Distraction osteogenesis in CLP
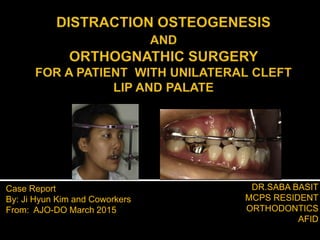
- 1. DR.SABA BASIT MCPS RESIDENT ORTHODONTICS AFID Case Report By: Ji Hyun Kim and Coworkers From: AJO-DO March 2015
- 3. 12/17/2016 3Medscape “A process in which increased amount of both bone and soft tissue are created as a result of the gradual displacement of surgically created bony fractures.” “A process used in orthopedic surgery and oral and maxillofacial surgery to repair skeletal deformities and in reconstructive surgery.” Also called ‘callus distraction’ ‘callotasis’ ‘Osteodistraction’ DO
- 4. “Distraction osteogenesis is a way to make a longer bone out of a shorter one.” 12/17/2016 4seattlechildrens.org
- 5. 12/17/2016 March 2015,Vol 147,Issue 3 5
- 6. 12/17/2016 March 2015,Vol 147,Issue 3 6
- 7. 22yrs old female Korean woman 12/17/2016 March 2015,Vol 147,Issue 3 7
- 8. Depressed upper lip Protruded lower jaw Midline deviation 12/17/2016 March 2015,Vol 147,Issue 3 8
- 9. Born with a complete unilateral CLP Received a cheilorrhaphy and a palatorrhaphy when she was 10 years old No history of orofacial congenital anomalies or deformities in her family No other relevant medical history 12/17/2016 March 2015,Vol 147,Issue 3 9
- 10. Midface deficiency Increased mandibular body length Lower facial height comparatively longer than midfacial height The length of the mental region was much greater than that of the upper lip 12/17/2016 March 2015,Vol 147,Issue 3 10
- 11. 12/17/2016 March 2015,Vol 147,Issue 3 11
- 12. Angle class III molar Anterior crossbite Maxillary jaw deviated to the right Missing maxillary second premolars Palatally ectopic maxillary right first premolar Maxillary dental midline deviated by 3mm Peg laterals 12/17/2016 March 2015,Vol 147,Issue 3 12
- 13. Reverse overjet 12/17/2016 March 2015,Vol 147,Issue 3 13
- 14. Original cleft defect in the maxillary left lateral incisor area Potentially impacted 3rd molars Multiple restorations 12/17/2016 March 2015,Vol 147,Issue 3 14
- 15. Skeletal class III relationship with a retrognathic maxilla. Hyperdivergent skeletal pattern. Retrusive upper lip shows high value of z-angle Bimax retroclinations 12/17/2016 March 2015,Vol 147,Issue 3 15
- 16. 12/17/2016 March 2015,Vol 147,Issue 3 16
- 17. The midface anteroposterior deficiency The maxillary Jaw deviation to the right The skeletal class III relationship and improve the facial profile The class III molar relationship and the anterior crossbite March 2015,Vol 147,Issue 3 17 TOCORRECT
- 18. 1. Orthodontic and Surgical treatment (Maxillary advancement with posterior impaction and mandibular setback) 2. Orthodontic with Distraction Osteogenesis and Orthognathic Surgery. (The maxillary advancement with DO followed by orthognathic surgery to posteriorly impact the maxilla and set back the mandible.) 12/17/2016 March 2015,Vol 147,Issue 3 18 Considering the severity of the skeletal discrepancy, the second option was chosen as a potentially more stable treatment method.The RED device was planned to be used to accomplish the maxillary DO.
- 19. 12/17/2016 March 2015,Vol 147,Issue 3 19 Disadvantages of Orthognathic Surgery in severe maxillary deficiency •Relapse rates of 25% to 40% •Instability •Limited amount of advancement •Highly invasive surgical technique
- 20. 12/17/2016 March 2015,Vol 147,Issue 3 20 Distraction Osteogenesis Predistraction phase Distraction and consolidation phase Post distraction phase Preoperative Orthodontics Orthognathic Surgery
- 21. Intraoral appliance fabricated Orthodontic bands Vertical wires with hooks soldered perpendicular to the labial wire Two additional short vertical wires with hooks were also soldered to the labial wire at the position of the canines. 12/17/2016 March 2015,Vol 147,Issue 3 21
- 22. 12/17/2016 March 2015,Vol 147,Issue 3 22
- 23. 12/17/2016 March 2015,Vol 147,Issue 3 23 Complete maxillary osteotomy A RED system with 3 screws on each side of cranium. The extraoral hooks were tied to the vertical pin of the RED device. Latency period of 8 days Distraction at the rate of 0.5 mm twice per day for 10 days Intraoral device maintained till 8 weeks
- 24. The extra-oral portion was cut Facemask for an additional 2 months to minimize relapse Force approximately 340 g (12 oz) with 2 heavy elastics 5/16 inc per side. 12/17/2016 March 2015,Vol 147,Issue 3 24
- 25. Preadjusted fixed appliances Preoperative orthodontics #14 was extracted. Aligning and leveling Decompensation 12/17/2016 March 2015,Vol 147,Issue 3 25
- 26. 12/17/2016 March 2015,Vol 147,Issue 3 26
- 27. Lefort I Osteotomy 1. 5 mm of advancement, 2. 3 mm of posterior impaction, 3. Horizontal rotation for midline correction Mandible set back 6mm bilateral sagittal split ramus osteotomy Genioplasty 12/17/2016 March 2015,Vol 147,Issue 3 27
- 28. 12/17/2016 March 2015,Vol 147,Issue 3 28
- 29. Appliances were removed Lingual fixed retainers Mandibular right second molar was splinted with adjacent tooth Removable wraparound retainers 12/17/2016 March 2015,Vol 147,Issue 3 29
