siliguri Just Call 8250077686 Top Class Call Girl Service Available
Top Rated Bangalore Call Girls Mg Road ⟟ 9332606886 ⟟ Call Me For Genuine S...

Top Rated Bangalore Call Girls Mg Road ⟟ 9332606886 ⟟ Call Me For Genuine S...
Call Girls Jabalpur Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Jabalpur Just Call 8250077686 Top Class Call Girl Service Available
Top Rated Bangalore Call Girls Richmond Circle ⟟ 9332606886 ⟟ Call Me For Ge...

Top Rated Bangalore Call Girls Richmond Circle ⟟ 9332606886 ⟟ Call Me For Ge...
Night 7k to 12k Navi Mumbai Call Girl Photo 👉 BOOK NOW 9833363713 👈 ♀️ night ...

Night 7k to 12k Navi Mumbai Call Girl Photo 👉 BOOK NOW 9833363713 👈 ♀️ night ...
♛VVIP Hyderabad Call Girls Chintalkunta🖕7001035870🖕Riya Kappor Top Call Girl ...

♛VVIP Hyderabad Call Girls Chintalkunta🖕7001035870🖕Riya Kappor Top Call Girl ...
ERCP.pptx
- 1. ERCP
- 2. The role of ERCP in managing pancreaticobiliary disorders is mostly therapeutic one because other of diagnostic testing (eg, MRI with MRCP, endoscopic ultrasound) high diagnostic accuracy without the risks associated with ERCP (eg, acute pancreatitis)
- 3. Indications for ERCP-guided interventions include : 1. Choledocholithiasis 2. Acute cholangitis 3. Drainage of malignant biliary obstruction (eg, pancreatic cancer, hilar cholangiocarcinoma) 4. Post-surgical biliary complications (eg, biliary stricture, bile leak) 5. Management of complications related to acute or chronic pancreatitis (eg, pancreatic duct stricture, pancreatic stones) 6. Extrahepatic biliary strictures related to primary sclerosing cholangitis 7. Endoscopic therapy for some patients with sphincter of Oddi
- 4. Contraindications ERCP is usually contraindicated in conditions where the risk of complications is high, and thus, the risks outweigh the potential benefits of the procedure. Some patients who are at high risk for complications, such as those with acute severe cholangitis associated with sepsis sepsis and cardiorespiratory dysfunction, may undergo interventional ERCP to relieve biliary obstruction because of the high risk of mortality related to severe cholangitis.
- 5. Relative contraindications to ERCP include: Patients who cannot tolerate monitored anesthesia care or general anesthesia Patients with an untreated hemostatic disorder who are deemed to be at high risk for bleeding by the advanced endoscopist Patients with gastrointestinal (luminal) obstruction may undergo endoscopy, but the examination is limited to an area proximal to the level of obstruction Patients with type III sphincter of Oddi dysfunction Type III SOD: biliary-type pain but normal liver tests and common bile duct diameter
- 6. Risk factors Some ERCP-related complications are due to the effect of procedural sedation (eg, hypotension), while others are due to the endoscopy itself or to an intervention. I. Procedure-related factors (eg, difficulty of cannulation, biliary sphincterotomy, precut [access] sphincterotomy) II. Patient-related factors (eg, surgically-altered anatomy, sphincter of Oddi dysfunction, periampullary diverticulum, cirrhosis, older age, and end-stage kidney disease)
- 7. Complications related to ERCP have also been characterized based on the following factors Location – Complications may be focal, occurring at the point of endoscopic contact (eg, perforation, bleeding, pancreatitis), or a complication may affect an organ system (eg, cardiopulmonary) Timing – Complications may occur early (typically within 30 days after the procedure) or late (beyond 30 days). Severity – The severity of complications can be assessed by duration and type of hospital stay (eg, intensive care unit); blood transfusion requirement; need for surgical, radiologic, or endoscopic interventions; and rates of morbidity and mortality
