Human reproductive system BY Manoj Dhital(M.Sc Medical Microbiology))
- 2. Reproductive system • It is a natural phenomenon by which organism reproduce young ones of their own kinds for continuation of race. • Human beings are unisexual or dioecious i.e. male and female reproductive system is separated in separate individual.
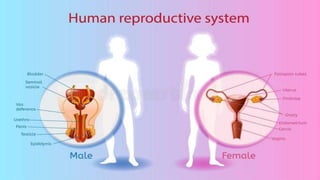
- 3. Male reproductive organs 1. Testes (one pair) 2. Epididymis (one pair) 3. Vasa deferens (one pair) 4. Ejaculatory duct (one pair) 5. Urethra. 6. Penis. 7. Accessory glands [Seminal vesicles, prostate gland, cowper’s gland] UrethraPenis
- 4. i. Testes: • pinkish-oval, lie inside the scrotum (scrotal sac). • scrotum lies outside the abdominal cavity so that temperature of testes remains 20c-30c below than temperature of body which is essential to produces sperm. Microscopic structure: • There are three layers to cover testes. • These are Outer-tunica vaginalis, Middle-tunica albugania and Inner-tunica vasculosa.
- 5. • There are 200-300 testicular lobules in testis. • Each lobule is composed of 1 to 4 coiled seminiferous tubules. • Each seminiferous tubule is of 75 cm. seminiferous tubules opens into tubuli recti which forms small tubules called rete testis. • These tubules of rete ends into 12-20 ducts called efferent ductules of vasa efferentia. • They merge to form 6 meter long ductus deferens which enters into the head of epididymis. • Seminiferous tubules are lined with germinal epithelial cells. • These are of two types; spermatogenic cells, which produce spermatozoa or sperms by spermatogenesis and sertoli cells which nourishes the developing sperms. • In between seminiferous tubules there are connective tissue which bears interstitial cells (cells of leydig). • The interstitial cells produce androgens (testosterone), which promotes development of male accessory glands and controls male sex features (moustache, beard, change of voice).
- 6. ii. Epididymis: • It is funnel like convoluted about 6 meters long tube. Board part of anterior epididymis is called caput epididymis. • Middle narrow part is corpus epididymis posterior end is cauda epididymis. • Function: store the sperm and secrets fluid to nourish sperm. iii. Vasa deferens: • It arises from cauda. It is 40 cm long. It forms a loop around urinary bladder and joins with duct of seminal vesicle and forms ejaculatory duct with seminal vesicle and opens into urethra. • Function: Carry sperm from testis to seminal vesicles. iii. Ejaculatory duct: • There are two short tubes of 2cm long formed by the union of duct from a seminal vesicle and vasa deferens, there carry the mixture of sperm and secretion of seminal vesicle. v. Urethra: • It is 20 cm long arises from urinary bladder. It discharges both urine and semen.
- 7. vi. Penis: • It is copulatory organ of human. It is made up of three columns of spongy tissues (two dorsal cavernosa and one ventral corpora spongiosum). • Enlarged-tip of penis is called glans penis which is highly sensitive. • Penis deposits the semen in vagina with spermatozoa.
- 8. vii. Accessory glands: a. Seminal vesicles: • These are two pouches like below-posteriorly of urinary bladder and opens into ejaculatory duct. • These secret a viscous fluid which keep sperms alive. b. Prostate gland: • It lies behind urinary bladder. It is secretes thin milky substance occupy 15-30% volume of semen. c. Cowper’s glands: • The paired glands lie below the prostate glands. Their alkaline secretion serves as lubricant. Erection of penis: • Erection is caused by dilation of blood vessel of blood vessel resulting collection of more blood spaces of spongy tissue. • During copulation or sexual intercourse penis releases semen on vagina called ejaculation. • About 3ml of semen is discharged by penis in each ejaculation. Semen : • Composition; Sperm + secretion of seminal vesicles, prostate gland & Cowper’s gland • PH= 7.5, 1ml of semen contains 100 millions of sperms(spermatozoa)
- 9. Female reproductive organs • Female reproductive organs are, 1. Ovaries 2. Fallopian tubes (oviduct) 3. Uterus 4. Vagina 5. Vulva 6. Acessory glands [Bartholin’s gland & mammary gland (breast)]
- 10. 1. Ovaries: • There is one pair of about 2.5-3.5cm long, pink, almond shaped and situated in abdominal cavity on either side of vertebral column. • Each ovary is attached to upper part of uterus by an ovarian ligament. • It is attached to dorsal body wall by mesovarium. • Internally each ovary is differentiate with i. Outer germinal epithelium : lined with cuboidal cells. ii. Tunica albunginea: connective tissue below germinal epithelium. iii. Stroma: Inner mass of connective tissues made up of cortex & medulla. • Throughout the cortex, there are about 4,00,000 ovarian follicles which are developed from germinal epithelial cells. • A fully matured ovarian follicle is known as graafian follicle (also called secondary oocyte). • A fully matured graffian follicle has an outer sheath membrane granulosa which encloses a follicular cavity filled with colourless fluid. • Inside the follicular cavity an ovum is situated. Ovum is surrounded by transparent layers- zona pellucida and zona radiate. • The fully matured graafian follicle releases ovum upon rupture of ovary. The release of ovum from ovary is called ovulation. • Then the cavity of ruptured follicle now get filled with blood clot to form corpus luteum. • It functions as endocrine gland which secrets a hormone called progesterone which activates the uterus and mammary gland for their development. • Gradually the corpus luteum reduced in size to form corpous albicans.
