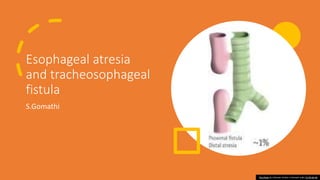
Tracheoesophageal fistula
- 1. Esophageal atresia and tracheosophageal fistula S.Gomathi This Photo by Unknown Author is licensed under CC BY-SA-NC
- 2. Esophageal atresia failure of the esophagus to form a continuous passage from the pharynx to the stomach during embryonic development. EA can occur with tracheoesophageal fistula (TEF), which is an abnormal connection between the trachea and esophagus.
- 3. incidence • EA/TEF occurs in approximately 1 in 3,500 births
- 4. Associations: • a. Down syndrome. • b. VACTERL syndrome (vertebral defects, anal atresia, cardiac anomaly, TEF fistula with EA, renal defects, and radial limb dysplasia).
- 5. Etiology • 1. Cause is unknown in most cases and likely multifactorial. • a. inheritable genetic factor • b. Six to 10% due to chromosomal (structural) abnormalities, including trisomies (12, 18, 21), and partial deletions such as 13q13-qter, 22q11.2. • c. Teratogenic stimuli, such as the anticancer drug adriamycin and diethylstilbestrol (DES).
- 7. pathophysiology Failure of proper separation of the embryonic channel into the esophagus and trachea during the 4th and 5th weeks of gestation.
- 8. classification • Esophageal atresia can be classified as • a. Type I (Type A): proximal and distal segments of esophagus are blind; there is no connection to trachea; accounts for approximately 7% of cases; second most common. • b. Type II (Type B): proximal segment of esophagus opens into trachea by a fistula; distal segment is blind; rare, 0.8% of cases.
- 9. • c. Type III (Type C): proximal segment of esophagus has blind end; distal segment of esophagus connects into trachea by a fistula; most common, with 86% of cases. (Discussion is limited to this type.) • d. Type IV (Type D): esophageal atresia with fistula between proximal and distal ends of trachea and esophagus (rare, 0.7% of cases). • e. Type V (Type E): proximal and distal segments of esophagus open into trachea by a fistula; no esophageal atresia but sometimes referred to as an H- type fistula; occurs in 4.2% of cases; not usually diagnosed at birth.
- 10. Clinical Manifestations These appear soon after birth. 1. Excessive secretions. a. Constant drooling. b. Large amount of secretions from nose. c. Saliva or formula accumulates in upper esophageal pouch and is aspirated into airway.
- 11. 2. Intermittent, unexplained cyanosis and laryngospasm • a. Caused by aspiration of accumulated saliva in blind pouch. • b. Gastric acid is regurgitated through distal fistula.
- 12. 3. Abdominal distention. • a. Occurs as a result of air entering the lower esophagus through the fistula and passing into the stomach, especially when the child is crying.
- 13. 4. Violent response after first or second swallow of feeding • a. Infant coughs and chokes. • b. Fluid returns through nose and mouth. • c. Cyanosis occurs. • d. Infant struggles.
- 14. • 5. Poor feeding. • 6. Inability to pass catheter through nose or mouth into stomach; tip of catheter stops at blind pouch, or atresia.
- 15. Diagnostic Evaluation • 1. Ultrasound scanning techniques enable TEF to be identified in utero for some infants. • 2. Failure to pass a 10F catheter (smaller catheters may coil) into the stomach through nose or mouth. Catheter is left in situ while an x-ray confirms the diagnosis. • 3. pH of tracheal secretions is acidic. • 4. Flat-plate x-ray of abdomen and chest may reveal presence of gas in stomach and catheter coiled in the blind pouch. Barium x-ray may be used in some cases. • 5. Electrocardiogram and echocardiogram are performed because there is a high association with cardiac anomalies.
- 16. Management Immediate Treatment 1. Propping infant at 30-degree angle, supine or side- lying, to prevent reflux of gastric contents. 2. Nasogastric (NG) tube remains in the esophagus and is aspirated frequently to prevent aspiration until continuous low suction is applied. 3. Pouch is washed out with normal saline to prevent thick mucus from blocking the tube. 4. Gastrostomy to decompress stomach and prevent aspiration; later used for feedings.
- 17. • 5. Nothing by mouth (NPO); IV fluids. • 6. Comorbidities, such as pneumonitis and heart failure, are treated. • 7. Supportive therapy includes meeting nutritional requirements, IV fluids, antibiotics, respiratory support, and maintaining thermally neutral environment.
