Upper and Lower Extremity fractures
- 2. Hand Fracture • A hand fracture is a break in one of the bones in the hand. This includes the small bones of the fingers (phalanges) and the long bones within the palm (metacarpals). Cause: A broken hand can be caused by a fall, crush injury, twisting injury, or through direct contact in sports. Tx: In most cases, a hand fracture will heal well with nonsurgical treatment • Cast • Splint • Buddy strap
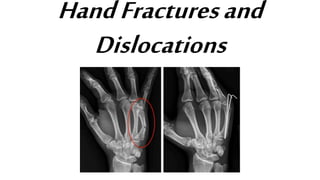
- 3. Surgical Treatment - Small devices such as wires, screws, pins, staples and plates may be used to hold the pieces of fractured bone in place - (Left) X-ray shows a metacarpal fracture of the ring finger. (Right) Here, the fracture has been repaired with a plate and screws. - (Left) X-ray shows fractures in the phalanges of two fingers. (Right) In this x-ray, the fractures have been repaired with screws.
- 4. • Signs and symptoms of a hand fracture may include: • Swelling • Bruising • Tenderness or pain • Deformity • Inability to move the finger • Shortened finger • The injured finger crosses or “scissors” over its neighbor when making a partial fist Diagnostic exam: X-ray Complications: - Fingers may become stiff
- 5. Fracture of Metacarpal: Boxer’s fracture• A Boxer’s fracture refers to a break at the end of the bone nearest the knuckle of the little finger. Cause: This type of fracture commonly occurs when someone punches a hard surface with a closed fist in which the little finger knuckle makes contact first.
- 6. Treatment Tx: Most Boxer’s fractures can be treated with a cast to stabilize the fracture. If the knuckle is severely deformed a procedure called a closed reduction may be needed to push the fracture back into proper alignment before casting. Closed reduction
- 7. Fracture of Finger: Busch’s fracture• is a type of fracture of the base of the distal phalanx of the fingers, produced by the removal of the bone insertion (avulsion) of the extensor tendon. Cause: is very common in motorcycle riders and soccer joggers, caused by a hyperflexion when the tendon is exercising the maximum tension (the closed hand tightening the clutch lever or the brake lever
- 9. Fracture of Metacarpal: Benett fracture• is a fracture of the base of the first metacarpal bone which extends into the carpometacarpal (CMC) joint. Cause: • When a person punches a hard object • It can also occur as a result of a fall onto the thumb. • Bike falls Complications: • tension from the abductor pollicis longus muscle (APL) subluxates the fragment in a dorsal, radial, and proximal direction • tension from the APL rotates the fragment into supination • tension from the adductor pollicis muscle displaces the metacarpal head into the palm
- 10. Tx: Closed reduction and percutaneous pin fixation (CRPP) with Kirschner wires Reduction of the displaced Benett fracture, dislocation is achieved by longitudinal traction of the end of the thumb coupled with abduction Benett fracture reduced and stabilize by percutaneous K- wire pinning Kirschner wire
- 12. Scaphoid fracture • is a break of the scaphoid bone in the wrist. Cause: Scaphoid fractures are most commonly caused by a fall on an outstretched hand Diagnostic exam: X-ray Complications: -AVN -Non union
- 13. Non surgical treatment Surgical - Wrist guard - Percutaenous screw fixation - Cast Scaphoid fracture stabilization by percutaneous screw fixation S/Sx swelling and tenderness over the thumb sideof the wrist. There is noticeable tenderness to the touch over the “anatomical snuff box.” Crunchiness and pain with gripping motions are also common symptoms that may be found with such an injury.
- 14. Fracture of the Phalanges: Tuftfracture • A break in any of the distal phalanges Cause: - Crush injuries Non-surgical tx: - Splint Complications: -Avulsion of the nail plate - Non union
- 16. Hand Dislocations: Wrist There are a few different types of wrist dislocations. They include: • Anterior lunate dislocation. The lunate bone rotates while the other wrist bones remain in place. • Perilunate dislocation. This type involves the lunate bone and the three ligaments around it. Lunate dislocations typically occur in young adults with Lunate dislocations typically occur in young adults with high energy trauma resulting in loading of a dorsiflexed wrist Anterior lunate dislocation Perilunate dislocation
- 17. • Wrist dislocation: Pain is usually localized to the dorsum of the wrist over the radioulnar joint. Pronation or supination against resistance causes pain, and occasionally, a click may be heard when the wrist is rotated. X-ray examination findings are usually grossly negative. - Dorsal dislocation - Volar dislocation
- 18. PIP Dislocation • dorsal dislocations results from PIPJ hyperextension with longitudinal compression (i.e. ball striking fingertip) - leads to tearing of the collateral ligaments and shearing of the volar plate off of the base of middle phalanx • Volar dislocation • dislocation without rotation, results from rupture of central slip • dorsal dislocations can lead to a swan neck deformity • volar dislocations can lead to a boutonniere deformity
- 19. Radius and Ulna shaft fractures
- 20. Radias shaft fracture • Isolated fractures of the radial shaft (proximal two-thirds) are less common than distal radius fractures. Cause: These injuries usually occur from either a direct blow to the forearm or a fall on outstretched hands Complications: include compartment syndrome, malunion, nonunion, infection, neurovascular damage, and synostosis.
- 21. Tx: - Sugar tong splint Generally the standard of care for radial shaft fractures is open reduction and internal fixation with 3.5mm dynamic compression plating is the treatment of choice.
- 22. Ulna shaft fracture: Nighstick fracture• isolated fractures of the ulna, typically transverse and located in the mid-diaphysis Cause: Results from a direct blow Complications: they have a higher rate of delayed union or non-union.
- 23. Treatment Non-Surgical - Bandage - Plaster - Functional brace Surgical - Plate fixation This fracture was treated by a cast Complications: • Damage to the nerves or blood vessels of the forearm. • Abnormal pressure build- up within the muscles of the arm/elbow that reduces blood flow, preventing oxygen and nourishment from reaching the nerve and muscle cells (termed as forearm compartment syndrome)
- 24. Ulnar fracture: Monteggiafracture • is a fracture of the proximal third of the ulna with dislocation of the proximal head of the radius. It is named after Giovanni Battista Monteggia. Cause: - Fall on an outstretched hand with the forearm in excessive pronation - Direct blow on back of upper forearm would be a very uncommon cause. Complications: - union or non-union.
- 25. Treatment: • Closed reduction • resetting and casting • Osteosynthesis
- 26. Classifications • I - Extension type (60%) - ulna shaft angulates anteriorly (extends) and radial head dislocates anteriorly. • II - Flexion type (15%) - ulna shaft angulates posteriorly (flexes) and radial head dislocates posteriorly. • III - Lateral type (20%) - ulna shaft angulates laterally (bent to outside) and radial head dislocates to the side. • IV - Combined type (5%) - ulna shaft and radial shaft are both fractured and radial head is dislocated, typically anteriorly
- 27. Ulnar fracture: Hume fracture The Hume fracture is an injury of the elbow comprising a fracture of the olecranon with an associated anterior dislocation of the radial head which occurs in children. Cause: - usually results in comminuted fracture - fall onto outstretched upper extremity - usually results in transverse or oblique fracture Hyperextension of the elbow
- 28. Treatment • Tension band technique Surgical - Intramedullary fixation - Plate and screw fixator - excision and triceps advancement
- 29. Complications • Stiffness • Heterotopic ossification • Posttraumatic arthritis • Nonunion • Anterior interosseous nerve injury • Loss of extension strength
- 30. Distal Radius fracture • A distal radius fracture almost always occurs about 1 inch from the end of the bone. The break can occur in many different ways, however. Other ways the distal radius can break include: • Intra-articular fracture. A fracture that extends into the wrist joint. ("Articular" means "joint.") • Extra-articular fracture. A fracture that does not extend into the joint is called an extra-articular fracture. • Open fracture. When a fractured bone breaks the skin, it is called an open fracture. These types of fractures require immediate medical attention because of the risk for infection. • Comminuted fracture. When a bone is broken into more than two pieces, it is called a comminuted fracture.
