23204955
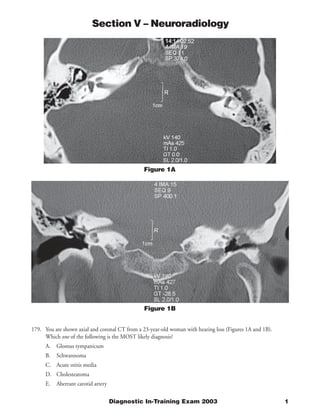
- 1. Section V – Neuroradiology Figure 1A Figure 1B 179. You are shown axial and coronal CT from a 23-year-old woman with hearing loss (Figures 1A and 1B). Which one of the following is the MOST likely diagnosis? A. Glomus tympanicum B. Schwannoma C. Acute otitis media D. Cholesteatoma E. Aberrant carotid artery Diagnostic In-Training Exam 2003 1
- 2. Section V – Neuroradiology Question #179 Findings: A soft tissue mass is present in the left middle ear cavity in Prussak’s space. There is erosion of the scutum apparent on the coronal image. There is demineralization of the ossicles. There is decreased aeration of the left mastoid air cells. Rationales: A) Incorrect. This is a rare type of glomus tumor, which usually presents with pulsatile tinnitus. A glomus tumor is located on the cochlear promontory rather than in Prussak’s space. It may also extend into the jugular foramen; in this case, it is termed glomus jugulotympanicum. B) Incorrect. Facial nerve schwannoma is a rare nerve sheath tumor. It may produce hearing loss if large. It may be seen along the course of the facial nerve between the internal auditory canal and the facial nerve canal. The facial nerve does not pass through Prussak’s space. Schwannomas of the vestibular nerve are common, but occur in the internal auditory canal rather than in the middle ear cavity. C) Incorrect. Findings of acute otitis media include middle ear and mastoid fluid. Middle ear fluid is usually dependent, unlike the opacity in this case. This condition may also produce hearing loss. Acute infection does not produce erosion of the scutum or ossicles. D) Correct. This is the most common middle ear soft tissue mass. The findings are those classically described for cholesteatoma. Acquired cholesteatoma is an inflammatory mass associated with chronic otitis media. It can result in conductive hearing loss by destruction of the ossicles. E) Incorrect. This lesion also may present as pulsatile tinnitus. A tubular soft tissue structure is seen passing adjacent to the cochlea. On adjacent sections, it is continuous with the carotid artery. This lesion may appear similar to a glomus tumor on clinical exam. Magnetic resonance angiography can confirm the diagnosis of aberrant internal carotid artery. 2 American College of Radiology
- 3. Section V – Neuroradiology Figure 2A Figure 2B 180. You are shown two images from a left common carotid artery angiogram (Figures 2A and 2B) from a 68-year- old woman with left eye pain and proptosis. Which one of the following is the MOST likely diagnosis? A. Meningioma B. Cavernous hemangioma C. Carotid artery-cavernous sinus fistula D. Pial arteriovenous malformation E. Venous angioma Diagnostic In-Training Exam 2003 3
- 4. Section V – Neuroradiology Question #180 Findings: Opacification of both cavernous sinuses and both superior ophthalmic veins is seen during the arterial phase of a left carotid artery injection. These findings represent early draining veins; normal veins are not seen during the arterial phase of injection. Flow in the ophthalmic veins is retrograde because this is the arterial phase. Rationales: A) Incorrect. Meningiomas may involve the cavernous sinus. They usually show a dense, persistent tumor stain. Meningiomas in this location may narrow or occlude the internal carotid artery. Although tumors may have mild arteriovenous shunting, this degree of early venous filling is not seen in meningiomas. B) Incorrect. Cavernous hemangioma is the most common intraconal orbital mass in adults. Hemangiomas may show delayed puddling of contrast material on angiography. There are low flow lesions and do not have prominent arteriovenous shunting. C) Correct. These lesions have multiple etiologies. In younger patients, direct fistulas are typically the result of trauma with rupture of the intracavernous internal carotid artery. They may also be caused by rupture of a cavernous carotid aneurysm. In older patients, indirect fistulas may results spontaneously from development of abnormal dural arteriovenous connections. Symptoms include proptosis, diplopia, chemosis, and injection. Cross-sectional imaging findings include enlarged superior ophthalmic veins and extra-ocular muscles, proptosis, and orbital edema. On angiography, there is early filling of the cavernous sinus and ophthalmic veins (usually bilateral). These lesions may be treated endo vascularly by occlusion