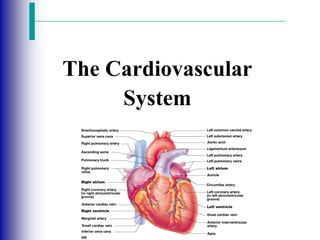
Anatomy of the cardiovascular system .
- 2. The Cardiovascular System A closed system of the heart and blood vessels The function of the cardiovascular system is to deliver oxygen and nutrients and to remove carbon dioxide and other waste products Extensive some 60,000 miles worth. Due to diffusion!
- 3. The Heart Location Thorax between the lungs Pointed apex directed toward left hip lies upon diaphragm About the size of your fist Average Size of Heart 14 cm long 9 cm wide
- 4. The Heart
- 5. Pericardium • Superficial fibrous pericardium • Protects, anchors, and prevents overfilling • Deep two-layered serous pericardium – Parietal layer lines the internal surface of the fibrous pericardium – Visceral layer (epicardium) on external surface of the heart – Separated by fluid-filled pericardial cavity (decreases friction)
- 6. The Heart: Heart Wall Three layers Epicardium Myocardium Endocardium
- 7. The Heart: Chambers Right and left side act as separate pumps Four chambers Atria- Receiving chambers Separated internally by the interatrial septum Coronary sulcus (atrioventricular groove) encircles the junction of the atria and ventricles Ventricles- Discharging chambers Separated by the interventricular septum
- 8. Figure 18.4b (b) Anterior view Brachiocephalic trunk Superior vena cava Right pulmonary artery Ascending aorta Pulmonary trunk Right pulmonary veins Right atrium Right coronary artery (in coronary sulcus) Anterior cardiac vein Right ventricle Right marginal artery Small cardiac vein Inferior vena cava Left common carotid artery Left subclavian artery Ligamentum arteriosum Left pulmonary artery Left pulmonary veins Circumflex artery Left coronary artery (in coronary sulcus) Left ventricle Great cardiac vein Anterior interventricular artery (in anterior interventricular sulcus) Apex Aortic arch Auricle of left atrium
- 9. Figure 18.4e Aorta Left pulmonary artery Left atrium Left pulmonary veins Mitral (bicuspid) valve Aortic valve Pulmonary valve Left ventricle Papillary muscle Interventricular septum Epicardium Myocardium Endocardium (e) Frontal section Superior vena cava Right pulmonary artery Pulmonary trunk Right atrium Right pulmonary veins Fossa ovalis Pectinate muscles Tricuspid valve Right ventricle Chordae tendineae Trabeculae carneae Inferior vena cava
- 10. Blood Flow • The heart is two side-by-side pumps –Right side is the pump for the pulmonary circuit • Vessels that carry blood to and from the lungs • Very thin myocardium? –Left side is the pump for the systemic circuit • Vessels that carry the blood to and from all body tissues • Very thick myocardium
- 11. Figure 18.5 Oxygen-rich, CO2-poor blood Oxygen-poor, CO2-rich blood Capillary beds of lungs where gas exchange occurs Capillary beds of all body tissues where gas exchange occurs Pulmonary veins Pulmonary arteries Pulmonary Circuit Systemic Circuit Aorta and branches Left atrium Heart Left ventricle Right atrium Right ventricle Venae cavae
- 14. Path of Blood Flow
- 15. Coronary Circulation • Arteries – Right and left coronary (in atrioventricular groove), marginal, circumflex, and anterior interventricular arteries • Veins – Small cardiac, anterior cardiac, and great cardiac veins
- 16. Figure 18.7a Right ventricle Right coronary artery Right atrium Right marginal artery Posterior interventricular artery Anterior interventricular artery Circumflex artery Left coronary artery Aorta Anastomosis (junction of vessels) Left ventricle Superior vena cava (a) The major coronary arteries Left atrium Pulmonary trunk
- 17. Figure 18.7b Superior vena cava Anterior cardiac veins Small cardiac vein Middle cardiac vein Great cardiac vein Coronary sinus (b) The major cardiac veins
- 18. The Heart: Valves Allow blood to flow in only one direction Four valves Atrioventricular valves – Bicuspid valve (left)- mitral valve Tricuspid valve (right) Chordae tendineae Semilunar valves between ventricle and artery Pulmonary semilunar valve- right ventricle Aortic semilunar valve- left ventricle
- 19. Figure 18.8c Pulmonary valve Aortic valve Area of cutaway Mitral valve Tricuspid valve Chordae tendineae attached to tricuspid valve flap Papillary muscle (c)
- 20. Operation of Heart Valves
- 21. The Heart: Associated Great Vessels Aorta Pulmonary arteries Vena cava Pulmonary veins (four)
- 22. The Heart: Conduction System Intrinsic conduction system (nodal system) 1% of cardiac cells are self excitable Heart muscle cells contract, without nerve impulses, in a regular, continuous way However, these cells are synchronized by the sinoatrial (SA) node, or pacemaker, located in the wall of the right atrium.