- 30. 12/17/2016 March 2015,Vol 147,Issue 3 30
- 31. The total maxillary advancement with DO was 10 mm Since 2-jaw surgery with mandibular setback was planned from the beginning, no further maxillary advancement through DO was performed. 12/17/2016 March 2015,Vol 147,Issue 3 31
- 32. 12/17/2016 March 2015,Vol 147,Issue 3 32
- 33. 12/17/2016 March 2015,Vol 147,Issue 3 33 Total 7 mm of maxillary advancement
- 34. The posttreatment extraoral photographs showed a balanced profile. 12/17/2016 March 2015,Vol 147,Issue 3 34
- 35. The intraoral photographs demonstrated good alignment with acceptable overjet and overbite. 12/17/2016 March 2015,Vol 147,Issue 3 35
- 36. Midline discrepancy was corrected. The molar relationship on the right side, class III. The molar relationship on the left side, class I. 12/17/2016 March 2015,Vol 147,Issue 3 36
- 37. The final cephalometric analysis: Improved profile Reduced mandibular body length Long mental region reduced Maxillary incisors remained retroclined Improved madibular incisor incliniation 12/17/2016 March 2015,Vol 147,Issue 3 37
- 38. Total treatment time 36 months 2-year posttreatment photographs and the cephalometric analysis showed good stability. Pt. was satisfied 12/17/2016 March 2015,Vol 147,Issue 3 38
- 39. 12/17/2016 March 2015,Vol 147,Issue 3 39
- 40. Patient’s strong concern 1. Midline coincidence 2. Improvement of lateral facial profile She decided to have: 2-jaw surgery Of 10 mm, the true amount of distraction achieved was 7 mm. The 10-mm distraction with the RED device used in this patient was insufficient. 12/17/2016 March 2015,Vol 147,Issue 3 40
- 41. Severe retrusion of the maxilla Dental midline deviation of 3 mm Lack of maxillary incisal exposure and upper lip support Depression of the nasolabial folds 12/17/2016 March 2015,Vol 147,Issue 3 41
- 42. RED appliance allows 3-plane guidance. Considering the occlusal plane angle and the maxillary incisal exposure ,it is intended to induce the force vector of the DO to be forward and downward by adjusting the length of the vertical hook. 12/17/2016 March 2015,Vol 147,Issue 3 42
- 43. The distraction vector can be controlled by both the external device and the intraoral device of the RED system 12/17/2016 March 2015,Vol 147,Issue 3 43
- 44. 12/17/2016 March 2015,Vol 147,Issue 3 44 In this patient, the amount of advancement needed was more than 10 mm; therefore, orthognathic surgery alone was considered insufficient and unstable. 10mm
- 45. Suggested retention period for DO 6 to 8 weeks. Red device 8 weeks of consolidation and 8 weeks of retention with the facemask to prevent relapse as much as possible. The 2.4 mm of relapse occurred during the preoperative orthodontic treatment 1. There was no supplementary appliance for retention 2. Soft tissue factors and muscle stretch 12/17/2016 March 2015,Vol 147,Issue 3 45
- 46. Patient had secondary caries on all 4 maxillary molars. To strengthen the anchorage, banding of all 4 molars was planned. For a patient with multiple missing teeth or not enough bone in the cranial vault, mini implants or plates could be considered for the skeletal anchorage. 12/17/2016 March 2015,Vol 147,Issue 3 46
- 47. Louis et al says that relapse rate of OGS increases as the amount of maxillary advancement increase. 12/17/2016 March 2015,Vol 147,Issue 3 47
- 48. According to some studies, the maximum maxillary advancement achieved by conventional OGS techniques varies, ranging from 5mm - 10mm,depending upon scar contracture. 12/17/2016 March 2015,Vol 147,Issue 3 48
- 49. 12/17/2016 March 2015,Vol 147,Issue 3 49 In our patient, 2.4 mm of relapse, which is about 34% of the total amount of advancement, occurred during the preoperative orthodontic treatment According to Hochban et al, Cheung et al, Erbe et al reported that relapse rate after maxillary advancement of 7.8mm,3.3mm and 4.6mm was 25%,27% and 40% respectively.
- 50. 12/17/2016 March 2015,Vol 147,Issue 3 50 Overcorrection during DO is suggested Cho and Kyung et al. recommended overcorrection is of 20% to 30% to minimize relapse.
- 51. DO is an efficient treatment modality in severe cleft-related maxillary hypoplasia. It promotes correction of bone and soft tissues simultaneously. Reduces the amount of maxillary movement during the surgery. 12/17/2016 March 2015,Vol 147,Issue 3 51
- 52. 12/17/2016 52 TITLE Distraction osteogenesis and orthographic surgery for a patient with unilateral cleft lip and palate STUDY DESIGN Case report STATISTICS USED Not Applicable DATA ANALYSIS Not Applicable LEVEL OF EVIDENCE 5 CONCLUSION DO is an efficient treatment modality in cleft-related maxillary hypoplasia. LIMITATIONS Single case RCT’s are not there Experimental study INFERENCE Such type of studies are already being conducted in our setup, they need to be continued.
- 53. 12/17/2016 March 2015,Vol 147,Issue 3 53
- 54. 12/17/2016 March 2015,Vol 147,Issue 3 54
- 55. 12/17/2016 March 2015,Vol 147,Issue 3 55
- 56. 12/17/2016 March 2015,Vol 147,Issue 3 56
- 57. 12/17/2016 March 2015,Vol 147,Issue 3 57
