multiplesclerosis-pdf.pdf
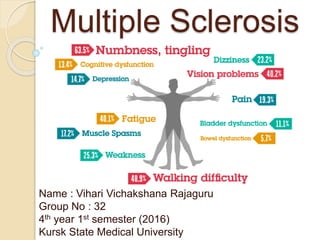
- 1. Multiple Sclerosis Name : Vihari Vichakshana Rajaguru Group No : 32 4th year 1st semester (2016) Kursk State Medical University
- 2. Introduction Transmission of action potentials along myelinated axons. An action potential “jumps” from node to node. Voltage-gated Na+ channels are present only at the nodes of Ranvier.
- 3. What is MS ? a chronic, typically progressive disease involving damage to the sheaths of nerve cells in the brain and spinal cord. The immune system attacks the protective sheath (myelin) that covers nerve fibers and causes communication problems between your brain and the rest of your body. Eventually, the disease can cause the nerves themselves to deteriorate or become permanently damaged
- 4. No 01 No 02 No 03
- 5. Global distribution of MS
- 6. Etiology Cause of MS is still not known, scientists believe that the interaction of several different factors may be involved. Immunologic Factors Environmental Factors Infectious Factors Genetic Factors
- 7. Path physiology Blood-brain barrier breakdown The BBB prevent entrance of T cells into the nervous system. The blood–brain barrier is normally not permeable to these types of cells, unless triggered by infection or a virus, which decreases the integrity of the tight junctions. When the blood–brain barrier regains its integrity, usually after infection or virus has cleared, the T cells are trapped inside the brain. Autoimmunology The immune system attacks the nervous system, forming plaques or lesions. Commonly involves white matter. Destroys oligodendrocytes- causing demyelination Remyelination occurs in early phase but not completely. Repeated attacks lead to fewer remyelination. Inflammation T-cells attacks on myelin triggers inflammatory processes, stimulating other immune cells and soluble factors like cytokines and antibodies. Leaks form in the BBB cause swelling, activation of macrophages, and more activation of cytokines and other destructive proteins
- 12. CLASSIFICATION OF MULTIPLE SCLEROS PRMS Progressive Relapsing MS SPMS Secondary Progressive MS PPMS Primary Progressive MS RRMS Relapsing/ Remitting MS Gradual progression of the disease from its onset with no relapses or remissions Unpredictable attacks which may or may not leave permanent deficits followed by periods of remission Initial RRMS that suddenly begins to decline without periods of remission and relapses. Steady decline since onset with super-imposed attacks.
- 13. Progressive Relapsing Mild infrequent sensory exacerbations with full recovery. Secondary Progressive Condition of patients with relapsing/remitting disease begins to gradually worsen over time with resulting accumulation of neurological signs and symptoms. In this form of the disease, relapses become more severe while remissions are less complete, shorter in duration, and eventually non- existent. The course of MS becomes steadily progressive.
- 14. Primary Progressive There is no history of relapse in these patients. Disease begins with a slow progression of neurologic deficits. Problems appear and gradually worsen over time. Common problems include spastic paraparesis, cerebellar ataxia, urinary incontinence. Relapsing Remitting Multiple Sclerosis Episodes of exacerbations and remissions during which not all symptoms resolve completely. The patient may be left with permanent disability which may vary in severity. Relapses are often more severe than in the previous group. Relapses also become more severe with time.
- 15. The most common initial symptoms • changes in sensation in the arms, legs or face : numbness (33%) • Optic neuritis (20%) • weakness (13%) • double vision- internuclear opthalmoplegia (7%) • unsteadiness when walking (5%) • and balance
- 16. sensory exam ◦ - ascending numbness starting in the feet; ◦ - bilateral hand numbness; ◦ - hemiparesthesia; ◦ - dysesthesia in one of the above distributions; ◦ - generalized heat intolerance Objectively the most common sensory findings in the"numb" areas are dorsal column signs, such as reduction of vibration, proprioception and stereognosis, rather than problems with spinothalamic tract.
- 17. Right internuclear ophthalmoplegia in a patient with multiple sclerosis. In the initial phase of leftward gaze (upper photograph), only the left eye is abducted. The right eye follows, after a delay (lower photograph).
- 18. Lhermitte's sign (25-40%) is an electrical sensation that runs down the back and into the limbs and is produced by bending the neck forwards. The sign suggests a lesion of the dorsal columns of the cervical cord or of the caudal Uhthoff's phenomenon is the worsening of neurologic symptoms in multiple sclerosis and other neurological, demyelinating conditions when the body gets overheated from hot weather,
- 19. Ongoing Symptoms and Signs Motor system: ◦ -weakness (variable severity mono- and paraparesis, hemiparesis, quadriparesis) ◦ -increased spasticity resulting in spastic gait ◦ -pathologic signs (Babinski's, Chaddock's, Hoffmann, Oppenheim's, etc.) -dysarthria Cerebellar signs: ◦ -incoordination (dysdiadochokinesia, problems with heel-to-shin test) ◦ -slowing of rapid repeating movements ◦ -cerebellar ataxia (ataxic gait) ◦ -scanning speech
- 20. INVESTIGATION CSF oligoclonal bands, abnormal colloidal gold curve, elevated γ- globulin IgG, mild mononuclear pleocytosis (<40 cells/mL), myelin debris, normal or slightly elevated protein. (Myelin basic Protein) Blood test •B-12 and folate levels or antinuclear antibody (ANA) titers. •Antiphospholipid antibody syndrome must be undertaken in patients with evidence of blood dyscrasia and in women with unexplained miscarriages or history of deep venous thrombosis. •elevated erythrocyte sedimentation rate (ESR) and positive titers of rheumatoid factor (RF) should help identify the presence of a vasculitic disorder that may be mimicking MS. MRI MRI of the head and spine (more sensitive than CT): May show many plaques. MRI reveals multiple lesions with high T2 signal intensity and one large white matter lesion. These demyelinating lesions may sometimes mimic brain tumors because of the associated edema and inflammation.
