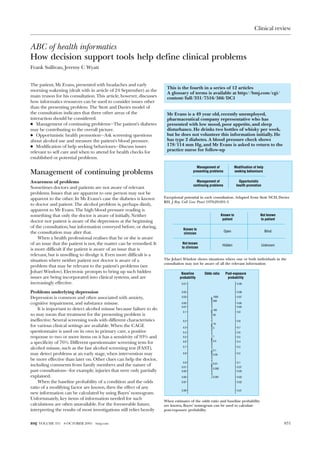
1) The document discusses how decision support tools can help doctors consider issues beyond a patient's presenting problem during a consultation, including management of ongoing medical problems, opportunistic health promotion, and modifying patient help-seeking behaviors.
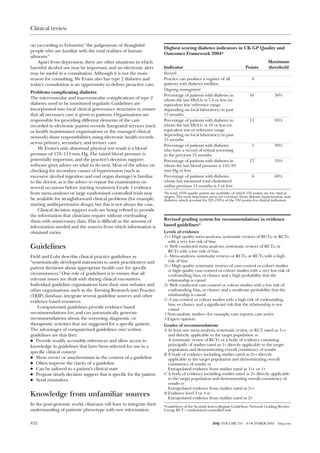
2) It provides an example consultation with patient Mr. Evans, who presented with headaches and sleep issues, but is also found to have high blood pressure and an alcohol problem complicating his known diabetes.
3) The document examines how electronic prompts can help bring hidden health issues to light to provide more effective treatment that addresses underlying problems driving a patient's symptoms.