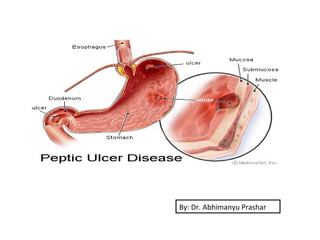
Gastric Acid Regulation, PUD Etiology, Diagnosis and Management
- 1. By: Dr. Abhimanyu Prashar
- 2. PUD: “A condition in which there is a discontinuity in the entire thickness of the gastric or duodenal mucosa” Ulcers: “The areas of degeneration and necrosis of gastrointestinal mucosa exposed to acid and pepsin secretion”
- 3. Regulation of gastric acid secretion Mediated by 3 pathways: Neurocrine (Ach) Paracrine (Histamine) Endocrine (Gastrin) • Activation of proton pump exchange of H+ • In addition, histamine, gastrin & ach receptors stimulate H+ production • Ach from post ganglionic vagal neurons • Gastrin fron antral G cells stimulates pepsinogen secrection, hepatic bile flow & pancreas (insulin)
- 4. It also stimulates gastric & intestinal motility Directly stimulates Hcl secretion by acting on gastrin receptors on parietal cells Gastrin activates ECL cells which releases histamine Histamine activates H2 rec, results in activation adenylate cyclase which convers ATP to cAMP and subsequent generation of H+ & proton pump mobilses & activated
- 5. Autoregulatory mechanism: Ingestion of meal gastrin release gastric acid secretion decreased PH release of somatostatin from D cells decreased release of gastrin, inhibits acid secretion, suppress histamine release Other NTs, vasoactive intestinal peptide, galanine, serotonin, are also involved in direct or indirect regulation of gastric acid secretion
- 7. Epidemiology PUD is more common in unskilled labourers and low socioeconomic groups Smokers and individuals who are on NSAIDs are more prone to develop PUD About 10% of the population in developed countries likely to be affected by PUD Duodenal ulcer is 4 times more common than gastric ulcer
- 8. Etiopathogenesis Infection with Helicobacter pylori Use of NSAIDs Local irritants Dietary factors Hormonal factors Decreased mucous secretion
- 9. H.pylori A spiral gram negative bacterium 95% of duodenal ulcers & 85% of gastric ulcers are associated with H.pylori infection H.Pylori produces Cag A proteins and vacuolating cytotoxins (Vac A) which activates inflammatory cascade It expresses sialic acid specific haemagglutinins and a lipid binding adhesion that mediate binding to the mucosal surface
- 10. Enzymes like urease, haemolysins, neuraminidase and fucosidase involve in tissue damage Altered gastrin homeostasis in H.pylori infection Hypergastinaemia leads to inflammation and ulcer formation
- 12. Use of NSAIDs NSAIDs cause 3 patterns of mucosal damage Superficial erosions & haemorrhages Silent ulcers detected at endoscopy Ulcers causing clinical symptoms Mechanism: reduction of mucosal PGs production Approx. 20% of patients taking NSAIDs experience Dyspepsia Approx. 4% of NSAID users suffer from ulcer and ulcer complications
- 13. Local irritants Pyloric antrum & lesser curvature of stomach most exposed for longer periods of irritants (like spicy food, alcohol, tobacco smoking) hence these are common sites for occurrence of gastric ulcer
- 14. Dietary factors Poor socio-economic status (malnutrition) Irregular food habits Social habits Consumption of spicy food
- 15. Hormonal factors Zollinger-Ellison syndrome (acid secreting tumours) leads to massive hypersecretion of gastric acid