- 8. Complications Pancreatitis — May result from mechanical injury to the pancreatic duct, hydrostatic injury from contrast injection or guidewire manipulation. Bleeding :Related to instrumentation such as biliary and/or pancreatic sphincterotomy. Infection — May be related to incomplete drainage of an infected biliary system, obstruction of the cystic duct, infected pancreatic fluid collection, or or rarely, contaminated endoscopic equipment
- 9. Perforation — ERCP may be complicated by perforation of the esophagus, stomach, or small intestine Other complications — Several rare complications have been associated with ERCP including gas embolism, pneumothorax,
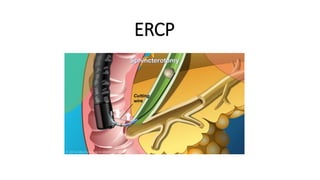
- 10. • Sphincterotomy-related complications Rates overall have ranged from 3 to 12 % . Sphincterotomy-related perforations are typically retroperitoneal. Other interventions that are performed in addition to sphincterotomy (eg, stone extraction, biliary stent placement) may also contribute to the risk of complications Anesthesia-related complications — Complications related to procedural sedation and anesthesia (eg, hypoxemia, hypotension)
- 11. Post ERCP pancreatitis • Post-ERCP pancreatitis (PEP) is the most common serious adverse event attributed to the ERCP, resulting in annual estimated costs exceeding 150 million dollars in the United States.
- 12. Elevated serum pancreatic enzyme levels alone do not constitute PEP, because transient increases in serum pancreatic enzyme levels may occur in up to 75% of individuals after the procedure, regardless of symptoms. Conversely, individuals with low serum amylase levels less than 1.5 times the upper limit of normal, obtained 2 to 4 hours after ERCP, are unlikely to have or develop PEP.
- 13. A recent meta-analysis of 108 randomized, controlled trials involving 13,296 patients, reported a 9.7% overall incidence of PEP (95% confidence interval [CI], 8.6%-10.7%), with an increased incidence of 14.7% (95% CI, 11.8%-17.7%) in high-risk patients. The majority of PEP cases were mild, with a mortality rate of 0.7%.
- 14. The definition of post-ERCP pancreatitis ●New or worsened abdominal pain combined with >3 times the normal value of amylase or lipase more than 24 hours after ERCP and requirement of hospital admission . Mortality rates related to post-ERCP pancreatitis have also been low and range from 0.1 to 0.7 percent
- 17. Pharmacologic prophylaxis • Rectal nonsteroidal anti-inflammatory drugs — We agree with society guidelines that endorse the use of NSAIDs; administered rectally to reduce the incidence of post-ERCP pancreatitis in patients undergoing ERCP who do not have contraindications for NSAIDs. We typically give indomethacin suppository 100 mg or diclofenac suppository 100 mg immediately before ERCP ERCP . Contraindications for rectal NSAIDs include pregnancy at ≥30 weeks gestation, history of skin disease such as Steven-Johnson syndrome, or NSAID allergy . Contraindications and adverse events associated with NSAIDs are discussed in more detail separately.
- 18. • NSAIDs inhibit several mediators of the inflammatory cascade that are thought to play a role in the pathogenesis of acute pancreatitis (ie, prostaglandins and phospholipase A2)
- 19. • Other pharmacologic strategies —However, some society guidelines suggest that nitrates may be a reasonable alternative alternative for prophylaxis in patients in whom NSAIDs and aggressive intravenous hydration .
- 20. IV hydration IV hydration is thought to prevent further injury to the pancreas from microvascular hypoperfusion. Aggressive IV hydration with lactated Ringer’s (LR) solution ( preferred). Patients in the aggressive hydration group received 3 mL/kg/hour during the procedure, a 20 mL/kg bolus immediately after the procedure, and 3 mL/kg/hour for 8 hours after the procedure.
- 21. THANKS