More Related Content
Similar to Anita Charlesworth: The Funding Outlook for Health Care (20)
More from Nuffield Trust (20)
Anita Charlesworth: The Funding Outlook for Health Care
- 1. The Funding Outlook for Health
Anita Charlesworth
Chief Economist
March 2013
Twitter: #NTSummit
© Nuffield Trust
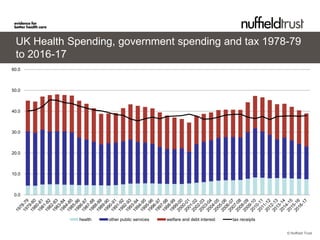
- 2. UK Health Spending, government spending and tax 1978-79
to 2016-17
60.0
50.0
40.0
30.0
20.0
10.0
0.0
health other public services welfare and debt interest tax receipts
© Nuffield Trust
- 3. The magic circle: health spending increases rapidly, overall
public spending and tax falls
Share of Total Public Health Other public Welfare and Receipts
GDP Spending spending services debt
interest
1978-79 45.1% 4.4% 25.9% 14.7% 40.1%
2007-08 40.7% 7.1% 20.3% 13.2% 38.6%
Difference - 4.4 +2.7 -5.6 -1.5 -1.5
Source: OBR, HMT PESA 2012
In 2016-17 spending as a share of GDP and receipts as a share of GDP will
be at the average for the 20 years pre-crisis (40% and 38%).
2 key differences: Health spending will be much larger (2 percentage
points of GDP) and spending on other public services will be at the share
last seen in at the end of 1990’s.
© Nuffield Trust
- 5. Closing £13 billion Funding Gap: 2010/11 to 2014/15
£105 Funding pressures on the NHS in England
Funding pressures after for pay restaint
Funding pressures after pay restraint and
managing hospital activity for chronic conditions
Funding (£billion in 2010/11 prices)
£100
Funding pressures after pay restraint, managing Pay
hospital activity for chronic conditions, and
productivity savings reduction:
Funding allocation based on 2010 spending review £5bn
£95 Disease
management:
£3bn
Acute QIPP
Actions: £4bn
£90
£85
2010/11 2011/12 2012/13 2013/14 2014/15
Year
© Nuffield Trust
- 6. Initial Progress in 2011-12?
Expected Actual Difference
Emergency Admissions trend 5,784,376 5,411,015 -7%
Emergency Admissions with QIPP actions 5,648,234 5,411,015 -4%
Emergency Bed Days trend 39,639,520 35,600,921 -11%
Emergency Bed Days with QIPP actions 37,352,528 35,600,921 -5%
Planned Admissions trend 8,766,957 8,735,584 0%
Modelled Planned Bed Days 16,747,173 16,555,415 -1%
Planned Bed Days with QIPP actions 16,159,549 16,555,415 2%
OP Appointments 67,079,975 72,799,662 8%
OP Appointments with QIPP actions 62,572,388 72,799,662 14%
A&E Attendances trend 15,503,662 17,602,055 12%
© Nuffield Trust
- 7. Variation in labour productivity at selected providers in
England: 2006/07 to 2011/12
© Nuffield Trust
- 9. Closing £11 billion Funding Gap: 2014/15 to 2017/18
£105
Funding pressures after pay restraint, managing hospital
activity for chronic conditions, and productivity savings
Funding pressure after releasing all semi-fixed costs
from QIPP
Funding (£billion in 2010/11 prices)
£100 Funding pressures after releasing all semi-fixed costs Releasing semi-fixed
from QIPP, and management of activity for chronic costs: £2bn
conditions
Funding pressures after releasing all semi-fixed costs Disease Management:
from QIPP, management of activity for chronic
conditions, and extension of pay restraint
£2bn
Flat Real
£95 Continued Pay
Restraint: £3bn
Remaining Gap:
£3bn
£90
£85
2014/15 2015/16 2016/17 2017/18
Year
© Nuffield Trust
- 10. Earnings will be key
2011 2012 2013 2014 2015 2016 2017
Nominal 2.2 2.7 2.2 2.8 3.7 4.0 4.0
average
earnings
growth
GDP 2.7 2.3 2.0 2.0 2.0 2.0 2.0
deflator
Nominal 1.7 1.7 2.5 2.5 ? ? ?
NHS pay bill
per head
growth
Source: OBR 2012, NHS employers 2012 © Nuffield Trust
- 11. Conclusions
• From 2010/11 to 2014/15 the NHS faces its tightest budget of last 50
years.
• This period of austerity is likely to extend at least until 2017-18.
• Only a even larger cut in other public services or welfare or relatively
large tax increases would allow NHS funding to grow at historic levels.
1p extra on income tax raises around £4 billion a year.
• Without unprecedented productivity gains, there is likely to be a rapid
growth in the gap between the demand for care and the ability to
provide high-quality services.
• Although the NHS is delivering headline savings its not clear that it is
making the necessary progress on service productivity and models of
care.
• The scale of workforce cost growth after 2015 will be crucial.
© Nuffield Trust