ULCERATIVE COLITIS.pptx
- 2. Agenda 01 INTRODUCTION 02 RISK FACTORS 03 ETIOLOGY 04 TYPES 05 COMPLICATIONS 06 SYMPTOMS 2
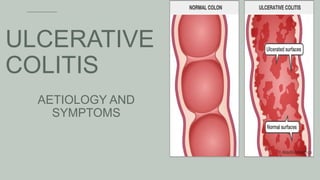
- 3. 01INTRODUCTIO N • Ulcerative colitis is an inflammatory bowel disease (IBD), characterized by the inflammation and ulcerative aberrations in the wall of the large intestine. It is also known as “colitis or proctitis”. • Ulcerative colitis can be debilitating and can sometimes lead to life-threatening complications. While it has no known cure, treatment can greatly reduce signs and symptoms of the disease and bring about long-term remission. • Rectum and lower part of the colon are commonly affected. Sometimes, the entire colon is affected. 3
- 4. Age Ulcerative colitis usually affects people in the age group of 15 to 30 years. But it can occur at any age, and some people may not develop the disease until after age 60. Race or Ethnicity Although whites have the highest risk of the disease, it can occur in any race. If you're of Ashkenazi Jewish descent, your risk is even higher. Family history. • You're at higher risk if you have a close relative, such as a parent, sibling or child, with the disease. 4 RISK FACTORS
- 5. 03 5 ETIOLOG Y Exact cause for ulcerative colitis is not known. Factors that may play a role in who develops UC include: 1. Genes: Genes may play a role; the disease sometimes runs in families. Researchers have found some genes that are potentially associated with the condition, and between 15 and 20 percent of people with Crohn’s have a relative with Ulcerative colitis. 2. Immune system: Ulcerative colitis happens when your immune system makes a mistake. White blood cells that usually protect you attack the lining of your colon instead. They cause the inflammation and ulcers. In inflammatory bowel diseases (ulcerative colitis and Crohn's disease), the immune response is triggered inappropriately by the normal contents of the gut. One experimental therapy for these diseases that seems to be successful is to block the action of cytokines released by the gut-associated lymphoid tissues 3. Other immune disorders. If a person has one type of immune disorder, his/her chance for developing a second is higher. 4. Environmental factors. Bacteria, viruses, and antigens may also trigger the Immune system.
- 6. 04 TYPES Doctors often classify ulcerative colitis according to its location. Types of ulcerative colitis include: Ulcerative proctitis. Inflammation is confined to the area closest to the anus (rectum), and rectal bleeding may be the only sign of the disease. Proctosigmoiditis. Inflammation involves the rectum and sigmoid colon — the lower end of the colon. Signs and symptoms include bloody diarrhoea, abdominal cramps and pain, and an inability to move the bowels in spite of the urge to do so (tenesmus). Left-sided colitis. Inflammation extends from the rectum up through the sigmoid and descending colon. Signs and symptoms include bloody diarrhoea, abdominal cramping and pain on the left side, and urgency to defecate. Pancolitis. This type often affects the entire colon and causes bouts of bloody diarrhoea that may be severe, abdominal cramps and pain, fatigue, and significant weight loss.
- 7. 1.Osteoporosis: People with ulcerative colitis are at an increased risk of developing osteoporosis, when the bones become weak and are more likely to fracture. 2. Primary sclerosing cholangitis: Primary sclerosing cholangitis (PSC), where the bile ducts become progressively inflamed and damaged over time, is a rare complication of ulcerative colitis. Bile ducts are small tubes used to transport bile (digestive juice) out of the liver and into the digestive system. 3.Toxic megacolon: Toxic megacolon is a rare and serious complication of severe ulcerative colitis where inflammation in the colon causes gas to become trapped, resulting in the colon becoming enlarged and swollen. This is potentially very dangerous as it can cause the colon to rupture (split) and cause infection in the blood (septicaemia). 4. Bowel cancer: People who have ulcerative colitis have an increased risk of developing bowel cancer (cancer of the colon, rectum or bowel), especially if the condition is severe or involves most of the colon. The longer a person have ulcerative colitis, the greater the risk. People with ulcerative colitis are often unaware they have bowel cancer as the initial symptoms of this type of cancer are similar. 7 COMPLICATIONS
- 8. SYMPTOMS AND CLINICAL FINDINGS • This disease is predominantly found in young adults. Initially, it may present itself as a need to defecate several times a day or diarrhoea with rectal bleeding. • Severe loss of water, electrolytes and bleeding cause weight loss, dehydration, fever, weakness, and anaemia. • If necrosis of the tissue is localized without any external symptoms, the case may be severe and remedy must be given immediately. 8
- 9. Symptoms: 1. Abdominal pain or cramps 2. Diarrhoea with blood in the stools 3. Early fatigue, weight loss and malnutrition 7. Liver diseases like hepatitis, cirrhosis, etc. 8. Skin rashes 9. Anaemia. 10. Increased stomach sounds 4. Loss of appetite, nausea and weight loss 5. Arthritis and osteoporosis characterized by joint pains and swelling 6. Eye inflammation 11. Fever 12. Rectal pain 13. Mouth sores 9
- 10. BIBLIOGRAPH Y 1. NUTRITION AND DIETETICS (With Indian Case Studies) Fourth Edition - Shubhangini A Joshi. 2. DIETETICS – Eighth Edition – B. Srilakshmi 3. Essentials of Medical Physiology - Sixth Edition - K Sembulingam Ph.D 4. Human Physiology_ An Integrated Approach-Prentice Hall College Division (2000) - Dee Unglaub Silverthorn, Andrew C. Silverthorn, Ober, William C, Claire W. Garrison. 5. https://www.webmd.com/ibd-crohns-disease/ulcerative-colitis/what-is-ulcerative-colitis 6. https://www.healthline.com/health/ulcerative-colitis 7.https://my.clevelandclinic.org/health/diseases/10351-ulcerative-colitis 8. https://www.nhs.uk/conditions/ulcerative-colitis/complications/ 10
Editor's Notes
- Line spacing + Page numbers