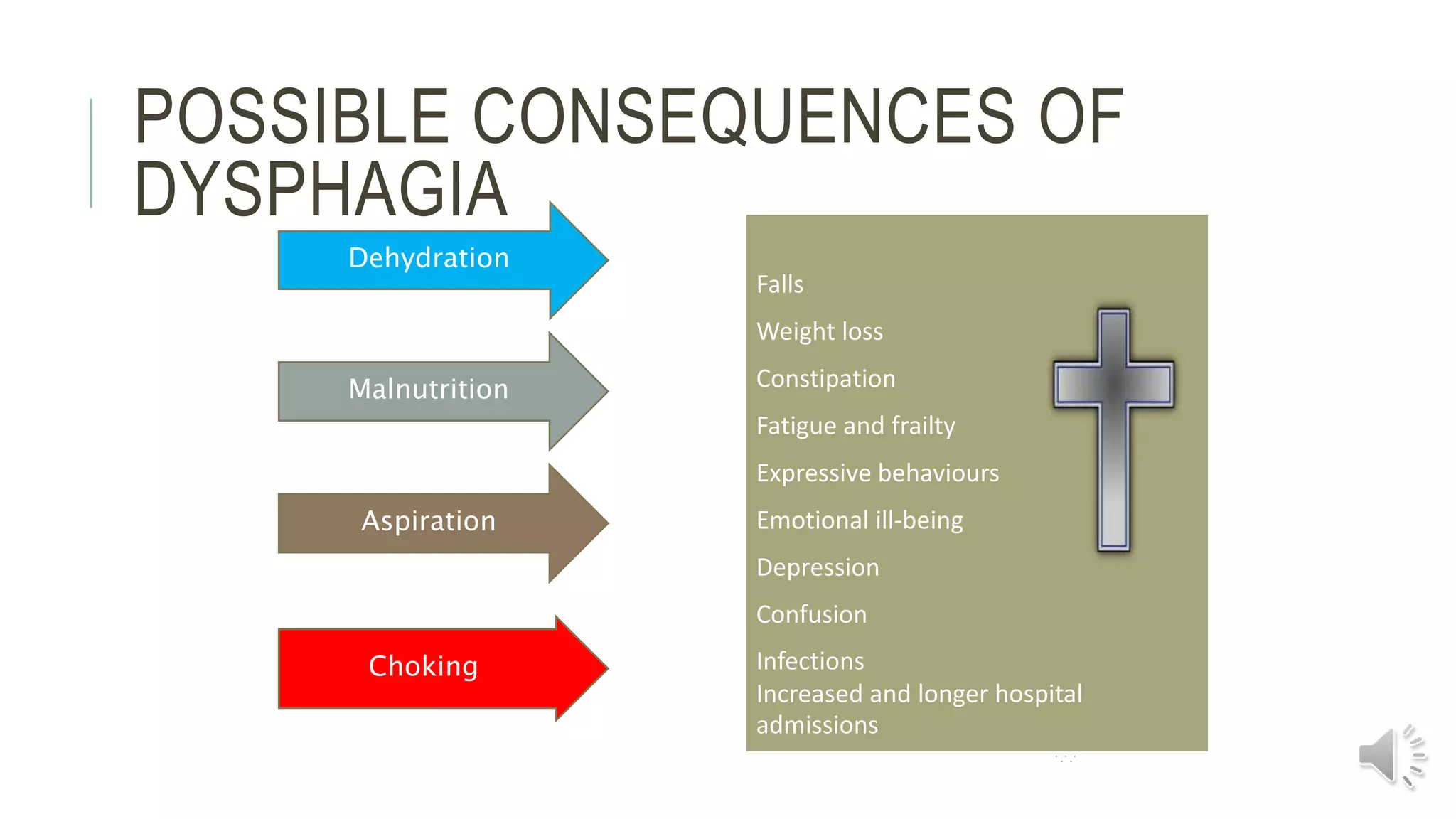
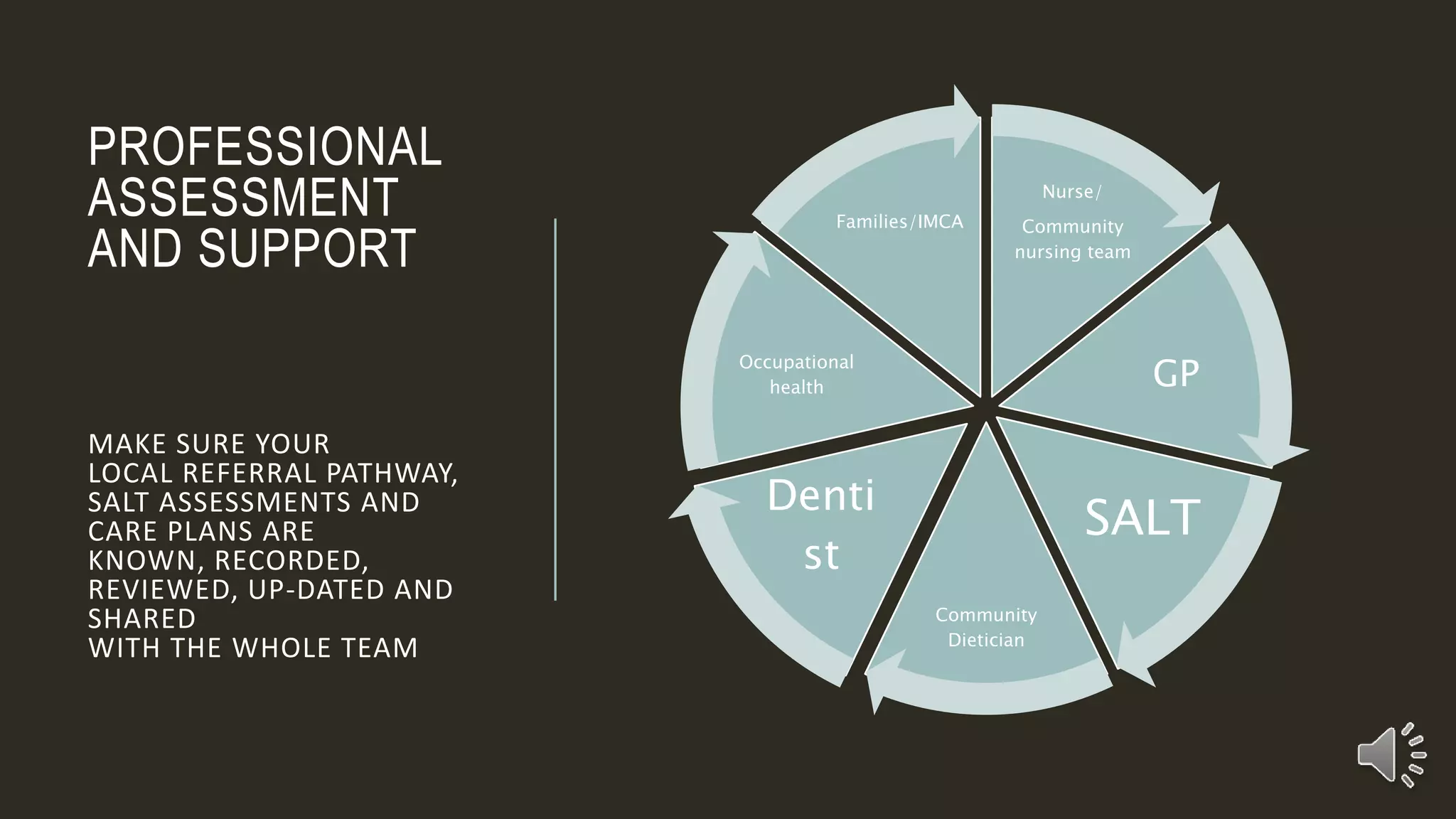
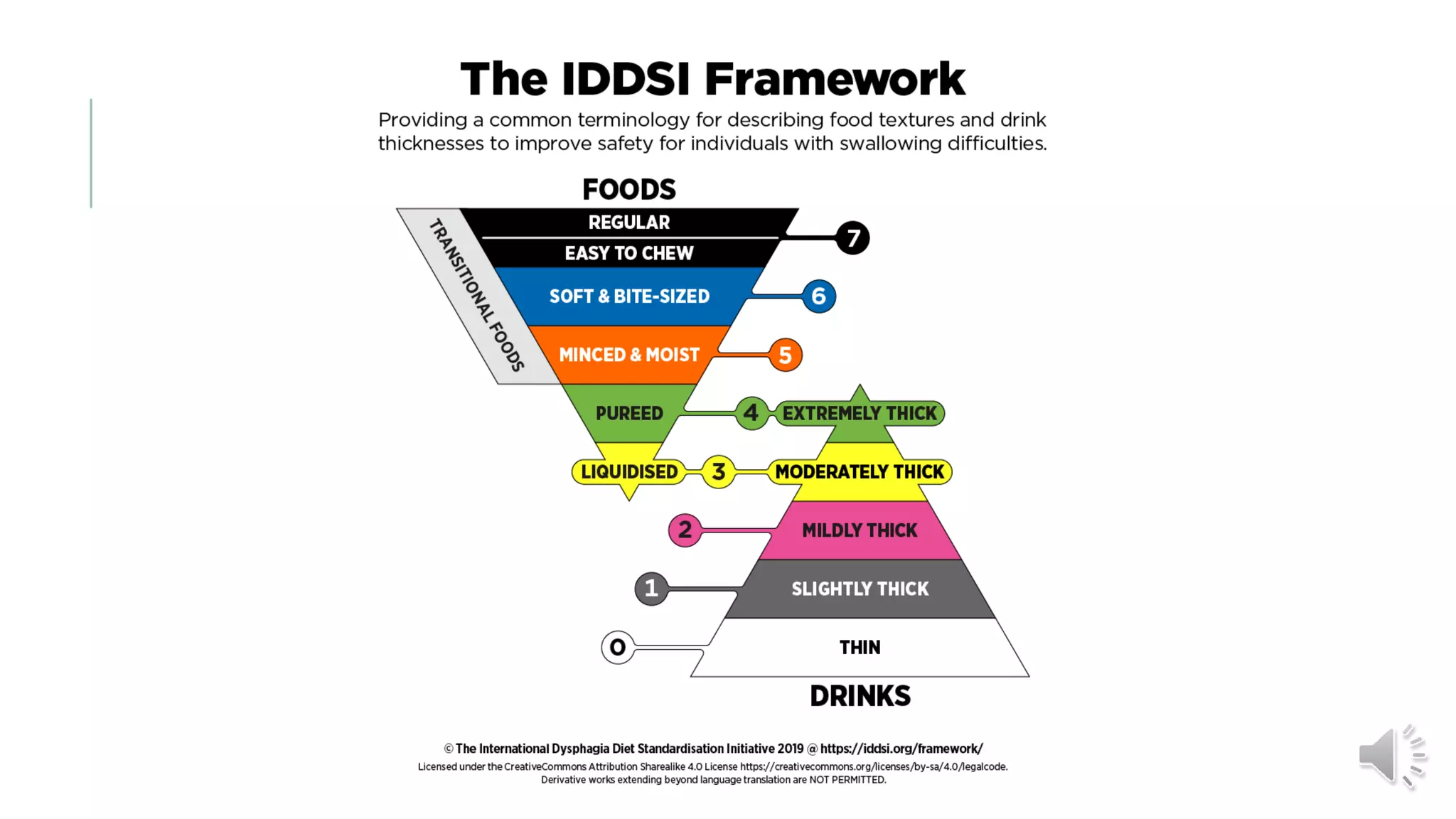
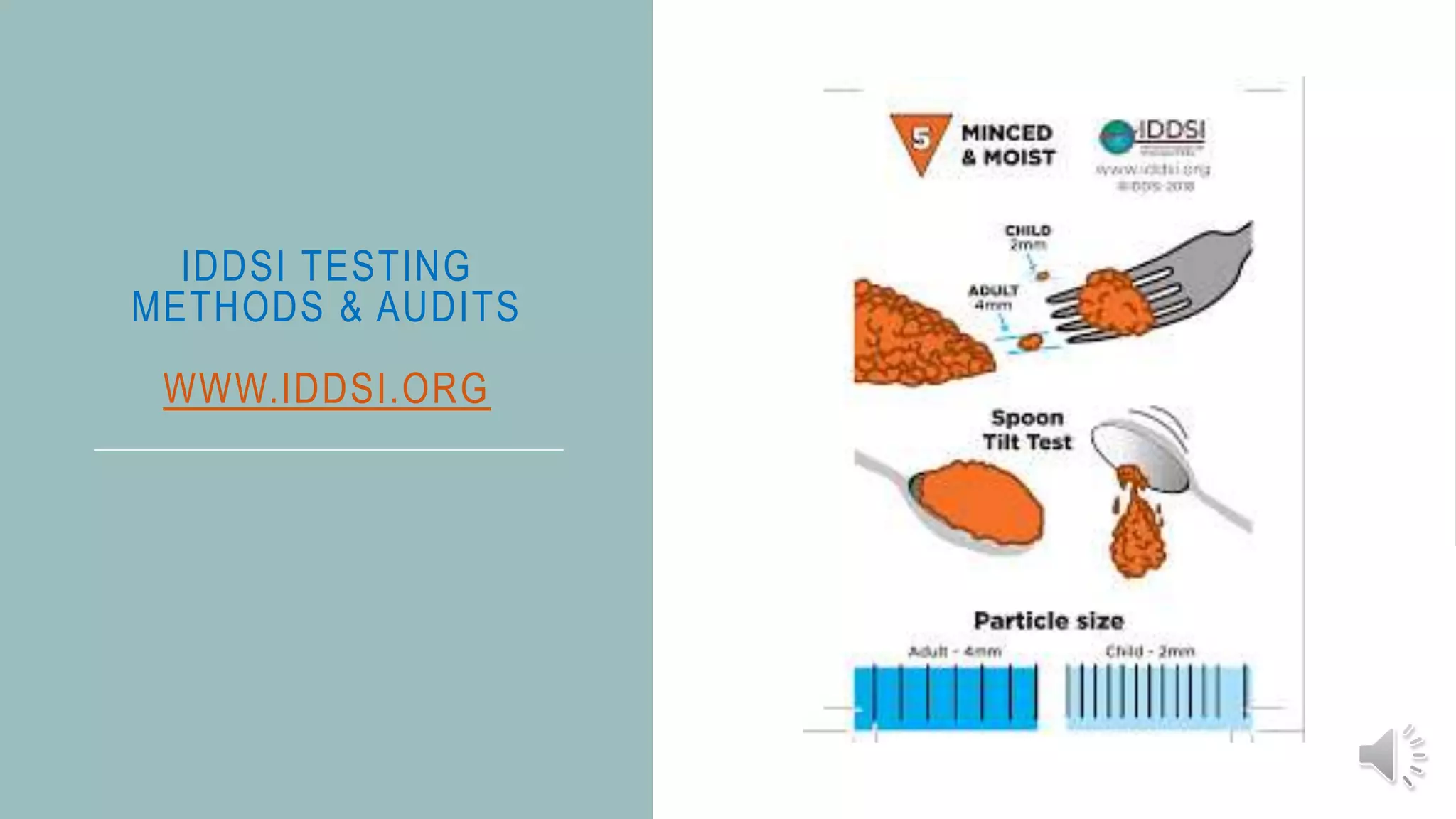
The document provides information on dysphagia (difficulty swallowing) and the International Dysphagia Diet Standardization Initiative (IDDSI) framework for classifying and describing texture-modified foods and thickened liquids for people with swallowing difficulties. It notes that over 51% of people in residential care have dysphagia, which can result in harm or death if not managed properly. It summarizes the IDDSI levels from 0 to 7 and emphasizes that staff must be trained to recognize dysphagia, manage risks, and prepare foods and liquids according to the correct IDDSI descriptors to help prevent choking and other complications. Resources and actions for implementing IDDSI standards are also outlined.