Nrgastro.2012.116
•
1 like•83 views
Scientists used novel high-resolution electrode arrays to accurately map abnormal patterns of gastric electrical activity in patients with gastroparesis. They identified two categories of dysrhythmias - abnormal initiation involving focal or ectopic pacemaking, and abnormal conduction with reduced velocities or blocks. Over 70% of patients showed dysrhythmias despite normal slow-wave frequencies. The findings provide the first detailed classification of gastric dysrhythmias and improve understanding of gastroparesis pathophysiology.
Report
Share
Report
Share
Download to read offline
Recommended
A neglected topic for way too long, the interest in fluid therapy seems to be quickly rising as the medical community is making a shift from looking at fluids as a mere method of stabilization towards the appreciation of its relevant side effects.
Many questions remain to be answered indeed:
Is the upgrade from saline 0.9% to balanced crystalloids worth the extra cost?
Does HES still have a place in the OR?
Do we have to fill the gap left by HES on ICU with crystalloids, other colloids or even albumin?
Is it really impossible to avoid fluid overload by using only crystalloids?
Is there still a definitive place for human albumin?
How do we treat and monitor specific patient populations, like patients with trauma, liver failure, brain edema and right heart failure among others?
How do we avoid a one-size-fits-all regimen in perioperative goal-directed therapy?
What with the fluids beyond resuscitation?
And what do the authors of the big fluid trials do in real life themselves?
The 9th International Fluid Academy Day will again be a 1 day concise meeting on all aspects of fluid managament and hemodynamic monitoring in the critically ill.
Date: October 26th 2019, 8:00 - 18:00
4. #ifad2019 what happened in meantime literature on fluid physiology (cair...

4. #ifad2019 what happened in meantime literature on fluid physiology (cair...International Fluid Academy
Recommended
A neglected topic for way too long, the interest in fluid therapy seems to be quickly rising as the medical community is making a shift from looking at fluids as a mere method of stabilization towards the appreciation of its relevant side effects.
Many questions remain to be answered indeed:
Is the upgrade from saline 0.9% to balanced crystalloids worth the extra cost?
Does HES still have a place in the OR?
Do we have to fill the gap left by HES on ICU with crystalloids, other colloids or even albumin?
Is it really impossible to avoid fluid overload by using only crystalloids?
Is there still a definitive place for human albumin?
How do we treat and monitor specific patient populations, like patients with trauma, liver failure, brain edema and right heart failure among others?
How do we avoid a one-size-fits-all regimen in perioperative goal-directed therapy?
What with the fluids beyond resuscitation?
And what do the authors of the big fluid trials do in real life themselves?
The 9th International Fluid Academy Day will again be a 1 day concise meeting on all aspects of fluid managament and hemodynamic monitoring in the critically ill.
Date: October 26th 2019, 8:00 - 18:00
4. #ifad2019 what happened in meantime literature on fluid physiology (cair...

4. #ifad2019 what happened in meantime literature on fluid physiology (cair...International Fluid Academy
More Related Content
What's hot
What's hot (20)
7. #ifad2019 how to assess volemic status (langer)

7. #ifad2019 how to assess volemic status (langer)
Autopsy standards for fetal lengths and organ weights

Autopsy standards for fetal lengths and organ weights
8. #ifad2019 review of recent monitoring trials (edwards)

8. #ifad2019 review of recent monitoring trials (edwards)
19. #ifad2019 triggering celular oxygenation (carmona)

19. #ifad2019 triggering celular oxygenation (carmona)
9. #ifad2019 review of recent fluid trials (funcke)

9. #ifad2019 review of recent fluid trials (funcke)
Anticoagulation in pediatric ventricular assist device - WCPCCS 2017

Anticoagulation in pediatric ventricular assist device - WCPCCS 2017
Similar to Nrgastro.2012.116
Similar to Nrgastro.2012.116 (20)
Improving early detection of gastric cancer a novel systematic alphanumeric c...

Improving early detection of gastric cancer a novel systematic alphanumeric c...
Eletro Stimulation of Lower Esophageal Sphincter on GERD treatment 

Eletro Stimulation of Lower Esophageal Sphincter on GERD treatment
A study on clinical and prognostic significance of gamma glutamyl transferase...

A study on clinical and prognostic significance of gamma glutamyl transferase...
Electrogastrogram based digestion detection system for coma patients

Electrogastrogram based digestion detection system for coma patients
Methods For Improving The Cellular Uptake Of Dna Origami...

Methods For Improving The Cellular Uptake Of Dna Origami...
Sacral Neuromodulation in Children with Neurogenic Bladder Dysfunction

Sacral Neuromodulation in Children with Neurogenic Bladder Dysfunction
A genomic approach to idiopathic liver disease in adults

A genomic approach to idiopathic liver disease in adults
A Paradigm Shift in the Utilization of Therapeutic Plasmapheresis in Clinical...

A Paradigm Shift in the Utilization of Therapeutic Plasmapheresis in Clinical...
A Paradigm Shift in the Utilization of Therapeutic Plasmapheresis in Clinical...

A Paradigm Shift in the Utilization of Therapeutic Plasmapheresis in Clinical...
IRIDOLOGY RESEARCH BY GAEL RIVERZ N.D., IRIDOLOGIST

IRIDOLOGY RESEARCH BY GAEL RIVERZ N.D., IRIDOLOGIST
ROLE OF ECHOGRAPHY AND COMPUTED TOMOGRAPHY IN DIAGNOSIS OF CHRONIC DIFFUSE LI...

