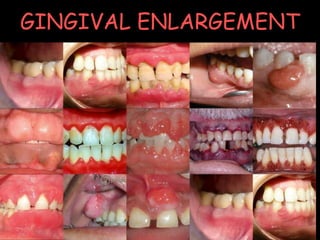
smitagingivalenlargement-160502160226.pptx
- 2. CONTENTS • Introduction • Classification • Indices • Inflammatory Enlargement • Enlargements associated with systemic diseases • Neoplastic enlargement • Drug-induced enlargement • Idiopathic gingival enlargement • False enlargement • Conclusion • References
- 3. INTRODUCTION Hypertrophic gingivitis Gingival enlargement Gingival overgrowth Gingival hyperplasia
- 4. CLASSIFICATION A] Based on etiologic factors and pathologic changes I. Inflammatory Enlargement -Acute - Chronic II. Drug-induced enlargement III. Enlargements associated with systemic diseases ii) Systemic diseases causing 1. Leukemia 2.Granulomatous diseases (Wegener's granulomatosis, sarcoidosis) i) Conditioned enlargement IV1..NP r ee og pn la an sc ty icenlargement (ggiinnggiivvaallteunmlaorgrse)ment 2. Puberty B3e.nVigitnamtuinmCodrseficiency M 4 a . lPiglansamnatcteullmgoinrgsivitisV .5F . a N ls oe nse pn ec la ifr ig ce cm one dn itt ioned enlargement
- 5. B] Based on location and distribution I. Localized II. Generalized III. Marginal IV. Papillary V. Diffuse VI. Discrete
- 6. INDICES Bokenkamp & Bohnhorst 1994 Grade 0 No signs of gingival enlargement Grade 1 Enlargement confined to IDP Grade 2 Enlargement involves IDP & marginal gingiva Grade 3 Enlargement covers three quarters / more of crown
- 7. Degree of gingival hyperplasia according to modified index by Angelopoulos & Goaz 1972 Grade Hyperplasia Size Tooth coverage 0 No Normal No 1 Minimal <2 mm Cervical 3rd or less 2 Moderate 2-4 mm Middle 3rd 3 Severe >4 mm More than 2/3rd
- 8. Gingival overgrowth index- Mc Gaw et al 1987 Grade 0 No overgrowth, feather edge gingival margin Grade 1 Blunting of gingival margin Grade 2 Moderate gingival overgrowth (one third crown length) Grade 3 Marked gingival overgrowth (more than one thirds of crown)
- 9. Clinical index for drug induced gingival overgrowth G r a d e 0 G G G G r r r r a a a a d. d d d e. e e e 1 2 3 4 Ingles et al 1999 1.MNoodoevreartgerovwetrhgrowthincrease incsriezaesoefinthdeepnaspitiyllaeand rolled gi rn ag ni u v lal rm ap a p re ga in ra snce 2 ap . p Te ha era cn oc ne tour concave or straight 3. buccolingual dimension of upto 2mm 4. Probing ≤ 6mm 5. Papillae retractable 11..MEaarrlkyedovoevregrrgorwowththslight e 2 n .csrliogahcthsmtiepnptlionng,thneo/cslliingihctal c2 r. o m w a n rked stippling and granular 2 3. T kn hie fe co en dt g o eum r c ao rg ni v n ex 3.tBipuocfcothlienpgaupailldlaiemiesnrsoiound s≥ iz3 e mm 4. The probing depth ≥ 6mm 5. Papillae retractable 1. Severe overgrowth, profound thickening of gingiva 2. Large % of the clinical crown is covered 3 4. . P no ap ii n lc la re ea -se re in tra th ce tad be le nsity or 4 4 . . p P r r o o b b i n i n g g d d e e p p t h t h≤ ≥ 3 6 m m m m 5.buccolingual dimension 3mm
- 11. a. Chronic inflammatory enlargement Etiology Plaque accumulation & retention Poor oral hygiene Anatomic abnormalities Improper restoration Orthodontic appliances Malocclusion
- 12. Clinical Features 1. Slight ballooning of IDP & marginal gingiva Life preserver shaped bulge Smooth , edematous , bleed easily Localised / generalised Progress- slowly and painlessly Pseudopockets
- 13. Discrete sessile or pedunculated tumor like mass Interproximal / marginal or attached gingiva Slow growing and painless Clinical Features 1. 2.
