KIDNEY LECTURE 2017.ppt
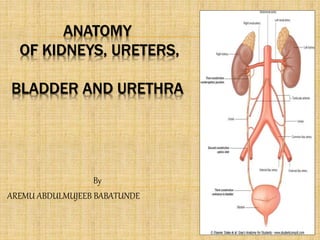
- 1. ANATOMY OF KIDNEYS, URETERS, BLADDER AND URETHRA By AREMU ABDULMUJEEB BABATUNDE
- 2. KIDNEYS Its main function is to excrete most of the waste products of metabolism It control the water and electrolyte balance of the body It maintain acid-base balance of the blood The waste products leave the kidneys as urine, which passes down the ureters to the urinary bladder The urine leaves the body through the urethra
- 3. KIDNEYS Kidneys are reddish brown in color Lie behind the peritoneum of the posterior abdominal wall It lie high up on either side of the vertebral column Are largely under cover of the costal margin The right kidney lies slightly lower than the left due to the large size of right lobe of the liver
- 4. KIDNEYS With contraction of the diaphragm during respiration, both kidneys move downward in a vertical direction as much as 2.5 cm On the medial border of each kidney is a vertical slit called the hilum The hilum extends into a large cavity called the renal sinus The hilum transmits the renal vein, two branches of renal artery, ureter, and the third branch of renal artery from the front backward (V.A.U.A.)
- 5. COVERINGS 1- Fibrous capsule: It surrounds the kidney 2- Perirenal fat: It covers the fibrous capsule 3- Renal fascia: it is a condensation of connective tissue that encloses the kidneys and suprarenal glands, it is continuous laterally with the fascia transversalis 4- Pararenal fat: it lies external to the renal fascia, and forms part of the retroperitoneal fat
- 6. THE KIDNEYS Each Kidney Is Protected and Stabilized By three concentric layers of connective tissue 1. Fibrous capsule • A layer of collagen fibers • Covers outer surface of entire organ 2. Perinephric fat capsule • A thick layer of adipose tissue • Surrounds renal capsule 3. Renal fascia • A dense, fibrous outer layer • Anchors kidney to surrounding structures
- 7. A superior view of a transverse section at the level indicated in part (a) Connective tissue layers Fibrous capsule Perinephric fat Renal fascia Left kidney External oblique Ureter Quadratus lumborum Psoas major Inferior vena cava Parietal peritoneumStomach Aorta Renal vein Renal artery Spleen Pancreas Vertebra
- 8. A posterior view of the trunk Abdominal aorta Urinary bladder Urethra Iliac crest Inferior vena cava Ureter Lumbar (L1) vertebra Right kidney Renal artery and vein 11th and 12th ribs Adrenal gland Diaphragm Left kidney
- 9. Anterior view Urinary bladder Peritoneum (cut) Hilum Right kidney Diaphragm Celiac trunk Inferior vena cava Right adrenal gland Quadratus lumborum muscle Iliacus muscle Psoas major muscle Rectum (cut) Gonadal artery and vein Abdominal aorta Left common iliac artery Superior mesenteric artery Left adrenal gland Esophagus (cut) Left kidney Left renal artery Left renal vein Left ureter
- 10. THE KIDNEYS Typical Adult Kidney Is about 10 cm long, 50.5 cm wide, and 3 cm thick (4 in. 2.2 in. 1.2 in.) Weighs about 150 g (5.25 oz) Hilum Point of entry for renal artery and renal nerves Point of exit for renal vein and ureter
- 11. THE KIDNEYS Sectional Anatomy of the Kidneys Renal sinus Internal cavity within kidney Lined by fibrous renal capsule Bound to outer surfaces of structures in renal sinus Stabilizes positions of ureter, renal blood vessels, and nerves
- 12. THE KIDNEYS Renal Cortex Superficial portion of kidney in contact with renal capsule Reddish brown and granular Renal Pyramids 6 to 18 distinct conical or triangular structures in renal medulla Base abuts cortex Tip (renal papilla) projects into renal sinus
- 13. THE KIDNEYS Renal Columns Bands of cortical tissue separate adjacent renal pyramids Extend into medulla Have distinct granular texture