- 11. 2. Fallopian tubes (oviducts): • These are ciliated tubes of 10-12cm long arises near the ovary and extends to uterus. It is composed of outer serosa, middle muscularis and inner mucosa. • A fallopian tube has four parts, a. Funnel like infundibulum near ovary with finger like structure fimbriae b. Wide curved part ampulla. c. Narrow part isthmus. d. Part near uterus (uterine). 3. Uterus: • It is a pear shaped hollow muscular organ. It is attached to the body wall by a double fold of peritoneum called mesometrium. • The wall of uterus has three layers outer perimetrium, middle myometrium and inner endometrium. Inner lining of endometrium is richely supplied with blood vessels. • Uterus is divided into three parts, Upper dome shaped part is called fundus. Main part is called body of uterus. • The cavity of uterus can expand 500 times during pregnancy. Lower portion of uterus is called cervix.
- 12. 4. Vagina: • It is female copulatory organ. It is tubular, about 10-12cm long. • It passage for menstrual flow and receptor of spermatozoa. • In virgins the vaginal orifice is partially covered by hymen membrane. • It acts as birth canal during child birth (partition). 5. Vulva: • It is external genitalia it is consists of mons pubis (hair part), clitoris (erectile organ) labia majora (two large fold of skin which forms the boundary of vulva) & Labia minora (two smaller folds of skin lie between labia majora). • Clitoris is a small erectile organ. Labia majora and Labia minora processes sebaceous(oil) glands.
- 13. 6. Accessory glands: • Bartholin’s glands and mammary glands. Bartholin glands: • These are two bean-shaped lie on either of side of vaginal orifice. • These glands secret viscid fluid for lubricant of vulva during sexual intercourse and sexual excitement. Mammary glands: • These are pair rounded with median nipple. • Nipple is surrounded by a pigmented area called arola. • Arola has many sebaceous glands called areolar glands. • Each gland made up of 15-25 lobules of milky glands. • Each gland sends a lactiferous duct toward nipple. • Milk gland produce milk under the control of prolactin and ejection of milk is controlled by pituitary gland.
- 14. Menstruation (ovarian) cycle: • It is cyclic changes occur in reproductive tract of human female on a period of 28 days. It is confirmed by loss of vaginal blood. • It occurs at about 13 years of age till the age of 50-55 years. The menstruation is seen in human, monkeys, gorilla etc. • The menstrual cycle is categorized into three phases ;Menstrual phase, Proliferative or follicle phase & Secretory or luteal or ovulatory phase A. Menstrual phase; it is the phase of blood flow (weeping of uterus). • It last for 3-5 days. It is caused due to cast off epithelia lining of endometrium. • Oestrogen and progesterone is very law in the blood. Menstruation is observed only when ovum remains unfertilized. B. Proliferative or follicle phase: • Number of endometrium cells are rapidly proliferated. It last for 9-10 days (5th -14th ) day. • The release of FSH from pituitary stimulates the development of follicles of ovary. • Ovarian follicle matured into gaafian follicle and secrete oestrogen hormone which increases up to 12th days. • Oestrogen enhances proliferation of cells of endometrium of uterus and fallopian tubes (up to 2-3mm thickens). • The wall is highly supply with blood vessels and ready for implantation.
- 15. C. Secretory or luteal or ovulatory phase • It last for about 12-14 days (14th - 28th day of menstrual cycle). • LH (luteinising hormone) is secreted by pituitary gland called luteal phase. • LH and FSH stimulate the ovulation (releases of ova). So that LH and FSH concentration become high at this time. • After ovulation follicles of ova (corpus luteum) secret progesterone hormone. • Progesterone inhabits maturation of any follicle and ovulation. • Progesterone stimulates thickening of endometrium for implantation of zygote. • It also stimulates to secret water mucus and also affects mammary glands. • If the ovum is not fertilized, corpus luteum starts degenerating and the level of the hormones progesterone & oestrogen decreases. • At about 28th day the progesterone level falls, the blood vessels constrict and prevent the blood supply to the endometrium. • It results in sheeding off the endometrium along with the blood vessels causing menstrual phase.
- 17. Menopause • It is phase of women’s life. It occurs between 50 to 55 years. • At that age ovaries are less responsive to FSH and LH. Ovulation and menstrual cycle becomes irregular and stop. • After the menopause female loses the ability to reproduce progesterone and oestrogen hormone becomes imbalance.
- 18. Fertilization