- 31. Cause: The most common cause of a distal radius fracture is a fall onto an outstretched arm. S/Sx: • A broken wrist usually causes immediate pain, tenderness, bruising, and swelling. In many cases, the wrist hangs in an odd or bent way (deformity). Non-Surgical Tx: - Plaster cast - Reduction - Splint Surgical: A plate and screws hold the broken fragments in position while they heal. External fixator
- 32. Reduction of Distal Radius fracture
- 33. Distal Radius fracture: Colles fracture • The term has come to mean a fracture within 1 inch of the distal end of the radius and is one of the commonest fractures of middle and old age. • The fracture may be comminuted as the bone is frequently osteoporotic. The styloid process of the ulna is often avulsed.
- 34. Complications: • Median nerve compression • Malunion • Rapture of tendon Treatment: - Reduction Surgical Tx: - Plates, screws, pins, external fixator
- 35. Distal Radius fracture: Smith’s fracture • This is a fracture of the lower end of the radius with palmar angulation. Cause: It is caused by a direct blow to the dorsal forearm Tx: Treatment Smith’s fracture is usually treated by open reduction and internal fixation with a plate applied to the palmar aspect of the radius.
- 36. Distal Radius fracture: Galleazi • is a fracture of the distal third of the radius with dislocation of the distal radioulnar joint. • the injury disrupts the forearm axis joint. • Cause: a fall that causes an axial load to be placed on a hyperpronated forearm.
- 38. S/Sx • Pain and soft-tissue swelling are present at the distal- third radial fracture site and at the wrist joint • AIN palsy • Wrist drop Treatment • Galeazzi fractures are best treated with open reduction of the radius and the distal radio-ulnar joint.
- 39. Distal Radius fracture: Barton’s fracture • is an intra-articular fracture of the distal radius with dislocation of the radiocarpal joint. Cause: - fall on an extended and pronated wrist increasing carpal compression force on the dorsal rim. Two types: volar and dorsal (based on direction of dislocation)
- 40. Complications • Malunion however is a common complication and is related to radial shortening, angulation and incongruity of the articular surface. • OA Tx: Closed reduction Kirschner wire External fixator Fracture treated with closed reduction, k wire and external fixator
- 41. Radial fracture: Essex-Lopresti fracture • is a fracture of the radial head with concomitant dislocation of the distal radio-ulnar joint and disruption of the interosseous membrane. Cause • This fracture occurs in patients who have fallen from a height.
- 42. Treatment • Open reducation and internal fixation • Radial head implant Complication: Delayed treatment of the radial head fracture will also lead to proximal migration of the radius
- 43. Elbowfracture• Elbow fractures are common childhood injuries, accounting for about 10% of all childhood fractures. Types of elbow fracture Above the elbow (supracondylar) - In this type of fracture, the upper arm bone (humerus) breaks slightly above the elbow. At the elbow knob (condylar) - This type of fracture occurs through one of the bony knobs (condyles) at the end of the upper arm bone. • At the inside of the elbow tip (epicondylar) - Fractures at this point usually occur on the inside, or medial, epicondyle in children from 9 to14 years of age. • Growth plate (physis) - The upper arm bone and both forearm bones have areas of cartilage called growth plates located near the end of the bone.
- 44. Causes: • A fall on an outstretched arm • A fall directly on the elbow • A direct blow to the elbow S/Sx • Swelling and pain • Numbness in the hand, a sign of potential nerve injury • Inability to straighten the arm Non-surgical Tx - Cast - Splint Surgical - Closed reduction and percutaneous pinning - Open reduction and internal fixation. This x-ray shows a supracondylar humerus fracture that has been put into the correct position and held in place with two pins. The pins will be removed after healing has begun.
- 46. DislocationofElbow • This is usually produced by a fall on the hand with the elbow partially flexed. Clinical features: The elbow is swollen and held in a flexed position. The ulna is displaced backwards on the lower end of the humerus. The radial head may be fractured, as may the coronoid process. Complications: Median nerve palsy occasionally occurs, but the prognosis for recovery is good. Brachial artery damage is rare.
- 47. Treatment • Reduction • The elbow is then initially immobilized in a simple sling or collar and cuff
- 48. Humeral Fracture • A humerus fracture is an injury to the bone of the upper arm that connects the shoulder to the elbow. Humerus fractures are generally divided into three types of injuries based on the location of the fracture. Cause: • Humerus fractures can occur by many different injuries but are most commonly caused by falls. • Automobile accidents
- 49. Treatment Non-surgical - Sling - Brace - Surgery may be required when the bone fragments are far out of position. Complications - Nonunion - Malunion - Nerve Injury - Shoulder or elbow stiffness
- 50. ProximalHumerusfracture • Proximal humerus fractures occur near the shoulder joint. • These fractures may involve the insertion of the important rotator cuff tendons. • Because these tendons are important to shoulder motion, treatment may depend on the position of these tendon insertions.
- 51. Mid-shaftHumerusfracture • Mid-shaft humerus fractures occur away from the shoulder and elbow joints. • Most humeral shaft fractures will heal without surgery, but there are some situations that require surgical intervention. • These injuries are commonly associated with injury to one of the large nerves in the arm, called the radial nerve. Injury to this nerve may cause symptoms in the wrist and hand.
- 52. DistalHumerusfracture • Distal humerus fractures are uncommon injuries in adults. These fractures occur near the elbow joint. • These fractures most often require surgical treatment unless the bones are held in proper position. • This type of fracture is much more common in children, but the treatment is very different in this age group.
- 53. Humeral Fracture: Fracture of Humeral neck • These fractures are often classifi ed as abduction or adduction types, depending on the relative positions of the proximal and distal fragments. • They are often comminuted, with the greater tuberosity forming a separate fragment. Stable fractures are impacted and may be safely mobilized early. Non - impacted fractures may be considerably displaced and can be associated with damage to the brachial plexus or axillary artery.
- 54. Treatment: • In this group of patients a broad sling is used to support the arm initially, but mobilization is encouraged as soon as possible.
- 55. Holstein–Lewis fracture • is a fracture of the distal third of the humerus resulting in entrapment of the radial nerve Treatment: - Cast - Plate fixation of humerus Complication: Radial nerve palsy
- 56. Clavicularfracture • also known as a broken collarbone, is a bone fracture of the clavicle. Cause: It is often caused by a fall onto a shoulder, outstretched arm, or direct trauma. Complications: • Include a collection of air in the pleural space surrounding the lung (pneumothorax), injury to the nerves or blood vessels in the area, and an unpleasant appearance
- 57. Signs and symptoms • Pain and Swelling • Sharp pain when any movement is made • Referred pain: dull to extreme ache in and around clavicle area, including surrounding muscles • Possible nausea, dizziness, and/or spotty vision due to extreme pain Non surgical Tx: - Figure of 8 splint - sling
- 58. Fracture of the Scapula • A scapular fracture is a fracture of the scapula, the shoulder blade. Cause: This could be anywhere from a car accident, motorcycle crash, or high speed bicycle crash but falls and blows to the area can also be responsible for the injury. S/Sx: Signs and symptoms are similar to those of other fractures: they include pain, tenderness, and reduced motion of the affected area although symptoms can take a couple of days to appear.
- 59. Treatment • Treatment involves pain medication and immobilization at first; later, physical therapy is used. • Ice over the affected area may increase comfort. • Movement exercises are begun within at least a week of the injury; with these, fractures with little or no displacement heal without problems. • Over 90% of scapular fractures are not significantly displaced; therefore, most of these fractures are best managed without surgery
- 60. Classification • Described based upon anatomic location Coracoid process fractures Type 1 Fracture proximal to the coracoclavi cular ligament Type 2 Fracture distal to the coracoclavi cular ligament
- 61. Acromion fractures Type 1 Non- or minimally-displaced Type 2 Displaced but not affecting the subacromial space Type 3 Displacement compromising the subacromial space
- 62. Acromioclavicular fracture • The distal clavicle and acromion process can also be fractured. Injury to the acromioclavicular joint may injure the cartilage within the joint and can later cause arthritis of the acromioclavicular joint. Cause: Acromioclavicular joint injuries are often seen after bicycle wrecks, contact sports, and car accidents.