- 14. THE KIDNEYS Renal Lobe Consists of: Renal pyramid Overlying area of renal cortex Adjacent tissues of renal columns Produces urine
- 15. THE KIDNEYS Renal Papilla Ducts discharge urine into minor calyx, a cup-shaped drain Major Calyx Formed by four or five minor calyces
- 16. THE KIDNEYS Renal Pelvis Large, funnel-shaped chamber Consists of two or three major calyces Fills most of renal sinus Connected to ureter, which drains kidney
- 17. A diagrammatic view of a frontal section through the left kidney Ureter Renal papilla Hilum Renal pelvis Adipose tissue in renal sinus Renal sinus Inner layer of fibrous capsule Fibrous capsule Renal columns Renal lobe Major calyx Minor calyx Connection to minor calyx Renal pyramid Renal medulla Renal cortex
- 18. A frontal section of the left kidney Renal columns Renal medulla Renal cortex Ureter Hilum Renal pyramids Renal sinus Renal pelvis Major calyx Minor calyx Renal papilla Renal lobe Fibrous capsule
- 19. THE KIDNEYS Blood Supply to the Kidneys Kidneys receive 20%–25% of total cardiac output 1200 mL of blood flows through kidneys each minute Kidney receives blood through renal artery
- 20. THE KIDNEYS Segmental Arteries Receive blood from renal artery Divide into interlobar arteries Which radiate outward through renal columns between renal pyramids Supply blood to arcuate arteries Which arch along boundary between cortex and medulla of kidney
- 21. THE KIDNEYS Afferent Arterioles Branch from each cortical radiate artery (also called interlobular artery) Deliver blood to capillaries supplying individual nephrons
- 22. THE KIDNEYS Cortical Radiate Veins Also called interlobular veins Deliver blood to arcuate veins Empty into interlobar veins Which drain directly into renal vein
- 23. THE KIDNEYS Renal Nerves Innervate kidneys and ureters Enter each kidney at hilum Follow tributaries of renal arteries to individual nephrons
- 24. THE KIDNEYS Sympathetic Innervation Adjusts rate of urine formation By changing blood flow and blood pressure at nephron Stimulates release of renin Which restricts losses of water and salt in urine By stimulating reabsorption at nephron
- 25. A sectional view, showing major arteries and veins Interlobar veins Renal vein Renal artery Adrenal artery Segmental artery Interlobar arteries Cortical radiate arteries Cortical radiate veins Cortex Medulla Arcuate veins Arcuate arteries
- 26. Circulation in a single renal lobe Cortical radiate vein Cortical radiate artery Arcuate artery Arcuate vein Renal pyramid Glomerulus Afferent arterioles Cortical nephron Juxtamedullary nephron Interlobar vein Interlobar artery Minor calyx
- 27. A flowchart of renal circulation Renal vein Renal artery Segmental arteries Interlobar arteries Arcuate arteries Cortical radiate arteries Afferent arterioles Glomerulus Efferent arteriole Peritubular capillaries Interlobar veins Arcuate veins Cortical radiate veins Venules NEPHRONS
- 28. THE KIDNEYS The Nephron Consists of renal tubule and renal corpuscle Renal tubule Long tubular passageway Begins at renal corpuscle
- 29. THE KIDNEYS The Nephron Renal corpuscle Spherical structure consisting of: Glomerular capsule (Bowman’s capsule) Cup-shaped chamber Capillary network (glomerulus)
- 30. RENAL STRUCTURE Each kidney has a dark brown outer cortex and a light brown inner medulla Medulla is composed of about a dozen renal pyramids Each pyramid having its base directed laterally toward the cortex, and its apex, (the renal papilla), projecting medially The cortex extends into the medulla between adjacent pyramids as the renal column
- 31. RENAL STRUCTURE Extending from the bases of the renal pyramids into the cortex are striations known as medullary rays The renal sinus within the hilum, contains the upper expanded end of the ureter, the renal pelvis Renal pelvis divides into two or three major calyces, which divides into two or three minor calyces
