Lect. 6 specialized ct cartilage
- 2. Bone and Cartilage: Why are they CTs? Both have: – Cells, extracellular fibers, and matrix • Collagen & Elastic fibers • Glycoproteins: Gel-like matrix • Fibroblast-type cells – Chondroblasts/chondrocytes Osteoblasts/osteocytes
- 3. Both have: – General functions of mechanical & physiological support and protection • Structural framework • Reserves of Ca & P Interrelated with other CT’s in history and development
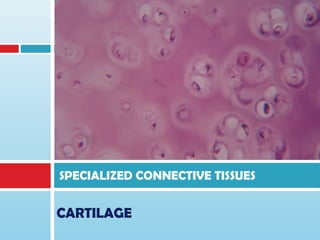
- 4. CARTILAGE A specialized CT in which the firm ECM allows the tissue to bear mechanical stresses without permanent distortion. SOLID yet FLEXIBLE
- 5. Ground substance Proteoglycans Sulfated GAGs – keratan sulfate, chondroitin sufate Non-sulfated GAG – hyalurinic acid (backbone of the complex) Glycoproteins Chondronectin and chondrocalcin No mineral (inorganic) component no calcium salt Water (tissue fluid) – highly hydrated (75%)
- 6. Fibers Collagen fibers Collagen Type I – in fibrocartlage Collagen Type II – in hyaline cartilage (except in articular cartilage) Elastic fibers - in elastic cartilage Ground substance components interact with the fibers. Variations in the composition of these matrix components produce three types of cartilage.
- 7. Molecular organization in cartilage matrix. Link proteins noncovalently bind the protein core of proteoglycans to the linear hyaluronic acid molecules. The chondroitin sulfate side chains of the proteoglycan electrostatically bind to the collagen fibrils, forming a cross-linked matrix. The oval outlines the area shown larger in the lower part of the figure.
- 8. Cells Fibroblast-like – progenitor cells Cells in the perichondrium (inner layer) Also refered as Chondrogenic cells Undergo mitosis and differentiate into -- Chondroblasts Synthesize the precursors of extracellular fibers and other organic subs. in the matrix when surrounded by the matrix, they acquire lacunae and transform into -- Chondrocytes Cells in the matrix, still mitotic, still synthesizing the materials in the matrix.
- 9. Chondrocytes Vary in shape and size Elliptical; parallel to the cart. surface - young Round – mature cartilage Cytoplasm – finely granular, basophilic Well developed rER and Golgi c.- secretory Inclusions – fat droplets, glycogen granules Possess cytoplasmic processes Nucleus – ovoid; chromatin concentated on inner nuclear mem.; 1 or more nucleoli
- 11. Cartilage development Mesenchymal cells differentiated into chondroblasts which became its precursorial cells. Chondroblast mitosis isogenous groups grow and begin synthesis of ground substance and fibrous extracellular (EC) materials. Secretion of EC materials trap each chondroblasts in the matrix thereby separating the cells (interstitial growth). Chondrocytes develop and maintain matrix integrity.
- 12. Develops from somites and somatopleure of mesoderm (mesenchyme) A. mesenchyme condenses to form cellular primordium B. chondroblasts form and begin secreting matrix C. cells separate from chondrocytes D. cartilage grows by interstitial growth – isogenous groups.
- 14. There are no capillaries within the cartilage matrix. Perichondrium harbors the vascular supply for the avascular cartilage and also contains nerves and lymphatic vessels.
- 15. Perichondrium is a sheath of dense irregular CT that surrounds cartilage in most places, forming an interface between the cartilage and the tissue supported by the cartilage.
- 16. Cartilage Nutrition Chondrocytes respire under low O2 tension since it is devoid of capillaries. metabolize glucose mainly by anaerobic glycolysis to produce lactic acid. Nutrients from the blood cross the perichondrium to reach more deeply placed cartilage cells by diffusion and transport of water and solute promoted by the pumping action of intermittent cartilage compression and decompression.
- 17. Articular cartilage which covers the surfaces of the bones of movable joints. devoid of perichondrium . This cartilage is sustained by the diffusion of oxygen and nutrients from the synovial fluid.
- 18. Articular cartilage - devoid of perichondrium
- 19. Types of Cartilage Hyaline cartilage Elastic cartilage Fibrocartilage
- 20. Hyaline Cartilage The most common and best studied of the three forms. Fresh hyaline cartilage - bluish-white and translucent. In embryo: A temporary skeleton until it is gradually replaced by bone. Perichondrium is well-defined.