- 14. Histopathology 1.Soft and friable 2.Firm and resilient
- 15. B. ACUTE INFLAMMATORY ENLARGEMENT 1. GINGIV ALABSCESS Etiology Foreign substances Clinical features Marginal gingiva or IDP Red swelling smooth shiny surface Fluctuant and pointed with a surface orifice expresses purulent exudate
- 16. 2. PERIODONTALABSCESS Lateral abscess / parietal abscess Depending on location - Gingival - Periodontal (Acute / Chronic) - Pericoronal Meng et al ’99 Depending on number - Single - Multiple
- 17. Etiology PERIODONTITIS RELATED Extension of infection from PD pocket Lateral extension of inflammation Pocket with a tortuous course Incomplete removal of calculus
- 18. Etiology NON PERIODONTITIS RELATED Impaction of foreign bodies Endodontic perforation Lateral cyst infection Factors affecting morphology of root
- 19. Signs and symptoms Acute abscess - Mild to severe discomfort - Localized red, ovoid swelling - Periodontal pocket - Mobility - Tooth elevation in the socket - Tenderness to percussion or biting - Suppuration - Elevated temperature - Regional lymphadenopathy Chronic abscess - No pain or dull pain - Localized inflammatory lesion - Slight tooth elevation - Intermittent exudation -Fistulous tract often associated with deep pocket - Usually without systemic involvement
- 20. ENLARGEMENTS ASSOCIATED WITH SYSTEMIC DISEASES Two mechanisms 1. Magnification of an existing inflammation initiated by dental plaque - conditioned enlargement 2. Manifestation of the systemic disease independently of the inflammatory status of the gingiva - systemic disease causing enlargement
- 21. 1. Conditioned enlargement • Systemic condition exaggerates or distorts usual gingival response to plaque • Bacterial plaque Types 1. Hormonal – pregnancy , puberty 2. Nutritional – vitamin C deficiency 3. Allergic Non specific conditioned
- 22. 1. Marginal and generalised enlargement 2. Single or multiple tumor like masses Hormonal changes - Progesterone and estrogen - Vascular permeability – edema , inflammatory response Subgingival microbiota – P. intermedia a. Enlargement in pregnancy
- 23. 1. Marginal enlargement - Generalised , more prominent interdentally - Bright red or magenta colour - Friable , smooth & shiny surface - Bleeding – spontaneously or on slight provocation “ Pregnancy rhinitis”
- 24. 2. Tumor like gingival enlargement “Pregnancy tumor” - Discrete mushroomlike , flattened spherical mass - Dusky red or magenta , smooth glistening surface - Doesnot invade underlying bone - Semifirm – soft , friable - sessile or pedunculated - Painless unless its size and shape foster accumulation of debris
- 25. Angiogranuloma Thickened epilthelium Newly formed, engorged capillaries Fibrous stroma Inflammatory infiltrate Histopathology
- 26. Treatment • Removal of plaque and calculus • Tumor like gingival enlargement - surgical excision and SRP • Recurrence • Spontaneous reduction – termination of pregnancy
- 27. • Male and female adoloscents • Areas of plaque accumulation • Facial surface • Marginal and interdental Histopathology - Similar to Chronic inflammation Difference b. Enlargement in puberty
- 28. c. Enlargement in vitamin C deficiency • Classic description of scurvy • Acute deficiency – hemorrhage , collagen degeneration , edema • modify response to plaque Clinical features - Bluish red , soft , friable, boggy - smooth & shiny surface - Haemorrhage – spontaneous / slight provocation - Surface necrosis with pseudomembrane formation
- 29. d. Plasma cell gingivitis • Atypical gingivitis / plasma cell gingivostomatitis • Plasma cell granuloma – localised form • Allergic in origin Clinical features
- 30. • Pyogenic granuloma Clinical features • Discrete spherical , tumorlike mass , pedunculated , smooth surface • Bright red or purple , friable or firm • Painless • Hemorrhage e. Nonspecific conditioned enlargement
