Nephrolithiasis_SHISODIA.pptx.pptx
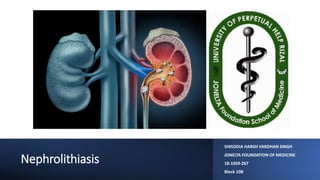
- 1. Nephrolithiasis SHISODIA HARSH VARDHAN SINGH JONELTA FOUNDATION OF MEDICINE 18-1059-267 Block 10B
- 2. Index • Introduction • Epidemiology • Pathogenesis • Risk factors • Approach to the patient
- 3. Introduction • kidney stone disease • common, painful, and costly condition • stone may form due to crystallization of lithogenic factors in the upper urinary tract • patients who have had renal colic report that it is the worst pain
- 4. • There are various types of kidney stones Calcium oxalate stones calcium phosphate uric acid struvite cystine
- 5. Calcium Oxalate is include higher urine calcium, higher urine oxalate, and lower urine citrate. This stone type is insensitive to pH in the physiologic range.
- 6. Calcium phosphate are more common in patients with distal renal tubular acidosis and primary hyperparathyroidism, Including higher concentrations of urine calcium and lower concentrations of urine citrate.
- 7. Uric Acid has two main risk factors for uric acid stones are persistently low urine pH and higher uric acid excretion. Urine pH is the predominant influence on uric acid solubility,Alkalinizing the urine can be readily achieved by increasing the intake of foods rich in alkali (e.g., fruits and vegetables) and reducing the intake of foods that produce acid (e.g., animal flesh).
- 8. Cystine is not easily modified and long-term dietary cystine restriction is not feasible and is unlikely to be successful.
- 9. Struvite Also known as infection stone or triple phosphate stone , form only when the upper urinary tract is infected with urease producing bacteria
- 10. • Infectious stones, if not appropriately treated, can have devastat- ing consequences and lead to end-stage renal disease.
- 11. Epidemiology • Nephrolithiasis is a global disease • NationalHealth and Nutrition Examination Survey data 2007–2010 - 19% of men 9% of women will develop
- 12. ASSOCIATED MEDICAL CONDITIONS • systemic disorder • Several conditions predispose to stone formation gastrointestinal malabsorption primary hyperparathyroid- ism Obesity Type 2 diabetes mellitus distal renal tubular acidosis
- 13. • Other medical condition with a history of nephrolithiasis Hypertension Gout Cholelithiasis reduced bone mineral density chronic kidney disease
- 14. Individuals with medullary sponge kidney (MSK) • condition designated by an anatomic description • have metabolic abnormality higher levels of urine calcium lower levels of urine citrate
- 15. • As intravenous urography is now rarely used, the diagnosis of MSK has become less frequent • nephrolithiasis does not directly cause upper urinary tract infections
- 16. Pthogenesis • processes involved in crystal formation • helpful to view urine as a complex solution • Supersaturation • most clinically important inhibitor of calcium-containing stones is urine citrate. • supersaturation
- 17. • Supersaturation calculated value and does not perfectly predict stone formatinon useful guide as it integrates the multiple factors that are measured in a 24-h urine collection.
- 18. • Thus, the process of stone formation may begin years before a clinically detectable stone is identified. The processes involved in interstitial deposition are under active investigation.
- 19. Risk factor • categorized as Dietary Risk Factors Nondietary Risk Factors Urinary Risk Factors Genetic Risk Factors
- 20. Dietary Risk Factors • animal protein • Oxalate • Sodium • Sucrose • Fructose • Dietary factors associated with a lower risk include calcium, potassium, and phytate.
- 21. Calcium • higher dietary calcium intake is related to a lower risk of stone formation • Low calcium intake is contraindicated as it increases the risk of stone formation and may contribute to lower bone density in stone formers.
- 22. OXALATE • derived from both endogenous production and absorption of dietary oxalate. • absorption may be higher in stone formers • dietary oxalate is only a weak risk factor for stone formation • urinary oxalate is a strong risk factor for calcium oxalate stone formation
- 23. OTHER NUTRIENTS • Vitamin C • Higher intake of animal protein • Higher sodium and sucrose intake
- 24. Nondietary Risk Factors • Age • Race • body size • environment
- 25. Urinary Risk Factors • low urine volume • randomized trial has demonstrated the effectiveness of elevated fluid intake in increasing urine volume and reducing the risk of stone recurrence.
