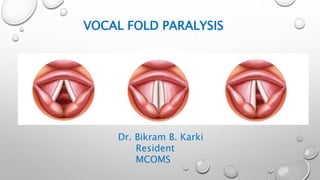
Vocal cord paralysis
- 1. VOCAL FOLD PARALYSIS Dr. Bikram B. Karki Resident MCOMS
- 2. ANATOMY OF VAGUS NERVE • Provides innervation to intrinsic muscles and sensory structures • Some fibres originate in medulla ( nucleus ambiguus) while others originate at higher level • Leaves skull through jugular foramen • Descends within carotid sheath as far as superior border of thyroid cartilage • Then between IJV and CCA to root of neck
- 3. SUPERIOR LARYNGEAL NERVE • Arises from lower portion of inferior ganglion • Descend on side wall of pharynx, posterior and medial to ICA • At greater cornu of hyoid bone – • Divides into internal laryngeal branch external laryngeal branch
- 4. • Internal branch • Descends to thyrohyoid membrane piercing it above superior laryngeal artery • Inferiorly communicates with ascending branch of RLN • External branch • Descend deep to superior thyroid artery on inferior constrictor muscle • Pierces muscle and supplies cricothyroid muscle
- 5. RECURRENT LARYNGEAL NERVE • RIGHT RLN • Arises- right vagus nerve infront of right subclavian artery in neck • Winds backward around it • Ascends obliquely behind CCA • Into trachea - oesophageal groove • Reaches lower pole of thyroid and intimately related to ITA
- 6. • LEFT RLN • Arises- left vagus nerve in mediastinum and loops around arch of aorta • Passed medially and posteriorly to ligamentum arteriosum • Ascends in trachea - oesophageal groove • Both right and left RLN intimately related to medial surface of thyroid • Passes deep to lower border of inferior constrictor muscle • Enter larynx behind cricothyroid joint
- 7. NERVE SUPPLY OF LARYNX • motor supply: • cricothyroid muscle: superior laryngeal nerve • all other intrinsic muscles: recurrent laryngeal nerve • sensory supply: • above level of vocal cord: superior laryngeal nerve • below level of vocal cord: recurrent laryngeal nerve
- 8. CLASSIFICATION • Can be unilateral or bilateral • On the basis of nerve involvement: • SLN paralysis • RLN paralysis • Combined paralysis ( both RLN and SLN )
- 9. PATHOPHYSIOLOGY • Most cases of laryngeal paralysis result – from peripheral nerve damage • Larynx - strong propensity for re-innervation • However, regeneration of RLN - more problematic than most peripheral nerve • Re-innervation is often dysfunctional and does not yield physiologic motion
- 10. SEMON’S LAW • Motor fiber innervating abductor and adductor lay in separate bundle • Progessive nerve injury - selectively damages abductor nerve fibre • So in partial injury, VF lie close to midline with weak abduction • Over times, adductor muscle weaken- VF move laterally (cadaveric position )
- 11. WAGNER AND GROSSMAN THEORY • In absence of cricoarytenoid joint fixation • An immobile vocal fold in paramedian position - pure unilateral RLN paralysis • An immobile VF in lateral ( cadaveric position ) - combined paralysis of SLN and RLN • Widely accepted theory
- 12. MODERN THEORY • Final position of paralysed VF is not static and is decided by • Degree of paralyzed muscle atrophy and fibrosis • Degree of re-innervation following injury • Extent of synkinesis of all intrinsic muscle • Crico-arytenoid joint - Fibrosis and ankylosis
- 13. SITE OF LESION • Supranuclear • Rare • Requires B/L symmetrical lesion of cortex • Nucelar • Tumor of medulla • PICA thrombosis, Bulbar palsy • Encephalitis, Cranial polyneuritis • MND
- 14. • Posterior fossa and jugular foramen • Vernet syndrome – 9,10,11 CN • Villaret’s syndrome- 9,10,11,12 CN and horners syndrome • Collet- siccard syndrome- 9,10,11,12 CN • Hughling’s jackson syndrome – 10,11,12 CN • Schmidt’s syndrome – 10,11CN