of the cavernous sinus. D) Incorrect. Arteriovenous malformations demonstrate early draining veins, as seen in this case. However, pial (parenchymal) AVMs have an intra-axial nidus, which contains the abnormal arterial-venous connections. In this case, the fistulous connection is extra-axial, being contained entirely within the cavernous sinus. E) Incorrect. Venous angioma is also known as developmental venous anomaly. This is an anomalous vein draining normal brain parenchyma with a feeding network of smaller vessels known as a caput medusa. The caput medusa is named for its resemblance to the mythical creature with snakes for hair. Unlike the medusa, venous angiomas are typically benign incidental findings. They may be associated with capillary hemangiomas, which may bleed and become symptomatic. Venous angiomas are seen during the venous phase of angiography as an enlarged vein fed by a caput medusa. This may take the shape of an open umbrella. 4 American College of Radiology
- 5. Section V – Neuroradiology Figure 3A 181. You are shown T1-weighted pre-contrast (Figure 3A) and post-contrast (Figure 3B) and T2-weighted MR images (Figure 3C) on a 6-month-old boy with vomiting. Which one of the following is the MOST likely diagnosis? A. Giant cell astrocytoma B. Choroid plexus papilloma C. Meningioma D. Ependymoma E. Teratoma Diagnostic In-Training Exam 2003 5
- 6. Section V – Neuroradiology Figure 3B Figure 3C 6 American College of Radiology
- 7. Section V – Neuroradiology Question #181 Findings: There is a large enhancing mass in the left lateral ventricle. There is moderate hydrocephalus. Flow voids are seen within the lesion on the T2 image. Rationales: A) Incorrect. This is a tumor associated with tuberous sclerosis. It occurs near the foramen of Monro and may produce hydrocephalus. It is generally found in adolescence or early adulthood. Other intracranial findings of T.S. include subependymal nodules and cortical tubers. B) Correct. This is the most common intraventricular tumor in infants. Imaging findings include enlarged choroid plexus in the trigone of the lateral ventricle and hydrocephalus. Enlarged feeding choroidal vessels may be seen as flow voids. Carcinoma of the choroid plexus can also occur and has similar imaging findings, although it is about 10 times less frequent. Choroid plexus papilloma is rare in adults, where it is usually found in the fourth ventricle. C) Incorrect. Meningiomas may occur in the lateral ventricle, although this is very rare. Meningioma is extremely rare in infants and should not be considered as the most likely lesion. When meningiomas are found in children, they are usually associated with a genetic disorder such as neurofibromatosis type 2. D) Incorrect. Ependymoma usually occurs in the fourth ventricle in young children. Supratentorial ependymomas are less common and are usually solid parenchymal masses. Subependymoma is a distinct histologic lesion. It is a benign mass found in the lateral ventricle in older adults. E) Incorrect. Teratomas may present as congenital tumors. They are more common in older children in the pineal region. Only five cases of intraventricular teratoma have been reported in the literature (see reference), making this diagnosis highly unlikely. Teratomas have heterogenous appearance on imaging, often containing lipids or calcium. Citations: Chidambaram B, Yasha TC, Balasubramaniam V. Childs Nerv Syst 2001 Oct; 17(10): 618-22 Diagnostic In-Training Exam 2003 7
- 8. Section V – Neuroradiology Figure 4 182. You are shown a non-contrast axial CT image (Figure 4) from a 50-year-old man who is unresponsive in the emergency department. Which one of the following is the MOST likely diagnosis? A. Subarachnoid hemorrhage B. Epidural hematoma C. Cerebral infarction D. Meningioma E. Subdural hematoma 8 American College of Radiology
