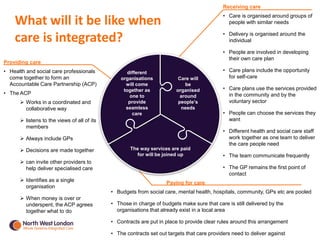
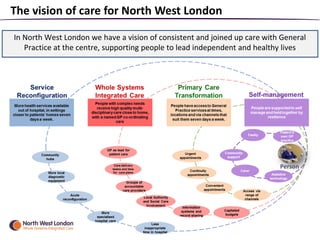
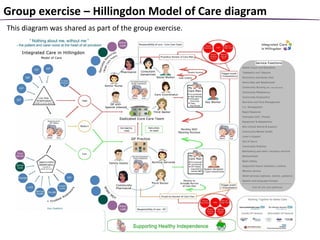
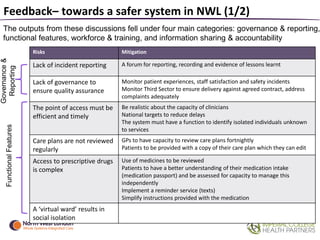
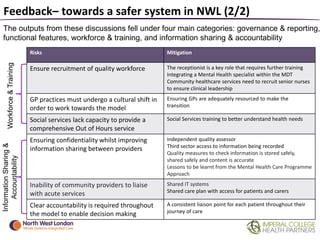
The document summarizes a patient safety workshop that introduced the Whole Systems Integrated Care (WSIC) programme and Imperial College Health Partners (ICHP) patient safety initiatives in North West London. The workshop aimed to gather feedback on how patients can get more involved in improving safety. It covered the vision for integrated care in NWL and patient stories. Group exercises discussed risks to a safer system and how patients and professionals can work together on safety. The Patient Safety Champion Network was introduced to promote patient engagement in safety work across NWL.