- 15. Extra cranial Cervical region • Penetrating injuries • Tumors of hypopharynx, thyroid, upper oesophagus, PPS • Surgery of thyroid gland Thorax • Aortic aneurysm • Enlarged left atrium • Carcinoma of bronchus • Mediastinal tumors, • Enlarged mediastinal glands
- 16. AETIOLOGY • Congenital • Acquired CONGENITAL • Idiopathic – most common • CNS lesion • Hydrocephalus • Arnold- chiari malformation • Cerebral palsy • Mediastinal lesion • Vascular malformation of great vessels or heart
- 17. ACQUIRED • Idiopathic (13%) • Although viral infections – influenza and infectious mononucleosis • Inflammatory (13%) • Pulmonary tuberculosis • Malignant (25%) • Lung • Oesophagus • Thyroid • nasopharynx
- 18. • Surgical trauma (20%) • Thyroid, oesophagus, lung ,heart, mediastinum • Non-surgical trauma (11%) • Aortic aneurysm • Left atrium enlargement • Neurological (7%) • CVA, MS, parkinson’s disese, head injuries, diabetic neuropathy, alcohol • Miscellaneous (11%) • Rheumatoid disease • Collagen disease
- 19. CLINICAL FEATURES • SLN PALSY • Unilateral • Voice – not severely affected • Compensation occurs quickly • Disability to professional voice user- significant • Bilateral • Voice - lower, weaker and breathy • With good compensation - speaking voice returns but singing voice compromised • Cough and choking
- 20. RLN PARALYSIS • Unilateral abductor paralysis • Initial hoarsenss - disappear as normal VF compensates • Voice tire with repeated use • May aspirate – particularly liquid • Bilateral abductor paralysis • VF- paramedian position • Voice – good but degree of stridor variable • Stridor and dyspnoea
- 21. • Unilateral adductor paralysis • Flaccid paralysed VF – Lateral position • Voice - Weak husky, sometimes whisper only • Aspiration • Bilateral adductor paralysis • Rare • VF - lateral position • Aphonia • Aspiration • Unable to cough
- 22. INVESTIGATION • Assessment of vocal folds movement • Flexible fibreoptic laryngoscopy • Stroboscopy • Endoscopy • Panendoscopy – need for biopsy • Radiology • Chest X-ray – screen for intrathoracic region • CT Scan from skull base to mid- thorax • MRI – imaging skull base or CNS
- 23. • Modified barium swallow • Thyroid scan • Hematological test • Full blood count, ESR, serology • Laryngeal electromyography ( LEMG ) • Measures electric activity of larynx muscle via thin percutaneous needle electrodes • Allows better differentiation between neural lesion and other cause • Provide evidence of re-innervation and denervation • Localization of lesion along nerve
- 24. • EVALUATION OF LEMG • Normal- joint fixation, post scar • Fibrillation - denervation • Polyphasic - reinnervation synkineses
- 25. MANAGEMENT FOR UNILATERAL ADDUCTOR PARALYSIS • Voice therapy • Vocal fold injection • Medialization thyroplasty • Arytenoid adduction • Laryngeal nerve re-innervation • Combination of above
- 26. VOCAL FOLD INJECTION • Injection of absorbable bulking material in paralysed fold to improve glottic insufficiency • Brunnings (1911) • First describe injection of vocal folds • Injected paraffin • Arnold (1962) • Popularized the technique • Introduction of Teflon
- 27. MATERIALS USED • Paraffin • Teflon • Autologous fat • Cymetra • Collagen • Calcium hydroxyapatite • Gelfoam paste • Hyaluronic acid formulations
- 28. TEFLON • Polymer of tetrafluoroethylene • Contain 50% glycerine • Glycerine absorbed in few weeks • Length of effect – permanent • Disadvantage • Inflammatory reaction → encapsulation of remaining teflon (granuloma ) • If placed superficially - erosion of overlying mucosa
- 29. AUTOLOGOUS FAT • Insertion deep into VF ( High density ) • 30–50% - absorbed within 1st month • Good immediate voice quality • Length of effect - permanent • Advantages: • Easily harvested • Readily available ( lower abdomen and inner thigh) • No foreign body reaction
