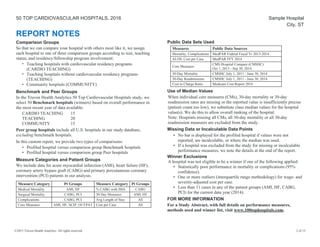
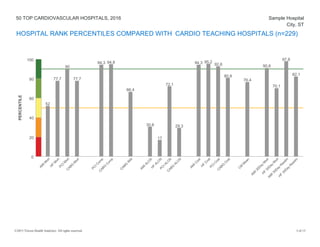
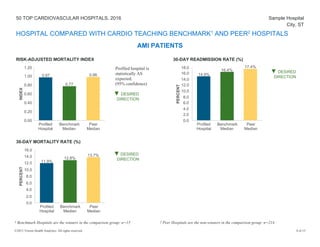
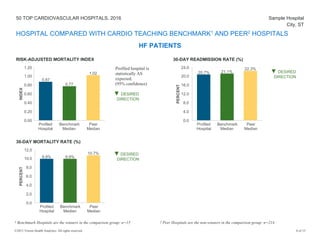
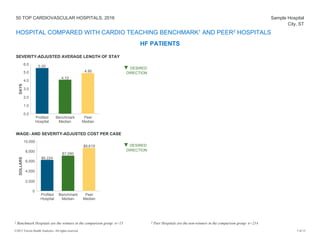
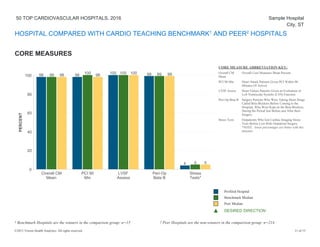
The document provides a performance report on the 50 top cardiovascular hospitals in 2016, outlining comparisons of specific metrics across different hospital types: teaching hospitals with cardiovascular residency programs, teaching hospitals without such programs, and community hospitals. It details measures related to acute myocardial infarction, heart failure, coronary artery bypass graft, and primary percutaneous coronary intervention patients, alongside benchmark statistics and definitions for evaluating hospital performance. Additionally, it notes the criteria for hospital exclusions from the rankings based on performance outliers and missing data.