- 32. ANTERIOR RELATIONS OF THE KIDNEYS RIGHT KIDNEY Suprarenal gland Liver, Second part of the duodenum, Right colic flexure Coils of small intestine LEFT KIDNEY Suprarenal gland, Spleen, Stomach, Pancreas (body), Left colic flexure, Descending colon Coils of jejunum
- 34. RIGHT KIDNEY Diaphragm, Costodiaphragmatic recess of the pleura, Twelfth rib & last intercostal space, Psoas major Quadratus lumborum, Transversus abdominis muscle Subcostal nerve (T12) Iliohypogastric nerve (L1) Ilioinguinal nerve (L1) LEFT KIDNEY Same as the right except it is higher it reaches up to the 11th rib. Posterior Relations of the Kidneys
- 35. BLOOD SUPPLY The renal artery arises from the aorta at the level of the second lumbar vertebra Each renal artery divides into five segmental arteries that enter the hilum of the kidney, four infront and one behind the renal pelvis Lobar artery arise from each segmental artery, one for each renal pyramid
- 36. BLOOD SUPPLY Each lobar artery gives two or three interlobar arteries The interlobar arteries run toward the cortex on each side of the renal pyramid Interlobar arteries give the arcuate arteries at the junction of the cortex and medulla The arcuate arteries give several interlobular arteries Afferent glomerular arterioles arise as branches of interlobular arteries
- 37. VEINS, LYMPH, NERVE SUPPLY Renal vein emerges from the hilum in front of the renal artery and drains into the IVC Left renal vein is longer than the right renal vein Lateral aortic lymph nodes lie around the origin of the renal artery Renal sympathetic plexus: afferent fibers that travel through the renal plexus enter the spinal cord in the 10th, 11th, and 12th thoracic nerves
- 38. URETERS The two ureters are muscular tubes that extend from the kidneys to the posterior surface of the urinary bladder The urine is propelled along the ureter by peristaltic contractions Each ureter measures about 25 cm long Each ureter has three constrictions along its course, 1- Where the renal pelvis joins the ureter, 2- As it crosses the pelvic brim, 3- Where it pierces the bladder wall ( intra-mural
- 39. URETER The renal pelvis is the funnel-shaped expanded upper end of the ureter It lies within the hilum of the kidney and receives the major calyces It enters the pelvis by crossing the bifurcation of the common iliac artery in front of the sacroiliac joint It runs downward & forward on the lateral wall of the pelvis to enter the lateral angle of the bladder
- 40. RELATIONS, RIGHT URETER Anterior: Duodenum, Terminal part of the ileum, Right colic vessels, Iliocolic vessels, Right testicular or ovarian vessels, and the Root of the mesentery. Posterior: Right psoas muscle, Bifurcation of the right common iliac artery
- 41. RELATIONS, LEFT URETER Anterior: Sigmoid colon, Sigmoid mesocolon, Left colic vessels, Left testicular or ovarian vessels Posterior: Left psoas muscle, Bifurcation of left common iliac artery
- 42. BLOOD SUPPLY Upper end is supplied by the renal artery Middle portion by (gonadal) testicular or ovarian artery In the pelvis is supplied by the superior vesical artery The lymph drains to the lateral aortic nodes and the iliac nodes
- 43. NERVE SUPPLY Renal, testicular (or ovarian), and hypogastric plexus (in the pelvis) Afferent fibers travel with the sympathetic nerves and enter the spinal cord in the first and second lumbar segments
- 44. URINARY BLADDER SHAPE: It has the shape of three-sided pyramid placed on one of its angles, with the apex of pyramid is directed forward & its base is directed backward SITE: It lies behind the body of pubis & is separated from it by the retropubic space