- 30. COLLAGEN • Protein - natural constituent of lamina propria of VF • Popularized by ford et al. for use in larynx • Injected superficially into vocal ligament • Length of effect - 3 – 4 months • Advantage • Better stability • Reduces rate of hypersensitivity, which is < 1%
- 31. SILICONE • Silicon gel • Injected deep in body of VF – to prevent migration • Length of effect – permanent • Inflammatory reaction → fibrous capsule CALCIUM HYDROXYAPATITE • Widespread usage • Injected deep in VF otherwise lead to long-term hoarseness • Length of effect - 2-5 years
- 32. METHODS • Percutaneous injection • Transoral injection • Laryngoscopic injection
- 33. PERCUTANEOUS INJECTION • May be • Lateral approach or • Anterior approach
- 34. • Lateral approach • Through thyroid ala at level of vocal fold • Determined by palpation of thyroid notch and inferior border of thyroid ala anteriorly • Vocal fold lies at midpoint
- 35. • Anterior approach • Through cricothyroid membrane • Needle is inserted - angled superiorly and Laterally under direct visualization with • Flexible fiberoptic nasopharyngoscope • Transthyrohyoid approach
- 36. TRANSORAL INJECTION • Apply topical lidocaine spray to pharyngeal + laryngeal mucosa • Patient holds tongue forward - indirect visualization • Injection of material with curved laryngeal needle • Direct bevel away from midline ( minimize intramucosal injection)
- 38. LARYNGOSCOPIC INJECTION • Performed under general anesthesia • Introduction of kleinsasser’s microlaryngoscope
- 39. • Complication • Under injection - requires repeat procedures • Over injection - airway compromise • Improper placement – subglottal extension and potential stenosis • Granuloma formation • Migration of materials (Teflon)
- 41. MEDIALIZATION THYROPLASTY • Medialization of VF by an implant placed through a window in thyroid cartilage • Insertion of prosthesis - lateral to inner perichondrium
- 42. IMPLANTS USED • Silastic implants (montgomery) Carved or prefabricated • Dense hydroxyapatite (vocom) implants • Gore-tex strip
- 43. TECHNIQUE • Supine position • LA - administered subcutaneously and in four quadrants over ipsilateral lamina • A 5-cm incision - made through platysma • Flaps elevated Superiorly and inferiorly - subplatysmal plane - expose thyroid notch and inferior border (thyroid cartilage)
- 44. • Strap muscles - split in midline and • Are retracted laterally off thyroid lamina
- 45. • Window measures 6 mm (vertical) by 10 mm (horizontal; • Anterior aspect of window • Positioned 5 to 8 mm posterior to ventral midline - women and 8 to 10 mm - men • Superior aspect of window • Placed at level of true fold • Level of true fold • A point half distance between Thyroid notch and Anterior-inferior border of
- 46. • Outer perichondrium incised and • Elevated from thyroid cartilage • Cutting bur is used, followed by a diamond bur • To remove cartilage and to protect underlying perichondrium
- 47. • Inner perichondrium is circumferentially elevated with blunt dissector • Template or appropriately sized prosthesis – placed in most effective position • Small suction drain placed deep to strap muscles • Closure of skin
- 48. • Variations in placement of implant • Vertical and horizontal implants relative to plane of vocal fold
- 49. • Advantages • performed with local anesthesia • potentially reversible • better assessment of voice during procedure • structural integrity of VF – preserved • Disadvantages • open procedure • procedure is technically more difficult • closure of posterior glottis may be limited