- 16. Decreased mucous secretion Conditions like stress, anxiety that decreases quantity or quality of normal protective mucous barrier predisposes to the development of PUD
- 18. Duodenal ulcer • Pain-food relief pattern • Night pain common • No vomiting • Melena (blood in stool) more common • No loss of weight Gastric ulcer • Food-pain pattern • No night pain • Vomiting present • Hematemesis (blood in vomit) more common • Significant loss of weight
- 19. Investigations
- 21. H. pylori detection: Serology to detect Abs Urea breath test Histology & culture
- 22. Management
- 23. Triple therapy Omeprazole 20 mg PO bid + Clarithromycin 500 mg PO bid for 7 days + Amoxicillin 1 gram PO bid Omeprazole 20 mg PO bid + Clarithromycin 500 mg PO bid for 7 days + Metronidazole 400 mg PO tid
- 24. Quadruple therapy Bismuth 107.7 mg PO qid + Metronidazole 200 mg PO tid & 400 mg at night + Tetracycline 500 mg PO qid for 14 days + Omeprazole 20 mg or Lansoprazole 30 mg or Pantoprazole 40 mg PO bid
- 26. Follow on antisecretory therapy for complicated ulcers and larger ulcers of ≥ 1 cm diameter H2 Rec antagonists Ranitidine 300 mg PO or Nizatidine 300 mg PO or Famotidine 40 mg PO or Cimetidine 800 mg PO With evening meal For additional 4-6 weeks PPIs Pantoprazole 40 mg PO or Lansoprazole 30 mg PO or Omeprazole 20 mg PO or Rabeprazole 20 mg PO For additional 2-4 weeks
- 27. Bleeding peptic ulcers Endoscopic haemostasis using a heater probe or Inj. Adrenaline 1: 10000 or 1: 100000 Omeprazole 80 mg as a bolus dose then 8 mg/hr infusion for 3 days
- 28. Stress ulceration prophylaxis Ranitidine 300 mg PO 1-0-1 or Famotidine 40 mg PO 1-0-1 or Sucralfate 1 gram every 6 hourly or Omeprazole 20/40 mg PO 1-0-1 or Pantoprazole 20/40 mg PO 1-0-1
- 29. Antacids Magnesium hydroxide (1g≈ 30 m eq HCl) Magnesium trisilicate (1g ≈ 10 m eq HCl) Aluminium hydroxide gel (5 ml ≈ 1 m eq HCl) Calcium carbonate (1g ≈ 20 m eq HCl) Sodium bicarbonate (1 g ≈ 12 m eq HCl) Sodium citrate (1g ≈ 12 m eq HCl)
- 30. Ulcer protective drugs Sucralfate (aluminium salt of sulphated sucrose) Colloidal bismuth sub citrate
- 31. Prostaglandin analogues: Misoprostol (methyl PGE1 ester) 200 mcg Anticholinergics: Pirenzepine 100-150 mg/day
- 32. Drugs causing dyspepsia Corticosteroids Bisphosphonates Potassium chloride Iron Antibiotics CCBs Nitrates Theophylline Drugs with anti muscarinic effects e.g. TCAs NSAIDs: High risk: Long acting - piroxicam, ketoprofen low risk: short acting- ibuprofen, diclofenac reduced risk: highly selective COX-2 inhibitors
- 33. ZES Characterized by severe peptic ulceration, gastric acid hyper secretion and a non β-cell islet tumor of the pancreas (gastrinoma) ZES is the cause of about 0.1 % of cases of duodenal ulceration
- 34. Gastrinoma Secretes Large amount of gastrin Stimulates Parietal cells Maximal acid secretion & increased parietal cell mass Increased acid output Reduced luminal PH to 2 or less Inactivate pancreatic lipase & precipitates bile acids Diarrhea & steatorrhoea Pathogenesis
- 35. Clinical features: Diarhoea & Steatorrhoea Investigations: serum gastrin levels Endoscopic ultrasound
- 36. Management Non-pharmacological: Tumor resection Pharmacological: Omeprazole 60-80 mg/D Synthetic somatostatin analogue: Octreotide SC 200-300 mcg/D BD
Editor's Notes
- Regulation read in KDT before class