- 31. 2.Systemic Disease That Cause Gingival Enlargement 1. Leukemia malignant neoplasia of WBC precursors -diffuse replacement of bone marrow – proliferating leukemic cells - abnormal number and forms of immature WBCs - widespread infiltrates Acute myeloid leukemia
- 32. Clinical features • Diffuse / marginal • Localised / generalised • Overextension of marginal gingiva • Discrete tumorlike interproximal mass • Bluish red , shiny surface • Firm • Hemorrhage
- 33. Leukemic infiltration Leukemic cell infiltration of gingival corium Gingival thickness Gingival pockets Plaque accumulation Secondary inflammatory lesion
- 34. Histopathology - Connective tissue – dense mass of immature and proliferating leukocytes , engorged capillaries , edema - Epithelium – degree of leukocytic infiltration and edema
- 35. 2. Granulomatous disease a.Wegeners granulomatosis - Acute granulomatous necrotising lesions of respiratory tract , nasal and oral defects - Acute necrotising vasculitis Clinical features -oral mucosal ulcerations -delayed healing -Papillary enlargement – reddish purple , - bleeds easily -Strawberry gingiva
- 36. Etiology - Unknown - Immunologically mediated tissue injury Histopathology
- 37. b. Sarcoidosis - Unknown etiology - Involve any organ Clinical features
- 38. NEOPLASTIC ENLARGEMENT 1. Benign tumors of gingiva Epulis a. Fibroma i) Giant cell fibroma ii) Peripheral ossifying fibroma
- 39. b. Papilloma - Proliferations of surface epithelium associated with HPV - HPV 6 & 11
- 40. c. Peripheral Giant Cell Granuloma Peripheral giant cell tumors d.Central Giant Cell Granuloma - Arise within the jaw – central cavitation
- 41. e. Leukoplakia • WHO: White patch or plaque that does not rub off & cannot be diagnosed as any other disease • Associated use of tobacco Other probable factors: Candida, HPV-16, HPV-18 & Trauma
- 42. Gingival Cyst: Develop from odontogenic epithelium or traumatically implanted sulcular epithelium
- 43. 2. Malignant tumors of gingiva Squamous cell carcinoma: 12th - females • 90% of all Oral cancer • 6th –most common cancer in males • • Most common malignant tumor of gingiva
- 44. Malignant melanoma: • Rare tumor hard palate, maxillary gingiva -older persons • Darkly pigmented, rapid growth, early metastasis
- 45. Thankyou
- 47. Contents • Introduction • Classification • Indices • Inflammatory Enlargement • Enlargements associated with systemic diseases • Neoplastic enlargement • Drug-induced enlargement • Idiopathic gingival enlargement • False enlargement • Conclusion • References
- 48. Drug induced gingival enlargement • Side effect – non dental treatment • First case – Kimball 1939 Drugs associated with gingival overgrowth Anticonvulsants Phenytoin Sodium valproate Phenobarbitone Vigabatrin Immunosuppressants Cyclosporin Calcium channel blockers Dihydropyridines Nifedipine Felopdipine Amlodipine Phenylalkylamine Verapamil Benzothiazepine Diltiazem
- 49. Prevalence of DIGO • 50 % - phenytoin (Angelopoulous & Goaz 1972) • 30% - Cyclosporine • 10% - Nifedipine (Seymour 1987 , Barclay 1992) • In India, 57% of epileptic children - aged 8-13 years - phenytoin therapy Prasad et al 2002
- 50. Risk factors for DIGO Risk factors Age Sex Drug variables Concomitant medication Genetic factors Periodontal variables
- 51. •Early studies on phenytoin – teenagers , hospitalised or institutionalised •Two community based studies – 1. mean age 40.6 years – Thomason 1992 2.Younger age – Casetta 1997 •Cyclosporin - children (Daley 1994) •Calcium channel blockers – not applicable •Middle age and older Circulating androgen + gingival fibroblasts Testosterone – 5α dihydrotestosterone PHT – enhances metabolism Circulating androgen – adoloscents and teenagers Age
