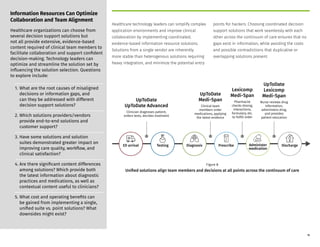
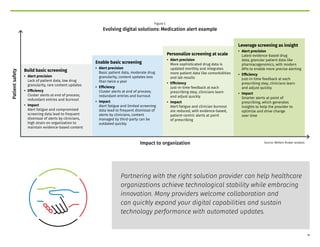
The document discusses the critical role of healthcare technology leaders in evolving digital medication decision support solutions to ensure timely and accurate patient care. It emphasizes the importance of interoperability, effective use of electronic health records (EHRs), and the integration of evidence-based decision support tools to improve clinical outcomes and operational efficiency. Additionally, it highlights the necessity of aligning caregiver resources and accreditation efforts to enhance patient safety and quality of care within healthcare organizations.