- 50. • Complications • Incomplete glottal closure (10-15%) • Penetration of endo laryngeal mucosa - Airway obstruction • Chondritis • Wound infection • Post op hematoma, odema • Suboptimal voice outcome – most common • Implant migration or extrusion
- 51. ARYTENOID ADDUCTION • Partial division of sternohyoid muscle 1 cm below its insertion • Posteriorly based flap separates muscle away from posterior cartilaginous border • Paraglottic space - connected between posterior cartilage border
- 52. • Posterior “cookie –bite” window - created with kerrison rongeur • Pyriform mucosa - dissected posteriorly using a kitner • Muscular process of arytenoid - identified
- 53. • 4-0 prolene suture passed through muscular process in figure of eight fashion • Passage of suture through ML window • Final tying of a surgeon’s knot over thyroid ala
- 54. LARYNGEAL REINNERVATION • Horsley (1909) - reported first successful vocal fold reinnervation ( RLN ) • Two most common reinnervation techniques • Neuromuscular pedicle (NMP) • Ansa cervicalis to RLN (ANSA-RLN) anastomosis/transfer • Additional techniques • Hypoglossal nerve – RLN transfer • Primary anastomosis of RLN • Direct nerve implantation • Muscle-nerve-muscle graft
- 55. NEUROMUSCULAR PEDICLE (NMP) • Attempts to transfer - nerve with a portion of its motor units intact to a denervated muscle • Technique • Horizontal incision - near lower border of thyroid cartilage • Anterior border of SCM muscle – exposed and retracted laterally
- 56. • Branch of ansa cervicalis - supplies anterior belly of omohyoid muscle • Identified in two ways: • First, finding main trunk of ansa cervicalis as it crosses IJV and tracing proximally and distally, until appropriate branch recognized • Second, • By medial border of omohyoid mobilized near its attachment to hyoid and dissecting in medial to lateral direction along muscle
- 57. • NMP harvested from omohyoid muscle • Branch of ansa cervicalis nerve to omohyoid is removed With 2 to 3 mm attached block of muscle
- 58. • NMP placed into PCA muscle ( for lateralization ) • PCA muscle recognized by its fibers, which pass at right angles to inferior constrictor • NMP placed in LCA muscle via window in thyroid ala • NMP - sutured in place with two or three sutures of 5-0 nylon.
- 59. ANSA CERVICALIS TO RLN • Technique • Incision - natural creases of neck below cricoid cartilage (thyroidectomy incison) • Strap muscles - separated vertically in midline • RLN - identified in tracheoesophageal groove, and - dissected at its entrance into larynx • Ansa cervicalis - identified along lateral border of sternothyroid muscle at level of omohyoid muscle or along IJV
- 61. • Advantage • Procedure relatively easy • Can be reversed ( extralaryngeal procedure ) • Subsequent use of vocal fold injection or thyroplasty is not limited • No foreign body reaction ( No permanent implant material ) • Disadvantage • Typically takes longer to perform • Delay of several months - before substantial improvement in voice occurs • Can be difficult after thyroid surgery or after bilateral neck surgery
- 62. MANAGEMENT OF BILATERAL ABDUCTOR PARALYSIS • Good voice but lack abduction during inspiration • Maintenance of airway is primary goal • Airway preservation often damages an otherwise good voice
- 63. • Surgical management • Tracheostomy • Vocal fold lateralization • Lateralization thyroplasty • Endoscopic cordotomy • Endoscopic cordectomy • Arytenoidectomy • Laryngeal reinnervation
- 64. VOCAL FOLD LATERALIZATION • EXTERNAL APPROACH • Thyroid cartilage exposed via horizontal incision • 16-gauge IV cannula inserted through thyroid cartilage • 4 mm anterior & 2 mm below mid-point of oblique line into laryngeal lumen, just above tip of vocal process, Under MLS. Guidance • Another 16-gauge IV cannula inserted 5 mm below 1st cannula