- 63. Pathophysiology • The most common mechanism for an acromioclavicular joint injury is a fall directly onto the acromion, with the arm adducted up against the body. • When a person falls onto their shoulder, the force pushes the tip of the shoulder down. The clavicle is usually kept in its anatomic position, whereas the shoulder is driven down, which injures the different ligaments or causes a fracture. • A fall onto an outstretched hand (FOOSH injury) and a downward force on the upper extremity have also been implicated in acromioclavicular joint injuries.
- 64. ShoulderDislocations • Anterior dislocations of the shoulder are caused by the arm being forcefully twisted outward (external rotation) when the arm is above the level of the shoulder. These injuries can occur from many different causes, including a fall or a direct blow to the shoulder.
- 65. • Posterior dislocations of the shoulder are much less common than anterior dislocations of the shoulder. Posterior dislocations often occur from seizures or electric shocks when the muscles of the front of the shoulder contract and forcefully tighten.
- 66. LOWER EXTREMITY FRACTURE & DISLOCATION
- 67. HIP FRACTURE
- 68. DEFINITION • is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture is primarily based on the bones and soft tissues affected or on the level of the fracture.
- 69. CAUSES • Hip fractures most commonly occur from a fall or from a direct blow to the side of the hip. • Some medical conditions such as osteoporosis, cancer, or stress injuries can weaken the bone and make the hip more susceptible to breaking. In severe cases, it is possible for the hip to break with the patient merely standing on the leg and twisting.
- 70. SYMPTOMS • Pain over the outer upper thigh or in the groin. • Significant discomfort with any attempt to flex or rotate the hip. • If the bone has been weakened by disease, the patient may notice aching in the groin or thigh area for a period of time before the break. • If the bone is completely broken, the leg may appear to be shorter than the non-injured leg. • Patient will often hold the injured leg in a still position with the foot and knee turned outward (external rotation).
- 71. DIAGNOSTIC PROCEDURES • X-ray • MRI • CT SCAN
- 72. TYPES OF HIP FRACTURES 1. Intracapsular Fracture: oOccur at the level of the neck and the head of the femur, and is generally within the capsule.
- 73. TYPES OF HIP FRACTURES 2. Intertrochanteric Fracture: o Occurs between the neck of the femur and a lower bony prominence called the lesser trochanter. o Intertrochanteric fractures generally cross in the area between the lesser trochanter and the greater trochanter.
- 74. TYPES OF HIP FRACTURES 3. Subtrochanteric Fracture: o This fracture occurs below the lesser trochanter, in a region that is between the lesser trochanter and an area approximately 2 1/2 inches below . o In more complicated cases, the amount of breakage of the bone can involve more than one of these zones. This is taken into consideration when surgical repair is considered.
- 75. TREATMENT • CONSIDERATIONS: • In very rare cases, If patient is very ill then surgery would not be recommended. In these cases, the patient's overall comfort and level of pain must be weighed against the risks of anesthesia and surgery. • Most surgeons agree that patients do better if they are operated on fairly quickly. It is, however, important to insure patients' safety and maximize their overall medical health before surgery. This may mean taking time to do cardiac and other diagnostic studies.
- 76. TREATMENT • NONSURGICAL TREATMENT: • Activity Modification • Electronic and Ultrasonic Bone Stimulation • Physical Therapy • Pain Medications • Avoiding Nonsteroidal Anti-Inflammatory Drugs
- 77. TREATMENT • SURGICAL TREATMENT: • Before Surgery • Anesthesia for surgery could be either general anesthesia with a breathing tube or spinal anesthesia. In very rare circumstances, where only a few screws are planned for fixation, local anesthesia with heavy sedation can be considered. All patients will receive antibiotics during surgery and for the 24-hours afterward. • Appropriate blood tests, chest X-rays, electrocardiograms, and urine samples will be obtained before surgery. Many elderly patients may have undiagnosed urinary tract infections that could lead to an infection of the hip after surgery.
- 78. TREATMENT 1. Intracapsular Fracture: o If the head of the femur ("ball") alone is broken, management will be aimed at fixing the cartilage on the ball that has been injured or displaced. Frequently with these injuries, the socket, or acetabulum, may also be broken. The surgeon will need to take this into consideration as well. o These injuries may be approached either from the front or back of the hip. In some cases, both approaches are required in order to clearly see and fix the injured bone. o For true intracapsular hip fractures, the surgeon may decide either to fix the fracture with individual screws (percutaneous pinning) or a single larger screw that slides within the barrel of a plate. This compression hip screw will allow the fracture to become more stable by having the broken area impact on itself. Occasionally, a secondary screw may be added for stability.
- 79. Repair of an intracapsular fracture with individual screws. Repair of an intercapsular fracture with a single compression hip screw
- 80. TREATMENT oIf the intracapsular hip fracture is displaced in a younger patient, a surgical attempt will be made to reduce or realign the fracture through a larger incision. The fracture will be held together with either individual screws or with the larger compression hip screw. oIn these cases, the blood supply to the ball, or head of the femur, may have been damaged at the time of injury (avascular necrosis). Even though the fracture is realigned and fixed into place, the cartilage and underlying supporting bone may not receive adequate blood. Over a period of time, this may cause the femoral head to flatten out. When this occurs, the joint surface becomes irregular. Ultimately, the hip joint may develop a painful arthritis, despite the surgical repair.
- 81. Although the fracture is repaired, the blood supply to the "ball" of the femur is damaged.
- 82. TREATMENT oIn the older patient, the chance that the head of the femur is damaged in this way is higher. It is generally felt that for these displaced fractures, patients will do better if some of the components of the hip are replaced. In some cases, this can mean a replacement of the ball, or head of the femur (hemiarthroplasty). In other cases, this can mean the replacement of both the ball and socket, or head of the femur and acetabulum (total hip replacement).
- 83. Hemiarthroplasty is a type of hip replacement in which only the "ball" of the hip is replaced. A total hip replacement replaces both the hip socket and ball.
- 84. TREATMENT 2. Intertrochanteric Fracture: o Most intertrochanteric fractures are managed with either a compression hip screw or an intramedullary nail, which also allows for impaction at the fracture site. o The compression hip screw is fixed to the outer side of the bone with bone screws and has a large secondary screw (lag screw) that is placed through the plate into the neck and head of the hip. The design of the device allows for impaction and compression at the fracture site. This may increase the stability of the area and promote healing. o The intramedullary nail is placed directly into the marrow canal of the bone through an opening made at the top of the greater trochanter. A lag screw is then placed through the nail and up into the neck and head of the hip. As with the compression hip screw, sliding of the lag screw and impaction of the fracture take place.
- 85. Repair of an intertrochanteric fracture with an intramedullary nail. The nail is in the hollow cavity of the femur (thighbone) rather than on the side of it (as with a plate).
- 86. TREATMENT 3. Subtrochanteric Fracture: oAt the subtrochanteric level, most fractures are managed with a long intramedullary nail together with a large lag screw or they are managed with screws that capture the neck and head of the femur or the area immediately underneath it, if it has remained intact.
- 87. Repair of subtrochanteric fracture with a long intramedullary nail. Interlocking screws at the end of the nail make the fixation more secure.
- 88. TREATMENT oIn order to keep the bones from rotating around the nail or from shortening ("telescoping") on the nail, additional screws may be placed at the lower end of the nail in the area of the knee. These are called interlocking screws. oIn certain cases, the surgeon may choose to use a plate rather than a nail. The plate will have screws that go into the bone from the lateral, or outer, side of the femur. A single large screw goes into the neck and the head of the femur and appears similar to the compression hip screw, but at a different angle. Secondary screws are then placed through the plate into the bone to hold the fracture in place.