- 9. Section V – Neuroradiology Question #182 Findings: There is a crescentic fluid collection overlying the left cerebral convexity. It is isodense to the brain. The fluid collection lies between the cerebral cortex and the skull. It is producing mass effect on the left hemisphere. Rationales: A) Incorrect. Subarachnoid hemorrhage is seen as increased attenuation within the sulci. It is frequently associated with hydrocephalus due to obstruction of CSF flow by clot. The most common causes are trauma and aneurysmal rupture. The fluid collection in this case displaces brain rather than lying within the sulci. B) Incorrect. Epidural hematomas are the result of trauma. They present as a lens-shaped fluid collection with a convex inner border, rather than the concave inner border seen here. Acute epidural hematomas usually are high in attenuation. This finding requires emergent neurosurgical consultation, as rapid arterial bleeding can result in brain herniation and death. Bleeding from a lacerated middle meningeal artery is the most common cause. This hematoma is usually associated with a skull fracture overlying the hematoma. Epidural hematomas from venous hemorrhage are less common. C) Incorrect. Cerebral infarction shows decreased attenuation of gray and white matter on unenhanced CT. Severe mass effect can develop within several days of a large hemispheric infarction and may cause brain herniation and death. The fluid collection in this case is extra-axial and does not represent infarction. D) Incorrect. Meningiomas are extra-axial masses, which may be isodense to brain on non-contrast CT. However, they are commonly increased in density due to the presence of calcifications. They are usually focal rounded masses rather than the crescentic lesion seen here. En plaque meningiomas can have a crescentic morphology but are usually found adjacent to the sphenoid bone rather than in the frontal or parietal bones as in this case. E) Correct. This subdural hematoma is isodense to brain. Acute subdural hemorrhage is usually increased in attenuation. Most subacute (7-28 days) subdural hematomas are isodense to brain, with chronic subdurals being low in attenuation. Careful attention to the location of cortex between the fluid collection and brain is required to make this diagnosis. Contrast administration may be helpful in difficult cases by demonstrating enhancing vessels between the brain and the subdural fluid collection. Citations: Lee, KS, et al, J Korean Med Sci 12:353 (1997); Scotti, et al, J Neurosurgery 47:311 (1977) Diagnostic In-Training Exam 2003 9
- 10. Section V – Neuroradiology Figure 5A Figure 5B Figure 5C 183. You are shown T1-weighted pre-contrast (Figure 5A) and post-contrast (Figure 5B) and T2-weighted MR images (Figure 5C) from a 79-year-old man with back pain. Which one of the following is the MOST likely diagnosis? A. Osteomyelitis B. Schmorl’s node C. Multiple myeloma D. Chance fracture E. Hemangioma 10 American College of Radiology
- 11. Section V – Neuroradiology Question #183 Findings: There is a compression fracture of the L2 vertebral body. The marrow signal is diffusely abnormal. There is mottled decreased T1 and increased T2 signal throughout the spine including posterior elements. The areas of decreased T1 signal show contrast enhancement. Rationales: A) Incorrect. Vertebral osteomyelitis is most common in the lumbar spine. It can result in back pain and compression fractures. However, it should not produce diffusely abnormal marrow. Involvement of adjacent disk spaces and paraspinal masses are frequent associated findings. B) Incorrect. Schmorl’s nodes represent herniations of the intervertebral disk through the endplate. They are common findings, but are usually asymptomatic. Schmorl’s nodes do not usually produce significant loss of vertebral height. The loss of height and diffusely abnormal marrow signal in this case point towards an alternative diagnosis. C) Correct. The diffuse marrow abnormality suggests an infiltrative process. The most common diffuse marrow diseases in older adults include multiple myeloma and metastatic disease. Prostate or breast carcinoma can produce diffuse marrow disease in advanced cases. Fractures in the setting of widespread marrow abnormality should be considered pathologic fractures. D) Incorrect. Chance fracture is a traumatic injury associated with lap safety belt use in motor vehicle collisions. It is a transverse fracture, which usually occurs at L1. It may involve the posterior elements and result in vertebral malalignment. The abnormal marrow signal in this case suggests a pathologic fracture rather than trauma. E) Incorrect. Hemangioma is a common lesion in the vertebral body. It usually has increased T1 and T2 signal. It is seen as a rounded lesion within the vertebral body. Coarsening of trabecular pattern is seen on plain films or CT. It is rarely associated with compression fractures. Although hemangiomas may be multiple, they do not diffusely involve the marrow as in this case. Diagnostic In-Training Exam 2003 11