- 22. Hyaline cartilage In adult mammals: This cartilage is located in the articular surfaces of the movable joints walls of larger respiratory passages (nose, larynx, trachea, bronchi), ventral ends of ribs, where they articulate with the sternum epiphyseal plate, where it is responsible for the longitudinal growth of bone.
- 24. Articular cartilage on surfaces of movable joints
- 25. Ventral ends of ribs, where cartilage articulate with the sternum.
- 26. Epiphyseal plate, where it is responsible for the longitudinal growth of bone Larynx, thyroid cart., cricoid cart. trachea
- 27. Elastic Cartilage Fresh form – yellowish due to elastin in the fibers. Identical to hyaline cartilage except that it contains an abundant network of fine elastic fibers in addition to collagen type II fibrils.
- 29. ELASTIC CARTLAGE its elasticity is derived from the presence of numerous bundles of branching elastic fibres in the cartilage matrix this network of elastic fibres (stained black in this preparation) is particularly dense in the immediate vicinity of the chondrocytes.
- 30. Perichondrium is defined. Collagen (stained red) is also a major constituent of the cartilage matrix and makes up the bulk of the perichondrium P intermingled with a few elastic fibres.
- 31. Elastic cartilage Found in the auricle of the ear walls of the external auditory canals the auditory (eustachian) tubes the epiglottis cuneiform cartilage in the larynx.
- 32. Parts of the Ear (with elastic cartilage)
- 33. Epiglottis • utilizes the structural support and flexibility which elastic cartilage provides. • leaf-shaped flap of tissue, the epiglottis, closes the opening into the larynx during swallowing
- 34. Fibrocartilage A tissue intermediate between dense connective tissue and hyaline cartilage. It is always associated with dense CT, and the border areas between these two tissues are not clear-cut, showing a gradual transition. Chondrocytes are either singly or in isogenous groups, arranged in long rows separated by coarse collagen type I fibers . Because it is rich in collagen type I, the fibrocartilage matrix is acidophilic. Perichondrium is poorly defined.
- 37. Fibrocartilage found where strong support and the ability to withstand heavy pressure are required. intervertebral disks attachments of certain ligaments to the cartilaginous surface of bones and in the symphysis pubis.
- 39. Intervertebral Disks (IVD) IVD are symphysial joints that unite vertebral bodies. permit movement between the vertebral bodies while maintaining a union of great strength. acts as a lubricated cushion that prevents adjacent vertebrae from being eroded by abrasive forces during movement of the spinal column.
- 40. • The IVDs have two components: the fibrous annulus fibrosus (AF) and the nucleus pulposus (NP). • The nucleus pulposus serves as a shock absorber to cushion the impact between vertebrae.
- 41. Annulus fibrosus external layer of dense CT mainly composed of overlapping laminae of fibrocartilage in which collagen bundles are orthogonally arranged in adjacent layers. The multiple lamellae provide the disk with unusual resilience that enables it to withstand the pressures generated by impinging vertebrae. Nucleus pulposus derived from the embryonic notochord consists of a few rounded cells embedded in a viscous matrix rich in hyaluronic acid and type II collagen fibrils In children, the nucleus pulposus is large, but it gradually becomes smaller with age and is partially replaced by fibrocartilage.
- 42. Pubic symphysis
- 43. Assignment: Read about Interstitial growth Appositional growth
- 44. Growth of cartilage tissues Expands the cartilage within matrix. Also for growth in length of long bones. Endogenous growth. Possible only in young cartilage. Occurs at the edges of cartilaginous structures. Exogenous growth A function of the perichondrium. chondrogenic layer of perichondrium Interstitial growth Appositional growth
- 45. Interstitial growth In young cartilage, the intercellular substance is still malleable and the chondrocytes possess the capacity to multiply.
- 46. 1. Mitosis of young chondrocytes. 2. Daughter cells secrete precursor materials for ECM. Secretory capacity of daughter cells is limited, the amt. of intercellular substance they deposit is also limited. Result: Isogenous groups (chondrocytes that lie close to each other up to maturity.) 1. Intercellular substance becomes rigid with age, interstitial growth ceases.
- 48. Appositional growth 1. Cells in perichondrium differentiate into chondrocytes 2. Matrix is made and laid down, lacunae formed 3. Shape of structure can be changed May be localized 1. Same process as interstitial growth: different location!
- 50. Cartilage repair Cartilage has very limited repair capability Cartilage is AVASCULAR! Dependent on diffusion kinetics If chondrocytes live, matrix can be replaced Chondrocyte loss means loss of structure Some limited regeneration by differentiation of cells from perichondrium. Injury to articular cartilage not a good thing: no perichondrium! Usual “repair” by fibrosis & collagen proliferation Calcification may occur.
- 51. END