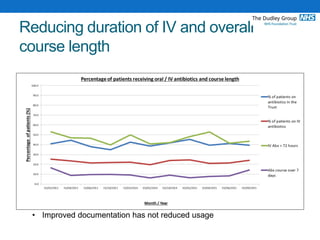
The document outlines antimicrobial stewardship efforts led by Public Health England to reduce the spread of antimicrobial resistance (AMR) in the general population. It details a draft guideline aimed at changing risk-related behaviors, specifically through public information campaigns, education in schools, and interventions in healthcare settings. The guidelines target various audiences, including healthcare providers and the public, and emphasize the importance of using antibiotics responsibly and implementing effective infection prevention strategies.