Hyperphosphatemia
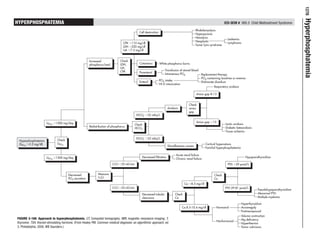
- 1. 1278 Hyperphosphatemia HYPERPHOSPHATEMIA ICD-9CM # 995.5 Child Maltreatment Syndrome Rhabdomyolysis Cell destruction Hyperpyrexia Hemolysis Leukemia Neoplastic CPK Ͼ110 mg/dl Lymphoma Tumor lysis syndrome LDH Ͼ220 mg/dl UA Ͼ7.5 mg/dl Increased Check phosphorus load LDH, Cutaneous White phosphorus burns UA, CPK Transfusion of stored blood Parenteral Intravenous PO4 Replacement therapy PO4-containing laxatives or enemas Enteral PO4 intake Etidronate disodium Vit D intoxication Respiratory acidosis Anion gap 8-13 Check Acidosis anion gap HCOϪ Ͻ22 mEq/L 3 UPO4 Ͼ1500 mg/day Anion gap Ͼ13 Check Lactic acidosis Redistribution of phosphorus Diabetic ketoacidosis HCOϪ3 Tissue ischemia HCOϪ Ͼ22 mEq/L 3 Hyperphosphatemia Check (SPO4 Ͼ5.2 mg/dl) UPO4 Cortical hyperostosis Miscellaneous causes Familial hyperphosphatemia Acute renal failure UPO4 Ͻ1500 mg/day Decreased filtration Hypoparathyroidism Chronic renal failure CrCI Ͻ25 ml/min PTH Ͻ29 pmol/L Decreased Measure Check PO4 excretion CrCI Ca Ca Ͻ8.5 mg/dl CrCI Ͼ25 ml/min PTH 29-81 pmol/L Pseudohypoparathyroidism Decreased tubular Check Abnormal PTH clearance Ca Multiple myeloma Hyperthyroidism Ca 8.5-10.4 mg/dl Hormonal Acromegaly Postmenopausal Volume contraction FIGURE 3-166 pproach to hyperphosphatemia. CT, Computed tomography; MRI, magnetic resonance imaging; T, A Mg deficiency Nonhormonal thyroxine; TSH, thyroid-stimulating hormone. (From Healey PM: Common medical diagnosis: an algorithmic approach, ed Hyperthermia 3, Philadelphia, 2000, WB Saunders.) Tumor calcinosis
