Improving Outcomes for Patients With Refractory Rheumatoid Arthritis: The Role of JAK Inhibitors.
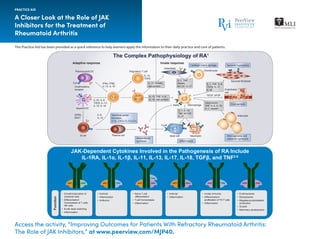
- 1. This Practice Aid has been provided as a quick reference to help learners apply the information to their daily practice and care of patients. A Closer Look at the Role of JAK Inhibitors for the Treatment of Rheumatoid Arthritis PRACTICE AID Access the activity, “Improving Outcomes for Patients With Refractory Rheumatoid Arthritis: The Role of JAK Inhibitors,” at www.peerview.com/MJP40. JAK2/TYK2 JAK2/JAK2JAK1/JAK2JAK1/JAK2/TYK2JAK1/TYK2JAK1/JAK3• Growth/maturation of lymphoid cells • Differentiation/ homeostasis of T cells, NK cells • B-cell class switching • Inflammation • Antiviral • Inflammation • Antitumor • Naïve T-cell differentiation • T-cell homeostasis • Inflammation • Antiviral • Inflammation • Innate immunity • Differentiation/ proliferation of Th17 cells • Inflammation • Erythropoiesis • Myelopoiesis • Megakaryocyte/platelet production • Growth • Mammary development Function JAK1 JAK1 JAK1 JAK1 JAK2 JAK2 TYK2 JAK2 JAK2 TYK2 JAK2TYK2JAK3 The Complex Pathophysiology of RA1 JAK-Dependent Cytokines Involved in the Pathogenesis of RA Include IL-1RA, IL-1α, IL-1β, IL-11, IL-13, IL-17, IL-18, TGFβ, and TNF2-6 Adaptive response Plasmacytoid DC TLR Costimulatory receptor IFNα, IFNβ, IL-15, IL-18 Regulatory T cell IL-10, TGFβ IL-23, IL-6, TGFβ, IL-12, IL-15, IL-18 TH0 TH17 (or TH1) APRIL, BAFF IL-6, IL-10 Germinal-center formation (LTβ, CXCL13, CCL21) B cell Plasma cell Myeloid DC Autoantibody synthesis Cartilage matrix damage Innate response Synovial hyperplasia Osteoblast Chondrocyte Synovial fibroblast PAR2 Macrophage VEGF, bFGF Endothelial cell Angiogenesis Adipocyte FcγR Mast cell Neutrophil Inflammation Atherogenesis and metabolic syndrome IL-17, RANKL, cell contact IL-15, TNF, IL-6, IL-18, cell contact IL-1, TNF, RANKL, M-CSF, IL-17 IL-1, IL-18, TNF, M-CSF, IL-17 IL-1, TNF, IL-6, TGFβ, IL-17, IL-32 Adiponectin, TNF, IL-6, IL-15, IL-1, resistin
- 2. A Closer Look at the Role of JAK Inhibitors for the Treatment of Rheumatoid Arthritis APRIL: A proliferation-inducing ligand; BAFF: B-cell activating factor; bFGF: basic fibroblast growth factor; CCL21: C-C motif chemokine ligand 2; CXCL: CXC chemokine ligand; DC: dendritic cells; csDMARDs: conventional synthetic disease-modifying antirheumatic drugs; DMARDs: disease-modifying antirheumatic drugs; FCyR: Fc-gamma receptor; IFN: interferon; IL: interleukin; IL-1RA: interleukin 1 receptor antagonist; IR: incidence rates; JAK: Janus kinase; LTβ: lymphotoxin-beta; M-CSF: macrophage colony-stimulating factor; MTX: methotrexate; NK: natural killer (cells); PAR2: proteinase-activated receptor-2; RANKL: receptor activator of nuclear factor-ΚB ligand; STAT: signal transducers and activators of transcription; TGFβ: transforming growth factor beta; Th17: T helper 17 (cells); TLR: toll- like receptors; TNF: tumor necrosis factor; URTI: upper respiratory tract infection; VEGF: vascular endothelial growth factor. 1. McInnes IB, Schett G. Nat Rev Immunol. 2007;7:429-442. 2. Ghoreschi K et al. J Immunol. 2011;186:4234-4243. 3. Kontzias A et al. Curr Opin Pharmacol. 2012;12:464-470. 4. McInnes IB, Schett G. N Engl J Med. 2011;365:2205-229. 5. O’Sullivan LA et al. Mol Immunol. 2007;44:2497-2506. 6. Vijayakrishnan L et al. Trends Pharmacol Sci. 2011;32:25-34. 7. Louder A et al. Am Health Drug Benefits. 2016;9:84-93. 8. Alten R et al. Patient Prefer Adherence. 2016;10:2217-2228. 9. https://www.accessdata.fda.gov/drugsatfda_docs/ label/2016/208246s000lbl.pdf. Accessed September 6, 2018. 10. https://www.accessdata.fda.gov/drugsatfda_docs/label/2018/207924s000lbl.pdf. Accessed September 6, 2018. 