- 25. Diagnostic Criteria Clinical Presentation Additional Data Needed * 2 or more attacks (relapses) * 2 or more objective clinical lesions None; clinical evidence will suffice (additional evidence desirable but must be consistent with MS) * 2 or more attacks * 1 objective clinical lesion Dissemination in space, demonstrated by: * MRI * or a positive (cerebrospinal fluid) CSF and 2 or more MRI lesions consistent with MS * or further clinical attack involving different site Diagnosis is based on McDonald’s Criteria (Revised 2010)
- 26. * 1 attack * 2 or more objective clinical lesions Dissemination in time, demonstrated by: * MRI * or second clinical attack * 1 attack * 1 objective clinical lesion (monosymptomatic presentation) Dissemination in space demonstrated by: * MRI * or positive CSF and 2 or more MRI lesions consistent with MS and Dissemination in time demonstrated by: * MRI * or second clinical attack Insidious neurological progression suggestive of MS (primary progressive MS) One year of disease progression (retrospectively or prospectively determined) andTwo of the following: a. Positive brain MRI (nine T2 lesions or four or more T2 lesions with positive VEP)b. Positive spinal cord MRI (two focal T2 lesions)c. Positive CSF
- 27. Treatment As of 2011, six treatments have been approved by FDA 1. Interferon beta 1a (Avonex, CinnoVex,ReciGen and Rebif) 2. Interferon beta-1b (Betaseron ) 3. Glatiramer acetate (Copaxone), a non- steroidalimmunomodulator. 4. Mitoxantrone, is an immunosuppressant 5. Natalizumab (Tysabri) Steroids: methylprednisolone (MP) 500–1,000 mg/d IV for 5 days followed by tapered oral prednisone or MP 1 g/d IV for 3 days ± oral taper
- 28. MANAGEMENT Spasticity Baclofen 5 mg PO 1–3 t.i.d. and increase as needed Diazepam 2–5 mg PO at bedtime Pain NSAIDs Gabapentin effective vs. MS pain syndromes at 300 mg/d PO, may increase to 1,800 mg/d within 1 week, max dose 3,600 mg/d Bladder dysfunction Propantheline 7.5 mg PO q3–4h to start, increase to 15 mg t.i.d. to q.i.d. plus 15–30 mg at bedtime Oxybutynin chloride 5 mg PO t.i.d.–q.i.d. Prophylactic antibiotics for urinary infections Self-catheterizations for inadequate bladder emptying Constipation: Stool softeners, bulk-producing agents, laxative suppositories Incoordination or tremors: Incoordination or tremors: Depression and emotional lability Antidepressant agents such as SSRIs. Psychotherapy and support Paranoia or mania Haloperidol lithium or atypical antipsychotic Hemifacial and dysesthesias Carbamazepine 100–200 mg PO once or twice a day to start; increase to total daily dosage of 600–1,600 mg t.i.d.–q.i.d. Must monitor serum levels
- 29. Other regime A main focus for MS patients is intake of foods that lower inflammation, not aggravate it. • Polyphenols (including flavonoids and nonflavonoids) and carotenoids: vegetables, fruits, wine, spices, and herbs • Polyunsaturated fats , omega-3 fatty acids and DHA: olive oil, oily fish, fish oil. ◦ Limiting saturated fats of animal origin ◦ limit caffeine consumption to decrease bone mineralization loss
- 30. Vitamin B12 deficits is associated with demyelination of nerve fibers so supplementation of Vitamin B12 and Vitamin B complex assists in prevention. Calcium supplementation is important as the incidence of osteoporosis , related to decreased mobility, is higher in MS patients. vitamin D, selenium, and zinc have all been found to decrease the production of inflammatory molecules associated with MS as well.
- 31. Prognostic Factors in Patients with Multiple Sclerosis Good prognosis Optic Neuritis Isolated sensory symptoms Long interval to second relapse No evidence of disability after 5 years Female gender Poor Prognosis ‘Multifocal’ Clinically Isolated Syndrome Efferent (motor/cerebellar) systems High relapse rate in 5 years Substantial disability after 5 years Abnormal MRI with
- 32. Mortality Rates for Multiple Sclerosis The average life span of an individual with MS is 25-35 years after initial diagnosis. Most MS patients live into the 7th decade Studies have shown that individuals with MS die around 10 years earlier than the general population Studies have indicated that MS is not a cause of death, whereas deaths occur as a result of other chronic complications resulting from immobility, chronic urinary tract infections, dypsnea, dysphagia, aspiration & bacterial pneumonia