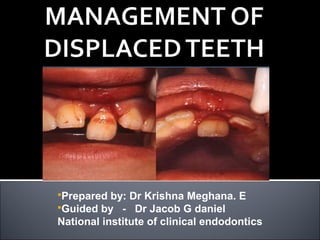
Managing Displaced Teeth: Diagnosis and Treatment
- 1. Prepared by: Dr Krishna Meghana. E Guided by - Dr Jacob G daniel National institute of clinical endodontics
- 2. Introduction to displaced tooth History and examination Types of displacement injuries Concussion – diagnosis, management Horizontal displacements- a.minor b.major diagnosis & management. Vertical displacement – intrusion and extrusion, diagnosis & management Importance of Follow up in Management Sequelae of displaced tooth
- 3. Biologically two features are common for all displaced teeth, irrespective of direction of displacement 1.The main vascular and neural bundle entering into the pulp cavity through the apical foramen is either stretched or snapped during the displacement. 2.The PDL attachment either damaged or completely torn all around the tooth.
- 4. Knowledge of these two features are important for proper management and follow up of prognosis The physiology of both internal and external structures of the tooth being deranged, biologic reaction following treatment becomes unpredictable
- 5. Case History Chief complaint History of present illness Medical History
- 6. Clinical Examination External Examination Soft Tissues Facial Skeleton Teeth and Supporting Structures Occlusion
- 7. Periapical Occlusal Panoramic
- 8. Injuries which do not cause clinically discernible displacements are categorized as concussion injuries Based on the direction of dislocation A. Horizontal displacements – buccal, lingual, mesial & distal B. Vertical displacements 1. Intrusion 2. Extrusion
- 9. An injury to the tooth-supporting structures with slight mobility or without increased mobility of the tooth, but with pain to percussion.
- 10. tooth is slight mobile but not displaced periodontal ligament (PDL) absorbs injury and becomes inflamed leaves tooth tender to biting pressure and percussion CONCUSSION
- 11. Visual sign: not displaced Percussion test: tender to touch or tapping Mobility test: no increased mobility CONCUSSION
- 12. Pulp Test: are unreliable the future vitality of the pulp will depend on the severity of the injury to the vascular bundle at the apical foramen lack of response to the test indicates an increased risk of later pulp necrosis CONCUSSION
- 13. Radiographic findings: no radiographic abnormalities Radiographs: occlusal, periapical, lateral view from mesial , distal aspect of suspected tooth should be taken CONCUSSION
- 14. Treatment Objectives: usually there is no immediate treatment except relieving the tooth from occlusion Treatment: frequent follow up at 1,3,6,12 month intervals is mandatory monitor pulpal condition for at least 1 year CONCUSSION
- 15. Patient Instructions: soft food for 1 week brush with soft bristle rinse with chlorhexidine 0.1% to prevent plaque accumulation CONCUSSION
- 16. Horizontal displacements may be in buccal, lingual ,mesial or Distal direction For the management purpose horizontal displacement divided into A. Minor displacement B. Major displacement
- 17. Clinically and radiographically the tooth should be checked for any accompanying root or alveolar fracture
- 18. It requires only repositioning and splinting of tooth during the emergency treatment Splint can be removed after week or two Root canal treatment need not be initiated immediately.
- 19. Follow up is mandatory As up to half of all such teeth may lose vitality of the pulp. Tooth be carefully observed for either signs of non vital tooth or external root resorption
- 20. At the first evidence of either of the two, the pulp canal be cleaned and temporarily filled with calcium hydroxide paste or powder This chemical which has a PH of around 11.4 is believed to prevent external resorption by diffusing through the dentinal tubule and reaching the external surface of the root
- 21. Major displacements in which the clinician believes that the blood supply to the tooth must have got cut off •root canal treatment should be instituted It is recommended that the tooth be repositioned and splinted in the emergency appointments and after a week RCT can be done This 1 week delay is in order to allow for the healing of the PDL Instituting RCT immediately could apply more stress on the already torn PDL Increasing the chance for the external resorption
- 22. Special care should be shown if patient reports for treatment after blood clot is fully formed In that part of socket left by the displaced tooth Although it may be tempting, clinician must desist from repositioning the tooth by applying pressure against the clot
- 23. Application of such a pressure can adversely affect the status of the torn PDL on the surface of the root and increase the chance for external resorption The tooth either be allowed to heal in the displaced position and subsequently brought to the desired (original) position using orthodontic means or the tooth be extracted and the socket cleansed off of the clot using saline & treatment proceeded as that for an avulsed tooth
- 24. Vertical displacements may be either A.INTRUSION B.EXTRUSION (with reference to Alveolar crest)
- 25. The behavior of extruded tooth is similar to that of horizontally displaced tooth except for the higher chance of necrosis of the pulp and requirement for two month splinting
- 27. Intruded tooth behave in a more complicated manner & are managed as follows Intruded tooth should always be decided for root canal treatment as almost always the pulp of an intruded tooth dies One week after the repositioning and splinting procedure root canal may be opened and filled with calcium hydroxide to reduce the possibility of occurrence of external resorption
- 28. Ankylosis is known to occur subsequent to intrusion Turley et al have demonstrated in animal studies that Ankylosis might get initiated within a week time following Intrusive injuries
- 29. It has been recommended that the tooth should be preferred ,to be moved to its original position using orthodontic means rather than forceps in a single attempt as complications are less following such relatively slow repositioning
- 30. In cases of teeth with incompletely formed apex there is no need for immediate iatrogenic intervention for repositioning of tooth The tooth can be kept under close observation as there is chance for the re-eruption of the tooth and also it has better chance for survival of the pulp However frequent & careful monitoring of immature permanent tooth is important as it has been reported that resorption once sets in, progresses rapidly in these teeth
- 31. Soft food for 1 week. Good healing following an injury to the teeth and oral tissues depends, in part, on good oral hygiene. Brushing with a soft brush and rinsing with chlorhexidine 0.1 % is beneficial to prevent accumulation of plaque and debris. FOLLOW-UP after 2 weeks. Splint removal and follow-up after 4 weeks, 6-8 weeks, 6 months, 1 year and yearly for 5 years
- 32. Follow up of the tooth for knowing 1.Signs of necrosis of the pulp forms 2.External root resorption 3.Healing of PDL & BONE 4.Ankylosis
- 33. Yellow discoloration Grey discoloration Resorption – 5 to 15% Incomplete root formation Primary teeth – pulp space obliteration by calcification
- 34. Thank you