- 89. A locking plate may be used for more difficult to treat fractures.
- 90. HIP DISLOCATION
- 91. DEFINITION • Occurs when the head of the thighbone (femur) is forced out of its socket in the hip bone (pelvis). • It typically takes a major force to dislocate the hip. Car collisions and falls from significant heights are common causes and as a result, other injuries like broken bones often occur with the dislocation. • A hip dislocation is a serious medical emergency. Immediate treatment is necessary.
- 92. DESCRIPTION • POSTERIOR DISLOCATION: • In approximately 90% of hip dislocation patients, the thighbone is pushed out of the socket in a backwards direction. This is called a posterior dislocation. • A posterior dislocation leaves the lower leg in a fixed position, with the knee and foot rotated in toward the middle of the body.
- 93. DESCRIPTION • ANTERIOR DISLOCATION: • When the thighbone slips out of its socket in a forward direction, the hip will be bent only slightly, and the leg will rotate out and away from the middle of the body. • When the hip dislocates, the ligaments, labrum, muscles, and other soft tissues holding the bones in place are often damaged, as well. The nerves around the hip may also be injured.
- 94. SYMPTOMS • Very painful • Unable to move the leg • If there is nerve damage, may not have any feeling in the foot or ankle area.
- 95. CAUSE • Motor vehicle collisions are the most common cause of hip dislocations. The dislocation often occurs when the knee hits the dashboard in a collision. This force drives the thigh backwards, which drives the ball head of the femur out of the hip socket. • A fall from a significant height (such as from a ladder) or an industrial accident can also generate enough force to dislocate a hip. • With hip dislocations, there are often other related injuries, such as fractures in the pelvis and legs, and back, abdominal, knee, and head injuries. • Perhaps the most common fracture occurs when the head of the femur hits and breaks off the back part of the hip socket during the injury. This is called a posterior wall acetabular fracture-dislocation.
- 97. TREATMENT • REDUCTION PROCEDURES: • If there are no other injuries, the doctor will administer an anesthetic or a sedative and manipulate the bones back into their proper position. This is called a reduction. • In some cases, the reduction must be done in the operating room with anesthesia. In rare cases, torn soft tissues or small bony fragments block the bone from going back into the socket. When this occurs, surgery is required to remove the loose tissues and correctly position the bones. • Following reduction, the surgeon will request another set of x-rays and possibly a computed tomography (CT) scan to make sure that the bones are in the proper position.
- 98. (Left) This x-ray, taken from the front, shows a patient with a posterior dislocation of the left hip. (Right) Normal alignment after the hip has been reduced.
- 99. COMPLICATIONS • A hip dislocation can have long-term consequences, particularly if there are associated fractures. • Nerve injury – As the thighbone is pushed out of the socket, particularly in posterior dislocations, it can crush and stretch nerves in the hip. The sciatic nerve, which extends from the lower back down the back of the legs, is the nerve most commonly affected. Injury to the sciatic nerve may cause weakness in the lower leg and affect the ability to move the knee, ankle and foot normally. Sciatic nerve injury occurs in approximately 10% of hip dislocation patients. The majority of these patients will experience some nerve recovery.
- 100. COMPLICATIONS • Osteonecrosis – As the thighbone is pushed out of the socket, it can tear blood vessels and nerves. When blood supply to the bone is lost, the bone can die, resulting in osteonecrosis (also called avascular necrosis). This is a painful condition that can ultimately lead to the destruction of the hip joint and arthritis. • Arthritis – The protective cartilage covering the bone may also be damaged, which increases the risk of developing arthritis in the joint. Arthritis can eventually lead to the need for other procedures, like a total hip replacement.
- 101. FEMUR SHAFT FRACTURE
- 102. DEFINITION • Femur (Thighbone) is the longest and strongest bone in the body. Because the femur is so strong, it usually takes a lot of force to break it. Motor vehicle collisions, for example, are the number one cause of femur fractures. • The long, straight part of the femur is called the femoral shaft. When there is a break anywhere along this length of bone, it is called a femoral shaft fracture. This type of broken leg almost always requires surgery to heal.
- 103. TYPES OF FEMORAL SHAFT FRACTURES • Fractures are describe using a classification systems. Femur fractures are classified depending on: • The location of the fracture • The pattern of the fracture • Whether the skin and muscle over the bone is torn by the injury
- 104. TYPES OF FEMORAL SHAFT FRACTURES • The most common types of femoral shaft fractures include: • Transverse fracture: the break is a straight horizontal line going across the femoral shaft. • Oblique fracture: This type of fracture has an angled line across the shaft. • Spiral fracture: The fracture line encircles the shaft like the stripes on a candy cane. A twisting force to the thigh causes this type of fracture. • Comminuted fracture: the bone has broken into three or more pieces. In most cases, the number of bone fragments corresponds with the amount of force needed to break the bone. • Open (Compound) fracture: If a bone breaks in such a way that bone fragments stick out through the skin or a wound penetrates down to the broken bone. Open fractures often involve much more damage to the surrounding muscles, tendons, and ligaments. They have a higher risk for complications—especially infections—and take a longer time to heal.
- 105. (Left) An oblique fracture has an angled line across the shaft. (Right) A comminuted fracture is broken into three or more pieces.
- 106. CAUSE • Femoral shaft fractures in young people are frequently due to some type of high-energy collision. The most common cause of femoral shaft fracture is a motor vehicle or motorcycle crash. • Being hit by a car while walking is another common cause, as are falls from heights and gunshot wounds. • A lower-force incident, such as a fall from standing, may cause a femoral shaft fracture in an older person who has weaker bones.
- 107. SYMPTOMS • Immediate, severe pain • Unable to put weight on the injured leg, • May look deformed—shorter than the other leg and no longer straight.
- 108. DIAGNOSTIC PROCEDURES • Medical History and Physical Examination • Assessment: • Visual Inspection: An obvious deformity of the thigh/leg (an unusual angle, twisting, or shortening of the leg), Breaks in the skin, Bruises, and Bony pieces that may be pushing on the skin. • Palpation • STD • ROM • X-ray • CT SCAN
- 109. TREATMENT • NONSURGICAL TREATMENT: • Cast (For very young children) • But most femoral shaft fractures require surgery to heal. It is unusual for femoral shaft fractures to be treated without surgery.
- 110. TREATMENT • SURGICAL TREATMENT: • Timing of Surgery • Most femur fractures are fixed within 24 to 48 hours. On occasion, fixation will be delayed until other life-threatening injuries or unstable medical conditions are stabilized. To reduce the risk of infection, open fractures are treated with antibiotics as soon as you arrive at the hospital. The open wound, tissues, and bone will be cleaned during surgery. • For the time between initial emergency care and your surgery, your doctor may place your leg either in a long-leg splint or in traction. This is to keep your broken bones as aligned as possible and to maintain the length of your leg. • Skeletal traction is a pulley system of weights and counterweights that holds the broken pieces of bone together. It keeps your leg straight and often helps to relieve pain.
- 111. TREATMENT 1. External Fixation: o In this type of operation, metal pins or screws are placed into the bone above and below the fracture site. The pins and screws are attached to a bar outside the skin. This device is a stabilizing frame that holds the bones in the proper position. o External fixation is usually a temporary treatment for femur fractures. Because they are easily applied, external fixators are often put on when a patient has multiple injuries and is not yet ready for a longer surgery to fix the fracture. An external fixator provides good, temporary stability until the patient is healthy enough for the final surgery. In some cases, an external fixator is left on until the femur is fully healed, but this is not common.
- 112. External fixation is often used to hold the bones together temporarily when the skin and muscles have been injured.
- 113. TREATMENT 2. Intramedullary Nailing: o Currently, the method most surgeons use for treating femoral shaft fractures is intramedullary nailing. oDuring this procedure, a specially designed metal rod is inserted into the canal of the femur. The rod passes across the fracture to keep it in position. oAn intramedullary nail can be inserted into the canal either at the hip or the knee. Screws are placed above and below the fracture to hold the leg in correct alignment while the bone heals. oIntramedullary nails are usually made of titanium. They come in various lengths and diameters to fit most femur bones.