ROLE OF ECHOGRAPHY AND COMPUTED TOMOGRAPHY IN DIAGNOSIS OF CHRONIC DIFFUSE LI...
More from Elsa von Licy
More from Elsa von Licy (20)
Styles of Scientific Reasoning, Scientific Practices and Argument in Science ...

Styles of Scientific Reasoning, Scientific Practices and Argument in Science ...
Strategie Decisions Incertitude Actes conference fnege xerfi

Strategie Decisions Incertitude Actes conference fnege xerfi
Bioph pharm 1an-viscosit-des_liquides_et_des_solutions

Bioph pharm 1an-viscosit-des_liquides_et_des_solutions
Nrgastro.2012.116
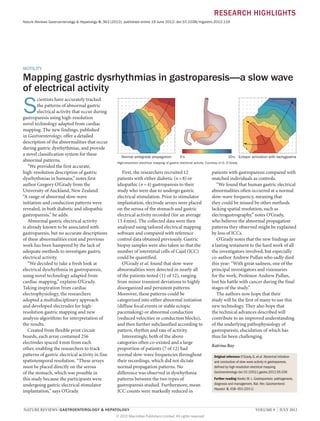
- 1. NATURE REVIEWS | GASTROENTEROLOGY & HEPATOLOGY VOLUME 9 | JULY 2012 Nature Reviews Gastroenterology & Hepatology 9, 363 (2012); published online 19 June 2012; doi:10.1038/nrgastro.2012.116 RESEARCH HIGHLIGHTS S cientists have accurately tracked the patterns of abnormal gastric electrical activity that occur during gastroparesis using high-resolution novel technology adapted from cardiac mapping. The new findings, published in Gastroenterology, offer a detailed description of the abnormalities that occur during gastric dysrhythmias, and provide a novel classification system for these abnormal patterns. “We provided the first accurate, high-resolution description of gastric dysrhythmias in humans,” notes first author Gregory O’Grady from the University of Auckland, New Zealand. “A range of abnormal slow-wave initiation and conduction patterns were revealed, in both diabetic and idiopathic gastroparesis,” he adds. Abnormal gastric electrical activity is already known to be associated with gastroparesis, but no accurate descriptions of these abnormalities exist and previous work has been hampered by the lack of adequate methods to investigate gastric electrical activity. “We decided to take a fresh look at electrical dysrhythmia in gastroparesis, using novel technology adapted from cardiac mapping,” explains O’Grady. Taking inspiration from cardiac electrophysiology, the researchers adopted a multidisciplinary approach and developed electrodes for high- resolution gastric mapping and new analysis algorithms for interpretation of the results. Created from flexible print circuit boards, each array contained 256 electrodes spaced 4 mm from each other, enabling the researchers to track patterns of gastric electrical activity in fine spatiotemporal resolution. “These arrays must be placed directly on the serosa of the stomach, which was possible in this study because the participants were undergoing gastric electrical stimulator implantation,” says O’Grady. MOTILITY Mapping gastric dysrhythmias in gastroparesis—a slow wave of electrical activity First, the researchers recruited 12 patients with either diabetic (n = 8) or idiopathic (n = 4) gastroparesis to their study who were due to undergo gastric electrical stimulation. Prior to stimulator implantation, electrode arrays were placed on the serosa of the stomach and gastric electrical activity recorded (for an average 13.4 min). The collected data were then analysed using tailored electrical mapping software and compared with reference control data obtained previously. Gastric biopsy samples were also taken so that the number of interstitial cells of Cajal (ICC) could be quantified. O’Grady et al. found that slow-wave abnormalities were detected in nearly all of the patients tested (11 of 12), ranging from minor transient deviations to highly disorganized and persistent patterns. Moreover, these patterns could be categorized into either abnormal initiation (diffuse focal events or stable ectopic pacemaking) or abnormal conduction (reduced velocities or conduction blocks), and then further subclassified according to pattern, rhythm and rate of activity. Interestingly, both of the above categories often co-existed and a large proportion of patients (7 of 12) had normal slow-wave frequencies throughout their recordings, which did not dictate normal propagation patterns. No difference was observed in dysrhythmia patterns between the two types of gastroparesis studied. Furthermore, mean ICC counts were markedly reduced in patients with gastroparesis compared with matched individuals as controls. “We found that human gastric electrical abnormalities often occurred at a normal slow-wave frequency, meaning that they could be missed by other methods lacking spatial resolution, such as electrogastrography,” notes O’Grady, who believes the abnormal propagation patterns they observed might be explained by loss of ICCs. O’Grady notes that the new findings are a lasting testament to the hard work of all the investigators involved, but especially co-author Andrew Pullan who sadly died this year: “With great sadness, one of the principal investigators and visionaries for the work, Professor Andrew Pullan, lost his battle with cancer during the final stages of the study.” The authors now hope that their study will be the first of many to use this new technology. They also hope that the technical advances described will contribute to an improved understanding of the underlying pathophysiology of gastroparesis, elucidation of which has thus far been challenging. Katrina Ray Original reference O’Grady, G. et al. Abnormal initiation and conduction of slow-wave activity in gastroparesis, defined by high-resolution electrical mapping. Gastroenterology doi:10.1053/j.gastro.2012.05.036 Further reading Hasler,W. L. Gastroparesis: pathogenesis, diagnosis and management. Nat.Rev.Gastroenterol. Hepatol. 8, 438–453 (2011) Normal antegrade propagation Ectopic activation with tachygastria 0s 20s High-resolution electrical mapping of gastric electrical activity. Courtesy of G. O’Grady. © 2012 Macmillan Publishers Limited. All rights reserved