- 65. • 1-0 prolene suture threaded through inferior cannula into laryngeal lumen • Suture thread brought out with forceps into laryngeal lumen & inserted into superior cannula • External traction - on both suture ends - pull vocal cord laterally to give 5 mm airway • Threads tied over thyroid lamina
- 66. VOCAL FOLD LATERALIZATION – ENDOSCOPIC
- 70. VOCAL CORDOTOMY • Laser cordotomy - first described in 1989 by kashima • Only frees vocal ligament and vocal muscle from vocal process of arytenoids • Tissue retraction enlarges airway • If one vocal fold seems to have - light degree of motion, cordotomy performed on opposite side
- 71. • Technique • CO2 laser with 0.2 mm spot size used • Performed 1-2 mm anterior to vocal process • Carried laterally through width of vocal ligament and vocalis muscle to thyroid lamina • Opens air way posteriorly
- 72. • Complication • Posterior glottic web • Postoperative edema • Granuloma • Scar formation
- 73. POSTERIOR CORDECTOMY • Dennis and kashima - first described in 1989 • Technique • CO2 laser 3.5-4 mm • C- shaped wedge of posterior vocal cord excised from free border of cord, anterior to vocal process • Extending 4 mm laterally over ventricular band
- 74. • Excision - anterior to vocal process and cartilage should not be exposed • Creates 6-7 mm transverse opening at posterior larynx
- 75. ARYTENOIDECTOMY • Thornell (1948) - First endolaryngeal arytenoidectomy • Permanent and irreversible surgical procedure whereby laryngeal inlet is widened in its transverse axis • May be Medial arytenoidectomy Total arytenoidectomy
- 76. • Medial arytenoidectomy (partial arytenoidectomy) • Most medial 2-3 mm of body of arytenoid cartilage removed • Vocal process and intra-arytenoid mucosa - not disturbed • Total arytenoidectomy (complete arytenoidectomy) • CO2 laser ablation of entire body of arytenoid until defect is flush with wall of cricoid ring
- 77. MANAGEMENT OF BILATERAL ADDUCTOR PARALYSIS (CHRONIC ASPIRATION) • Non surgical management • All oral intake is discontinued • Alternative route of alimentation - nasogastric feeding tubes, gastrostomy, and jejunostomy • Appropriate antibiotics for infectious complications • Aggressive pulmonary therapy
- 79. LARYNGOTRACHEAL SEPARATION (LTS) • Division of trachea horizontally between 2nd and 3rd tracheal rings or at level of an existing tracheotomy • Proximal tracheal edges closed antero-posteriorly as blind pouch • Distal tracheal segment - used to create tracheostoma
- 80. TRACHEOESOPHAGEAL DIVERSION (TED) • Lindeman (1975) • Horizontal division at 4th and 5th tracheal rings • Proximal tracheal segment – end anastomosed to anterior esophagus • Distal tracheal segment - used to create a tracheostoma
- 81. ENDOLARYNGEAL STENT • Solid stent • Weisberger and huebsch • Solid silicone laryngeal stent – placed endoscopically • Secured transcervically with sutures • Tracheotomy tube necessary
- 82. • Vented stent • Eliachar • Vented silicone laryngeal stents inserted through tracheotomy • Secured by flexible strap of silicone that extends from tracheotomy tract above tracheotomy tube • Disadvantage • Discomfort to patient • Dislodgement of implant
- 83. VERTICAL LARYNGOPLASTY • Incision - made along outer borders of epiglottis, aryepiglottic folds, over arytenoids and into interarytenoid area • Epiglottis and supraglottic larynx - closed vertically in two layers as a tube, with small opening left superiorly
- 84. EPIGLOTTIC FLAP CLOSURE • Supraglottic larynx - approached through an infrahyoid pharyngotomy • Supraglottic larynx - closed after edges of epiglottis, aryepiglottic folds and arytenoids are denuded • Tracheotomy is required