- 114. (Left) a transverse fracture of the femur. (Right) femoral shaft fracture that has been treated with intramedullary nailing.
- 115. TREATMENT 3. Plates and Screws: • During this operation, the bone fragments are first repositioned (reduced) into their normal alignment. They are held together with screws and metal plates attached to the outer surface of the bone. • Plates and screws are often used when intramedullary nailing may not be possible, such as for fractures that extend into either the hip or knee joints.
- 116. COMPLICATIONS • Complications from Femoral Shaft Fractures: • The ends of broken bones are often sharp and can cut or tear surrounding blood vessels or nerves, though this is very rare. • Acute compartment syndrome may develop. This is a painful condition that occurs when pressure within the muscles builds to dangerous levels. This pressure can decrease blood flow, which prevents nourishment and oxygen from reaching nerve and muscle cells. Unless the pressure is relieved quickly, permanent disability may result. This is a surgical emergency. During the procedure, your surgeon makes incisions in your skin and the muscle coverings to relieve the pressure. • Open fractures expose the bone to the outside environment. Even with good surgical cleaning of the bone and muscle, the bone can become infected. Bone infection is difficult to treat and often requires multiple surgeries and long-term antibiotics. • Occasionally, the ligaments around the knee can be injured during a femoral shaft fracture. If you have knee pain after surgery, tell your doctor.
- 117. COMPLICATIONS • Complications from Surgery: • Blood loss • Problems with anesthesia • Infection • Injury to nerves and blood vessels • Blood clots • Fat embolism • Misalignment or the inability to correctly position the broken bone fragments • Delayed union or nonunion • Hardware irritation
- 119. DEFINITION • Fractures of the thighbone that occur just above the knee joint are called distal femur fractures. The distal femur is where the bone flares out like an upside-down funnel. • Distal femur fractures most often occur either in older people whose bones are weak, or in younger people who have high energy injuries, such as from a car crash. • In both the elderly and the young, the breaks may extend into the knee joint and may shatter the bone into many pieces.
- 120. DESCRIPTION • Distal femur fractures vary. The bone can break straight across (transverse fracture) or into many pieces (comminuted fracture). • Sometimes these fractures extend into the knee joint and separate the surface of the bone into a few (or many) parts. These types of fractures are called intra-articular. Because they damage the cartilage surface of the bone, intra-articular fractures can be more difficult to treat.
- 121. (Left) A transverse fracture across the distal femur. (Center) An intra-articular fracture that extends into the knee joint. (Right) A comminuted fracture that extends into the knee joint and upwards into the femoral shaft
- 122. DESCRIPTION • Distal femur fractures can be closed — meaning the skin is intact — or can be open. • When the distal femur breaks, both the hamstrings and quadriceps muscles tend to contract and shorten. When this happens the bone fragments change position and become difficult to line up with a cast.
- 123. The muscles at the front and back of the thigh have shortened and pulled the broken pieces of bone out of alignment.
- 124. CAUSE • Fractures of the distal femur most commonly occur in two patient types: younger people (under age 50) and the elderly. • Distal femur fractures in younger patients are usually caused by high energy injuries, such as falls from significant heights or motor vehicle collisions. Because of the forceful nature of these fractures, many patients also have other injuries, often of the head, chest, abdomen, pelvis, spine, and other limbs. • Elderly people with distal femur fractures typically have poor bone quality. As we age, our bones get thinner. Bones can become very weak and fragile. A lower-force event, such as a fall from standing, can cause a distal femur fracture in an older person who has weak bones. Although these patients do not often have other injuries, they may have concerning medical problems, such as conditions of the heart, lungs, and kidneys, and diabetes.
- 125. SYMPTOMS • The most common symptoms of distal femur fracture include: • Pain with weight bearing • Swelling and bruising • Tenderness to touch • Deformity: the knee may look "out of place" and the leg may appear shorter and crooked • In most cases, these symptoms occur around the knee, but you may also have symptoms in the thigh area.
- 126. DIAGNOSTIC PROCEDURE • Medical History and Physical Examination • X-ray • CT SCAN
- 127. TREATMENT • NONSURGICAL TREATMENT: • Skeletal traction • Casting and bracing • Patients with distal femoral fractures of all ages do best when they can be up and moving soon after treatment (such as moving from a bed to a chair, and walking). Early motion of the knee lessens the risk of knee stiffness, and prevents problems caused by extended bed rest, such as bed sores and blood clots.
- 128. TREATMENT • SURGICAL TREATMENT: • Timing of Surgery • Most distal femur fractures are not operated on right away — unless the skin around the fracture has been broken (open fracture) • In most cases, surgery is delayed 1 to 3 days to develop a treatment plan and to prepare the patient for surgery.
- 129. TREATMENT 1. External Fixation: ometal pins or screws are placed into the middle of the femur and tibia (shinbone). The pins and screws are attached to a bar outside the skin. This device is a stabilizing frame that holds the bones in the proper position until you are ready for surgery.
- 130. An external fixator is used to stabilize the fracture before surgery.
- 131. TREATMENT 2. Internal Fixation: o Methods most surgeons use for distal femur fractures include: • Intramedullary Nailing – a specially designed metal rod is inserted into the marrow canal of the femur. The rod passes across the fracture to keep it in position. • Plates and screws – the bone fragments are first repositioned (reduced) into their normal alignment. They are held together with special screws and metal plates attached to the outer surface of the bone. o Both of these methods can be done through one large incision or several smaller ones, depending on the type of fracture you have and the device your surgeon uses.
- 132. TREATMENT • If the fracture is in many small pieces above your knee joint, your surgeon will not try to piece the bone back together like a puzzle. • Instead, your surgeon will fix a plate or rod at both ends of the fracture without touching the many small pieces. This will keep the overall shape and length of the bone correct while it heals. The individual pieces will then fill in with new bone, called a callous.
- 133. Healed fractures treated with a plate (left) and a rod (right). When the femur breaks into several pieces, new bone will grow and fill in gaps during the healing process.
- 134. TREATMENT • In cases where a fracture may be slow to heal, such as when a patient is elderly with poor bone quality, a bone graft may be used to help the callous develop. Bone grafts may be obtained from the patient (most often taken from the pelvis) or from a tissue bank (cadaver bone). Other options include the use of artificial bone fillers. • In extreme cases, a fracture may be too complicated and the bone quality too poor to fix. These types of fractures are often treated by removing the fragments and replacing the bone with a knee replacement implant.
- 135. TREATMENT 3. Fractures and knee replacements These x-rays taken from the front (left) and the side (right) show a fracture near an artificial knee joint.
- 136. TREATMENT • Those fractures are typically treated with rods or plates, just like other distal femur fractures. In rare cases, the artificial implant must be removed and replaced with a larger implant. This procedure is called a revision and may be necessary if the implant is loose or not supported by surrounding good bone.
- 137. Fractures near knee implants may be treated with plates, rods, or with a revision surgery.
- 138. TREATMENT • SURGICAL COMPLICATIONS : • to prevent infection, intravenous antibiotics will be given before the procedure. Because blood clots in leg veins may develop after surgery, the doctor may also give blood thinners. • There will be blood loss during your surgery. How much blood is lost will depend upon the severity of your fracture and the procedure used to treat it. Your doctor will assess your blood level during the operation and, if low, will determine whether it is in your best interest to have a blood transfusion.
- 139. COMPLICATIONS • INFECTIONS: • Newer techniques in treating difficult fractures have cut the infection rate by more than a half: Currently less than 5% of patients have infections. If you have surgery, your doctor will give you antibiotics to help prevent infection. • Open fractures (those with tears in the skin) and high energy fractures (such as car accidents) are at higher risk for infection. If the infection is deep, it may involve the bone and the device used to fix the bone. • A bone infection can require long-term, intravenous antibiotic treatment, as well as several surgeries to clean out the infection.