- 18. Surgery • 1. Prompt primary repair: fistula found by bronchoscopy is divided, followed by esophageal anastomosis of proximal and distal segments if infant weight permits and is without pneumonia.
- 19. 2. Short-term delay: • subsequent primary repair is used to stabilize infant and prevent deterioration when the patient’s condition contraindicates immediate surgery.
- 20. 3. Staging: • initially, fistula division and gastrostomy are performed with later secondary esophageal anastomosis or colonic transposition performed approximately 1 year later to effect total repair. • Approach may be used with a very small, premature infant or a very sick neonate or when severe congenital anomalies exist.
- 21. 4. Circular esophagomyotomy performed on proximal pouch to gain length and allow for primary anastomosis at initial surgery.
- 22. • 5. Cervical esophagostomy: when ends of esophagus are too widely separated, esophageal replacement with segment of intestine (colonic transposition) is done at ages 18 to 24 months. • 6. Fiberoptic tracheoscopy-assisted repair of tracheoesophageal fistula can expedite and facilitate surgery on ventilated patients. • 7. Staged repair resulted in least amount of GI dysmotility postoperatively
- 23. Nursing Diagnoses Preoperative • Risk for Aspiration related to structural abnormality. • Risk for Deficient Fluid Volume related to inability to take oral fluids. • Anxiety of parents related to critical situation of neonate.
- 24. Postoperative • Ineffective Airway Clearance related to surgical intervention. • Ineffective Infant Feeding Pattern related to defect. • Acute Pain related to surgical procedure. • Impaired Tissue Integrity related to postoperative drainage. • Risk for Injury related to complex surgery. • Risk for Impaired Attachment related to prolonged hospitalization.
- 25. Nursing Interventions • Preventing Aspiration 1. Position the infant supine with head and chest elevated 20 to 30 degrees to prevent or decrease reflux of gastric juices into the tracheobronchial tree. a. This position may also ease respiratory effort by dropping the distended intestines away from the diaphragm. b. Side-lying position can be used if the risk of aspiration from being supine is greater than the risk of sudden infant death syndrome (SIDS); supine positioning is preferred to reduce the risk of SIDS. c. Turn frequently to prevent atelectasis and pneumonia.
- 26. • 2. Perform intermittent nasopharyngeal suctioning or maintain indwelling Sump tube with constant suction to remove secretions from esophageal blind pouch. • a. Tip of tube is placed in the blind pouch. • b. Sump tube allows air to be drawn in through a second lumen and prevents tube obstruction by mucous membrane of pouch. • c. Maintain indwelling tube patency by irrigating with 1 mL normal saline solution frequently
- 27. • 3. Place the infant in an Isolette or under a radiant warmer with high humidity to aid in liquefying secretions and thick mucus. Maintain the infant’s temperature in thermoneutral zone and ensure environmental isolation to prevent infection by using Isolette. • 4. Administer oxygen, as needed. • 5. Suction mouth to keep it clear of secretions and prevent aspiration. Provide mouth care. • 6. Be alert for indications of respiratory distress. a. Retractions. b. Circumoral cyanosis. c. Restlessness. d. Nasal flaring. e. Increased respiration and heart rate.
- 28. • 7. Maintain NPO status. • 8. Administer antibiotics, as ordered, to prevent or treat associated pneumonitis.
- 29. Observe Observe infant carefully for any change in condition; report changes immediately. Check Check vital signs, color and amount of secretions, abdominal distention, and respiratory distress. Evaluate Evaluate for complications that can occur in any neonate or premature infant.
- 30. 10. Be available and recognize need for emergency care or resuscitation. a. Have resuscitation equipment on hand. b. Accompany the infant to other departments and the operating room in Isolette with portable oxygen and suction equipment. 11. Monitor for signs or symptoms that may indicate additional congenital anomalies or complications. 12. Gastrostomy tube (GT) may be placed before definitive surgery to aid in gastric decompression, prevention of reflux, or nutrition.
- 31. Preventing Dehydration • 1. Administer parenteral fluids and electrolytes as prescribed. • 2. Monitor vital signs frequently for changes in blood pressure (BP) and pulse, which may indicate dehydration or fluid volume overload. 3. Record intake and output, including gastric drainage (if GT for decompression is present) and weight of diapers.
- 32. Reducing Parental Anxiety Explain procedures and necessary events to parents as soon as possible. Explain Orient parents to hospital and intensive care nursery environment. 3. Allow family to hold and assist in caring for infant. Orient Offer reassurance and encouragement to family frequently. Offer Provide for additional support by social worker, clergy, and counselor, as needed. Provide
- 33. Concept map on EA& TEF
- 34. Thank you
