OCD
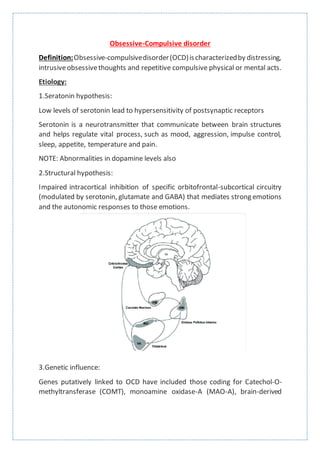
- 1. Obsessive-Compulsive disorder Definition:Obsessive-compulsivedisorder(OCD)ischaracterizedby distressing, intrusiveobsessivethoughts and repetitive compulsive physical or mental acts. Etiology: 1.Seratonin hypothesis: Low levels of serotonin lead to hypersensitivity of postsynaptic receptors Serotonin is a neurotransmitter that communicate between brain structures and helps regulate vital process, such as mood, aggression, impulse control, sleep, appetite, temperature and pain. NOTE: Abnormalities in dopamine levels also 2.Structural hypothesis: Impaired intracortical inhibition of specific orbitofrontal-subcortical circuitry (modulated by serotonin, glutamate and GABA) that mediates strong emotions and the autonomic responses to those emotions. 3.Genetic influence: Genes putatively linked to OCD have included those coding for Catechol-O- methyltransferase (COMT), monoamine oxidase-A (MAO-A), brain-derived
- 2. neurotrophicfactor (BDNF),myelin oligodendrocyteglycoprotein(MOG),GABA- type B-receptor 1, and the mu opioid receptor. 4.Infections: In responseto streptococcal infection, antibodies are produced and antibodies produce inflammation of the basal ganglia. This leads to increased volumes of the caudate, putamen, and the globus pallidus 5. Brain trauma, stimulant abuse, and carbon monoxide poisoning Pathophysiology/ signs and symptoms: Diagnosis: Once OCD is suspected, the following should be performed: 1. Define the rangeand severity of OCD symptoms; the Yale-Brown ObsessiveCompulsiveScale(Y-BOCS)is a good tool for this purpose 2. Complete Mental Status Examination; look for comorbid symptoms and disorders
- 3. Treatment: Goals: -To reduce frequency and severity of obsessivethoughts and time spent performing compulsiveacts -Efforts should be made to minimize adverse drug events and prevent drug interactions. General approach to treatment: Firstline treatment: -Cognition behaviour therapy alone for 13-20 sessions -SSRIs alone for 8-12 wk -CBT+SSRIs if, inadequate response occurs Second line treatment: -Switch to another SSRIs or Clomipramine -Augmentation with antipsychotics if, inadequate responseoccurs Third line treatment: -Augmentation of SSRIs with Clomipramine - Switch to another antipsychotic augmenting agent Nonpharmacological therapy: 1. Transcranialmagnetic stimulation (TMS), 2. Deep brain stimulation (DBS), 3. Ablative neurosurgery Pharmacological therapy: DRUG Initial dose Maximum dose SSRIs Fluoxetin 20mg/day 80mg/day Paroxetine 20 60 Fluvoxamine 50 300 Citalopram 20 80 Escitalopram 10 40 Sertraline 50 200
- 4. TCAs Clomipramine 25 250 1. Tricyclic Antidepressants: MOA: Depression is associated with low levels of NA and 5-HT. Physiologically largeamountsof theseneurotransmittersliberated atthe nerveterminals are reabsorbed into storage sites making them less available for transmission. TCAs inhibit the reuptake of monoamines into their respective neurons. This causes an increase in monoamine concentration in the synaptic cleft in the CNS and periphery leading to their enhanced neuro transmission. Thus inhibition of this 5-HT and NA reuptake produces antidepressant effects. They also block alpha-adrenergic, H1 and Muscarinic receptors leading to ADRs. ADRs: Antimuscarinic effects- Blurred vision, constipation, dry mouth and urinary retention CNS- Sedation, confusion and seizures CVS- Postural hypotension, tachycardia and arrhythmias Also Jaundice, weight gain, tremors and skin rash Contraindication: In epilepsy, narrow angle glaucoma and patients on MAO inhibitors 2. Selective serotonin reuptake inhibitors: MOA: SSRIs selectively inhibits the neuronal uptake of serotonin, thereby potentiates the action of serotonin by making it more available for transmission.
- 5. ADRs: Common symptoms- Nausea, vomiting, diarrhoea, headache, anorexia, insomnia, impaired ejaculation Withdrawal symptoms- anxiety, agitation, paraesthesia, sleep disturbances, irritability Serotonin syndrome- Autonomic- nausea, salivation, diaphoresis, diarrhoea, hyperthermia Cognitive- agitation, anxiety, mania, insomnia Neuromuscular- twitching, rigidity, shivering Contraindications: Patients on MAO inhibitors,