- 52. •Phenytoin – no difference Hassell 1981 •CsA- Male •CCBs – male 3 times more Sex Concomitant medication •Nifedipine + cyclosporin – increases prevalence but not the severity •Polypharmacy – PHT – metabolised by P450 •other anticonvulants – induce P450 isoenzyme
- 53. Drug variables 1. Drug dosage – poor predictor •Dose / pts body weight •PHT & CCB – therapeutic drug level 7-10 days •Cyclosporin – trough concentration •Area under plasma/ serum concentration time curve (AUC) 2. Type of preparation CsA– solution - 37 % - early onset – higher in saliva capsules – 43% (Wondimu 1996) 3. Salivary concentration PHT &CsA– salivary concentration positive correlation with OG 4. GCF – nifedipine
- 54. Genetic factors Cytochrome P450 gene polymorphism HLA- DR1 – protection against OG HLA-DR2 – OG susceptible Pernu 1994 Periodontal variables Plaque scores & gingival inflammation – exacerbate OG
- 55. General features of DIGO Painless beadlike enlargement of IDP Marginal gingiva Massive tissue fold Plaque control difficult Secondary inflammatory process Combined enlargement
- 56. • Generalised • Not in edentulous areas • Chronic , slow • Recurs • Discontinuation of drug – spontaneous reduction
- 57. Histopathology
- 58. Anticonvulsants • Epilepsy – • First antiepileptic drug – phenytoin – DOC • Merritt & Putman 1938 • 1st DIGO case • Active metabolite – 5 parahydroxyphenyl – 5 phenylhydantoin • Other hydantoins – ethotoin , mephenytoin • Other anticonsulvant – succinimides , valproic acid
- 59. Anticonvulsant properties 1. Reduces excessive discharge 2. Reduces spread of excitation Stabilising neuronal membrane Na – prevents influx K – blocks outward flow Ca – decreases calcium influx
- 60. • Clinical features 1. Esthetic disfigurement, 2. Malpositioning of teeth, 3. Interfere masticatory function, 4. Speech, 5. Oral hygiene
- 61. Theories of pathogenesis 1. Gingival fibroblasts 1. High activity 2. Low activity Hasell 1983
- 62. 2. Lack of collagen breakdown • FBS – inactive collagenase • mRNA collagenase levels are diminished • Gene expression of MMP-1, 2, and 3 was reduced by phenytoin administration, • the TIMP-1 mRNA was markedly augmented 2005, Kato et al • macrophages pretreated with phenytoin - lower production of MMPs • intracellular pathway - related to a lower expression of α2β1-integrin
- 63. 3. Non collagenous matrix • Non collagenous matrix – 20% of dry weight • Increased hexoamine , uronic acid • Increased sulphated GAG • Higher volume density of non collagenous protein compared to collagenous Dahllof et al 1984
- 64. 4. Role of growth factors • TGF-β - stimulating collagen biosynthesis • latency-associated protein (LAP) - TGF-β inactive • CTGF levels are increased • Epithelial mesenchymal transition • PDGF – PHT facilitated expression of PDGF B – 6 times
- 66. 5.Immunosuppression sIgA - decreased Repair process Gingival overgrowth
- 67. 6. PHT andAdrenal gland Suppression ofACTH production Suppression of adrenocortical function Reduction of glucocorticoid synthesis compensatory increase in the Somatotrophic hormone Fibroblast proliferation
- 68. 7. PHT and folic acid depletion Decreases absorption of folic acid Blocks transport - intestinal epithelium Enzyme folate reductase Folic acid – DNAsynthesis Impaired maturation – sulcular epithelium CT susceptible to inflammation
- 69. Cyclosporin induced gingival overgrowth • Cyclosporin (CsA) - 1972 James Borel • Organ transplantation , autoimmune disease • Monotherapy - CsA • 2 drugs – CsA+ cortisone / dihydropyridine • 3 drugs – CsA+ cortisone + azathiprine • Cyclosporin-induced gingival overgrowth – 1983 Rateitschak- Plu¨ss et al
- 70. Cyclosporin and T cells • a) Inhibits T cell helper function to accessory cells - interleukin 1 • b) Prevents the formation of receptors to interleukin I on the membrane of the T-cell. • c) Renders T-cells unresponsive to - interleukin 2 .