11. https://clinicaltrials.gov. Accessed September 6, 2018. PRACTICE AID Access the activity, “Improving Outcomes for Patients With Refractory Rheumatoid Arthritis: The Role of JAK Inhibitors,” at www.peerview.com/MJP40. • Treatment with biologic agents results in disease suppression for many patients with RA, but only ~30% achieve complete remission; and the majority of patients treated with biologics experience disease exacerbation following cessation of treatment • The route of administration is also an important consideration, with some studies suggesting that patients may prefer oral therapies over those with other routes of administration • Given the important role played by JAK-STAT signaling in the development of RA and other autoimmune conditions, small-molecule JAK inhibitors have been proposed as an important treatment option JAK Inhibitors Currently in Phase 3 Development for the Treatment of RA11 Filgotinib (FINCH program) Peficitinib (RAJ program) Upadacitinib (SELECT program) Why Is There a Need for JAK Inhibitors in the RA Treatment Landscape?7,8 Approved JAK Inhibitors for the Treatment of RA Overview Efficacy in Specific Clinical Scenarios Monotherapy + csDMARDs MTX-IR After anti-TNF failure Tofacitinib9 • Approval date: November 2012 • JAK selectivity: JAK1 and JAK3 • Indication: Treatment of adult patients with moderately to severely active RA who have had an inadequate response or intolerance to MTX; may be used as monotherapy or in combination with MTX or other nonbiologic DMARDs • Most common side effects: URTI, nasopharyngitis, diarrhea, and headache Barcitinib10 • Approval date: May 2018 • JAK selectivity: JAK1 and JAK2 • Indication: Treatment of adult patients with moderately to severely active RA who have had an inadequate response to one or more TNF-antagonist therapies • Most common side effects: URTI, nausea, cold sores, and shingles
- 3. This Practice Aid has been provided as a quick reference to help learners apply the information to their daily practice and care of patients. The Impact of Rheumatoid Arthritis on Patients1 RA: rheumatoid arthritis. 1. https://rheumatoidarthritis.net/infographic/ra-not-just-joints-or-bones-but-so-much-more/. Accessed August 31, 2018. PRACTICE AID Access the activity, “Improving Outcomes for Patients With Refractory Rheumatoid Arthritis: The Role of JAK Inhibitors,” at www.peerview.com/MJP40. Apart from joint pain, there are many more symptoms patients may experience 73% of patients wish they had known more about all RA symptoms when they were first diagnosed Also affected: heart, skin, kidneys, and lungs RA impacts various body parts, joint pain being a key symptom At diagnosis, 66% of patients reported wishing they knew more about the impact RA can have on mental health Hands and wrists 95% Fingers 88% Feet 84% Legs and knees 78% Shoulders 70% Ankles 66% Hips 66% Arms and elbows 65% Neck 55% Back 52% Eyes 45% Head and jaw 40% Chest 21% 19% initially experienced anxiety and/or depression 53% actively experience anxiety and/or depression 25% actively experience mood disorder Patients report that rheumatoid arthritis negatively impacts: Exercise 70% Household/family duties 64% Sleep 61% Work 61% Social life/participating in activities 59% Osteoarthritis and obesity are the most common of other health conditions 95% of patients suffer from other health conditions Chronic pain 41% Hypertension 37% Neuropathy 34% Fibromyalgia 31% Dental issues 31% Sleep disorders 23% Sjörgren’s syndrome 17% Heart disease 7% Fatigue 89% Reduced grip strength 70% Difficulty sleeping 67% Cognitive impairment 54% Visual symptoms 51% Numbness/ tingling 47% Dry mouth 42%