- 26. URINE CALCIUM Higher urine calcium excretion increases the likeli- hood of formation of calcium oxalate and calcium phosphate stones. URINE OXALATE Higher urine oxalate excretion increases the likelihood of calcium oxalate stone formation.
- 27. URINE CITRATE Urine citrate is a natural inhibitor of calcium containing stones, lower urine citrate excretion increases the risk of stone formation. URINE URIC ACID Higher urine levels of uric acid—a risk factor for uric acid stone formation found in individuals with excess purine consumption and rare genetic conditions that lead to overproduction of uric acid.
- 28. URINE pH Urine pH influences the solubility of some crystal types. Uric acid stones when pH <5.5 or lower calcium phosphate stones when ph >6.5 or higher • Cystine is more soluble at higher urine pH Note - Calcium oxalate stones are not influenced by urine pH.
- 29. Genetic Risk Factors • The risk of Nephrolithiasis is more than twofold greater in individuals with a family history of stone disease due to a combination of genetic predisposition and similar environmental exposures • number of monogenic disorders cause Nephrolithiasis
- 30. • most common and well-characterized rare monogenic disorders that lead to stone formation are primary hyperoxaluria and cystinuria Hyperoxaluria Cystinuria
- 31. APPROACH TO THE PATIENT CLINICAL PRESENTATION There are two common presentations for individuals with an acute stone event: renal colic and painless gross hematuria. Renal colic is a misnomer because pain typically does not subside completely; rather, it varies in intensity. When a stone moves into the ureter, the discomfort often begins with a sudden onset of unilateral flank pain. The intensity of the pain can increase rapidly. If the stone lodges in the upper part of the ureter, pain may radiate anteriorly; if the stone is in the lower part of the ureter, pain can radiate to the ipsilateral testicle in men or the ipsilateral labium in women.
- 32. DIAGNOSIS • The diagnosis is often made on the basis of the history, physical examination, and urinalysis. Thus, it may not be necessary to wait for radiographic confirmation before treating the symptoms. The diagnosis is confirmed by an appropriate imaging study—prefer- ably helical CT, which is highly sensitive, allows visualization of uric acid stones • History and physical examination • Helical computed tomography (CT) • Abdominal ultrasound • Renal ultrasound
- 33. Other Diagnosis maybe confused • Other diagnoses may be confused with acute renal colic. If the stone is lodged at the right ureteral pelvic junction, symptoms may mimic those of acute cholecystitis • If the stone blocks the ureter as it crosses over the right pelvic brim, symptoms may mimic acute appendicitis, whereas blockage at the left pelvic brim may be confused with acute diverticulitis • Acute renal colic • Acute appendicitis • Acute pyelonephritis
- 34. LABORATORY EVALUATION • The following serum levels should be determined: • Electrolytes (to uncover hypokalemia or renal tubular acidosis) • Creatinine • Calcium • Uric acid • PTH level should be measure if indicated by high- normal or elevated serum and urine calcium concentrations. • Examination of the sediment • 24-h urine collections
- 35. LONG-TERM FOLLOW-UP • The preventive regimens described above do not cure the underlying pathophysiologic process. Thus these recommendations typically need to be followed for the patient’s lifetime, and it is essential to tailor recommendations in a way that is acceptable to the patient. Because the memory of the acute stone event fades and patients often return to old habits (e.g., insufficient fluid intake), long-term follow-up, including repeat 24-h urine collections, is important to ensure that the preventive regimen has been implemented and has has resulted in the desired reduction in the risk of new stone formation.
- 36. PREVENTION OF NEW STONE FORMATION • Recommendations for preventing stone formation depend on the stone type and the results of metabolic evaluation. • After remediable secondary causes of stone formation (e.g., primary hyperparathyroidism) are excluded, the focus should turn to modification of the urine composition to reduce the risk of new stone formation. • For all stone types, consistently diluted urine reduces the likelihood of crystal formation. The urine volume should be at least 2 L/d.