- 72. Pathogenesis of Cs GO Cyclosporin Cytokines Extracellular matrix metabolism Cell proliferation Apoptosis Synthesis Degradation -I/C pathway -E/C pathway
- 73. • More in labial aspect • Soft, red or bluish-red, extremely fragile and bleed easily, more hyperemic than PIGO
- 74. Histopathology
- 75. Calcium channel blockers • CCB’s introduced in 1980’s • Used extensively in the management of CV disorders(HTN, angina, coronary artery spasm, cardiac arrythmia) • NIFEDIPINE angina, mild to moderate HTN • Relaxes smooth muscles and dilates the coronary arteries • NIGO 1984 by Lederman et al
- 76. Pathogenesis: Nifedipine • Affects calcium metabolism similar to phenytoin • Role of TGF beta • Heparan GAG Verapamil Subpopulation of fibroblast
- 77. • IDPmarginal attached • Lobulated and nodular • Anteriorly, facial surface • Inflammation Combination enlargement
- 79. Idiopathic gingival enlargement • Gingivomatosis , Elephantiasis, Idiopathic fibromatosis, Hereditary gingival hyperplasia , Congenital familial fibromatosis , Hereditary gingival fibromatosis • rare oral disease • autosomal dominant • hypertrichosis, mental retardation and epilepsy
- 80. • Nodular form • Symmetric form- most common type • During eruption of permanent teeth
- 81. • most common effects • diastemas, • Malpositioning of teeth • prolonged retention of primary teeth • cover the dental crowns • the alveolar bone is not affected (Bittencourt et al. 2000).
- 83. TGF 1 Increased proliferation HGF cells Low levels of MMP 1, MMP 2 Myofibroblasts High level of extracellular matrix proteins (collagen) TGF 1 Gingival overgrowth
- 84. False enlargement a. Underlying osseous lesions • Commonly Tori, Exostosis • Also seen in Paget’s disease, Fibrous dysplasia, Cherubism, Central giant cell granuloma,Ameloblastoma, Osteoma and Osteosarcoma
- 85. b. Underlying dental lesions • Various stages of eruption of primary dentition labial gingiva • Developmental enlargement
- 86. Conclusion Gingival enlargement are multifactorial and complex in nature , which may be in respone to various interaction between host and environment. GO considerably reduce the quality of life and may result in serios emotional and social problems due to esthetics and functionality hence the prevention and treatment based on the understanding the cause and underlying pathologic changes ,
- 87. References • Newman MG , Takei HH , Klokkevold PR , Carranza FA . Carranza’s Clinical Periodontology, 10th edition • Marshall R , Bartold M A clinical review of drug induced gingival overgrowth Australian dental journal 1999 ;44:4 219- 232 • Seymour RA, Ellis JS, Thomason JM: Risk factors for drug- induced gingival overgrowth.J Clin Periodontol 2000; 27: 217– 223. • Seymour RA , Thomasan JM Pathogenesis of Drug Induced Gingival Overgrowth- J Clin Periodontol 1996;23:165-175 • Strawberry –like gingival tumor as first sign of Wegener’s Granulomatosis. J Periodontol 2008; 79: 1297-1303 • Seymour RA and Heasman PA: Drugs and the periodoniium. J Clin Periodontol 1988: 15: 1-16
- 88. • Jˆoice Dias Corrˆea et al Phenytoin-Induced Gingival Overgrowth: A Review of the Molecular, Immune, and Inflammatory Features ISRN Dentistry 2011,1-8 • Williamw . Hallmo&n J Effrey A. Rossmann The role of drugs in the pathogenesis of gingival overgrowth A collective review of current concepts Periodontology 2000, Vol. 21, 1999, 176-196 • Paulom. Camargo, Philip R.Melnick, Flavia Q. M. Pirih, Rodrigo Lagos & Henry H. Takei Treatment of drug-induced gingival enlargement: aesthetic and functional considerations Periodontology 2000, Vol. 27, 2001, 131–138 • Dustin Tedesco and Lukas Haragsim Cyclosporine: A Review Journal of Transplantation Volume 2012 • Bitu CC, Sobral LM, Kellermann MG, Martelli-Junior H, Zecchin KG, Graner E, Coletta RD. Heterogeneous presence of myofibroblasts in hereditary gingival fibromatosis. J Clin Periodontol 2006; 33: 393–400
- 89. Thankyou