- 45. Upper Surface Inferolateral surface Inferolateral surface Apex Neck
- 46. MALE PELVIS
- 47. MALE PELVIS
- 48. BASE OF MALE BLADDER
- 49. FEMALE PELVIS
- 50. FEMALE PELVIS
- 51. URINARY BLADDER RETROPUBIC SPACE: It is a space filled with extraperitoneal fatty tissue continuous with that of lower part of anterior abdominal wall It accomodates distention of urinary bladder In case of rupture of urinary bladder, urine may escape upward into the anterior abdominal wall
- 52. URINARY BLADDER APEX: Is directed forward Is related to upper border of symphysis pubis Is connected to umbilicus by the median umbilical ligament (obliterated part of urachus)
- 53. URINARY BLADDER BASE (POSTERIOR SURFACE): Is directed backward Its superolateral angles receive the ureters In male: 1. Its upper part is covered by peritoneum 2. It is related to vasa deferentia & seminal vesicles separating it from rectum In female: 1. It has no peritoneal covering 2. It is related to vagina
- 54. URINARY BLADDER SUPERIOR SURFACE: Is covered by peritoneum in both sexes In male: it is related to sigmoid colon & loops of ileum In female: it is related to the uterus separating it from sigmoid colon & loops of ileum
- 55. URINARY BLADDER INFEROLATERAL SURFACES: Are related to retropubic fat separating them from: 1. Body of pubis 2. Levator ani 3. Obturator internus
- 56. URINARY BLADDER NECK: Is the lowest & most fixed part Lies behind symphysis pubis Is continuous with urethra In male: 1. It rests on upper surface of prostate 2. Anteriorly: it is attached to puboprostatic ligament 3. Posteriorly: it is related to beginning of ejaculatory ducts In female: 1. Anteriorly: it is attached to pubovesical ligament 2. Posteriorly: it is related to anterior wall of vagina
- 57. URINARY BLADDER LIGAMENTS: 1. Median umbilical ligament 2. Puboprostatic (pubovesical) ligament: Forms the floor of retropubic space In male: is called “puboprostatic” & extends from body of pubis to prostatic fascia & neck of bladder In female: is called “pubovesical” & extends from body of pubis to neck of bladder
- 58. INTERIOR OF URINARY BLADDER
- 59. INTERIOR OF URINARY BLADDER The mucous membrane forms folds (rugae) that disappear when the bladder is distended TRIGONE: 1. A triangular area in the base of bladder, bounded by the 2 ureteric orifices & the internal urethral orifice 2. Its mucous membrane is elastic, more vascular & more sensitive UVULA VESICA: is an elevation immediately behind internal urethral orifice produced by the underlying median lobe of prostate
- 61. URINARY BLADDER CAPACITY: Is about 300 ml with a maximum capacity of 500 ml Distended bladder: Is circular in shape Bulges upward into abdominal cavity Removes peritoneum form lower part of anterior abdominal wall & becomes into direct contact with it
- 62. URINARY BLADDER IN CHILD It is an abdominal organ even when empty It begins to enter the enlarging pelvis at six years of age It is not entirely a pelvic organ till after puberty Median sagittal section of a new-born female child
- 63. URINARY BLADDER ARTERIAL SUPPLY: Superior & inferior vesical arteries VENOUS DRAINAGE: Veins from the vesical venous plexus that drain into the internal iliac vein LYMPHATIC DRAINAGE: Into internal & external iliac lymph nodes
- 64. URINARY BLADDER NERVE SUPPLY: by the inferior hypogastric plexuses 1. Parasympathetic fibers: from S2,3,4 motor to detrusor muscle (muscle coat of bladder) & inhibitory to internal urethral sphincter, produce micturation 2. Sympathetic fibers: from first & second lumbar ganglia 3. Ascending sensory fibers: carry sensation of fullness (distention) & pain sensation