- 140. COMPLICATIONS • STIFFNESS: • Some knee stiffness is expected after a distal femur fracture. Moving your knee soon after surgery is the best way to prevent stiffness. • BONE HEALING PROBLEMS: • In some cases, bone healing can be slow or not happen at all. If a follow-up x-ray shows rods, plates, and screws breaking or pulling out of the bone, it may be a sign that the bone is not healing. This can happen even if your fracture has been fixed well and you have followed your doctor's guidelines.
- 141. COMPLICATIONS • Open fractures and high energy fractures are most at risk for not healing. These challenging fractures are also most at risk for infection, and infection can cause bone healing problems. • To help the fracture heal, your doctor may suggest applying a bone graft to the fracture, and changing or adding to how it was fixed (plates, screws, rods).
- 142. COMPLICATIONS • KNEE ARTHRITIS: • Distal femur fractures that enter the knee joint may heal with a defect in the normally smooth surface of the joint. • Because the knee is the largest weight bearing joint in the body, any defect can damage the protective articular cartilage and, over time, result in arthritis. In some cases, the joint surface may wear down to bare bone. • Arthritis caused by fracture or injury is called post-traumatic arthritis. It can be treated like other forms of osteoarthritis — with physical therapy, braces, medications, and lifestyle changes. • In cases of severe arthritis that limits activity, a total knee replacement may be the best option to relieve symptoms.
- 143. KNEE DISLOCATION
- 144. KNEE DISLOCATION • Knee dislocations are ligamentous disruptions with loss of continuity of tibiofemoral articulation. • A combination of tears of the anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial collateral ligament (MCL), lateral collateral ligament (LCL), and other stabilizing structures are typical of knee dislocations. • The vast majority of knee dislocations involve disruption of both the ACL and PCL.
- 145. KNEE DISLOCATION • Anterior displacement is considered the most common type of knee dislocation. • The least common type is the posterolateral dislocation. • They most commonly occur from high-energy mechanisms (motor-vehicle wrecks, industrial accidents), but they can also occur from low-energy trauma (sporting activities and minor falls). • In the absence of vascular and open injuries, treatment options include nonsurgical and surgical management options.
- 146. PATELLAR FRACTURE
- 147. DEFINITION • Patellar fracture is a break in the patella, or kneecap, the small bone that sits at the front of your knee. • Because the patella acts as a shield for your knee joint, it is vulnerable to fracture if you fall directly onto your knee or hit it against the dashboard in a vehicle collision. • A patellar fracture is a serious injury that can make it difficult or even impossible to straighten your knee or walk. • Some simple patellar fractures can be treated by wearing a cast or splint until the bone heals. • In most patellar fractures, however, the pieces of bone move out of place when the injury occurs. For these more complicated fractures, surgery is needed to restore and stabilize the kneecap and allow for the return of function.
- 148. DESCRIPTION • The patella can fracture in many ways. A fracture may be a simple, clean, two-piece break or the bone can break into many pieces. • A break can occur at the top, center, or lower part of the bone. Sometimes, fractures occur in more than one area of the kneecap.
- 149. This x-ray of a knee taken from the side shows a patella that has been fractured in three places.
- 150. TYPES OF PATELLAR FRACTURES • STABLE FRACTURE: • This type of fracture is nondisplaced. The pieces of bone may remain in contact with each other or be separated by just a millimeter or two. • In a stable fracture, the bones usually stay in place during healing.
- 151. TYPES OF PATELLAR FRACTURES • DISPLACED FRACTURE: • the broken ends of the bone are separated and do not line up correctly. The normally smooth joint surface may also be disrupted. • This type of fracture often requires surgery to put the pieces of bone back together.
- 152. TYPES OF PATELLAR FRACTURES • COMMINUTED FRACTURE: • the bone shatters into three or more pieces. Depending on the specific pattern of the fracture, a comminuted fracture may be either stable or unstable.
- 153. TYPES OF PATELLAR FRACTURES • OPEN FRACTURE: • the bone breaks in such a way that bone fragments stick out through the skin or a wound penetrates down to the bone. • An open fracture often involves damage to the surrounding soft tissues and may take a longer time to heal.
- 154. CAUSE • Patellar fractures are most often caused by: • Falling directly onto the knee • Receiving a sharp blow to the knee, such as might occur during a head-on vehicle collision if your kneecap is driven into the dashboard • The patella can also be fractured indirectly. For example, a sudden contraction of the quadriceps muscle in the knee can pull apart the patella.
- 155. SYMPTOMS • The most common symptoms of a patellar fracture are: • pain and swelling in the front of the knee. • Other symptoms may include: • Bruising • Inability to straighten the knee or keep it extended in a straight leg raise • Inability to walk
- 156. DIAGNOSTIC PROCEDURE • Physical Examination • X- Ray
- 157. TREATMENT • NONSURGICAL TREATMENT: • If the pieces of bone are not out of place (displaced), cast or splint may be apply to keep your knee straight and help prevent motion in your leg. This will keep the broken ends of bone in proper position while they heal. • Depending upon the specific fracture, weight bearing on the leg may be allowed while wearing a cast or brace. With some fractures, however, weight bearing is not allowed for 6 to 8 weeks.
- 158. TREATMENT • SURGICAL TREATMENT: • Fractured patellar bones that are not close together often have difficulty healing or may not heal. The thigh muscles that attach to the top of the patella are very strong and can pull the broken pieces out of place during healing. • Surgical Procedures – the type of procedure performed often depends on the type of fracture you have.
- 159. TREATMENT 1. TRANSVERSE FRACTURE : o These two-part fractures are most often fixed in place using screws or pins and wires and a "figure-of-eight" configuration tension band. The figure-of- eight band presses the two pieces together. o This procedure is best for treating fractures that are located near the center of the patella because pieces at the ends of the kneecap are too small for this procedure. o Another approach is to secure the bones using small screws or small screws and small plates.
- 160. TREATMENT 2. COMMINUTED FRACTURE: o In some fractures, the top or bottom (MC) of the patella is broken into several small pieces. o This type of fracture occurs when the kneecap is first pulled apart from the injury, and is then crushed when the patient falls on it. Because the bone fragments are too small to be fixed back into place, the doctor will remove them and then attach the loose patellar tendon back to the remaining patellar bone. o If the kneecap is broken in many pieces at its center and the pieces are separated, the doctor may use a combination of wires and screws to fix it. Removing small portions of the kneecap that cannot be reconstructed may also have good results. o Complete removal of the kneecap is a last resort in treating a comminuted fracture.
- 161. COMPLICATIONS OF PATELLAR FRACTURES • Posttraumatic Arthritis – is a type of arthritis that develops after an injury. Even when your bones heal normally, the articular cartilage covering the bones can be damaged, leading to pain and stiffness over time. Severe arthritis occurs in a small percentage of patients with patellar fractures. Mild to moderate arthritis—a condition called chondromalacia patella—is much more common. • Muscle Weakness – Some patients may have permanent weakness of the quadriceps muscle in the front of the thigh after a fracture. Some loss of motion in the knee, including both straightening (extension) and bending (flexion), is also common. This loss of motion is not usually disabling.
- 162. COMPLICATIONS OF PATELLAR FRACTURES • Chronic Pain – Long-term pain in the front of the knee is common with patellar fractures. While the cause of this pain is not completely understood, it is likely that it is related to posttraumatic arthritis, stiffness, and muscle weakness. Some patients find that they are more comfortable wearing a knee brace or support.
- 163. TIBIA & FIBULA FRACTURE
- 164. DEFINITION • The tibia, or shinbone, is the most commonly fractured long bone in the body. • A tibial shaft fracture occurs along the length of the bone, below the knee and above the ankle. • It typically takes a major force to cause this type of broken leg. Motor vehicle collisions, for example, are a common cause of tibial shaft fractures. • In many tibia fractures, the smaller bone in the lower leg (fibula) is broken as well.