- 85. • Advantages • Reversible • True vocal cords not injured • Deglutition and speech preservation ( if posterior laryngeal inlet left open ) • Disadvantages • High rate of flap dehiscence and failure • Need of transcervical approach and tracheotomy • Supraglottic stenosis - potential complication
- 86. GLOTTIC CLOSURE • Described by Montgomery • Closed at level of true and false VF • Technique • Midline thyrotomy - to expose endolarynx • True and false VF, ventricles, and posterior commissure - denuded of mucosa • Nonabsorbable sutures – to provide glottic closure • Absorbable sutures - approximate margins of false vocal cords • Tracheotomy tube necessary
- 88. NARROW- FIELD LARYNGECTOMY • Before 1970, laryngectomy - considered surgical procedure of choice • Can be performed with LA • Preserves 1) Hyoid 2) Strap muscles 3) Hypopharyngeal mucosa as much as possible • Closure without tension and reinforced with strap muscle ( Minimizes post-op. complications of pharyngeal stenosis and fistula) • Tracheostomy is necessary
- 90. SUBPERICHONDRIAL CRICOIDECTOMY • Technique • Anterior aspect of cricoid cartilage exposed • Cricoid incision • Perichondrium of anterior cricoid cartilage- divided vertically in midline - expose cricoid cartilage
- 91. • Outer cricoid perichondrium – elevated to posterior cricoid lamina • Inner cricoid perichondrium – elevated from cricoid cartilage circumferentially • Cricoid cartilage - removed piecemeal - bilaterally with biting forceps • Posterior cricoid lamina - preserved
- 92. • Inner perichondrium and mucosa - divided and closed • Both proximal and distal cut ends of inner mucosal tube are folded in and closed
- 93. • Sternohyoid muscle – insinuated into cricoid space • Outer perichondrium closed over muscle • Tracheotomy is necessary
- 94. • Advantage • High success rate • Low morbidity • Preferable to narrow-field laryngectomy and other procedure • Disadvantages • Irreversible • Need for tracheotomy • Possibility of fistula into upper trachea
- 95. RECENT ADVANCES • In recent years, botulinum toxin (botox) injection – used in laryngeal synkinesis • Currently being investigated include • Gene therapy • Stem cell therapy • Laryngeal pacing
- 96. BOTULINUM TOXIN • Neurotoxin - by clostridium botulinum • Prevents - release of acetylcholine from axon terminals - causes flaccid paralysis • In case of BVFP, • Used to block aberrant reinnervation of adductor muscles by inspiratory motoneurons • Thus, abductor inspiratory motoneurons would gain advantage and become more effective in producing glottal opening • Marie et al. - First described botox injection into bilateral adductor muscles as a treatment for BVFP
- 97. GENE THERAPY • Delivering genes by vector to injured neurons and/or denervated muscles • After genes are transduced into nucleus of target cells • Produce peptides • Promote a) RLN regeneration, synaptic formation b) muscle growth • Patients with BVFP caused by neurodegenerative diseases - benefited
- 98. STEM CELL THERAPY • Improve healing potential in degenerative tissue by tissue regeneration • Autologous stem cells - isolated from small samples of tissue from patients – cultured to a critical mass - re-implanted • May promote a) regrowth of atrophic muscle mass b) provide better platform for reinnervation • Halum et al. (2007) - introduced use of autologous muscle-derived stem cell for treatment of VFP
- 99. LARYNGEAL PACING • Application of functional electrical stimulation (FES) of the PCA muscle • Mueller and his associates - recently conducted a clinical trial of unilateral pacing in 9 patients with BVFP • Used minimally invasive electrodes activated by an external pacemaker affixed to the chest wall • Significant improvement in ventilation ( no negative effect on voice quality)