- 23. The Heart: Conduction System Sinoatrial node- Pacemaker 75 bpm Atrioventricular node 50 bpm Atrioventricular bundle Bundle branches Purkinje fibers 30 BPM
- 24. Figure 18.14a (a) Anatomy of the intrinsic conduction system showing the sequence of electrical excitation Internodal pathway Superior vena cava Right atrium Left atrium Purkinje fibers Inter- ventricular septum 1 The sinoatrial (SA) node (pacemaker) generates impulses. 2 The impulses pause (0.1 s) at the atrioventricular (AV) node. The atrioventricular (AV) bundle connects the atria to the ventricles. 4 The bundle branches conduct the impulses through the interventricular septum. 3 The Purkinje fibers depolarize the contractile cells of both ventricles. 5
- 25. Control • While the SA node sets the tempo for the entire heat, it is influenced by a variety of physiological cues. – Two sets of nerves affect heart rate with one set speeding up the pacemaker and the other set slowing it down. – The pacemaker is also influenced by hormones. • For example, epinephrine from the adrenal glands increases heart rate. – The rate of impulse increases in response to increases in body temperature and with exercise.
- 26. Figure 18.15 Thoracic spinal cord The vagus nerve (parasympathetic) decreases heart rate. Cardioinhibitory center Cardio- acceleratory center Sympathetic cardiac nerves increase heart rate and force of contraction. Medulla oblongata Sympathetic trunk ganglion Dorsal motor nucleus of vagus Sympathetic trunk AV node SA node Parasympathetic fibers Sympathetic fibers Interneurons
- 27. The Heart: Cardiac Cycle Atria contract simultaneously Atria relax, then ventricles contract Systole = contraction Diastole = relaxation
- 29. The Heart: Cardiac Output Cardiac output (CO) CO = (heart rate [HR]) x (stroke volume [SV]) 5.25 L/min up to 35 L/min Stroke volume The average stroke volume for a human is about 75 mL Heart Rate Varies but at rest is 70 bpm
- 31. The Heart: Regulation of Heart Rate Starling’s law of the heart – more stretch = stronger contraction Changing heart rate is the most common way to change cardiac output
- 32. The Heart: Regulation of Heart Rate Increased heart rate Sympathetic nervous system Crisis Low blood pressure Hormones Epinephrine Thyroxine Exercise Decreased blood volume
- 33. The Heart: Regulation of Heart Rate Decreased heart rate Parasympathetic nervous system High blood pressure or blood volume Dereased venous return
- 34. Electrocardiogram • recording of electrical changes that occur in the myocardium: • P wave – atrial depolarizatoin • QRS wave – ventricular depolarization • T wave – ventricular repolarization
- 36. Figure 18.17 Atrial depolarization, initiated by the SA node, causes the P wave. P R T Q S SA node AV node With atrial depolarization complete, the impulse is delayed at the AV node. Ventricular depolarization begins at apex, causing the QRS complex. Atrial repolarization occurs. P R T Q S P R T Q S Ventricular depolarization is complete. Ventricular repolarization begins at apex, causing the T wave. Ventricular repolarization is complete. P R T Q S P R T Q S P R T Q S Depolarization Repolarization 1 2 3 4 5 6
- 37. Figure 18.18 (a) Normal sinus rhythm. (c) Second-degree heart block. Some P waves are not conducted through the AV node; hence more P than QRS waves are seen. In this tracing, the ratio of P waves to QRS waves is mostly 2:1. (d) Ventricular fibrillation. These chaotic, grossly irregular ECG deflections are seen in acute heart attack and electrical shock. (b) Junctional rhythm. The SA node is nonfunctional, P waves are absent, and heart is paced by the AV node at 40 - 60 beats/min.
- 38. Blood Vessels: The Vascular System Arteries Arterioles Capillaries Venules Veins
- 40. Blood Vessels: Anatomy Three layers (tunics) Tunic interna Endothelium Tunic media Smooth muscle Tunic externa Mostly fibrous connective tissue
- 41. Differences Between Blood Vessel Types Walls of arteries are the thickest Lumens of veins are larger Skeletal muscle “milks” blood in veins toward the heart Walls of capillaries are only one cell layer thick to allow for exchanges between blood and tissue
- 42. Movement of Blood Through Vessels Most arterial blood is pumped by the heart Veins use the milking action of muscles to help move blood
- 43. Capillary Beds
- 44. Diffusion at Capillary Beds
- 45. Major Arteries of Systemic Circulation
- 46. Major Veins of Systemic Circulation
- 47. Pulse Pulse – pressure wave of blood Monitored at “pressure points” where pulse is easily palpated
- 48. Blood Pressure Systolic –ventricular contraction Diastolic –ventricles relax Pressure in blood vessels decreases as the distance away from the heart increases
- 49. Measuring Arterial Blood Pressure
- 50. Comparison of Blood Pressures in Different Vessels
- 51. Blood Pressure: Effects of Factors Neural factors Autonomic nervous system adjustments (sympathetic division) Renal factors Regulation by altering blood volume Renin – hormonal control
- 52. Blood Pressure: Effects of Factors Temperature Heat has a vasodilation effect Cold has a vasoconstricting effect Chemicals Various substances can cause increases or decreases Diet
- 53. Factors Determining Blood Pressure
- 54. Variations in Blood Pressure Human normal range is variable Normal 140–110 mm Hg systolic 80–70 mm Hg diastolic Hypotension (below 110 mm HG) Often associated with illness Hypertension (above 140 mm HG) Can be dangerous if it is chronic
- 55. Capillary Exchange: Mechanisms Direct diffusion across plasma membranes Endocytosis or exocytosis Some capillaries have gaps (intercellular clefts) Fenestrations of some capillaries Fenestrations = pores
- 56. OLD AGE STINKS • deposition of cholesterol in blood vessels • heart enlarges • cardiac muscle cells die • fibrous connective tissue of heart increases • adipose tissue of heart increases • blood pressure increases • resting heart rate decreases