- 165. TYPES OF TIBIA & FIBULA FRACTURE • TRANSVERSE FRACTURE: • In this type of fracture, the break is a straight horizontal line going across the tibial shaft. • OBLIQUE FRACTURE: • This type of fracture has an angled line across the shaft.
- 166. TYPES OF TIBIA & FIBULA FRACTURE • SPIRAL FRACTURE: • The fracture line encircles the shaft like the stripes on a candy cane. This type of fracture is caused by a twisting force. • COMMINUTED FRACTURE: • In this type of fracture, the bone breaks into three or more pieces. • OPEN FRACTURE: • If a bone breaks in such a way that bone fragments stick out through the skin or a wound penetrates down to the broken bone.
- 167. CAUSE • Tibial shaft fractures are often caused by some type of high-energy collision, such as a motor vehicle or motorcycle crash. In cases like these, the bone can be broken into several pieces (comminuted fracture). • Sports injuries, such as a fall while skiing or a collision with another player during soccer, are lower-energy injuries that can cause tibial shaft fractures. These fractures are typically caused by a twisting force and result in an oblique or spiral fracture.
- 168. SYMPTOMS • A tibial shaft fracture usually causes immediate, severe pain. • Other symptoms may include: • Inability to walk or bear weight on the leg • Deformity or instability of the leg • Bone "tenting" over the skin at the fracture site or bone protruding through a break in the skin • Occasional loss of feeling in the foot
- 169. DIAGNOSTIC PROCEDURE • Medical History and Physical Examination • X-ray • CT SCAN
- 170. TREATMENT • NONSURGICAL TREATMENT : • May be recommended for patients who: (1) are poor candidates for surgery due to their overall health problems; (2) less active, so are better able to tolerate small degrees of angulation or differences in leg length; (3) have closed fractures with minimal movement of the fracture ends • Initial treatment: most injuries cause some swelling for the first few weeks. Your doctor may initially apply a splint to provide comfort and support. Unlike a full cast, a splint can be tightened or loosened to allow swelling to occur safely. Once the swelling goes down, your doctor will consider a range of treatment options.
- 171. TREATMENT • Casting and bracing: may immobilize the fracture in a cast for initial healing. After several weeks, the cast can be replaced with a functional brace made of plastic and fasteners. The brace will provide protection and support until healing is complete. The brace can be taken off for hygiene purposes and for physical therapy.
- 172. TREATMENT • SURGICAL TREATMENT: • Surgery may be recommended for certain types of fractures, including: (1) Open fractures with wounds that need monitorinG; (2) Fractures that have not healed with nonsurgical treatment; (3) Fractures with many bone fragments and a large degree of displacement • Intramedullary nailing • Plates and screws • External fixation
- 173. COMPLICATIONS • Complications from Tibial Shaft Fractures: • The ends of broken bones are often sharp and can cut or tear surrounding muscles, nerves, or blood vessels. • Acute compartment syndrome may develop. This is a painful condition that occurs when pressure within the muscles builds to dangerous levels. This pressure can decrease blood flow, which prevents nourishment and oxygen from reaching nerve and muscle cells. Unless the pressure is relieved quickly, permanent disability may result. • Open fractures expose the bone to the outside environment. Even with good surgical cleaning of the bone and muscle, the bone can become infected. Bone infection is difficult to treat and often requires multiple surgeries and long-term antibiotics. • Complications from Surgery: • Infection • Injury to nerves and blood vessels • Blood clots (these may also occur without surgery) • Misalignment or the inability to correctly position the broken fragments • Delayed union or nonunion (when the fracture heals slower than usual or not at all) • Angulation (with treatment by external fixation)
- 174. ANKLE FRACTURE & DISLOCATION
- 175. DEFINITION • A broken ankle is also known as an ankle "fracture." This means that one or more of the bones that make up the ankle joint are broken. • A fractured ankle can range from a simple break in one bone, which may not stop you from walking, to several fractures which forces your ankle out of place and may require that you not put weight on it for a few months. • Simply put, the more bones that are broken, the more unstable the ankle becomes. There may be ligaments damaged as well. The ligaments of the ankle hold the ankle bones and joint in position. • Broken ankles affect people of all ages. During the past 30 to 40 years, doctors have noted an increase in the number and severity of broken ankles, due in part to an active, older population of "baby boomers."
- 176. TYPES OF ANKLE FRACTURE & DISLOCATION • LATERAL MALLEOLUS FRACTURE: • is a fracture of the fibula. • There are different levels at which that the fibula can be fractured. The level of the fracture may direct the treatment.
- 177. TYPES OF ANKLE FRACTURE & DISLOCATION • MEDIAL MALLEOLUS FRACTURE: • is a break in the tibia, at the inside of the lower leg. • Fractures can occur at different levels of the medial malleolus. • Medial malleoli fractures often occur with a fracture of the fibula (lateral malleolus), a fracture of the back of the tibia (posterior malleolus), or with an injury to the ankle ligaments.
- 178. TYPES OF ANKLE FRACTURE & DISLOCATION • POSTERIOR MALLEOLUS FRACTURE: • is a fracture of the back of the tibia at the level of the ankle joint. • In most cases of posterior malleolus fracture, the lateral malleolus (fibula) is also broken. This is because it shares ligament attachments with the posterior malleolus. There can also be a fracture of the medial malleolus. • Depending on how large the broken piece is, the back of the ankle may be unstable. Some studies have shown that if the piece is bigger than 25% of the ankle joint, the ankle becomes unstable and should be treated with surgery. • It is important for a posterior malleolus fracture to be diagnosed and treated properly because of the risk for developing arthritis. The back of the tibia where the bone breaks is covered with cartilage. Cartilage is the smooth surface that lines a joint. If the broken piece of bone is larger than about 25% of your ankle, and is out of place more than a couple of millimeters, the cartilage surface will not heal properly and the surface of the joint will not be smooth. This uneven surface typically leads to increased and uneven pressure on the joint surface, which leads to cartilage damage and the development of arthritis.
- 180. TYPES OF ANKLE FRACTURE & DISLOCATION • BIMALLEOLAR: • means that two of the three parts or malleoli of the ankle are broken. • In most cases of bimalleolar fracture, the lateral malleolus and the medial malleolus are broken and the ankle is not stable. • A "bimalleolar equivalent" fracture means that in addition to one of the malleoli being fractured, the ligaments on the inside (medial) side of the ankle are injured. Usually, this means that the fibula is broken along with injury to the medial ligaments, making the ankle unstable. • A stress test x-ray may be done to see whether the medial ligaments are injured. • Bimalleolar fractures or bimalleolar equivalent fractures are unstable fractures and can be associated with a dislocation.
- 182. TYPES OF ANKLE FRACTURE & DISLOCATION • TRIMALLEOLAR FRACTURES: • means that all three malleoli of the ankle are broken. These are unstable injuries and they can be associated with a dislocation.
- 183. CAUSE • Twisting or rotating your ankle • Rolling your ankle • Tripping or falling • Impact during a car accident
- 184. SYMPTOMS • Because a severe ankle sprain can feel the same as a broken ankle, every ankle injury should be evaluated by a physician. • Common symptoms for a broken ankle include: • Immediate and severe pain • Swelling • Bruising • Tender to touch • Cannot put any weight on the injured foot • Deformity ("out of place"), particularly if the ankle joint is dislocated as well
- 185. DIAGNOSTIC PROCEDURE • Medical History and Physical Examination • X-ray • Stress Test • CT SCAN • MRI
- 186. TREATMENT: LATERAL MALLEOLUS FRACTURE • NONSURGICAL TREATMENT: • Several different methods are used for protecting the fracture while it heals, ranging from a high-top tennis shoe to a short leg cast. • SURGICAL TREATMENT: • the bone fragments are first repositioned (reduced) into their normal alignment. They are held together with special screws and metal plates attached to the outer surface of the bone. • In some cases, a screw or rod inside the bone may be used to keep the bone fragments together while they heal.