- 65. PELVIC PART OF URETER Crosses the front of bifurcation of common iliac artery to reach the pelvis Descends downward & backward, along the lower border of internal iliac artery, crossing (from above downward): 1. External iliac artery & vein 2. Obturator nerve, artery & vein Curves forward & medially
- 66. IN MALE It is crossed anteriorly by vas deferens
- 67. IN FEMALE It passes below the root of broad ligament, lateral to lateral fornix of vagina & is crossed superiorly by the uterine artery
- 68. PELVIC PART OF URETER TERMINATION: It reaches the posterosuperior angle of bladder It runs an oblique course of about 2 cm through the wall of bladder before it opens into its lumen (intramural part of ureter). This part forms a valve-like mechanism that prevents reflux of urine into the ureter when bladder is distended
- 69. MALE URETHRA About 8 inches (20cm) long Extends from the neck of bladder to the external urinary meatus on the tip of the glans penis Divided into three parts: Prostatic Membranous Penile
- 71. Prostatic urethra Length=3 cm Widest & most dilatable Extends from neck of bladder inside prostate gland Structures openings into prostatic urethra: Ejaculatory ducts Ducts of prostate gland Membranous urethra Length=1 cm Surrounded by external urethral sphincter Penile (spongy) urethra Length=16 cm narrowest part of whole urethra Extends inside penis & opens externally through external urethral orifice
- 72. FEMALE URETHRA Extends from neck of urinary bladder to open externally through the external urethral orifice (anterior to the vaginal opening) Has only urinary function
- 73. DIURETICS Diuretics are medicines that increase the amount of urine that is produced. People who have high blood pressure might be prescribed diuretics to decrease the blood volume. Alcohol is a diuretic and this is what contributes to the symptoms of a hangover. The best way to prevent a hangover after drinking is to consume a lot of water before you go to bed. Caffeine is also a diuretic, so coffee, energy drinks, and regular Coca-cola are diuretics. You should drink one cup of water for every cup of those beverages to prevent dehydration. 73
- 74. PROBLEMS URETHRITIS = infection and inflammation of the urethra PYELITIS= infection of the renal calyxes CYSTITIS = infection of the urinary bladder. CHOLEOCYTITIS = infection of the gall bladder Nephritis: inflammation of the nephrons. Hydronephritis: excess fluid in the nephron. 74
- 75. PROBLEMS KIDNEY STONES Develop in the renal pelvis Stones are made out of a variety of things: uric acid, calcium, cystine (an amino acid), or cholesterol. They keep growing. 75
- 76. KIDNEY STONES They can block the ureter, causing the kidney to enlarge. As the kidney stretches, the capsule stretches, causing excruciating pain in cycles of hours. As pressure builds up from fluid accumulating around the stone, urine can pass, and the kidney stone moves down the urethra slowly. Symptomatic kidney stones may be pea sized or larger (up to 1 ½ inches). They get stuck in three places: Renal pelvis In the ureter as it bends over the common iliac artery In the urinary bladder at the trigone. 76
- 77. KIDNEY FAILURE Things can happen to the kidney that can lead to kidney failure: infection, excess proteins, pH change, and blood pressure drops. Treatment for kidney failure is DIALYSIS, which removes blood, send it through a filter, and returns it without the wastes. It is done three times a week, six hours a day. Ideally, they need a kidney transplant because the kidney has other functions as well. The brain, heart, and kidney are the only three organs in the body that have to get oxygen to sustain life. 77
- 78. WHO IS MOST LIKELY TO GET RENAL FAILURE? Kidney or Liver Disease Diabetes High Blood Pressure Heart Failure Obesity Bone Marrow Transplant Heart or Belly Surgery 78