Ineffective Breathing Pattern Nursing Care Plan
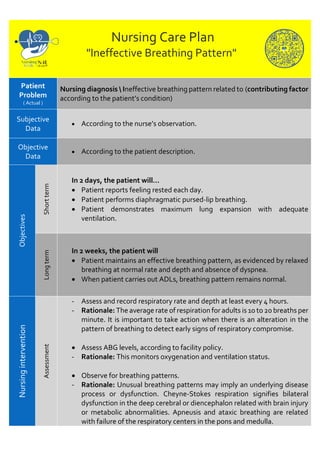
- 1. Nursing Care Plan "Ineffective Breathing Pattern" Patient Problem ( Actual ) Nursing diagnosis Ineffective breathing pattern related to (contributing factor according to the patient’s condition) Subjective Data According to the nurse’s observation. Objective Data According to the patient description. Objectives Short term In 2 days, the patient will… Patient reports feeling rested each day. Patient performs diaphragmatic pursed-lip breathing. Patient demonstrates maximum lung expansion with adequate ventilation. Long term In 2 weeks, the patient will Patient maintains an effective breathing pattern, as evidenced by relaxed breathing at normal rate and depth and absence of dyspnea. When patient carries out ADLs, breathing pattern remains normal. Nursing intervention Assessment - Assess and record respiratory rate and depth at least every 4 hours. - Rationale: The average rate of respiration for adults is 10 to 20 breaths per minute. It is important to take action when there is an alteration in the pattern of breathing to detect early signs of respiratory compromise. Assess ABG levels, according to facility policy. - Rationale: This monitors oxygenation and ventilation status. Observe for breathing patterns. - Rationale: Unusual breathing patterns may imply an underlying disease process or dysfunction. Cheyne-Stokes respiration signifies bilateral dysfunction in the deep cerebral or diencephalon related with brain injury or metabolic abnormalities. Apneusis and ataxic breathing are related with failure of the respiratory centers in the pons and medulla.
- 2. Auscultate breath sounds at least every 4 hours. - Rationale: This is to detect decreased or adventitious breath sounds. Ask if they are “short of breath” and note any dyspnea. - Rationale: Sometimes anxiety can cause dyspnea, so watch the patient for “air hunger” which is a sign that the cause of shortness of breath is physical. Assess for use of accessory muscle. - Rationale: Work of breathing increases greatly as lung compliance decreases. Monitor for diaphragmatic muscle fatigue or weakness (paradoxical motion). - Rationale: Paradoxical movement of the abdomen (an inward versus outward movement during inspiration) is indicative of respiratory muscle fatigue and weakness. Observe for retractions or flaring of nostrils. - Rationale: These signs signify an increase in respiratory effort. Assess the position that the patient assumes for breathing. - Rationale: Orthopnea is associated with breathing difficulty. Utilize pulse oximetry to check oxygen saturation and pulse rate. - Rationale: Pulse oximetry is a helpful tool to detect alterations in oxygenation initially; but, for CO2 levels, end tidal CO2 monitoring or arterial blood gases (ABGs) would require being obtained. Assess ability to mobilize secretions. - Rationale: The incapability to mobilize secretions may contribute to change in breathing pattern. Evaluate skin color, temperature, capillary refill; observe central versus peripheral cyanosis. - Rationale: Lack of oxygen will cause blue/cyanosis coloring to the lips, tongue, and fingers. Cyanosis to the inside of the mouth is a medical emergency!
- 3. Assess for thoracic or upper abdominal pain. - Rationale: Pain can result shallow breathing. Interventions Place patient with proper body alignment for maximum breathing pattern. - Rationale: A sitting position permits maximum lung excursion and chest expansion. Encourage sustained deep breaths by: Using demonstration: highlighting slow inhalation, holding end inspiration for a few seconds, and passive exhalation Utilizing incentive spirometer Requiring the patient to yawn - Rationale: These techniques promotes deep inspiration, which increases oxygenation and prevents atelectasis. Controlled breathing methods may also aid slow respirations in patients who are tachypneic. Prolonged expiration prevents air trapping Encourage diaphragmatic breathing for patients with chronic disease. - Rationale: This method relaxes muscles and increases the patient’s oxygen level. Evaluate the appropriateness of inspiratory muscle training. - Rationale: Thistraining improvesconscious control of respiratory muscles and inspiratory muscle strength. Provide respiratory medications and oxygen, per doctor’s orders. - Rationale: Beta-adrenergic agonist medications relax airway smooth muscles and cause bronchodilation to open air passages. Avoid high concentration of oxygen in patients with COPD. - Rationale: Hypoxia triggers the drive to breathe in the chronic CO2 retainer patient. When administering oxygen, close monitoring is very important to avoid uncertain risings in the patient’s PaO2, which could lead to apnea. Maintain a clear airway by encouraging patient to mobilize own secretions with successful coughing. - Rationale: This facilitates adequate clearance of secretions. Encourage small frequent meals. - Rationale: This prevents crowding of the diaphragm.
- 4. Health Teaching Educate patient or significant other proper breathing, coughing, and splinting methods. - Rationale: These allow sufficient mobilization of secretions. Educate patient about medications: indications, dosage, frequency, and possible side effects. Incorporate review of metered-dose inhaler and nebulizer treatments, as needed. - Rationale: This information promotes safe and effective medication administration. Teach patient about: pursed-lip breathing abdominal breathing performing relaxation techniques performing relaxation techniques taking prescribed medications (ensuring accuracy of dose and frequency and monitoring adverse effects) scheduling activities to avoid fatigue and provide for rest periods - Rationale: These measures allow patient to participate in maintaining health status and improve ventilation. Evaluation Achieved ( ) Partially achieved ( ) Not achieved ( ) Evidence by: Important Note "We just recommend examples of nursing care plans. There are many references and interventions may change according to patient condition. You should consider this, search, and see more than one reference to reach the best quality for writing the care plan"