- 187. TREATMENT: MEDIAL MALLEOLUS FRACTURE • NONSURGICAL TREATMENT: • The fracture may be treated with a short leg cast or a removable brace. • SURGICAL TREATMENT: • If the fracture is out of place or the ankle is unstable, surgery may be recommended. Though in some cases, surgery may be considered even if the fracture is not out of place. This is done to reduce the risk of the fracture not healing (called a nonunion), and to allow you to start moving the ankle earlier. • A medial malleolus fracture can include impaction or indenting of the ankle joint. Impaction occurs when a force is so great it drives the end of one bone into another one. Repairing an impacted fracture may require bone grafting. This graft acts as a scaffolding for new bone to grow on, and may lower any later risk of developing arthritis. • Depending on the fracture, the bone fragments may be fixed using screws, a plate and screws, or different wiring techniques.
- 188. TREATMENT: POSTERIOR MALLEOLUS FRACTURE • NONSURGICAL TREATMENT: • Treatment may be with a short leg cast or a removable brace. Patients are typically advised not to put any weight on the ankle for 6 weeks. • SURGICAL TREATMENT: • Different surgical options are available for treating posterior malleoli fractures. One option is to have screws placed from the front of the ankle to the back, or vice versa. Another option is to have a plate and screws placed along the back of the shin bone.
- 189. TREATMENT: BIMALLEOLAR FRACTURES/ BIMALLEOLAR EQUIVALENT FRACTURES • NONSURGICAL TREATMENT: • Immediate treatment typically includes a splint to immobilize the ankle until the swelling goes down. A short leg cast is then applied. Casts may be changed frequently as the swelling subsides in the ankle. • In most cases, weight bearing is not be allowed for 6 weeks. After 6 weeks, the ankle may be protected by a removable brace as it continues to heal. • SURGICAL TREATMENT: • treated with the same surgical techniques as written above for each fracture listed.
- 190. TREATMENT: TRIMALLEOLAR FRACTURES • NONSURGICAL TREATMENT: • Similar with bimalleolar fracture treatment • SURGICAL TREATMENT: • can be treated with the same surgical techniques as written above for each individual fracture.
- 191. COMPLICATIONS • People who smoke, have diabetes, or are elderly are at a higher risk for complications after surgery, including problems with wound healing. This is because it may take longer for their bones to heal. • NONSURGICAL TREATMENT: • Malunion • SURGICAL TREATMENT: • Infection • Bleeding • Pain • Blood clots in your leg • Damage to blood vessels, tendons, or nerves • Difficulty with bone healing • Arthritis • Pain from the plates and screws that are used to fix fracture. Some patients choose to have them removed several months after their fracture heals
- 192. FOOT FRACTURE & DISLOCATION
- 193. DEFINITION • Fractures of the toes and forefoot are quite common. Fractures can result from a direct blow to the foot—such as accidentally kicking something hard or dropping a heavy object on your toes. • They can also result from the overuse and repetitive stress that comes with participating in high-impact sports like running and basketball. • Although fracturing a bone in your toe or forefoot can be quite painful—it rarely requires surgery. In most cases, a fracture will heal with rest and a change in activities.
- 194. DESCRIPTION • Toe and forefoot fractures often result from trauma or direct injury to the bone. Fractures can also develop after repetitive activity, rather than a single injury. This is called a "stress fracture." • Fractures may either be "non-displaced," where the bone is cracked but the ends of the bone are together, or "displaced," where the end of the broken bones have partially or completely separated. • Fractures can also be divided into "closed fractures" where the skin is not broken and "open fractures" where the skin is broken and the wound extends down to the bone.
- 195. SYMPTOMS • The most common symptoms of a fracture are: • pain and swelling. • Other symptoms may include: • Bruising or discoloration that extends to nearby parts of the foot • Pain with walking and weight bearing
- 196. DIAGNOSTIC PROCEDURE • Physical Examination: • Swelling • Tenderness over the fracture site • Bruising or discoloration—your foot may be red or ecchymotic ("black and blue") • Deformity • Skin abrasions or open wounds • Loss of sensation—an indication of nerve injury • X-ray • MRI
- 197. FRACTURES OF THE TOES • Even though toes are very small, injuries to the toes can often be quite painful. • The proximal phalanx is the toe bone that is closest to the metatarsals. Because it is the longest of the toe bones, it is the most likely to fracture. • Cause: • A fracture of the toe may result from a direct injury, such as dropping a heavy object on the front of your foot, or from accidentally kicking or running into a hard object. • A fracture may also result if you accidentally hit the side of your foot on a piece of furniture on the ground— and your toes are twisted or pulled sideways or in an awkward direction. • Symptoms: • A fractured toe may become swollen, tender and discolored. • If the bone is out of place, your toe will appear deformed.
- 198. METATARSAL FRACTURES • The metatarsals are the long bones between your toes and the middle of your foot. Each metatarsal has the following four parts: • Head which makes a joint with the base of the toe • Neck which is the narrow area between the head and the shaft • Shaft which is the long part of the bone • Base which makes a joint with the midfoot • Fractures can occur in any part of the metatarsal, but most often occur in the neck or shaft of the bone. • Some metatarsal fractures are stress fractures. Stress fractures are small cracks in the surface of the bone that may extend and become larger over time.
- 199. METATARSAL FRACTURES • Cause: • Like toe fractures, metatarsal fractures can result from either a direct blow to the forefoot or from a twisting injury. • Stress fractures are typically caused by repetitive activity or pressure on the forefoot. They are common in runners and athletes who participate in high-impact sports such as soccer and basketball. • A stress fracture can also come from a sudden increase in physical activity or a change in your exercise routine. (Left) The four parts of each metatarsal. (Right) fracture in the shaft of the 2nd metatarsal.
- 200. FIFTH METATARSAL FRACTURES • The fifth metatarsal is the long bone on the outside of your foot. Injuries to this bone may be different than fractures of the first four metatarsals. • Most commonly, the fifth metatarsal fractures occur through the base of the bone. This usually cause from an injury where the foot and ankle are twisted downward and inward. • In this type of injury, the tendon that attaches to the base of the fifth metatarsal may stretch and pull a fragment of bone away from the base. Since the fragment is pulled away from the rest of the bone, this type of injury is called an "avulsion fracture." • An avulsion fracture is also sometimes called a "ballerina fracture" or "dancer's fracture" because of the "pointe" position that ballet dancers assume when they are up on their toes. • Another type of fifth metatarsal fracture is a horizontal or transverse fracture through the junction of the base and shaft of the bone. This is sometimes called a "Jones fracture." Since the blood supply to this area is poor, Jones fractures are more prone to difficulties in healing.
- 201. an avulsion fracture at the base of the fifth metatarsal (arrow). (Left) Jones fracture at the base of the fifth metatarsal (arrow). (Right) A screw has been used to hold the bone in place while it heals.
- 202. TREATMENT: FRACTURES OF TOES • NONSURGICAL TREATMENT: • Buddy taping • Wear a wider than normal shoe. • SURGICAL TREATMENT: • manipulate or "reduce" the fracture. This procedure is most often done in the doctor's office. You will be given a local anesthetic to numb your foot, then your doctor will manipulate the fracture back into place and straighten your toe.
- 203. TREATMENT: METATARSAL FRACTURES • NONSURGICAL TREATMENT: • Most metatarsal fractures can be treated with an initial period of elevation and limited weight bearing. This is followed by gradual weight bearing, as tolerated, in a cast or walking boot • SURGICAL TREATMENT: • Surgery is not often required. However, if you have fractured several metatarsals at the same time and your foot is deformed or unstable, surgery is necessary. • Internal Fixation
- 204. TREATMENT: FIFTH METATARSAL FRACTURES • NONSURGICAL TREATMENT: • Most fifth metatarsal fractures can be treated with weight bearing as comfortable in a walking boot. • SURGICAL TREATMENT: • Avulsion Fracture: open reduction and internal fixation (plates and screws). • Jones Fracture: if it become nonunion, surgery is required.
