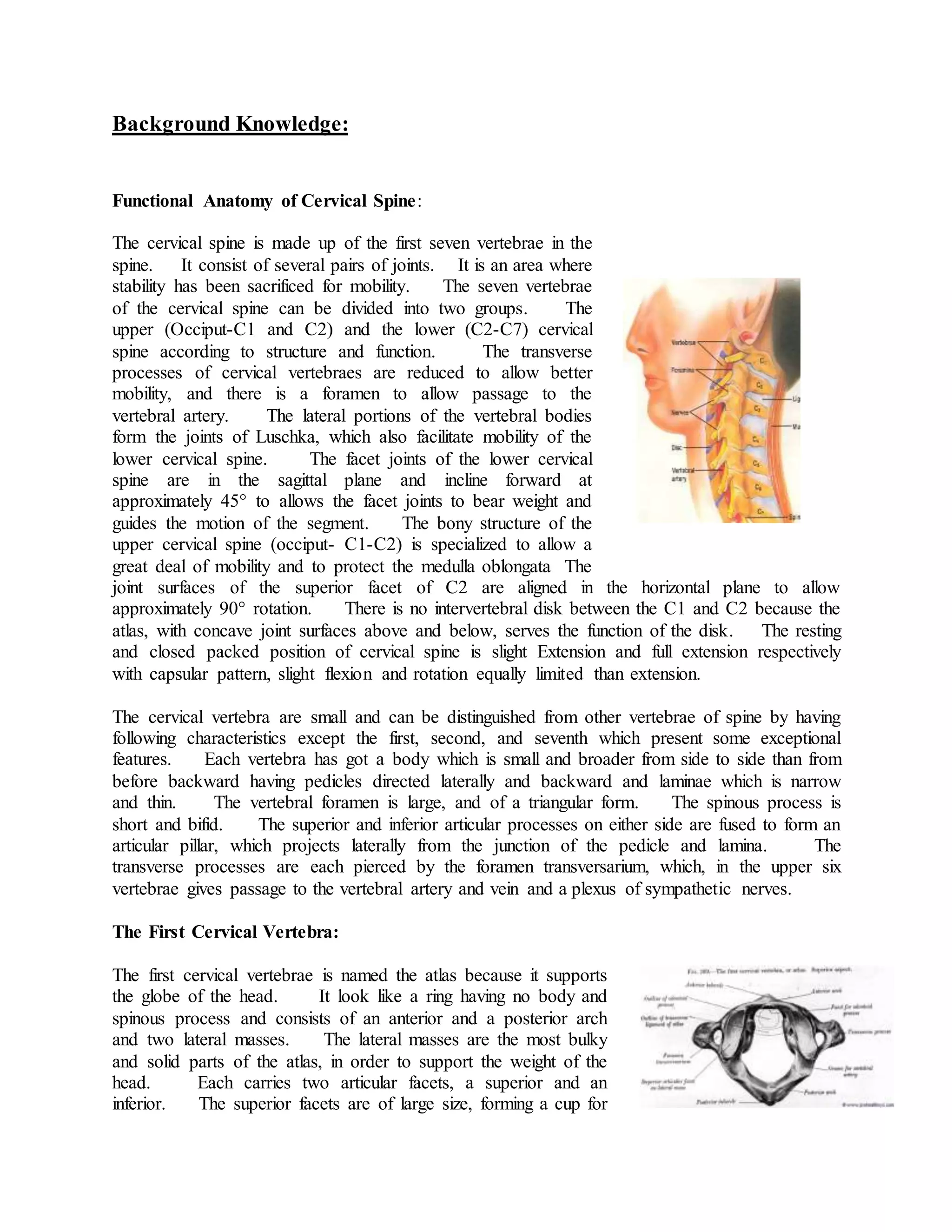
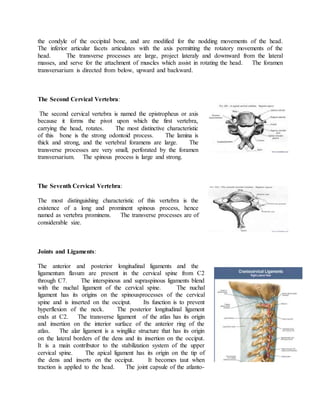
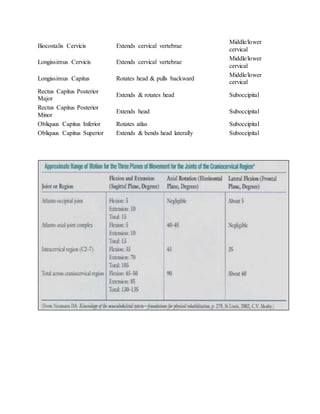
The cervical spine consists of seven vertebrae that provide mobility but less stability than other regions of the spine. It has three subsystems that contribute to stability - passive (bones and ligaments), active (muscles), and neural control. Cervical instability occurs when the neutral zone between ranges of motion increases, the stabilizing subsystems can no longer compensate, and motion quality becomes poor. It can result from trauma, surgery, disease, or degeneration and often involves pain.